Abstract
Background
Better understanding of the brain regions involved in performing laparoscopic surgery is likely to provide important insights for improving laparoscopic training and assessment in the future. To our knowledge, this is the first study using real Fundamentals of Laparoscopy Training (FLS)-based laparoscopic surgery training tasks in the functional magnetic resonance imaging (fMRI) environment to provide extensive characterization of the brain regions involved in this specific task execution.
Methods
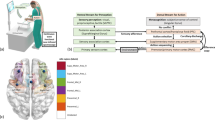
Nine right-handed subjects practiced five FLS-modified laparoscopic surgery-training tasks with a training box for ten sessions in a simulated fMRI environment. Following the last practice session, they underwent 3 T fMRI while performing each task.
Results
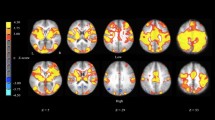
An increase in the extent of brain activation was observed as the complexity of the tasks increased. Activation in the precentral gyrus, postcentral gyrus, and premotor regions was observed in the performance of all tasks, whereas the superior parietal lobe (SPL) was activated in the more complex tasks. The mean score and brain activation for performance with the dominant hand were larger than those observed during performance with the non-dominant hand.
Conclusions
Performing more complex tasks requires higher visual spatial ability and motor planning. Given the need for ambidextrous skills during laparoscopic tasks, the finding that lower scores and smaller brain recruitment occurred in executing tasks with the non-dominant hand than with the dominant hand suggests designing future training tasks to train the non-dominant hand more effectively. This may serve to improve overall performance in bi-manual tasks. Studies of this kind may facilitate the evidence-based development of strategies to improve the quality of laparoscopy training and assessment.


Similar content being viewed by others
References
Veldkamp R, Kuhry E, Hop WCJ, Jeekel J, Kazemier G, Bonjer HJ, Haglind E, Pahlman L, Cuesta MA, Msika S, Morino M, Lacy AM (2005) Laparoscopic surgery versus open surgery for colon cancer: short-term outcomes of a randomised trial. Lancet Oncol 6:477–484
Munz Y, Kumar BD, Moorthy K, Bann S, Darzi A (2004) Laparoscopic virtual reality and box trainers: is one superior to the other? Surg Endosc 18:485–494
Rosser JC, Rosser LE, Savalgi RS (1997) Skill acquisition and assessment for laparoscopic surgery. Arch Surg 132:200–204
Ohuchida K, Kenmotsu H, Yamamoto A, Sawada K, Hayami T, Morooka K, Takasugi SH, Konish K, Ieri S, Tanoue K, Iwamoto Y, Tanaka M, Hashizume M (2009) The frontal cortex is activated during learning of endoscopic procedures. Surg Endosc 23:2296–2301
Leff DR, Orihuela Espina F, Atallah L, Athanasiou T, Leong JJH, Darzi AAW, Yang GZ (2008) Modelling dynamic fronto-parietal behaviour during minimally invasive surgery—a Markovian trip distribution approach. Med Image Comput Comput Assist Interv 11:595–602
Cui X, Bray S, Bryant DM, Glover GH, Reiss AL (2011) A quantitative comparison of NIRS and fMRI across multiple cognitive tasks. Neuroimage 54:2808–2821
Huettel SA, Song AW, McCarthy G (2004) Functional magnetic resonance imaging, 1st edn. Sinauer, Sunderland
Debaerea F, Wenderotha N, Sunaertb S, Van Heckeb P, Swinnen SP (2004) Cerebellar and premotor function in bimanual coordination: parametric neural responses to spatiotemporal complexity and cycling frequency. Neuroimage 21:1416–1427
Vakil E, Kahan Sh, Huberman M, Osimani A (2000) Motor and non-motor sequence learning in patients with basal ganglia lesions: the case of serial reaction time. Neuropsychologia 38:1–10
Wanzel KR, Hamstra SJ, Anastakis DJ, Matsumoto E, Cusimano M (2002) Effect of visual-spatial ability on learning of spatially-complex surgical skills. Lancet 359:230–231
Wanzel KR, Anastakis DJ, McAndrews MP, Grober ED, Sidhu RS, Taylor K, Mikulis DJ, Hamstra SJ (2007) Visual-spatial ability and fMRI cortical activation in surgery residents. Am J Surg 193:507–510
Botden S, Torab F, Buzink SN, Jakimowicz JJ (2008) The importance of haptic feedback in laparoscopic suturing training and the additive value of virtual reality simulation. Surg Endosc 22:1214–1222
Soper NJ, Fried GM (2008) The fundamentals of laparoscopic surgery: its time has come. Bull Am Coll Surg 93:30–32
Scott DJ, Ritter M, Tesfay ST, Pimentel EA, Nagji A, Fried GM (2008) Certification pass rate of 100 % for fundamentals of laparoscopic surgery skills after proficiency-based training. Surg Endosc 22:1887–1893
Bahrami P, Schweizer TA, Tam F, Grantcharov TP, Cusimano MD, Graham SJ (2011) Functional MRI-compatible laparoscopic surgery training simulator. Magn Reson Med 65:873–881
Oldfield RC (1971) The assessment and analysis of handedness: the Edinburgh inventory. Neuropsychologia 9:97–114
Cox RW (1996) AFNI: software for analysis and visualization of functional magnetic resonance neuroimages. Comput Biomed Res 29:162–173
Martin JH (2003) Neuroanatomy: text and Atlas, 3rd edn. McGraw Hill, New York
Karimyan V, Orihuela-Espina F, Leff DR, Clark J, Sodergren M, Darzi A, Yang GZ (2012) Spatial awareness in Natural Orifice Transluminal Endoscopic Surgery (NOTES) navigation. Int J Surg 10:80–86
Tsuda H, Aoki T, Oku N, Kimura Y, Hatazawa J, Kinoshita H (2009) Functional brain areas associated with manipulation of a prehensile tool: a PET study. Hum Brain Mapp 30:2879–2889
Rushworth MFS, Walton ME, Kennerley SW, Bannerman DM (2004) Action sets and decisions in the medial frontal cortex. Trends Cognit Sci 8:410–417
Mason MF, Norton MI, Van Horn JD, Wegner DM, Grafton ST, Macrae CN (2007) Wandering minds: the default network and stimulus-independent thought. Science 393:315
Buckner RL, JAndrews-Hanna JR, Schacter DL (2008) The brain’s default network: anatomy, function, and relevance to disease. Ann N Y Acad Sci 1124:1–38
Jäncke L, Petersc M, Himmelbacha M, Nösselta T, Shahb J, Steinmetz H (2000) fMRI study of bimanual coordination. Neuropsychologia 38:164–174
Gupta R, Cathelineau X, Robert F, Vallancien G (2004) Feedback from operative performance to improve training program of laparoscopic radical prostatectomy. J Endourol 18:836–839
Nieboer TE, Sari V, Kluivers KB, Weinans MJN, Vierhout ME, Stegeman DF (2012) A randomized trial of training the non-dominant upper extremity to enhance laparoscopic performance. Minim Invasive Ther 21:259–264
Grafton ST, Hazeltine E, Ivry RB (2002) Motor sequence learning with the nondominant left hand: a PET functional imaging study. Exp Brain Res 146:369–378
Halsband U, Lange RK (2006) Motor learning in man: a review of functional and clinical studies. J Physiol Paris 99:414–424
Leff DR, Elwell CE, Orihuela-Espina F, Atallah L, Delpy DT, Darzi AW, Yang GZ (2008) Changes in prefrontal cortical behaviour depend upon familiarity on a bimanual co-ordination task: an fNIRS study. Neuroimage 39:805–813
Acknowledgments
The authors acknowledge the generous Grant support from the Natural Sciences and Engineering Research Council (NSERC) of Canada.
Disclosure
P. Bahrami, Dr. S.J. Graham, Dr. T.P. Grantcharov, Dr. M.D. Cusimano, Dr. O.D. Rotstein, A. Mansur, and Dr. T.A. Schweizer have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bahrami, P., Graham, S.J., Grantcharov, T.P. et al. Neuroanatomical correlates of laparoscopic surgery training. Surg Endosc 28, 2189–2198 (2014). https://doi.org/10.1007/s00464-014-3452-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-014-3452-7