Abstract
Background
To date, several training and evaluation systems for endoscopic surgery have been developed, such as virtual-reality simulators and box trainers. However, despite current advances in these objective assessments, no functional brain studies during learning of endoscopic surgical skills have been carried out. In the present study, we investigated cortical activation using near-infrared spectroscopy (NIRS) during endoscopic surgical tasks.
Study design
A total of 21 right-handed subjects, comprising 4 surgical experts, 4 trainees, and 13 novices, participated in the study. Suturing and knot-tying tasks were performed in a box trainer. Cortical activation was assessed in all subjects by task-related changes in hemoglobin (Hb) oxygenation using NIRS.
Results
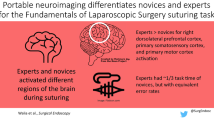
In surgical experts and novices with no experience of endoscopic surgical training, we found no changes in oxy-Hb, deoxy-Hb or total-Hb levels in any of the frontal channels. In surgical trainees and one novice with experience of endoscopic surgical training, we found significant increases in oxy-Hb and total-Hb levels in most of the frontal channels. There were significant differences in oxy-Hb and total-Hb levels in CH-19 between surgical experts and trainees (p = 0.02 for both), and between surgical trainees and novices with no experience of endoscopic surgical training (p = 0.008 for both). Furthermore, additional training increased oxy-Hb levels in the frontal cortex of novices with no experience of endoscopic surgical training but had no such effect on surgical experts.
Conclusions
The present data suggest that NIRS is a feasible tool for assessing brain activation during endoscopic surgical tasks, and may have a large impact on the future development of teaching, training, and assessment methods for endoscopic surgical skills.



Similar content being viewed by others
Abbreviations
- NIRS:
-
Near-infrared spectroscopy
- Hb:
-
Hemoglobin
References
Atkeson CG (1989) Learning arm kinematics and dynamics. Annu Rev Neurosci 12:157–183
Bermas H, Fenoglio M, Haun W, Moore JT (2004) Laparoscopic suturing and knot tying: a comparison of standard techniques to a mechanical assist device. JSLS 8:187–189
Doyon J, Benali H (2005) Reorganization and plasticity in the adult brain during learning of motor skills. Curr Opin Neurobiol 15:161–167
Gallagher AG, Lederman AB, McGlade K, Satava RM, Smith CD (2004) Discriminative validity of the Minimally Invasive Surgical Trainer in Virtual Reality (MIST-VR) using criteria levels based on expert performance. Surg Endosc 18:660–665
Grantcharov TP, Bardram L, Funch-Jensen P, Rosenberg J (2003) Learning curves and impact of previous operative experience on performance on a virtual reality simulator to test laparoscopic surgical skills. Am J Surg 185:146–149
Halsband U, Lange RK (2006) Motor learning in man: a review of functional and clinical studies. J Physiol Paris 99:414–424
Hamilton EC, Scott DJ, Fleming JB, Rege RV, Laycock R, Bergen PC, Tesfay ST, Jones DB (2002) Comparison of video trainer and virtual reality training systems on acquisition of laparoscopic skills. Surg Endosc 16:406–411
Hatakenaka M, Miyai I, Mihara M, Sakoda S, Kubota K (2007) Frontal regions involved in learning of motor skill-A functional NIRS study. Neuroimage 34:109–116
Hikosaka O, Nakamura K, Sakai K, Nakahara H (2002) Central mechanisms of motor skill learning. Curr Opin Neurobiol 12:217–222
Jaeger JJ, Lockwood AH, Van Valin RD Jr, Kemmerer DL, Murphy BW, Wack DS (1998) Sex differences in brain regions activated by grammatical and reading tasks. NeuroReport 9:2803–2807
Jordan JA, Gallagher AG, McGuigan J, McClure N (2001) Virtual reality training leads to faster adaptation to the novel psychomotor restrictions encountered by laparoscopic surgeons. Surg Endosc 15:1080–1084
Kelly AM, Garavan H (2005) Human functional neuroimaging of brain changes associated with practice. Cereb Cortex 15:1089–1102
Larsson A (2001) Intracorporeal suturing and knot tying in surgical simulation. Stud Health Technol Inform 81:266–271
Madan AK, Frantzides CT, Shervin N, Tebbit CL (2003) Assessment of individual hand performance in box trainers compared to virtual reality trainers. Am Surg 69:1112–1114
Miyai I, Tanabe HC, Sase I, Eda H, Oda I, Konishi I, Tsunazawa Y, Suzuki T, Yanagida T, Kubota K (2001) Cortical mapping of gait in humans: a near-infrared spectroscopic topography study. Neuroimage 14:1186–1192
Schreppel T, Egetemeir J, Schecklmann M et al (2008) Activation of the prefrontal cortex in working memory and interference resolution processes assessed with near-infrared spectroscopy. Neuropsychobiology 57:188–193
Schreppel TJ, Pauli P, Ellgring H, Fallgatter AJ, Herrmann MJ (2008) The impact of prefrontal cortex for selective attention in a visual working memory task. Int J Neurosci 118:1673–1688
Munz Y, Kumar BD, Moorthy K, Bann S, Darzi A (2004) Laparoscopic virtual reality and box trainers: is one superior to the other? Surg Endosc 18:485–494
Nguyen NT, Mayer KL, Bold RJ, Larson M, Foster S, Ho HS, Wolfe BM (2000) Laparoscopic suturing evaluation among surgical residents. J Surg Res 93:133–136
Shaywitz BA, Shaywitz SE, Pugh KR, Constable RT, Skudlarski P, Fulbright RK, Bronen RA, Fletcher JM, Shankweiler DP, Katz L, Gore CJ (1995) Sex differences in the functional organization of the brain for language. Nature 373:607–609
Strom P, Kjellin A, Hedman L, Johnson E, Wredmark T, Fellander-Tsai L (2003) Validation and learning in the Procedicus KSA virtual reality surgical simulator. Surg Endosc 17:227–231
Suzuki M, Miyai I, Ono T, Oda I, Konishi I, Kochiyama T, Kubota K (2004) Prefrontal and premotor cortices are involved in adapting walking and running speed on the treadmill: an optical imaging study. Neuroimage 23:1020–1026
Szabo Z, Hunter J, Berci G, Sackier J, Cuschieri A (1994) Analysis of surgical movements during suturing in laparoscopy. Endosc Surg Allied Technol 2:55–61
Tanoue K, Ieiri S, Konishi K, Yasunaga T, Okazaki K, Yamaguchi S, Yoshida D, Kakeji Y, Hashizume M (2008) Effectiveness of endoscopic surgery training for medical students using a virtual reality simulator versus a box trainer: a randomized controlled trial. Surg Endosc 22:985–990
Vikingstad EM, George KP, Johnson AF, Cao Y (2000) Cortical language lateralization in right-handed normal subjects using functional magnetic resonance imaging. J Neurol Sci 175:17–27
Author information
Authors and Affiliations
Corresponding author
Additional information
Supported in part by a grant from the New Energy and Industrial Technology Development Organization.
Rights and permissions
About this article
Cite this article
Ohuchida, K., Kenmotsu, H., Yamamoto, A. et al. The frontal cortex is activated during learning of endoscopic procedures. Surg Endosc 23, 2296–2301 (2009). https://doi.org/10.1007/s00464-008-0316-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-008-0316-z