Abstract
Background
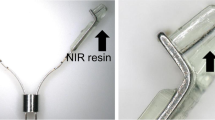
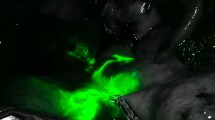
In totally laparoscopic distal gastrectomy, determining the resection line with safe proximal margins is often difficult, particularly for tumors located in a relatively upper area. This is because, in contrast to open surgery, identifying lesions by palpating or opening the stomach is essentially impossible. This study introduces a useful method of tumor identification that is accurate, safe, and rapid.
Methods
On the operation day, after inducing general anesthesia, a mixture of sodium hyaluronate and patent blue is injected into the submucosal layer of the proximal margin. When resecting stomach, all marker spots should be on the resected side. In all cases, the proximal margin is examined histologically by using frozen sections during the operation.
Results
From October 2009 to September 2011, a prospective study that evaluated this method was performed. A total of 34 patients who underwent totally laparoscopic distal gastrectomy were enrolled in this study. Approximately 5 min was required to complete the procedure. Proximal margins were negative in all cases, and the mean ± standard deviation length of the proximal margin was 23.5 ± 12.8 mm. No side effects, such as allergy, were encountered.
Conclusions
As a method of tumor identification for totally laparoscopic distal gastrectomy, this procedure appears accurate, safe, and rapid.








Similar content being viewed by others
References
Kitano S, Iso Y, Moriyama M, Sugimachi K (1994) Laparoscopy-assisted Billroth I gastrectomy. Surg Laparosc Endosc 4:146–148
Song KY, Park CH, Kang HC, Kim JJ, Park SM, Jun KH, Chin HM, Hur H (2008) Is totally laparoscopic gastrectomy less invasive than laparoscopy-assisted gastrectomy? Prospective, multicenter study. J Gastrointest Surg 12:1015–1021
Kinoshita T, Shibasaki H, Oshiro T, Okazumi S, Katoh R (2011) Comparison of laparoscopy-assisted and total laparoscopic Billroth-I gastrectomy for gastric cancer: a report of short-term outcomes. Surg Endosc 25:1395–1401
Jeong O, Cho SB, Joo YE, Ryu SY, Park YK (2011) Novel technique for intraoperative tumor localization during totally laparoscopic distal gastrectomy: autologous blood tattooing. Surg Endosc 26:1778–1783
Kim HI, Hyung WJ, Lee CR, Lim JS, An JY, Cheong JH, Choi SH, Noh SH (2011) Intraoperative portable abdominal radiograph for tumor localization: a simple and accurate method for laparoscopic gastrectomy. Surg Endosc 25:958–963
Park DJ, Lee HJ, Kim SG, Jung HC, Song IS, Lee KU, Choe KJ, Yang HK (2005) Intraoperative gastroscopy for gastric surgery. Surg Endosc 19:1358–1361
Union for International Cancer Center (2009) TNM classification of malignant tumours, 7th edn. Wiley-Blackwell, New Jersey
Kanaya S, Kawamura Y, Kawada H, Iwasaki H, Gomi T, Satoh S, Uyama I (2011) The delta-shaped anastomosis in laparoscopic distal gastrectomy: analysis of initial 100 consecutive procedures of intracorporeal gastroduodenostomy. Gastric Cancer 14:365–371
Japanese Gastric Cancer Association (2011) Japanese gastric cancer treatment guidelines 2010 (ver.3). Gastric Cancer 14:113–123
Yamamoto H, Yahagi N, Oyama T, Gotoda T, Doi T, Hirasaki S, Sugano K, Tajiri H, Saito D (2008) Usefulness and safety of 0.4 % sodium hyaluronate solution as a submucosal fluid “cushion” in endoscopic resection for gastric neoplasms: a prospective multicenter trial. Gastrointest Endosc 67:830–839
Longnecker SM, Guzzardo MM, Van Voris LP (1985) Life-threatening anaphylaxis following subcutaneous administration of isosulfan blue 1 %. Clin Pharm 4:219–221
Daley MD, Norman PH, Leak JA, Nguyen DT, Bui TP, Kowalski AM, Srejic U, Popat K, Arens JF, Gershenwald JE (2004) Adverse events associated with the intraoperative injection of isosulfan blue. J Clin Anesth 16:332–341
Wong A, Spillane A (2012) Patent blue V dye anaphylaxis: experience of Australian and New Zealand surgeons. ANZ J Surg. doi:10.1111/j.1445-2197.2012.06277.x
Momeni R, Ariyan S (2004) Pulse oximetry declines due to intradermal isosulfan blue dye: a controlled prospective study. Ann Surg Oncol 11:434–437
Koivusalo AM, VonSmitten K, Lindgren L (2002) Sentinel node mapping affects intraoperative pulse oximetric recordings during breast cancer surgery. Acta Anaaestheiol Scand 46:411–414
Rabin I, Chikman B, Lavy R, Poluksht N, Halpern Z, Wassermann I, Gold-Deutch R, Sandbank J, Halevy A (2010) The accuracy of sentinel node mapping according to T stage in patients with gastric cancer. Gastric Cancer 13:30–35
Orsenigo E, Tomajer V, Di Palo S, Albarello L, Doglioni C, Masci E, Viale E, Staudacher C (2008) Sentinel node mapping during laparoscopic distal gastrectomy for gastric cancer. Surg Endosc 22:118–121
Disclosures
Masatoshi Nakagawa, Kazuhisa Ehara, Masaki Ueno, Tsuyoshi Tanaka, Sachiko Kaida, and Harushi Udagawa have no conflict of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nakagawa, M., Ehara, K., Ueno, M. et al. Accurate, safe, and rapid method of intraoperative tumor identification for totally laparoscopic distal gastrectomy: injection of mixed fluid of sodium hyaluronate and patent blue. Surg Endosc 28, 1371–1375 (2014). https://doi.org/10.1007/s00464-013-3319-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-013-3319-3