Abstract
Background
Success of totally extraperitoneal (TEP) inguinal herniorrhaphy depends upon strengthening of the weakened native tissue by inflammation resulting in mesh–aponeurosis scar tissue (MAST) complex formation. The inflammatory response attributable to polypropylene (PP) content of the mesh is linked to weight of PP and pore size of the mesh. Continuation of the inflammatory process beyond MAST complex formation can entrap contiguous structures, leading to adverse outcome such as groin pain. Reduction of PP content has been shown to be beneficial in animal studies. Paucity of randomized controlled trials (RCTs) on human beings has left choice of mesh to surgeon preference or cost. We carried out a double-blind RCT comparing heavy- and lightweight PP-based meshes in TEP.
Patients and methods
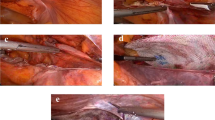
Consecutive, married, sexually active male candidates for bilateral TEP herniorrhaphy were enrolled without any exclusion, with ethical and informed consent protocol. Standard TEP technique was followed for day-care surgery. Heavy- and lightweight meshes were implanted in each patient, one in either groin after randomization. Surgeon and patient were blinded to side of groin and type of mesh. An independent doctor (AID) evaluated the patients for groin pain, discomfort, sexual dysfunction, and clinical recurrence. A nonmedical secretary/AID transferred prospective data for both sides of groin collected by AID to Microsoft Excel.
Results
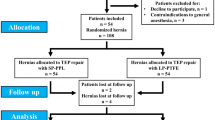
Twenty-five bilateral TEPs implanting 25 heavy- and 25 lightweight PP meshes, one of each type in each patient, were performed from December 2005 to July 2007 without difficulty or complication. Lightweight PP mesh was associated with significantly better pain scores, patient comfort, and sexual function. There was no infection or recurrence with either type of mesh.
Conclusion
Lightweight PP mesh is associated with significantly better outcomes in TEP inguinal herniorrhaphy as compared with heavyweight PP mesh.
Similar content being viewed by others
References
Bowne WB, Morgenthal CB, Castro AE, Shah P, Ferzli GS (2007) The role of endoscopic extraperitoneal herniorrhaphy: where do we stand in 2005? Surg Endosc 21(5):707–712
Fitzgibbons RJ Jr (2005) Can we be sure polypropylene mesh causes infertility? Ann Surg 241(4):559–561
Loos MJA, Roumen RMH, Scheltinga MRM (2007) Classifying postherniorrhaphy pain syndromes following elective inguinal hernia repair. World J Surg 31(9):1760–1765
Shin D, Lipshultz LI, Goldstein M, Barmé GA, Fuchs EF, Nagler HM, McCallum SW, Niederberger CS, Schoor RA, Brugh VM 3rd, Honig SC (2005) Herniorrhaphy with polypropylene mesh causing inguinal vasal obstruction: a preventable cause of obstructive azoospermia. Ann Surg 241(4):553–558
Aasvang EK, Møhl B, Kehlet H (2007) Ejaculatory pain: a specific postherniotomy pain syndrome? Anesthesiology 107(2):298–304
Novitsky YW, Cristiano JA, Harrell AG, Newcomb W, Norton JH, Kercher KW, Heniford BT (2008) Immunohistochemical analysis of host reaction to heavyweight-, reduced-weight-, and expanded polytetrafluoroethylene (ePTFE)-based meshes after short- and long-term intraabdominal implantations. Surg Endosc 22(4):1070–1076
Benes Z, Herdegen P, Puskárová G, Antos Z (2007) Complications of laparoscopic procedures of inguinal hernias, diagnosed on colonoscopy. Rozhl Chir 86(8):420–422
Harrell AG, Novitsky YW, Cristiano JA, Gersin KS, Norton HJ, Kercher KW, Heniford BT (2007) Prospective histologic evaluation of intra-abdominal prosthetics four months after implantation in a rabbit model. Surg Endosc 21(7):1170–1174
Bingener J, Buck L, Richards M, Michalek J, Schwesinger W, Sirinek K (2007) Long-term outcomes in laparoscopic vs open ventral hernia repair. Arch Surg 142(6):562–567
Novitsky YW, Harrell AG, Cristiano JA, Paton BL, Norton HJ, Peindl RD, Kercher KW, Heniford BT (2007) Comparative evaluation of adhesion formation, strength of ingrowth, and textile properties of prosthetic meshes after long-term intra-abdominal implantation in a rabbit. J Surg Res 140(1):6–11
Eriksen JR, Gögenur I, Rosenberg J (2007) Choice of mesh for laproscopic ventral hernia repair. Hernia 11(6):481–492
Novitsky YW, Harrell AG, Hope WW, Kercher KW, Heniford BT (2007) Meshes in hernia repair. Surg Technol Int 16:123–127
Champault G, Bernard C, Rizk N, Polliand C (2007) Inguinal hernia repair: the choice of prosthesis outweighs that of technique. Hernia 11(2):125–128
Kehlet H, Bay-Nielsen M, for the Danish Hernia Database Collaboration (2008) Nationwide quality improvement of groin hernia repair from the Danish Hernia Database of 87,840 patients from 1998 to 2005. Hernia 12(1):1–7
Ausems ME, Hulsewé KW, Hooymans PM, Hoofwijk AG (2007) Postoperative analgesia requirements at home after inguinal hernia repair: effects of wound infiltration on postoperative pain. Anaesthesia 62(4):325–331
Pélissier E, Fingerhut A, Ngo P (2007) Inguinal hernia. What techniques are available for the surgeon? Theoretical and practical advantages and disadvantages. J Chir (Paris) 144 Spec No 4:5S35–5S40
Weyhe D, Belyaev O, Müller C, Meurer K, Bauer KH, Papapostolou G, Uhl W (2007) Improving outcomes in hernia repair by the use of light meshes–a comparison of different implant constructions based on a critical appraisal of the literature. World J Surg 31(1):234–244
Ersin S, Aydin U, Makay O, Icoz G, Tamsel S, Sozbilen M, Killi R (2006) Is testicular perfusion influenced during laparoscopic inguinal hernia surgery? Surg Endosc 20(4):685–689
Demirer S, Kepenekci I, Evirgen O, Birsen O, Tuzuner A, Karahuseyinoglu S, Ozban M, Kuterdem E (2006) The effect of polypropylene mesh on ilioinguinal nerve in open mesh repair of groin hernia. J Surg Res 131(2):175–181
Weyhe D, Belyaev O, Buettner G, Mros K, Mueller C, Meurer K, Papapostolou G, Uhl W (2008) In vitro comparison of three different mesh constructions. ANZ J Surg 78(1–2):55–60
Bay-Nielsen M, Perkins FM, Kehlet H, Danish Hernia Database (2001) Pain and functional impairment 1 year after inguinal herniorrhaphy: a nationwide questionnaire study. Ann Surg 233(1):1–7
Thompson JS, Gibbs JO, Reda DJ, McCarthy M Jr, Wei Y, Giobbie-Hurder A, Fitzgibbons RJ Jr (2008) Does delaying repair of an asymptomatic hernia have a penalty? Am J Surg 195(1):89–93
Weyhe D, Meurer K, Belyaev O, Senkal M, Harrer P, Zumtobel V, Bauer KH (2007) Do various mesh placement techniques affect the outcome in totally extraperitoneal hernia repair? What is the role of the surgeon? J Laparoendosc Adv Surg Tech A 17(6):749–758
Taylor C, Layani L, Liew V, Ghusn M, Crampton N, White S (2008) Laparoscopic inguinal hernia repair without mesh fixation, early results of a large randomised clinical trial. Surg Endosc 22(3):757–762
Koch CA, Greenlee SM, Larson DR, Harrington JR, Farley DR (2006) Randomized prospective study of totally extraperitoneal inguinal hernia repair: fixation versus no fixation of mesh. JSLS 10(4):457–460
Moreno-Egea A, Torralba Martínez JA, Morales Cuenca G, Aguayo Albasini JL (2004) Randomized clinical trial of fixation vs nonfixation of mesh in total extraperitoneal inguinal hernioplasty. Arch Surg 139(12):1376–1379
Chatzimavroudis G, Koutelidakis I, Papaziogas B, Tsaganos T, Koutoukas P, Giamarellos-Bourboulis E, Atmatzidis S, Atmatzidis K (2008) The effect of the type of intraperitoneally implanted prosthetic mesh on the systemic inflammatory response. Hernia 12(3):277–283
Cuschieri A (2007) Patient reported outcomes: cinderella subject, no more. Surg Endosc 21:501–502
Neugebauer EAM, Wilkinson RC, Kehlet H, Schug SA, on behalf of the PROSPECT Working Group (2007) PROSPECT: a practical method for formulating evidence-based expert recommendations for the management of postoperative pain. Surg Endosc 21(7):1047–1053
Acknowledgements
The authors are grateful to our secretary Ms Pooja Pant and a school child Nayan Agarwal who managed the data to ensure the study model.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Agarwal, B.B., Agarwal, K.A. & Mahajan, K.C. Prospective double-blind randomized controlled study comparing heavy- and lightweight polypropylene mesh in totally extraperitoneal repair of inguinal hernia: early results. Surg Endosc 23, 242–247 (2009). https://doi.org/10.1007/s00464-008-0188-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-008-0188-2