Abstract
Background
The two main treatment options for esophageal achalasia are laparoscopic distal esophageal myotomy (LM) and pneumatic dilatation (PD). Our objective was to compare the costs of these management strategies.
Methods
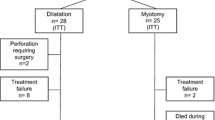
We constructed a decision analytic model consisting of two treatment strategies for patients diagnosed with achalasia. Probabilities of events were systematically derived from a literature review, supplemented by expert opinion when necessary. Costs were estimated from the perspective of a third-party payer and society, including both direct and indirect costs. Future costs were discounted at a rate of 5.5% over a time horizon of 5 and 10 years. Uncertainty in the probability estimates was incorporated using probabilistic sensitivity analyses. We tested uncertainty in the model by modifying key assumptions and repeating the analysis.
Results
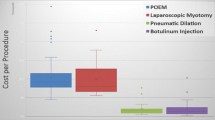
From the societal perspective, the expected cost per patient was $10,789 (LM) compared with $5,315 (PD) five years following diagnosis, and $11,804 (LM) compared with $7,717 (PD) after 10 years. The 95% confidence interval of the incremental cost per patient treated with LM was ($5,280, $5,668) after five years, and ($3,863, $4,311) after 10 years. The incremental cost of LM was similar from the third-party payer perspective and in the secondary model analyzed.
Conclusions
Initial LM is a more costly management strategy under all clinically plausible scenarios tested in this model. Further research is needed to determine patients’ preferences for the two treatment modalities, and society’s willingness to bear the incremental cost of LM for those who choose it.




Similar content being viewed by others
References
Bank of Canada. Available at: http://www.bankofcanada.ca/en/rates/interest-look.html. Accessed March 10, 2006
Ontario Case Costing Initiative. Available at: http://www.occp.com. Accessed March 10, 2006
Ontario Ministry of Health, Long-Term Care. Available at: http://www.health.gov.on.ca/english/providers/program/ohip/sob/physserv/physserv_mn.html. Accessed March 10, 2006
Statistics Canada. Available at: http://www.statcan.ca Accessed April 28, 2006
Allescher HD, Storr M, Seige M, Gonzales-Donoso R, Ott R, Born P, Frimberger E, Weigert N, Stier A, Kurjak M, Rosch T, Classen M (2001) Treatment of achalasia: botulinum toxin injection vs. pneumatic balloon dilation. A prospective study with long-term follow-Up. Endoscopy 33: 1007–1017
Alonso-Aguirre P, Aba-Garrote C, Estevez-Prieto E, Gonzalez-Conde B, Vazquez-Iglesias JL (2003) Treatment of achalasia with the Witzel dilator: a prospective randomized study of two methods. Endoscopy 35: 379–382
Anselmino M, Perdikis G, Hinder RA, Polishuk PV, Wilson P, Terry JD, Lanspa SJ (1997) Heller myotomy is superior to dilatation for the treatment of early achalasia. Arch Surg 132: 233–240
Bansal R, Nostrant TT, Scheiman JM, Koshy S, Barnett JL, Elta GH, Chey WD (2003) Intrasphincteric botulinum toxin versus pneumatic balloon dilation for treatment of primary achalasia. J Clin Gastroenterol 36: 209–214
Beckingham IJ (2006) Achalasia of the cardia: dilatation or division? Is pneumatic balloon dilatation justifiable anymore? Ann R Coll Surg Engl 88: 11–12
Boztas G, Mungan Z, Ozdil S, Akyuz F, Karaca C, Demir K, Kaymakoglu S, Besisik F, Cakaloglu Y, Okten A (2005) Pneumatic balloon dilatation in primary achalasia: the long-term follow-up results. Hepatogastroenterology 52: 475–480
Braga M, Vignali A, Zuliani W, Frasson M, Di Serio C, Di Carlo V (2005) Laparoscopic versus open colorectal surgery: cost-benefit analysis in a single-center randomized trial. Ann Surg 242: 890–895
Brauer CA, Rosen AB, Olchanski NV, Neumann PJ (2005) Cost-utility analyses in orthopaedic surgery. J Bone Joint Surg Am 87: 1253–1259
Bruley des Varannes S, Scarpignato C (2001) Current trends in the management of achalasia. Digest Liver Dis 33: 266–277
Caunedo A, Romero R, Hergueta P, Gomez BJ, Rodriguez-Tellez M, Linares E, Sanchez-Gey S, Pellicer FJ, Herrerias JM (2003) Short- and medium-term clinical efficacy of three endoscopic therapies for achalasia: a single-blinded prospective study. Rev Esp Enferm Dig 95: 13–21
Chan KC, Wong SKH, Lee DWH, Mui WLM, Chan ACW, Ng EKW, Wu JCY, Sung JJY, Chung SCS (2004) Short-term and long-term results of endoscopic balloon dilation for achalasia: 12 years’ experience. Endoscopy 36: 690–694
Codispoti M, Soon SY, Pugh G, Walker WS (2003) Clinical results of thoracoscopic Heller’s myotomy in the treatment of achalasia. Eur J Cardiothorac Surg 24: 620–624
Davis GE, Schwartz SR, Veenstra DL, Yueh B (2005) Cost comparison of surgery vs organ preservation for laryngeal cancer. Arch Otolaryngol Head Neck Surg 131: 21–26
Devaney EJ, Lannettoni MD, Orringer MB, Marshall B (2001) Esophagectomy for achalasia: patient selection and clinical experience. Ann Thorac Surg 72: 854–858
Dobrucali A, Erzin Y, Tuncer M, Dirican A (2004) Long-term results of graded pneumatic dilatation under endoscopic guidance in patients with primary esophageal achalasia. World J Gastroenterol 10: 3322–3327
Drummond MF, Sculpher MJ, Torrance GW, O’Brien BJ, Stoddart GL (2005) Methods for the economic evaluation of health care programmes. 3rd ed. Oxford University Press Inc., New York, pp 78–88
Eckardt VF, Gockel I, Bernhard G (2004) Pneumatic dilation for achalasia: late results of a prospective follow up investigation. Gut 53: 629–633
Falkenback D, Johansson J, Oberg S, Kjellin A, Wenner J, Zilling T, Johnsson F, Von Holstein CS, Walther B (2003) Heller’s esophagomyotomy with or without a 360 degrees floppy Nissen fundoplication for achalasia. Long-term results from a prospective randomized study. Dis Esophagus 16: 284–290
Gafni A (1991) Willingness-to-pay as a measure of benefits. Relevant questions in the context of public decisionmaking about health care programs. Med Care 29: 1246–1252
Gideon RM, Castell DO, Yarze J (1999) Prospective randomized comparison of pneumatic dilatation technique in patients with idiopathic achalasia. Dig Dis Sci 44: 1853–1857
Gupta R, Sample C, Bamehriz F, Birch D, Anvari M (2005) Long-term outcomes of laparoscopic heller cardiomyotomy without an anti-reflux procedure. Surg Laparosc Endosc Percutan Tech 15: 129–132
Horgan S, Galvani C, Gorodner MV, Omelanczuck P (2005) Robotic-assisted Heller myotomy versus laparoscopic Heller myotomy for the treatment of esophageal achalasia: multicenter study. J Gastrointest Surg 9: 1020–1029
Imperiale TF, O’Connor JB, Vaezi MF, Richter JE (2000) A cost-minimization analysis of alternative treatment strategies for achalasia. Am J Gastroenterol 95: 2737–2745
Janson M, Bjorholt I, Carlsson P, Haglind E, Henriksson M, Lindholm E, Anderberg B (2004) Randomized clinical trial of the costs of open and laparoscopic surgery for colonic cancer. Br J Surg 91: 409–417
Karamanolis G, Sgouros S, Karatzias G, Papadopoulou E, Vasiliadis K, Stefanidis G, Mantides A (2005) Long-term outcome of pneumatic dilation in the treatment of achalasia. Am J Gastroenterol 100: 270–274
Katsinelos P, Kountouras J, Paroutoglou G, Beltsis A, Zavos C, Papaziogas B, Mimidis K (2005) Long-term results of pneumatic dilation for achalasia: A 15 years’ experience. World J Gastroenterol 11: 5701–5705
Khan AA, Shah SW, Alam A, Butt AK, Shafqat F, Castell DO (1998) Pneumatic balloon dilation in achalasia: a prospective comparison of balloon distention time. Am J Gastroenterol 93: 1064–1067
Khan AA, Shah SWH, Alam A, Butt AK, Shafqat F (2005) Sixteen years follow up of achalasia: A prospective study of graded dilatation using Rigiflex ballon. Dis Esophagus 18: 41–45
Lamb PJ, Griffin SM (2006) Achalasia of the cardia: dilatation or division? The case for balloon dilatation. Ann R Coll Surg Engl 88: 9–11
Liu JF, Zhang J, Tian ZQ, Wang QZ, Li BQ, Wang FS, Cao FM, Zhang YF, Li Y, Fan Z, Han JJ, Liu H (2004) Long-term outcome of esophageal myotomy for achalasia. World J Gastroenterol 10: 287–291
Lyass S, Thoman D, Steiner JP, Phillips E (2003) Current status of an antireflux procedure in laparoscopic Heller myotomy. Surg Endosc 17: 554–558
Maher JW (1997) Thoracoscopic esophagomyotomy for achalasia: maximum gain, minimal pain. Surgery 122: 836–840
Mikaeli J, Bishehsari F, Montazeri G, Yaghoobi M, Malekzadeh R (2004) Pneumatic balloon dilatation in achalasia: a prospective comparison of safety and efficacy with different balloon diameters. Aliment Pharmacol Ther 20: 431–436
Miller DL, Allen MS, Trastek VF, Deschamps C, Pairolero PC (1995) Esophageal resection for recurrent achalasia. Ann Thorac Surg 60: 922–925
Muehldorfer SM, Hahn EG, Ell C (1996) High- and low-compliance balloon dilators in patients with achalasia: a randomized prospective comparative trial. Gastrointest Endosc 44: 398–403
Nelson AA, Frassica FJ, Gordon TA, Deune EG (2006) Cost analysis of functional restoration surgery for extremity soft-tissue sarcoma. Plast Reconstr Surg 117:277–283
Neumann P, Johannesson M (1994) The willingness-to-pay for in vitro fertilization: a pilot study using contingent valuation. Med Care 32: 686–699
O’Brien BJ, Gafni A (1996) When do the ‘dollars’ make sense? Toward a conceptual framework for contigent valuation studies in health-care. Med Decis Making 16: 288–299
O’Brien BJ, Goeree R, Gafni A, Torrance GW, Pauly MV, Erder H, Rusthoven J, Weeks J, Cahill M, Lamont B (1998) Assessing the value of a new pharmaceutical: a feasibility study of contingent valuation in managed care. Med Care 36: 370–384
O’Connor J, Singer M, Imperiale T, Vaezi M, Richter J (2002) The cost-effectiveness of treatment strategies for achalasia. Dig Dis Sci 47: 1516–1525
Panaccione R, Gregor JC, Reynolds RP, Preiksaitis HG (1999) Intrasphincteric botulinum toxin versus pneumatic dilatation for achalasia: a cost minimization analysis. Gastrointest Endosc 50: 492–498
Patti MG, Pellegrini CA, Horgan S, Arcerito M, Omelanczuk P, Tamburini A, Diener U, Eubanks TR, Way LW (1999) Minimally invasive surgery for achalasia: an 8-year experience with 168 patients. Ann Surg 230: 587–593
Ramacciato G, D’Angelo FA, Aurello P, Del Gaudio M, Varotti G, Mercantini P, Bellagamba R, Ercolani G (2005) Laparoscopic Heller myotomy with or without partial fundoplication: a matter of debate. World J Gastroenterol 11: 1558–1561
Richards WO, Torquati A, Holzman MD, Khaitan L, Byrne D, Lutfi R, Sharp KW (2004) Heller myotomy versus Heller myotomy with Dor fundoplication for achalasia: a prospective randomized double-blind clinical trial. Ann Surg 240: 405–412
Richardson JD (2005) Management of esophageal perforations: The value of aggressive surgical treatment. Am J Surgery 190: 161–165
Salem L, Jensen CC, Flum DR (2005) Are bariatric surgical outcomes worth their cost? A systematic review. J Am Coll Surg 200: 270–278
Sharp KW, Khaitan L, Scholz S, Holzman MD, Richards WO (2002) 10 Consecutive minimally invasive Heller myotomies: Lessons learned. Ann Surg 235: 631–639
St. Peter SD, Swain JM (2003) Achalasia: A comprehensive review. Surg Laparosc Endosc 4: 227–240
Thoma A, Sprague S, Tandan V (2001) Users’ guide to the surgical literature: how to use an article on economic analysis. Can J Surg 44: 347–354
Vaezi MF, Richter JE, Wilcox CM, Schroeder PL, Birgisson S, Slaughter RL, Koehler RE, Baker ME (1999) Botulinum toxin versus pneumatic dilatation in the treatment of achalasia: a randomised trial. Gut 44: 231–239
Vela MF, Vaezi MF (2003) Cost-assessment of alternative management strategies for achalasia. Expert Opin Pharmacother 4: 2019–2025
Woltman TA, Pellegrini CA, Oelschlager BK (2005) Achalasia. Surg Clin North Am 85: 483–493
Zaninotto G, Annese V, Costantini M, Del Genio A, Costantino M, Epifani M, Gatto G, D’Onofrio V, Benini L, Contini S, Molena D, Battaglia G, Tardio B, Andriulli A, Ancona E (2004) Randomized controlled trial of botulinum toxin versus laparoscopic heller myotomy for esophageal achalasia. Ann Surg 239: 364–370
Zerbib F, Thetiot V, Richy F, Benajah DA, Message L, Lamouliatte H (2006) Repeated pneumatic dilations as long-term maintenance therapy for esophageal achalasia. Am J Gastroenterol 101: 692–697
Acknowledgements
We would like to express our thanks to Dr. John Miller and Dr. William Paterson for providing additional expert opinions, and Randy Welch for extracting LHSC cost data. Dr. Karanicolas holds a Canada Graduate Scholarship from the Canadian Institutes of Health Research.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Karanicolas, P.J., Smith, S.E., Inculet, R.I. et al. The cost of laparoscopic myotomy versus pneumatic dilatation for esophageal achalasia. Surg Endosc 21, 1198–1206 (2007). https://doi.org/10.1007/s00464-007-9364-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-007-9364-z