Abstract
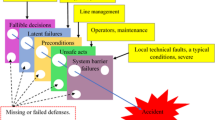
Technical operative errors cause surgical operative morbidity and adversely affect the clinical outcome of patients. Surgical proficiency thus underpins good and safe practice. In this context, standardization of endoscopic surgical operations and their execution are essential for the procurement and maintenance of quality assurance in endoscopic surgical practice. There is no clash between individual- (surgical proficiency) and system-based defense systems in the prevention of surgical errors — both underpin safe surgical practice. Although more human factors and surgical research are needed, it is possible to formulate and adopt a surgical error reduction system for endoscopic operations based on standardization of operations, surgical operative proficiency, and human reliability assessment and its related clinical counterpart, observational clinical human reliability assessment.
Similar content being viewed by others
References
Archer SB, Brown DW, Smith CD (2001) Bile duct injury during LC: results of a national survey Ann Surg 234: 776–777
Billings CE, Woods DD (2001) Human error in perspective. The patient safety movement Postgrad Med 109: 13–17
Brown SI, Frank TG, Cuschieri A, Sharpe R, Cartwright C (2003) Optimization of the projection screening a display system for minimal access surgery Surg Endosc 17: 1252–1255
Campbell PA, Creswell AB, Frank TG, Cuschieri A (2003) Real-time thermography during vessel sealing and dissection Surg Endosc 17: 1640–1645
Cooper MJ, Reid GD, Kaloo P (2002) Respiratory symptoms as an indication of undiagnosed bowel perforation following laparoscopic surgery: an observation Aust N Z Obstet Gynaecol 42: 545–547
Csendes A, Navarrette C, Burdeles P, et al. (2001) Treatment of common bile duct injuries during LC: endoscopic and surgical management World J Surg 25: 1346–1351
Cuschieri A, (2000) Human reliability assessment in surgery—a new approach for improving surgical performance and clinical outcome Ann R Coll Surg Engl 82: 83–87
Cuschieri A, (2003) Medical errors, incidents, accidents and violations Min Invas Ther Allied Technol 12: 111–120
Cuschieri A, (2003) Lest we forget the surgeon Sem Laparosc Surg 10: 141–148
Doganay M, Kama NA, Rees E, et al. (2002) Management of main bile duct injuries that occur during LC Surg Endosc 16: 2
Dondrin Y, Gopher D, Olin M, et al. (1995) A look into the nature and causes of human errors in the intensive care unit Crit Care Med 23: 294–300
Embrey DE (1986) SHERPA: a systematic error reduction and predictive approach. Proceedings of the Advances in Human Factors in Nuclear Power Systems meeting, Knoxville, TN, USA
Ferriman A, (2000) Two thirds of injuries initially missed Br Med J 321: 784
Haag R, Cuschieri A (1993) Recent advances in high-frequency electrosurgery: development of automated systems J R Coll Surg Edinburgh 38: 354–364
Hanna GB, Shimi SM, Cuschieri A (1988) Task performance in endoscopic surgery is influenced by location of image display Ann Surg 227:484
Hjelmqvist (2000) Complications of laparoscopic cholecystectomy as recorded in the Swedish Laparoscopic Registry. Eur J Surg Suppl 585: 18–21
Kennedy A, Baccino T (1995) The effects of screen refresh rate on editing operations using a computer mouse pointing device Q J Exp Psychol 48A: 55–71
Kennedy A, Murray WS (1996) Eye movement control during the inspection of words under conditions of pulsating illumination Eur J Cogn Psychol 8: 381–403
Kohn LT, Coorigan JM, Donaldson MS (eds) (1999) To err is human: building a safer heath system. National Academy Press, Washington DC
Morgenstern L, (1995) Achilles’ heel and laparoscopic surgery Surg Endosc 9: 383
Orlando R, Lirassi F (2000) Delayed recognition of inadvertent gut injury during laparoscopy Surg Endosc 14: 1188
Putcha RV, Burdick JS (2003) Management of iatrogenic perforation Gastroenterol Clin North Am 32: 1289–1309
Rasmussen J, (1983) Skill, rules and knowledge; signals, signs, and symbols, and other distinction in human performance models IEEE Trans Systems Man Cybernetics SMC 13: 257–266
Reason J (1990) Human error. Cambridge University Press, New York
Reason J, (2000) Human error: models and management Br Med J 30: 768–770
Savader S, Lillemoe K, Prescott C, et al. (1997) Laparoscopic cholecystectomy related bile duct injuries. A health and financial disater Ann Surg 225: 268–273
Tang B, Hanna GB, Bax NMA, Cuschieri A (2004) Analysis of technical surgical errors during initial experience of laparoscopic pyloromyotomy by a group of Dutch pediatric surgeons. Surg Endosc, online 26 Oct, 10.1007/s00464-004-8100-1
Tang B, Hanna GB, Joice P, Cuschieri A (2004) Identification and categorization of technical errors by observational clinical human reliability assessment (OCHRA) during laparoscopic cholecystectomy Arch Surg 139: 1215–1220
Tarek AE, Cuschieri A (2003) How safe is high-power ultrasonic dissection? Ann Surg 237: 186–191
Vilas GA, (2000) Laparoscopic bowel injuries: forty ligated gynaecological cases in Canada J Obstet Gynecol Can 24: 224–230
Wade NJ, (1996) Frames of reference in vision Min Invas Ther Allied Technol 5: 435–439
Way LW, Stewart L, Gantert W, et al. (2003) Causes and prevention of laparoscopic bile duct injuries: analysis of 252 cases from a human factors and cognitive psychology perspective Ann Surg 237: 460–469
Author information
Authors and Affiliations
Corresponding author
Additional information
These are some patients whom we cannot help, there are none whom we cannot harm. —Arthur L. Bloomfield (1888–1962)
Rights and permissions
About this article
Cite this article
Cuschieri, A. Reducing errors in the operating room. Surg Endosc 19, 1022–1027 (2005). https://doi.org/10.1007/s00464-005-8110-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-005-8110-7