Abstract
Coughing is an essential airway protective reflex. In healthy young adults, cough somatosensation changes when attention is divided (dual tasking). Whether the same is true in populations at risk of aspiration remains unknown. We present findings from a controlled study testing the effects of divided attention (via a dual-task paradigm) on measures of reflex cough in Parkinson’s disease. Volunteers with Parkinson’s disease (n = 14, age = 43–79 years) and 14 age-matched controls underwent five blocks of capsaicin-induced cough challenges. Within each block, capsaicin ranging from 0 to 200 μM was presented in a randomized order. Two blocks consisted of cough testing only (single task), and two blocks consisted of cough testing with simultaneous tone counting (dual task). Finally, participants completed a suppressed cough task. Measures of cough motor response, self-reported urge to cough, cough frequency, and cough airflow were collected. Historical data from healthy young adults was included for comparison. Between-group analyses revealed no differences between single- and dual-cough-task responses. However, post hoc analysis revealed a significant relationship between dual-task errors and cough frequency that was strongest in people with Parkinson’s disease [p = 0.004, r2 = 0.52]. Specifically, greater errors were associated with fewer reflexive coughs. Unlike healthy participants, participants with Parkinson’s disease did not change the number of coughs between the single-, dual-, and suppressed-task conditions [p > 0.05]. When distracted, people with Parkinson’s disease may prioritize coughing differently than healthy controls. Abnormal cortical resource allocation may be a mechanism involved in aspiration in this population.
Access this article
We’re sorry, something doesn't seem to be working properly.
Please try refreshing the page. If that doesn't work, please contact support so we can address the problem.

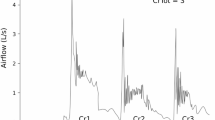
Copyright 2019 by the American Speech-Language-Hearing Association. Reprinted with permission

Copyright 2019 by the American Speech-Language-Hearing Association. Reprinted with permission






Similar content being viewed by others
References
Fernandez HH, Lapane KL. Predictors of mortality among nursing home residents with a diagnosis of Parkinson’s disease. Med Sci Monit. 2002;8(4):CR241–R246.
Singer RB. Mortality in patients with Parkinson’s disease treated with dopa. J Insur Med. 1992;24(2):126–7.
Fall P, Saleh A, Fredrickson M, Olsson J, Granerus A. Survival time, mortality, and cause of death in elderly patients with Parkinson’s disease. Mov Disord. 2003;18(11):1312–6.
D’Amelio M, et al. Long-term survival of Parkinson’s disease: a population-based study. J Neurol. 2006;253(1):33–7.
Robbins J, et al. Comparison of 2 interventions for liquid aspiration on pneumonia incidence: a randomized trial. Ann Intern Med. 2008;148(7):509–18.
Logemann JA, et al. A randomized study of three interventions for aspiration of thin liquids in patients with dementia or Parkinson’s disease. J Speech Lang Hear Res. 2008;51(1):173–83.
Brodsky MB, Abbott KV, McNeil MR, Palmer CV, Grayhack JP, Martin-Harris B. Effects of divided attention on swallowing in persons with idiopathic Parkinson’s disease. Dysphagia. 2012;27(3):390–400.
Troche MS, Okun MS, Rosenbek JC, Altmann LJ, Sapienza CM. Attentional resource allocation and swallowing safety in Parkinson’s disease: a dual task study. Park Relat Disord. 2014;20(4):439–43.
Penko AL, et al. Dual-task interference disrupts parkinson’s gait across multiple cognitive domains. Neuroscience. 2018;379:375–82.
O’Shea S, Morris ME, Iansek R. Dual task interference during gait in people With Parkinson disease: effects of motor versus cognitive secondary tasks. Phys Ther. 2002;82(9):888–97.
Camicioli R, Oken B, Sexton G, Kaye J, Nutt J. Verbal fluency task affects gait in Parkinson’s disease with motor freezing. J Geriatr Psychiatry Neurol. 1998;11(4):181–5.
Morris ME, Iansek R, Matyas T, Summers J. Stride length regulation in Parkinson’s disease: normalization strategies and underlying mechanisms. Brain. 1996;119:551–68.
Behrman A, Teitelbaum P, Cauraugh J. Verbal instructional sets to normalise the temporal and spatial gait variables in Parkinson’s disease. J Neurol Neurosurg Psychiatry. 1998;65:580–2.
Gao L, Zhang J, Hou Y, Hallett M, Chan P, Wu T. The cerebellum in dual-task performance in Parkinson’s disease. Sci Rep. 2017;7:1–11.
Kim Y, Oh B-M, Jung I-Y, Lee JC, Lee GJ, Han TR. Spatiotemporal characteristics of swallowing in Parkinson’s disease. Laryngoscope. 2015;125(2):389–95.
Han M, et al. Relationship between dysphagia and depressive states in patients with Parkinson’s disease. Park Relat Disord. 2011;17(6):437–9.
Mamolar Andrés S, Santamarina Rabanal M, Granda Membriela C, Fernández Gutiérrez M, Sirgo Rodríguez P, Álvarez Marcos C. Swallowing disorders in Parkinson’s disease. Acta Otorinolaryngol Española. 2017;68:15–22.
Chou KL, Evatt M, Hinson V, Kompoliti K. Sialorrhea in Parkinson’s disease: a review. Mov Disord. 2007;22(16):2306–13.
Rodrigues B, Nóbrega AC, Sampaio M, Argolo N, Melo A. Silent saliva aspiration in Parkinson’s disease. Mov Disord. 2010;26(1):138–41.
Hegland KW, Okun MS, Troche MS. Sequential voluntary cough and aspiration or aspiration risk in Parkinson’s disease. Lung. 2014;192(4):601–8.
Janssens T, Silva M, Davenport PW, Van Diest I, Dupont LJ, Van Den Bergh O. Attentional modulation of reflex cough. Chest. 2014;146(1):135–41.
Perry SE, Troche MS. Dual tasking influences cough sensorimotor outcomes in healthy young adults. J Speech Lang Hear Res. 2019;62(9):3596–606.
Troche MS, Brandimore AE, Godoy J, Hegland K. A framework for understanding shared substrates of airway protection. J Appl Oral Sci. 2014;22(4):251–60.
Davenport PW. Urge-to-cough: what can it teach us about cough? Lung. 2008;186(SUPPL. 1):107–11.
Beck A, Ward C, Mendelsohn M, Mock J, Erbaugh J. An inventory for measuring depression. Arch Gen Psychiatry. 1961;4:561–71.
Nasreddine Z, et al. The Montreal Cognitive Assessment, MoCA: a brief screening tool for mild cognitive impairment. J Am Geriatr Soc. 2005;53(4):695–9.
Julayanont P, Brousseau M, Chertkow H, Phillips N, Nasreddine ZS. Montreal Cognitive Assessment Memory Index Score (MoCA-MIS) as a predictor of conversion from mild cognitive impairment to Alzheimer’s disease. J Am Geriatr Soc. 2014;62(4):679–84.
Jensen AR. Scoring the Stroop test. Acta Psychol (Amst). 1965;24:398–408.
Werheid K, Hoppe C, Thone A, Muller U, Mungersdorf M, von Cramon D. The Adaptive Digit Ordering Test: clinical application, reliability, and validity of a verbal working memory test. Arch Clin Neuropsychol. 2002;17(6):547–65.
Lezak M, Howieson D, Loring D. Neuropsychological assessment. 4th ed. New York: Oxford University Press; 2004.
Vovk A, et al. Capsaicin exposure elicits complex airway defensive motor patterns in normal humans in a concentration-dependent manner. Pulm Pharmacol Ther. 2007;20(4):423–32.
Pecova R, Javorkova N, Kudlicka J, Tatar M. Tussigenic agents in the measurement of cough reflex sensitivity. J Physiol Pharmacol. 2007;58(Suppl 5):531–8.
Davenport PW, Vovk A. Cortical and subcortical central neural pathways in respiratory sensations. Respir Physiol Neurobiol. 2009;167(1):72–86.
Morice A, Higgins K, Yeo W. Adaptation of cough reflex with different types of stimulation. Eur Respir J. 1992;5(10):1296–7.
Davenport PW. Clinical cough I: the urge-to-cough: a respiratory sensation. Handb Exp Pharmacol. 2009;187:263–76.
Portney L, Watkins M. Foundations of clinical research: applications to practice. New Jersey: Prentice Hall; 2000.
Brandimore AE, Troche MS, Hegland KW. The influence of age on perception of the urge-to-cough in healthy older adults. Biol Psychol. 2017;129(2017):380.
Schaefer S, Schumacher V. The interplay between cognitive and motor functioning in healthy older adults: findings from dual-task studies and suggestions for intervention. Gerontology. 2011;57(3):239–46.
Plummer-D’Amato P, Altmann L, Saracino D, Fox E, Behrman A, Marsiskef M. Interactions between cognitive tasks and gait after stroke: a dual task study. Gait Posture. 2008;27(4):683–8.
Patel P, Bhatt T. Attentional demands of perturbation evoked compensatory stepping responses: examining cognitive-motor interference to large magnitude forward pertubations. J Mot Behav. 2015;47(3):201–10.
Janssens T, Brepoels S, Dupont L, Van den Bergh O. The impact of harmfulness information on citric acid induced cough and urge-to-cough. Pulm Pharmacol Ther. 2015;31:9–14.
Mosier KM, Liu WC, Maldjian JA, Shah R, Modi B. Lateralization of cortical function in swallowing: a functional MR imaging study. Am J Neuroradiol. 1999;20(8):1520–6.
Hamdy S, et al. Cortical activation during human volitional swallowing: an event-related fMRI study. Am J Physiol. 1999;277:G219–25.
Farrell MJ, Cole LJ, Chiapoco D, Egan GF, Mazzone SB. Neural correlates coding stimulus level and perception of capsaicin-evoked urge-to-cough in humans. Neuroimage. 2012;61(4):1324–35.
Malandraki G, Johnson S, Robbins J. Functional MRI of swallowing: from neurophysiology to neuroplasticity. Head Neck. 2011;33:S14-20.
Malandraki GA, Sutton BP, Perlman AL, Karampinos DC, Conway C. Neural activation of swallowing and swallowing-related tasks in healthy young adults: an attempt to separate the components of deglutition. Hum Brain Mapp. 2009;30(10):3209–26.
Martin RE, Macintosh BJ, Smith RC, Barr AM, Stevens TK, Gati JS. Cerebral areas processing swallowing and tongue movement are overlapping but distinct: a functional magnetic resonance imaging study. J Neurophysiol. 2004;92(4):2428–43.
Martin RE, Goodyear BG, Gati JS, Menon RS. Cerebral cortical representation of automatic and volitional swallowing in humans. J Neurophysiol. 2001;85(2):938–50.
Simonyan K, Saad ZS, Loucks TMJ, Poletto CJ, Ludlow CL. Functional neuroanatomy of human voluntary cough and sniff production. Neuroimage. 2007;37(2):401–9.
Nieuwhof F, et al. Impaired dual tasking in Parkinson’s disease is associated with reduced focusing of cortico-striatal activity. Brain. 2017;140(5):1384–98.
Tombu M, Jolicoæur P. A central capacity sharing model of dual-task performance. J Exp Psychol Hum Percept Perform. 2003;29(1):3–18.
Paas F. Training strategies for attaining transfer of problem-solving skill in statistics: a cognitive load approach. J Educ Psychol. 1992;84(4):429–34.
Langmore S, et al. Predictors of aspiration pneumonia: how important is dysphagia? Dysphagia. 1998;13(2):69–81.
Ebihara S, et al. Impaired efficacy of cough in patients with Parkinson disease. Chest. 2003;124(3):1009–15.
Reilly CA, Johansen ME, Lanza DL, Lee J, Lim J-O, Yost G. Calcium-dependent and independent mechanisms of capsaicin receptor (TRPV1)-mediated cytokine production and cell death in human bronchial epithelial cells. J Biochem Mol Toxicol. 2005;19(4):266–75.
Reilly CA, Taylor JL, Lanza DL, Carr BA, Crouch DJ, Yost G. Capsaicinoids cause inflammation and epithelial cell death through activation of vanilloid receptors. Toxicol Sci. 2003;73(1):170–81.
Morice A, et al. ERS guidelines on the assessment of cough. Eur Respir J. 2007;29(6):1256–76.
Carleton R, Abrams M, Asmundson G. The Attentional Resource Allocation Scale (ARAS): psychometric properties of a composite measure for dissociation and absorption. Depress Anxiety. 2010;27(8):775–86.
Robertson I, Ward T, Ridgeway V, Nimmo-Smith I. The structure of normal human attention: the test of everyday attention. J Int Neuropsychol Soc. 1996;2(6):525–34.
Funding
This study was funded by an ASHFoundation New Investigator’s Research Grant.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
S. Perry and M. Troche confirm that they have no relevant conflicts of interest to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Perry, S.E., Troche, M.S. Dual Tasking Influences Cough Reflex Outcomes in Adults with Parkinson’s Disease: A Controlled Study. Dysphagia 36, 959–973 (2021). https://doi.org/10.1007/s00455-020-10223-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00455-020-10223-x