Abstract
Of all the parasitic diseases, malaria is the number one killer. Despite tremendous efforts in disease control and research, nearly a million people, primarily children, still die from the disease each year, partly due to drug resistance and the lack of an effective vaccine. Many parasite antigens have been identified and evaluated for vaccine development; however, none has been approved for human use. Antigenic variation, complex life cycle, and inadequate understanding of the mechanisms of parasite–host interaction and of host immune response all contribute to the lack of an effective vaccine for malaria control. In a recent search of genome-wide polymorphism in Plasmodium falciparum, several molecules were found to be recognized by sera from patients infected with the P. falciparum parasite. Here, we have expressed a 350-amino acid N terminus from one of the homologous candidate antigen genes from the rodent malaria parasite Plasmodium yoelii (Py01157, a putative dentin phosphorin) in bacteria and evaluated the immune response and protection generated after immunization with the recombinant protein. We showed that the recombinant protein was recognized by sera from both mice and humans infected with malaria parasites. Partial protection was observed after challenge with non-lethal P. yoelii 17XNL but not with the lethal P. yoelii 17XL parasite. Further tests using a full-length protein or the conserved C terminus may provide additional information on whether this protein has the potential for being a malaria vaccine.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Malaria is present in nearly 100 tropical countries. It has been estimated that ∼500 million people are affected by malaria, and ∼one million people die from malaria each year, mostly in sub-Saharan Africa (Feachem et al. 2010; WHO 2008). Many preventive strategies have been employed to control malaria infection including the use of insecticide-treated bed nets, protective clothing, insect repellents, indoor residual insecticide spraying (Pluess et al. 2010), and limited-scale intermittent presumptive treatment with antimalarial drugs (Schellenberg et al. 2006). The success of artemisinin (ART) combination therapy in recent years has prompted discussions of malaria elimination or eradication in the near future (Feachem et al. 2010); however, measures to prevent or impede the appearance of drug-resistant parasites should be considered for such a large-scale use of ART to eliminate malaria parasites in endemic regions because delayed parasite clearance after treatment of ART derivative has been reported (Dondorp et al. 2009; Noedl et al. 2008).
A cost-effective approach for malaria control is to develop a vaccine that can protect against malaria infection or disease, which will greatly benefit hundreds of millions of people by reducing morbidity, mortality, and economic loss and by increasing the pace of social and economic development. Indeed, developing an effective malaria vaccine has been the dream of many scientists. A large number of malaria vaccine candidates have been identified and tested in past decades; unfortunately, no molecular vaccine that can provide complete protection against malaria parasites is currently available, and few have even reached advanced clinical trials (Anders et al. 2010). The most successful recombinant vaccine so far is the RTS,S that is directed to a pre-erythrocytic molecule (Plasmodium falciparum circumsporozoite surface protein [PfCSP]). At its best, RTS,S induced 53% protection against clinical malaria (Alloueche et al. 2003; Bojang et al. 2009; Bojang et al. 2001); extensive phase 3 trials are underway in Africa to confirm this level of efficacy. Recently, there has been increasing interest in testing whole attenuated parasite-based vaccines against malaria; most of these are based on live attenuated P. falciparum sporozoites (Hoffman et al. 2010; Labaied et al. 2007; McCarthy and Good 2010; Roestenberg et al. 2009). The whole-parasite-based vaccine, however, has its own unique challenges in terms of safety, mode of delivery, and difficulties associated with producing sufficient vaccine (Mahajan et al. 2010). Therefore, it remains of critically important to continue to search for and evaluate new malaria vaccine candidates.
Through a genome-wide search for highly polymorphic genes and potential immune targets, we previously identified several putative antigen genes in P. falciparum (Mu et al. 2007). One of these candidate genes, PFI0170w, encodes a hypothetical protein that can be recognized by pooled human immune sera from villagers of Mali, West Africa, but not by non-immune human sera. Because of ethical and other issues associated with testing human malaria vaccines, we decided to first examine the immune response and protection potential of the homologous molecule in a rodent malaria model, Plasmodium yoelii. The P. yoelii homolog of PFI0170w—a gene encoding a ∼140-kDa putative dentin phosphorin (Py01157)—appears to be expressed in asexual and sexual stages of the P. yoelii life cycle (Tarun et al. 2008). Homologous proteins of the PFI0170w are also present in Plasmodium vivax (PVX_098620), Plasmodium knowlesi (PKH_070070), Plasmodium chabaudi chabaudi (PCHAS_041880), and Plasmodium berghei ANKA (PBANKA_041790) with the N- and C-terminal segments being relatively well conserved (www.PlasmoDB.org) (Fig. 1), suggesting an important molecule for the Plasmodium parasites.
Sequence alignment of the N terminus of the homologs of Py01157 from five Plasmodium species. PVX_098620 is the sequence from P. vivax; PFI0170w, from P. falciparum; PKH_070070, from P. knowlesi; PCHAS_041880, from P. chabaudi chabaudi; and Py01157, from P. yoelii yoelii. The P. y. yoelii sequence is the segment expressed in bacteria for this study. The four substitutions between Py17XL and Py17XNL are highlighted in bold, with amino acids from Py17XL shown under the sequence of Py17XNL. The protein sequences were downloaded from PlasmoDB (www.PlasmoDB.org), except those from P. yoelii 17XL and P. yoelii 17XNL, which were sequenced in our laboratory. The full sequences of these genes can be found at PlasmoDB
To further evaluate the protein for a potential vaccine, we cloned and expressed in bacteria 350 residues from the N-terminal of the Py01157 as a recombinant protein (rPy01157-NT) and used the protein to immunize mice. We showed that the recombinant peptide could induce partial protection against a non-lethal P. yoelii parasite (Py17XNL) infection but not the lethal (Py17XL) parasite.
Materials and methods
Cloning of partial Py01157 sequence from P. yoelii cDNA
Infected red blood cells (iRBCs) were collected from Py17XL-infected BALB/c mice when parasitemia was approximately 20%. After lysis of erythrocytes with 0.01% saponin, the P. yoelii parasites were collected for RNA extraction. RNA was isolated using Trizol reagent (Invitrogen, USA), and cDNA was synthesized using the Thermoscript RT-PCR system kit (Invitrogen). The DNA sequence encoding the N-terminal 350 amino acids of Py01157 was PCR amplified from cDNA using specific primers: py01157-Nt forward (5′-catggatccgat gaataacaatggaggga-3′ with a BamH1 restriction site) and py01157-Nt reverse (5′-catctcgag aaatgaattaaagccaccac-3′ with a XhoI restriction site). After amplification, PCR products were digested with the restriction enzymes BamH1 and XhoI and cloned into plasmid vector pET32a (Invitrogen). Plasmids containing inserts were purified and sequenced to verify correct coding sequence and reading frame. We also attempted to clone a longer segment in bacteria without success (data not shown).
Expression and purification of recombinant protein
Recombinant plasmids were used to transform Escherichia coli (strain BL21; New England Biolabs, USA). Bacteria with the plasmid from an overnight culture were diluted (1:100) and grown to an optical density (OD) of 1 OD in the presence of 50 μg/ml ampicillin. Expression of recombinant protein rPy01157-NT-trxA (with a 109-amino acid [aa] trxA tag) was induced at 37°C by addition of 0.1 mM isopropyl-β-d-thiogalactoside (IPTG) for 5 h. The plasmid-encoded trxA tag of a thioredoxin protein plus six histidine residues was fused to its N terminus, producing a protein of approximately 52 kDa (466 aa). Pellets of induced bacterial cultures were resuspended in phosphate-buffered saline (PBS) and lysed by sonication. The rPy01157-NT-trxA fusion protein was produced and purified in insoluble inclusion bodies. The inclusion bodies were washed three times with PBS and dissolved in PBS containing 8 M urea. The denatured rPy01157-NT-trxA was purified using nickel-chelate affinity chromatography in the presence of 8 M urea according to instructions from the manufacturer (Qiagen, USA). After washing three times with washing buffer, the protein was eluted and dialyzed in PBS containing 6 M urea, followed by dialysis in PBS containing 4 M urea, 2 M urea, and 0 M urea. After dialysis, the precipitated protein was removed by centrifugation. The concentrations of the soluble protein fraction were determined using the BCA protein assay kit (Thermo, USA), and the purity of the protein was assessed using Coomassie blue staining following sodium dodecyl sulfate-polyacrylamide gel electrophoresis (SDS-PAGE) and western blot. Endotoxin levels were monitored using a chromogenic Limulus amebocyte lysate assay (Lindsay et al. 1989). Endotoxin levels were less than 2.5 endotoxin units per milligram of purified recombinant protein.
Western blot
The rPy01157-NT-trxA was dissolved in 1× sample loading buffer containing 0.5 M Tris–HCl (pH 6.8), 4.4% (w/v) SDS, 20% (v/v) glycerol, 2% (v/v) 2-mercaptoethanol, and 0.1% (w/v) bromophenol blue in deionized water and was further denatured by placing the proteins in boiling water for 10 min. SDS-PAGE gels were run under 180 V until the tracking dye reached the bottom of the gel. The proteins were transferred to a nitrocellulose membrane (Bio-Rad, USA), and the membrane was blocked with blocking buffer (5% skim milk in 1× PBS 0.05% Tween-20) for 2 h at room temperature (RT). The membrane was probed with sera from mice immunized with recombinant protein, sera from mice challenged with Py17XNL and Py17XL, human immune sera from villagers of Mali, or normal human sera from American volunteers. Sera were diluted appropriately and incubated with the membrane at RT for 2 h. After washing three times with washing buffer, the membrane was again incubated with goat anti-mouse IgG (R&D Systems, USA) or goat anti-rabbit IgG conjugated with horseradish peroxidase at RT for 1 h. The membrane was washed five times in washing buffer (10× solution contains 1.37 M sodium chloride, 0.027 M potassium chloride, and 0.25 M Tris/Tris–HCl) and developed in SuperSignal West Pico chemiluminescent substrate (Thermo, USA).
Immunization, antibody production, and parasite challenge
Five groups of five 4- to 6-week-old BALB/c mice (for challenges with Py17XL and Py17XNL, respectively) were immunized subcutaneously at three sites with 30 μg of rPy01157-NT-trxA. Identical numbers of mice were immunized with the same molar concentration of trxA protein as controls. The recombinant proteins were administered with complete Freund’s adjuvant (Sigma, USA) for the initial immunization; the second and third immunizations were given in incomplete Freund’s adjuvant (Sigma) at 3-week intervals. Sera were collected before the first immunization (pre-immune sera) and 2 weeks after the third immunization; at the latter time, the mice were infected intravenously with different doses of Py17XL or Py17XNL parasites. Blood smears were prepared daily post-infection. Parasitemia was determined microscopically by counting percentage of parasitized erythrocytes in 1,000 RBCs. Mice experiments were done in compliance with the Institutional Animal Care and Use Committee of the NIAID/NIH (protocol LMVR 10E) or with the approved protocol at Xiamen University in China. Pooled human sera were obtained from adult volunteers in Kenieroba, a malaria-endemic village in Mali, West Africa, or healthy adults in the USA (for control). The study was approved by the ethical review committees of the Faculty of Medicine, Pharmacy, and Dentistry at the University of Bamako (Mali) and the NIAID, National Institutes of Health (Bethesda, MD). Individual written informed consent was obtained from all participants, and the study was externally monitored for protocol compliance, data integrity, and protection of human subjects.
Indirect immunofluorescence assay
Parasitized blood samples were collected from mice infected with Py17XL when parasitemia reached 15% to 20%. Erythrocytes were pelleted by centrifugation for 10 min at 800×g and washed five times in PBS. The final pellet was suspended in an equal volume of PBS. Thin blood smears were prepared, air dried, and fixed in 4% formaldehyde for 30 min at RT. The fixed slides were permeabilized by incubation with 0.1% Triton X-100 for 10 min at RT. To reduce nonspecific binding, the slides were blocked with 3% BSA in PBS overnight at 4°C. Then, the slides were incubated with mouse anti-rPy01157-NT-trxA or anti-trxA sera for 2 h at RT. Primary antibody was detected using Alexa Fluor 488-conjugated goat anti-mouse IgG (Invitrogen). Following three washes, the slides were mounted with ProLong Gold anti-fade reagent with 4′,6-diamidino-2-phenylindole (DAPI, Invitrogen). Fluorescence was visualized using Leica SP2 confocal microscopy.
Results
Expression and purification of recombinant Py01157 protein
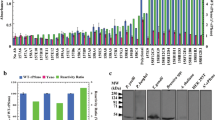
We cloned and sequenced the cDNA sequence encoding 350-aa N-terminal of Py01157 (Py01157-NT) from both Py17XL and Py17XNL parasites. Direct sequencing of PCR products showed that there were four aa differences between these two strains; all of the four substituted aa in the Py17XNL are also present in other Plasmodium species (Fig. 1). We next expressed the Py01157-NT protein from Py17XL parasite in E. coli. A recombinant protein with expected molecular weight (∼52 kDa), mostly expressed in inclusion bodies, was obtained (Fig. 2, lane 2). The recombinant protein contained a trxA Tag protein fused to its N terminus that was designed to increase the stability and solubility of the recombinant protein. The trxA tag protein contains a six-residue histidine tag for protein purification. The protein in inclusion bodies was first washed, dissolved in 8 M urea, purified using nickel-chelate affinity chromatography (Fig. 2, lane 3), and refolded after gradient dialysis. The leader sequence of the fusion protein was also expressed and purified (Fig. 2, lane 4).
The recombinant PY01157-NT protein is recognized by mouse and human immune sera
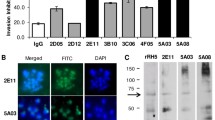
To determine whether Py01157 protein is a host immune-response target during P. yoelii infection, we collected immune sera from mice recovered from Py17XNL infection and used the immune sera to detect the rPy01157-NT-trxA protein on western blot. The results showed that sera from mice recovered from Py17XNL infection could recognize the rPy01157-NT-trxA protein, while no reactive band was observed with control sera from naïve mice (Fig. 3a). Additionally, we immunized the BALB/c mice with rPy01157-NT-trxA and trxA tag proteins to generate polyclonal antibodies against the protein and used the antibodies to detect the protein in the Py17XL parasite extract. Polyclonal antibodies against rPy01157-NT-trxA could recognize the native Py01157 protein, with a band of the expected size (∼140 kDa) as well as a smaller band of approximately 55 kDa that may represent a cross reactive protein, because the 55-kDa band was also present in the lane probed with anti-trxA tag (Fig. 3b). These results show that the Py01157 protein is the target of host immune response and that antibodies against the recombinant protein can recognize the native parasite protein. The results also suggest that the rPy01157-NT is immunogenic and has similar epitopes to the native Py01157 protein. Furthermore, we used sera from African volunteers infected with malaria parasites to detect the rPy01157-NT-trxA protein and showed that rPy01157-NT-trxA was also recognized by pooled human immune sera but not by non-immune human sera (Fig. 3c). The exposed human sera did not recognize the trxA tag, suggesting that the protein band recognized by the sera was specific for the rPy01157-NT. The results also suggest that there are some epitopes conserved in the proteins from mouse and human malaria parasites.
Western blots showing polyclonal antibodies recognizing both native and recombinant Py01157 protein. a Sera from mice recovered from Py17XNL infection recognize the recombinant Py01157 protein (lane 2) but not sera from naïve mice (lane 1). M designates molecular weight markers. b Antibodies from mice immunized with rPy01157-NT-trxA recognize a protein band of ∼140 kDa in the parasite lysate (lane 2, arrow) but not with sera against the trxA tag protein (lane 1). c rPy01157-NT-trxA protein (lane 1 and lane 3) and TrxA (lane 2 and lane 4) probed with pooled human sera infected with P. falciparum (lane 1 and lane 2) or with normal non-infected sera (lane 3 and lane 4). Molecular weights are as marked
Localization of Py01157 within parasite cells
The expression and localization of Py01157 parasitized erythrocytes was investigated using indirect immunofluorescence assay (IFA). Thin blood films of P. yoelii 17XL blood-stage parasites were prepared and detected with polyclonal mouse sera raised against rPy01157NT-trxA protein. A punctate pattern of fluorescence was observed within the parasite and the iRBCs. No fluorescence of P. yoelii-parasitized erythrocytes incubated with polyclonal mouse serum against the trxA protein tag was observed (Fig. 4). It appears that the protein is expressed in both asexual and sexual stages, with some staining in the cytoplasm of red blood cells infected with trophozoite (Fig. 4).
Indirect immunofluorescence assay staining of P. yoelii 17XNL parasites within red blood cells. BF bright field, DAPI 4′,6-diamidino-2-phenylindole staining parasite nucleus, AF488 anti-Py01157-NT-trxA indirectly labeled with AF488, Merged 1 overlay images of DAPI and AF488, Merged 2 overlay of BF and Merged 1. The parasite stages are as labeled. The gametocyte is determined based on the presence of large pigments and single nucleus, and a schizont has multiple nuclei. No staining was observed using antibodies against trxA protein tag (bottom panels)
Partial protection after immunization of mice with rPy01157NT-trxA
To evaluate the potential of Py01157-NT as a vaccine, five groups of five mice each were immunized with 30 μg rPy01157-NT-trxA proteins formulated with Freund’s adjuvants as described in “Materials and methods.” Another five groups of five mice each was immunized with the same molar amount of the trxA protein as controls. Two weeks after the third immunization, the mice were infected with 5 × 103, 104, and 106 parasites of Py17XL and Py17XNL (the 5 × 103 group was done with Py17XL only). For the mice challenged with 106 Py17XNL parasites, three of the five mice immunized with rPy01157-NT-trxA recovered completely, while only one of four (one died before challenge) survived in the mice immunized with trxA. The peak parasitemia of the mice immunized with rPy01157-NT-trxA and challenged with Py17XNL was also generally lower than that of those immunized with trixA tag controls (Fig. 5). For low-dose (104) challenge with Py17XNL, the protective effects were more obvious. The mice immunized with rPy01157-NT-trxA had significantly lower peak parasitemia (P < 0.001; paired t test) during the course of infection (Fig. 5c, d). All five mice immunized with rPy01157-NT-TrixA survived, whereas three of the five mice immunized with trxA died.
Partial protection for mice immunized with rPy01157-NT-trxA after challenge with P. yoelii 17XNL. a, b BALB/c mice challenged with 106 Py17XNL parasites after immunization with rPy01157-NT-trxA (a) or with trxA (b). c, d Mice challenged with 104 P. yoelii after immunization with rPy01157-NT-trxA (c) or with trxA (d). Parasitemia is the percentage of red blood cells infected with parasites, obtained after counting 1,000 cells in Giemsa-stained smears. Each color line represents parasitemia from a single mouse
We also challenged the mice with Py17XL, which usually kills its host within 7 days. No obvious differences were observed in mice immunized with both rPy01157-NT-TrixA and trxA, even with a dose of 5,000 infected RBCs (Fig. 6).
No protection in mice infected with Py17XL lethal parasite after immunization with rPy01157-NT-trxA. BALB/c mice immunized with rPy01157-NT-trxA or trxA were challenged with 106 (a and b), 104 (c and d), or 5 × 103 (e and f) infected red blood cells. Parasitemia was determined daily after infection. Note: the challenges using 104 parasites (c and d) were performed at the National Institutes of Health, USA, using a Py17XL strain that appears to grow faster than the one maintained in China that was used in the other two challenges (a, b) and (e, f)
Discussion
Development of an effective vaccine is obviously the first choice for controlling human malaria. Unfortunately, after decades of extensive research and development, we are still a distance away from having an effective malaria vaccine. Here, we cloned and expressed a segment of a gene encoding a putative P. yoelii dentin phosphorin in bacteria and evaluated the recombinant protein as a potential vaccine, which has not been reported previously. We showed that antibodies generated against the recombinant protein could recognize the native protein in the parasite lysates, and that sera from mice infected with P. yoelii or from human patients infected with P. falciparum could bind to the recombinant protein, suggesting that this protein is an antigen recognized by patient sera. The cross reactivity of the recombinant protein with both mouse and human immune sera also suggests that this protein may stimulate a broad (across strain and species) immune response. Antigenic variation and lack of protection between parasite strains have been among the difficult problems in malaria vaccine development. It would be interesting to investigate the epitopes that induce this cross reactivity.
The homolog of the Py01157 gene was initially identified from the P. falciparum genome by searches of polymorphic genes (Mu et al. 2007) based on the observation that all known malaria antigen genes are highly polymorphic and are mostly under immune selection (Polley et al. 2003; Polley and Conway 2001). However, polymorphic antigens identified using this approach may fail to generate protection against diverse parasite strains in the field due to polymorphic nature of the antigen genes. Candidate vaccine targets identified through polymorphism search therefore require experimental verification. Our study represents the first attempt to test candidate vaccine targets identified using this approach in vivo. Although the Py01157 protein appears to be quite polymorphic between the closely related YM and 17XNL parasites (Li et al. 2011; Pattaradilokrat et al. 2008) (there are four amino acid substitutions in the N terminus), the cross-strain/species antibody recognition suggests the presence of conserved epitope(s) in the protein. The recombinant protein from 17XL generated some protection against 17XNL but did not show any protection against 17XL that had the same sequence as the recombinant protein. The results suggested that the polymorphisms in the region did not interfere with the protective response against 17XNL and the protective epitopes were likely conserved, which is consistent with the observation that serum from human malaria patients could recognize the mouse recombinant protein. Many factors may influence whether an antigen identified using this approach will become an effective vaccine, including the level of protection a vaccine candidate can generate, the diversity of the parasite population to be tested, and our understanding of the mechanisms of immune response and protection.
The protection observed in our study was not very strong, and indeed no protection was found when mice were infected with the fast-growing Py17XL parasite, which causes fulminating and rapidly lethal infections. One possibility that may improve the efficacy of protection is to express a longer segment or even the full protein-coding region, which can be challenging. We attempted to express a longer segment of the protein without success. Expression of the protein in other systems such as yeast or even Tetrahymena that also has a relatively AT-rich genome (Shang et al. 2002) may result in improved protein expression. Other possibilities include codon harmonization by replacing the parasite codons with those favoring expression in bacteria, expressing the conserved C terminus and evaluating the potential for protection, or using a combination of N- and C-terminus segments in immunization.
We also noticed that the Py17XNL in our hands did not behave as a typical Py17XNL parasite, which generally does not kill its host. Mice infected with Py17XNL generally will clear all the parasites in circulation when immunity is fully developed and recover from the disease. The parasite we used appeared to have a virulence level between a typical lethal and a non-lethal strain. Because the immunity generated from the N terminus of the Py01157 was not strong enough to protect mice from infection by a fast-growing parasite such as Py17XL or high doses of a less virulent parasite, measures to improve host immune responses may be necessary in order to protect mice from a lethal challenge. Although our efforts may not eventually lead a successful malaria vaccine, we will not know how good this protein will be until we evaluate all the possibilities.
IFA analysis showed that the protein was expressed in the cytoplasm of trophozoite, schizont, and gametocyte (Fig. 4). The results are consistent with those from microarray analyses showing that the gene was also transcribed in many asexual stages, liver stage, and salivary gland sporozoites (Tarun et al. 2008). The protein also appeared to be present in the cytoplasm of some red blood cells infected with trophozoites, although no obvious signal peptide or protein export domain can be found in the protein sequence. The protein could also be released into the blood stream when a schizont ruptures, exposing to the host immune system. Presence of antibodies in the host blood may also reduce oocyst carriage, which requires further investigations.
Our results clearly show that the Py01157 protein is an antigen recognized by host immune systems. Although only a low level of protection was observed, this study provides preliminary information for further investigation of this antigen as a potential vaccine candidate.
Conclusion
A new malaria protein (Py01157 or putative dentin phosphorin) has been evaluated for its immunogenicity and potential as a vaccine candidate. Although the protection induced after immunization of mice with the recombinant protein was not adequate to protect mice from parasite challenges, our data showed that the protein was recognized by sera from mice recovered from P. yoelii infection and from humans infected with P. falciparum. The potential of this protein as a malaria vaccine candidate should be further investigated using full-length protein and/or the C terminus of the protein.
References
Alloueche A, Milligan P, Conway DJ, Pinder M, Bojang K, Doherty T, Tornieporth N, Cohen J, Greenwood BM (2003) Protective efficacy of the RTS, S/AS02 Plasmodium falciparum malaria vaccine is not strain specific. Am J Trop Med Hyg 68:97–101
Anders RF, Adda CG, Foley M, Norton RS (2010) Recombinant protein vaccines against the asexual blood stages of Plasmodium falciparum. Hum Vaccin 6:39–53
Bojang KA, Milligan PJ, Pinder M, Vigneron L, Alloueche A, Kester KE, Ballou WR, Conway DJ, Reece WH, Gothard P, Yamuah L, Delchambre M, Voss G, Greenwood BM, Hill A, McAdam KP, Tornieporth N, Cohen JD, Doherty T (2001) Efficacy of RTS, S/AS02 malaria vaccine against Plasmodium falciparum infection in semi-immune adult men in The Gambia: a randomised trial. Lancet 358:1927–1934
Bojang K, Milligan P, Pinder M, Doherty T, Leach A, Ofori-Anyinam O, Lievens M, Kester K, Schaecher K, Ballou WR, Cohen J (2009) Five-year safety and immunogenicity of GlaxoSmithKline’s candidate malaria vaccine RTS, S/AS02 following administration to semi-immune adult men living in a malaria-endemic region of The Gambia. Hum Vaccin 5:242–247
Dondorp AM, Nosten F, Yi P, Das D, Phyo AP, Tarning J, Lwin KM, Ariey F, Hanpithakpong W, Lee SJ, Ringwald P, Silamut K, Imwong M, Chotivanich K, Lim P, Herdman T, An SS, Yeung S, Singhasivanon P, Day NP, Lindegardh N, Socheat D, White NJ (2009) Artemisinin resistance in Plasmodium falciparum malaria. N Engl J Med 361:455–467
Feachem RG, Phillips AA, Hwang J, Cotter C, Wielgosz B, Greenwood BM, Sabot O, Rodriguez MH, Abeyasinghe RR, Ghebreyesus TA, Snow RW (2010) Shrinking the malaria map: progress and prospects. Lancet 376:1566–1578
Hoffman SL, Billingsley PF, James E, Richman A, Loyevsky M, Li T, Chakravarty S, Gunasekera A, Chattopadhyay R, Li M, Stafford R, Ahumada A, Epstein JE, Sedegah M, Reyes S, Richie TL, Lyke KE, Edelman R, Laurens MB, Plowe CV, Sim BK (2010) Development of a metabolically active, non-replicating sporozoite vaccine to prevent Plasmodium falciparum malaria. Hum Vaccin 6:97–106
Labaied M, Harupa A, Dumpit RF, Coppens I, Mikolajczak SA, Kappe SH (2007) Plasmodium yoelii sporozoites with simultaneous deletion of P52 and P36 are completely attenuated and confer sterile immunity against infection. Infect Immun 75:3758–3768
Li J, Pattaradilokrat S, Zhu F, Jiang H, Liu S, Hong L, Fu Y, Koo L, Xu W, Pan W, Carlton JM, Kaneko O, Carter R, Wootton JC, Su XZ (2011) Linkage maps from multiple genetic crosses and loci linked to growth-related virulent phenotype in Plasmodium yoelii. Proc Natl Acad Sci USA 108:E374–382.
Lindsay GK, Roslansky PF, Novitsky TJ (1989) Single-step, chromogenic Limulus amebocyte lysate assay for endotoxin. J Clin Microbiol 27:947–951
Mahajan B, Berzofsky JA, Boykins RA, Majam V, Zheng H, Chattopadhyay R, de la Vega P, Moch JK, Haynes JD, Belyakov IM, Nakhasi HL, Kumar S (2010) Multiple antigen peptide vaccines against Plasmodium falciparum malaria. Infect Immun 78:4613–4624
McCarthy JS, Good MF (2010) Whole parasite blood stage malaria vaccines: a convergence of evidence. Hum Vaccin 6:114–123
Mu J, Awadalla P, Duan J, McGee KM, Keebler J, Seydel K, McVean GA, Su X-z (2007) Genome-wide variation and identification of vaccine targets in the Plasmodium falciparum genome. Nat Genet 39:126–130
Noedl H, Se Y, Schaecher K, Smith BL, Socheat D, Fukuda MM (2008) Evidence of artemisinin-resistant malaria in western Cambodia. N Engl J Med 359:2619–2620
Pattaradilokrat S, Cheesman SJ, Carter R (2008) Congenicity and genetic polymorphism in cloned lines derived from a single isolate of a rodent malaria parasite. Mol Biochem Parasitol 157:244–247
Pluess B, Tanser FC, Lengeler C, Sharp BL (2010) Indoor residual spraying for preventing malaria. Cochrane Database Syst Rev CD006657
Polley SD, Conway DJ (2001) Strong diversifying selection on domains of the Plasmodium falciparum apical membrane antigen 1 gene. Genetics 158:1505–1512
Polley SD, Chokejindachai W, Conway DJ (2003) Allele frequency-based analyses robustly map sequence sites under balancing selection in a malaria vaccine candidate antigen. Genetics 165:555–561
Roestenberg M, McCall M, Hopman J, Wiersma J, Luty AJ, van Gemert GJ, van de Vegte-Bolmer M, van Schaijk B, Teelen K, Arens T, Spaarman L, de Mast Q, Roeffen W, Snounou G, Renia L, van der Ven A, Hermsen CC, Sauerwein R (2009) Protection against a malaria challenge by sporozoite inoculation. N Engl J Med 361:468–477
Schellenberg D, Abdulla S, Roper C (2006) Current issues for anti-malarial drugs to control P. falciparum malaria. Curr Mol Med 6:253–260
Shang Y, Song X, Bowen J, Corstanje R, Gao Y, Gaertig J, Gorovsky MA (2002) A robust inducible-repressible promoter greatly facilitates gene knockouts, conditional expression, and overexpression of homologous and heterologous genes in Tetrahymena thermophila. Proc Natl Acad Sci USA 99:3734–3739
Tarun AS, Peng X, Dumpit RF, Ogata Y, Silva-Rivera H, Camargo N, Daly TM, Bergman LW, Kappe SH (2008) A combined transcriptome and proteome survey of malaria parasite liver stages. Proc Natl Acad Sci USA 105:305–310
WHO (2008) Accessed 01 January 2008. World Malaria Report 2008. http://www.who.int/malaria/wmr2008/malaria2008.pdf. Accessed 27 Oct 2009
Acknowledgments
This work is supported by grants from the 973 Program 2007CB513103 of China, the Science Planning Program of Fujian Province (2010J1008), 111 Project of Education of China (no. B06016), and by the Intramural Research Program of the Division of Intramural Research, National Institute of Allergy and Infectious Diseases, National Institutes of Health. We thank NIAID intramural editor Brenda Rae Marshall for assistance.
Conflicts of interest
The authors declare no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhang, Y., Qi, Y., Li, J. et al. A new malaria antigen produces partial protection against Plasmodium yoelii challenge. Parasitol Res 110, 1337–1345 (2012). https://doi.org/10.1007/s00436-011-2630-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00436-011-2630-y