Abstract
Background
A nomogram is a valuable and easily accessible tool for individualizing cancer prognosis. This study aims to establish and validate two prognostic nomograms for long-term overall survival (OS) and cancer‐specific survival (CSS) in non-metastatic nasopharyngeal carcinoma (NPC) patients and to investigate the treatment options for the nomogram-based risk stratification subgroups.
Methods
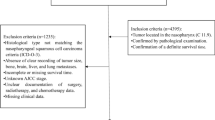
A total of 3959 patients with non-metastatic NPC between 2004 and 2015 were identified from the Surveillance, Epidemiology, and End Results (SEER) database. The patients were randomly allocated to the training and validation cohorts in a 7:3 ratio. Prognostic nomograms were constructed to estimate OS and CSS by integrating significant variables from multivariate Cox regression employing a backward stepwise method. We examined the correlation indices (C-index) and areas under the curves (AUC) of time-dependent receiver operating characteristic curves to assess the discriminative ability of our survival models. The comprehensive enhancements of predictive performance were evaluated with net reclassification operating improvement (NRI) and integrated discrimination improvement (IDI). Reliability was validated using calibration plots. Decision curve analysis (DCA) was used to estimate clinical efficacy and capability. Finally, the nomogram-based risk stratification system used Kaplan–Meier survival analysis and log-rank tests to examine differences between subgroups.
Results
The following independent parameters were significant predictors for OS: sex, age, race, marital status, histological type, median household income, AJCC stage tumor size, and lymph node size. Except for the race variables mentioned above, the rest were independent prognostic factors for CSS. The C-index, AUC, NRI, and IDI indicated satisfactory discriminating properties. The calibration curves exhibited high concordance with the exact outcomes. Moreover, the DCA demonstrated performed well for net benefits. The prognosis significantly differed between low- and high-risk patients (p < 0.001). In a treatment-based stratified survival analysis in risk-stratified subgroups, chemotherapy benefited patients in the high-risk group compared to radiotherapy alone. Radiotherapy only was recommended in the low-risk group.
Conclusions
Our nomograms have satisfactory performance and have been validated. It can assist clinicians in prognosis assessment and individualized treatment of non-metastatic NPC patients.












Similar content being viewed by others
Data availability
SEER is a widely recognized source of cancer statistics in the USA. Researchers can access the data by submitting an authorization request via the official website. On reasonable request, any of the data used in this study can be obtained from the corresponding authors.
Abbreviations
- NPC:
-
Nasopharyngeal carcinoma
- SEER:
-
Surveillance, epidemiology, and end results
- OS:
-
Overall survival
- CSS:
-
Cancer-specific survival
- AUC:
-
The area under the curve
- C-index:
-
Correlation index
- NRI:
-
Net weight classification operational improvement
- IDI:
-
Integrated discrimination improvement
- DCA:
-
Decision curve analysis
- AJCC:
-
American Joint Committee on Cancer
- TNM:
-
Tumor-node-metastasis
- EBV:
-
Epstein–Barr virus
- KSCC:
-
Keratinizing squamous cell carcinoma
- DNKC:
-
Differentiated non-keratinizing carcinoma
- UNKC:
-
Undifferentiated non-keratinizing carcinoma
- CI:
-
Confidence interval
- HR:
-
Hazard ratio
References
Aizer AA, Chen M-H, McCarthy EP et al (2013) Marital status and survival in patients with cancer. J Clin Oncol 31:3869–3876. https://doi.org/10.1200/JCO.2013.49.6489
Brody-Camp S, McCoul ED, Lefante JJ, Aslam R (2021) Socioeconomic status and survival in nasopharyngeal carcinoma: a population-based study. Laryngoscope 131:2719–2723. https://doi.org/10.1002/lary.29702
Chen C, Fei Z, Pan J et al (2011) Significance of primary tumor volume and T-stage on prognosis in nasopharyngeal carcinoma treated with intensity-modulated radiation therapy. Jpn J Clin Oncol 41:537–542. https://doi.org/10.1093/jjco/hyq242
Chen L, Zhang Y, Lai S-Z et al (2019) 10-year results of therapeutic ratio by intensity-modulated radiotherapy versus two-dimensional radiotherapy in patients with nasopharyngeal carcinoma. Oncologist 24:e38–e45. https://doi.org/10.1634/theoncologist.2017-0577
Chen Z-H, Yang K-B, Zhang Y et al (2021) Assessment of modifiable factors for the association of marital status with cancer-specific survival. JAMA Netw Open 4:e2111813. https://doi.org/10.1001/jamanetworkopen.2021.11813
Cheung F, Chan O, Ng WT et al (2012) The prognostic value of histological typing in nasopharyngeal carcinoma. Oral Oncol 48:429–433. https://doi.org/10.1016/j.oraloncology.2011.11.017
Cho J-K, Lee G-J, Yi K-I et al (2015) Development and external validation of nomograms predictive of response to radiation therapy and overall survival in nasopharyngeal cancer patients. Eur J Cancer 51:1303–1311. https://doi.org/10.1016/j.ejca.2015.04.003
Chua MLK, Wee JTS, Hui EP, Chan ATC (2016) Nasopharyngeal carcinoma. Lancet 387:1012–1024. https://doi.org/10.1016/S0140-6736(15)00055-0
Ford JL, Stowe RP (2013) Racial-ethnic differences in Epstein-Barr virus antibody titers among U.S. children and adolescents. Ann Epidemiol 23:275–280. https://doi.org/10.1016/j.annepidem.2013.02.008
Guo R, Wu H, Wang J et al (2019) Lymph node status and outcomes for nasopharyngeal carcinoma according to histological subtypes: a SEER population-based retrospective analysis. Adv Ther 36:3123–3133. https://doi.org/10.1007/s12325-019-01100-7
Hilden J, Gerds TA (2014) A note on the evaluation of novel biomarkers: do not rely on integrated discrimination improvement and net reclassification index. Stat Med 33:3405–3414. https://doi.org/10.1002/sim.5804
Houen G, Trier NH (2020) Epstein-Barr virus and systemic autoimmune diseases. Front Immunol 11:587380. https://doi.org/10.3389/fimmu.2020.587380
Huang S-J, Tang Y-Y, Liu H-M et al (2018a) Impact of age on survival of locoregional nasopharyngeal carcinoma: an analysis of the Surveillance, Epidemiology, and End Results program database, 2004–2013. Clin Otolaryngol 43:1209–1218. https://doi.org/10.1111/coa.13124
Huang X-D, Zhou G-Q, Lv J-W et al (2018b) Competing risk nomograms for nasopharyngeal carcinoma in the intensity-modulated radiotherapy era: a big-data, intelligence platform-based analysis. Radiother Oncol 129:389–395. https://doi.org/10.1016/j.radonc.2018.09.004
Huang C-L, Chen Y, Guo R et al (2020) Prognostic value of MRI-determined cervical lymph node size in nasopharyngeal carcinoma. Cancer Med 9:7100–7106. https://doi.org/10.1002/cam4.3392
Jalbout M, Bel Hadj Jrad B, Bouaouina N et al (2002) Autoantibodies to tubulin are specifically associated with the young age onset of nasopharyngeal carcinoma. Int J Cancer 101:146–150. https://doi.org/10.1002/ijc.10586
Johnson S, McDonald JT, Corsten MJ (2008) Socioeconomic factors in head and neck cancer. J Otolaryngol Head Neck Surg 37:597–601
Lee AWM, Ng WT, Chan JYW et al (2019a) Management of locally recurrent nasopharyngeal carcinoma. Cancer Treat Rev 79:101890. https://doi.org/10.1016/j.ctrv.2019.101890
Lee HM, Okuda KS, González FE, Patel V (2019b) Current perspectives on nasopharyngeal carcinoma. In: Rhim JS, Dritschilo A, Kremer R (eds) Human cell transformation: advances in cell models for the study of cancer and aging. Springer International Publishing, Cham, pp 11–34
Lu Y, Hua J, Yan F et al (2021) Combined radiotherapy and chemotherapy versus radiotherapy alone in elderly patients with nasopharyngeal carcinoma. Medicine (baltimore) 100:e26629. https://doi.org/10.1097/MD.0000000000026629
Ma BBY, Poon TCW, To KF et al (2003) Prognostic significance of tumor angiogenesis, Ki 67, p53 oncoprotein, epidermal growth factor receptor and HER2 receptor protein expression in undifferentiated nasopharyngeal carcinoma? A prospective study. Head Neck 25:864–872. https://doi.org/10.1002/hed.10307
Mao Y-P, Tang L-L, Chen L et al (2016) Prognostic factors and failure patterns in non-metastatic nasopharyngeal carcinoma after intensity-modulated radiotherapy. Chin J Cancer 35:103. https://doi.org/10.1186/s40880-016-0167-2
Moulla Y, Lyros O, Adolf D et al (2018) A nomogram based on clinical factors to predict the serum myoglobin levels following bariatric surgery. Obes Surg 28:1697–1703. https://doi.org/10.1007/s11695-017-3078-7
Müller von der Grün J, Martin D, Stöver T et al (2018) Chemoradiotherapy as definitive treatment for elderly patients with head and neck cancer. Biomed Res Int 2018:3508795. https://doi.org/10.1155/2018/3508795
Ng WT, Yuen KT, Au KH et al (2014) Staging of nasopharyngeal carcinoma: the past, the present and the future. Oral Oncol 50:549–554. https://doi.org/10.1016/j.oraloncology.2013.06.003
Ou S-HI, Zell JA, Ziogas A, Anton-Culver H (2007) Epidemiology of nasopharyngeal carcinoma in the United States: improved survival of Chinese patients within the keratinizing squamous cell carcinoma histology. Ann Oncol 18:29–35. https://doi.org/10.1093/annonc/mdl320
Pagedar NA, Davis AB, Sperry SM et al (2019) Population analysis of socioeconomic status and otolaryngologist distribution on head and neck cancer outcomes. Head Neck 41:1046–1052. https://doi.org/10.1002/hed.25521
Pan Z, You H, Bu Q et al (2019) Development and validation of a nomogram for predicting cancer-specific survival in patients with Wilms’ tumor. J Cancer 10:5299–5305. https://doi.org/10.7150/jca.32741
Pan X-X, Liu Y-J, Yang W et al (2020) Histological subtype remains a prognostic factor for survival in nasopharyngeal carcinoma patients. Laryngoscope 130:E83–E88. https://doi.org/10.1002/lary.28099
Reddy SP, Raslan WF, Gooneratne S et al (1995) Prognostic significance of keratinization in nasopharyngeal carcinoma. Am J Otolaryngol 16:103–108. https://doi.org/10.1016/0196-0709(95)90040-3
Ren Y, Qiu H, Yuan Y et al (2017) Evaluation of 7th edition of AJCC staging system for nasopharyngeal carcinoma. J Cancer 8:1665–1672. https://doi.org/10.7150/jca.19197
Rendall MS, Weden MM, Favreault MM, Waldron H (2011) The protective effect of marriage for survival: a review and update. Demography 48:481–506. https://doi.org/10.1007/s13524-011-0032-5
Richey LM, Olshan AF, George J et al (2006) Incidence and survival rates for young blacks with nasopharyngeal carcinoma in the United States. Arch Otolaryngol-Head Neck Surg 132:1035–1040. https://doi.org/10.1001/archotol.132.10.1035
Roy Chattopadhyay N, Das P, Chatterjee K, Choudhuri T (2017) Higher incidence of nasopharyngeal carcinoma in some regions in the world confers for interplay between genetic factors and external stimuli. Drug Discov Ther 11:170–180. https://doi.org/10.5582/ddt.2017.01030
Sham JS, Choy D, Wei WI (1990) Nasopharyngeal carcinoma: orderly neck node spread. Int J Radiat Oncol Biol Phys 19:929–933. https://doi.org/10.1016/0360-3016(90)90014-b
Sinha S, Gajra A (2022) Nasopharyngeal cancer. StatPearls Publishing
Song W, Lv C-G, Miao D-L et al (2018) Development and validation of a nomogram for predicting survival in patients with gastrointestinal stromal tumours. Eur J Surg Oncol 44:1657–1665. https://doi.org/10.1016/j.ejso.2018.07.004
Sun X, Su S, Chen C et al (2014) Long-term outcomes of intensity-modulated radiotherapy for 868 patients with nasopharyngeal carcinoma: an analysis of survival and treatment toxicities. Radiother Oncol 110:398–403. https://doi.org/10.1016/j.radonc.2013.10.020
Sung H, Ferlay J, Siegel RL et al (2021) Global Cancer Statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. Cancer J Clin 71:209–249. https://doi.org/10.3322/caac.21660
Talluri R, Shete S (2016) Using the weighted area under the net benefit curve for decision curve analysis. BMC Med Inform Decis Mak 16:94. https://doi.org/10.1186/s12911-016-0336-x
Tang L-L, Chen W-Q, Xue W-Q et al (2016) Global trends in incidence and mortality of nasopharyngeal carcinoma. Cancer Lett 374:22–30. https://doi.org/10.1016/j.canlet.2016.01.040
Tsao SW, Tsang CM, Lo KW (2017) Epstein-Barr virus infection and nasopharyngeal carcinoma. Philos Trans R Soc Lond B 372:20160270. https://doi.org/10.1098/rstb.2016.0270
Van Calster B, Vickers AJ (2015) Calibration of risk prediction models: impact on decision-analytic performance. Med Decis Mak 35:162–169. https://doi.org/10.1177/0272989X14547233
Vazquez A, Khan MN, Govindaraj S et al (2014) Nasopharyngeal squamous cell carcinoma: a comparative analysis of keratinizing and nonkeratinizing subtypes. Int Forum Allergy Rhinol 4:675–683. https://doi.org/10.1002/alr.21332
Vickers AJ, Elkin EB (2006) Decision curve analysis: a novel method for evaluating prediction models. Med Decis Mak 26:565–574. https://doi.org/10.1177/0272989X06295361
Wang Y, Zhang Y, Ma S (2013) Racial differences in nasopharyngeal carcinoma in the United States. Cancer Epidemiol. https://doi.org/10.1016/j.canep.2013.08.008
Wei WI, Sham JST (2005) Nasopharyngeal carcinoma. Lancet 365:2041–2054. https://doi.org/10.1016/S0140-6736(05)66698-6
Wu S-G, Lian C-L, Wang J et al (2019) The effect of histological subtypes on survival outcome in nasopharyngeal carcinoma after extensive follow up. Ann Transl Med 7:768–768. https://doi.org/10.21037/atm.2019.11.75
Wu W-T, Li Y-J, Feng A-Z et al (2021) Data mining in clinical big data: the frequently used databases, steps, and methodological models. Mil Med Res 8:44. https://doi.org/10.1186/s40779-021-00338-z
Yang L, Hong S, Wang Y et al (2015) Development and external validation of nomograms for predicting survival in nasopharyngeal carcinoma patients after definitive radiotherapy. Sci Rep. https://doi.org/10.1038/srep15638
Yang J, Li Y, Liu Q et al (2020) Brief introduction of medical database and data mining technology in big data era. J Evid Based Med 13:57–69. https://doi.org/10.1111/jebm.12373
Zhang Q-X, Zhuang L-P, Lin Z-Y (2021) Prognostic models for 1-year survival of NPC after radiotherapy in different ages. Eur Arch Otorhinolaryngol 278:4955–4965. https://doi.org/10.1007/s00405-021-06730-8
Acknowledgements
We are incredibly grateful for the SEER database that is publicly available.
Funding
The National Natural Science Foundation of China (No.82172346), and the Technology and Innovation Commission of the Guangzhou Science Association of China (No.202102010087), supported the project.
Author information
Authors and Affiliations
Contributions
HZ designed and developed the conceptual framework, collected the data, performed the statistical analysis, and drafted the manuscript. ML critically revised and created the manuscript. Both authors approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
It is declared that none of the authors have any commercial or financial relationships that could be considered a conflict of interest.
Ethical approval and patient consent
The collection of SEER data information is permitted by Section 411 of the Public Health Service Act (42 USC 285a). Study subjects are protected by the Privacy Act of 1974. SEER database releases updated research data each spring based on November submissions. Since the data contains no personally identifying information, informed consent is not required. Data in the SEER Registry are publicly available, and we have been granted access to them (License Number: xIFKJ11a).
Consent to publish
All authors consent to the publication of the manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zuo, H., Li, MM. Two web-based dynamically interactive nomograms and risk stratification systems for predicting survival outcomes and guiding treatment in non-metastatic nasopharyngeal carcinoma. J Cancer Res Clin Oncol 149, 15969–15987 (2023). https://doi.org/10.1007/s00432-023-05363-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-023-05363-0