Abstract
Purpose
Rising incidence of pancreatic ductal adenocarcinoma (PDAC) bind with insufficient therapy options showcases a great medical challenge. Further biomarkers are required to identify patients, who will benefit from more aggressive therapy.
Methods
320 patients were included by the PANCALYZE study group. Cytokeratin 6 (CK6) immunohistochemical staining as a putative marker for the basal-like subtype of PDAC was performed. The correlation between CK6 expression patterns and survival data, as well as various markers of the (inflammatory) tumor microenvironment, were analyzed.
Results
We divided the study population based on the expression pattern of CK6. Patients with a high CK6 tumor expression had a significantly shorter survival (p = 0.013), confirmed in a multivariate cox regression model. CK6-expression is an independent marker for a decreased overall survival (HR = 1.655, 95% CI 1.158–2.365, p = 0.006). In addition, the CK6-positive tumors showed significantly less plasma cell infiltration and more cancer-associated fibroblasts (CAFs) expressing Periostin and SMA.
Conclusions
CK6 could be considered as an independent biomarker for a shorter overall survival. CK6 is a clinically easily accessible biomarker for the identification of the basal-like subtype of PDAC. Therefore, it could be taken into consideration in deciding for the more aggressive therapy regimes. Prospectively, studies addressing the chemosensitive characteristics of this subtype are required.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Predicted to increase by 1.1% annually until 2050, the incidence of pancreatic ductal adenocarcinoma (PDAC) is rising worldwide (Hu et al. 2021). While the treatment of other cancer types demonstrates great improvements, the 5-year survival rate of the PDAC patients remains low (Bengtsson et al. 2020). The recent breakthrough in pancreatic cancer therapy was the modification of the standard chemotherapy from gemcitabine to FOLFIRINOX with a significant increase in the 5-year overall survival rate (Conroy et al. 2022). However, FOLFIRINOX therapy leads to significantly more frequent grade III and IV adverse events compared to gemcitabine (Conroy et al. 2018). Therefore, this therapy option is limited to young patients with only a few secondary diagnoses (Dosso, et al. 2021). Further biomarkers are, therefore, required to pre-select patients with certain tumor types that are sufficiently sensitive to more aggressive chemotherapy (Dosso, et al. 2021; Kalia 2015). Expanded therapy regimes are not only limited to the chemotherapeutic arm. The HOLIPANC study is already softening paradigms, which have been described in the guidelines for decades (Gebauer et al. 2021). Hence, the patients with oligometastatic adenocarcinoma of the pancreas are receiving neoadjuvant therapy before undergoing a subsequent curative resection. Since the study is still including patients, the first results are still pending (Gebauer et al. 2021). Surely, exact subtypes of pancreatic adenocarcinoma are required to be described to facilitate clinical decision-making and to further enhance the personalized oncology (Grullich and Kalle 2012).
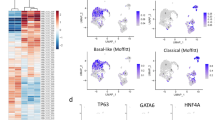
Moffitt et al. described stroma- and tumor specific subtypes of PDAC via virtual microdissection (Moffitt et al. 2015). Based on the RNA sequencing the authors were able to define the classical and the basal-like tumor-specific subtypes. Here, the patients with the basal-like subtype show a significantly poorer survival (Moffitt et al. 2015). Basal-like subtype has already been identified in other cancer types, for instance in the breast and bladder cancer (Perou et al. 2000; McConkey et al. 2015). This subtype is identified by a specific gene expression and correlates with patients’ shorter survival (McConkey et al. 2015). Basal-like subtypes of invasive bladder cancer may exhibit a different response to certain therapies. Hence, preclinical data show, that the basal-like cell lines are sensitive to the anti-EGFR therapy (Rebouissou, et al. 2014). In the COMPASS trial pretreated tumor tissue of patients with an advanced PDAC was collected (Aung et al. 2018). In this patient cohort, RNA sequencing and immunohistochemical stainings were performed. Here, GATA6 could be identified as a marker for the classical type. In addition, cytokeratin 5, which acts mainly inversely to GATA6, was identified as a marker for the basal-like subtype of PDAC (O’Kane et al. 2020). However, combined antibodies for cytokeratin 5 and 6 are widely used to identify basal-like subtypes in several cancer types (Nielsen et al. 2004; Plumb et al. 2004). Recent evidence shows that cytokeratin 5/6 expressions and diagnostic implications are not similar (Volkel et al. 2022). Cytokeratin 5 and 6 belong to the diverse family of filament proteins of the epithelial (Moll et al. 2008). Cytokeratins are part of the cellular cytoskeleton and intracellular pathways (Moll et al. 2008).
In this study, we sought to investigate cytokeratin 6 as a marker for the basal-like subtype in PDAC and its prognostic value. In addition, we elucidate the cellular microenvironment of the CK6-positive compared to the CK6-negative tumors.
Materials and methods
Patients and tumor samples
All selected cases (n = 320) underwent the surgical procedure between 2013 and 2020 with a curative intention in one of the participating centers of the PANCALYZE group. Written informed consent was obtained from every patient. The study was approved by the local ethics committees and was conducted in accordance with the declaration of Helsinki. The tumor stage was described based on the 7th edition of the Union for International Cancer Control. The tumor tissue samples were transferred to the University Hospital of Cologne. Here, two 1.2 mm tissue cylinders of each tumor sample were punched out with a semi-automated precision instrument and transferred in a recipient paraffin block. The so-formed tissue microarray (TMA) was then cut into 4 µm thick slides for further stainings and transferred to an adhesive-coated slide system (Instrumedics Inc., Hackensack, NJ).
Immunohistochemistry (IHC) and analysis
CD3 (T-cells), CD20, (B-cells) CD38 (plasma-cells), CD56 (natural killer cells), CD66b (tumor associated polymorph neutrophils), CD117 (mast cells), CD163 (M2 macrophages), CK5/6 (basal-like cytokeratin mix of cytokeratin 5 as well as cytokeratin 6), CK6 (basal-like cytokeratin 6 only), FAP (fibroblast-associated protein), Periostin (stroma-related protein), PDGFR (platelet-derived growth factor receptor-β), and SMA (α-SM actin) were determined using the immunohistochemistry. Further information regarding the used antibodies is given in Supp. Table 1. All stainings were conducted automatically with the Leica Bond-MAX automated system (Leica Biosystems, Germany). The performed stainings were digitalized with the Aperio GT 450 DX (Leica Biosystems, Germany). Two experienced, independent pathologists (S.L. and A.Q.) analyzed cytokeratin 6 and CK5/6 stainings according to previously published studies as following: the tumor cells without any positive staining were labeled negative, tissues with a weak positive staining ≤ 70% or a strong positive staining ≤ 30% were considered as CK6 low-positive and tissues with a weak positive staining > 70% or a strong positive staining > 30% as CK6 high-positive (Volkel et al. 2022). The tumor microenvironment stainings were evaluated digitally using QuPath v0.3.2 (Bankhead et al. 2017). Both entire cores of each tumor have been analyzed and the mean out of these has been calculated for each patient. Stainings were considered as highly positive if the calculated value was higher or equal to the mean of the whole study population.
Statistical analysis
Clinicopathologic variables and follow-up were obtained prospectively following the study protocol of the PANCALYZE study and analyzed retrospectively (Popp et al. 2017). Statistical analyses were executed with IBM SPSS Statistics (Version 28.0.1.1). P values below 0.05 were considered as significant. The overall survival was defined as the time from the surgical resection until patients’ death or loss of follow-up. Survival analyses were conducted with Kaplan-Meier curves. Furthermore, all clinicopathologic variables and CK6-expression were analyzed for interdependence with univariate and multivariate cox proportional hazards model. The comparison of qualitative values was performed with the Chi-square test.
Results
Patients were recruited from the study centers of the PANCALYZE study group. 320 tumor samples of patients with complete clinicopathologic variables and follow-up were included in this study. All patients were operated in curative intent from 2013 to 2020 following the German S3 guideline. The median overall follow-up was 18 months (range: 3–98 months). General patients’ characteristics are shown in Table 1. 94.7% received no neoadjuvant therapy prior to resection. 228 patients (70.2%) had histologically confirmed lymph node metastasis. Incomplete resection (R1/2) was seen in 35.6% of all included patients.
Since the goal of this study was to establish CK6 as a new biomarker for the basal-like subtype of PDAC we have performed immunohistochemical stainings with this marker and divided the total population in CK6-negative (n = 126), CK6-low (n = 108) and CK6-high (n = 86). Representative microscopy photographs of the stainings are shown in Fig. 1A. No significant differences in the clinicopathologic variables between these groups were identified (Table 1).
A Representative microscopy photographs of the different strengths of CK6-expression (left: CK6 negative, middle: CK6 low, right: CK6 high). B Kaplan-Meier curve for overall survival of patients with negative, low, or high CK6-staining (n(negative) = 126, n(low) = 108, n(high) = 86, p = 0.013). Scale bar: 50 µm
To assess the prognostic value of cytokeratin 6 a survival analysis with Kaplan-Meier curves was performed. Here, patients with a high CK6 tumor expression have shown a significantly decreased overall survival compared to CK6 negative tumor patients (p = 0.013; CK6 negative: OS = 35.2 months, 95% CI 30.1–40.2 months; CK6 low: OS = 39.5 months, 95% CI 31.5–47.5 months; CK6 high: OS = 24.5 months, 95% CI 19.4–29.5 months; Fig. 1B).
We then carried out the cox proportional hazards model to further evaluate the impact of the clinicopathologic variables on patients’ overall survival. Here, CK6-positivity proved to be a factor for a poorer survival (p = 0.016, Supp. Table 2). In addition, a higher pT-stage, a higher pN-stage, an incomplete resection, and perineural tumor infiltration showed to be the factors for shorter overall survival in the univariate cox proportional hazards model (pT: p = 0.004, pN: p < 0.001, R: p < 0.001, perineural invasion: p = 0.045, Supp. Table 2).
A multivariate cox proportional hazards model was performed to correct our results for cofounders as well as any effect modifiers. Following borders for the multivariate cox proportional hazards model were selected: for the pT-stage, pT1 was compared to pT2, pT3, or pT4; for pN-stage, no lymph node metastases (pN0) was compared to pathologically diagnosed lymph node metastases (pN1); for R-stage, complete resection (R0) was compared to incomplete resection (R1 and R2); for perineural invasion, Pn0 was compared to Pn1; for CK6, negative (0) stainings were compared to low (1) or high (2) positive stainings.
Cytokeratin 6 proves to be an independent factor for shorter patients’ overall survival (HR = 1.655, 95% CI 1.158–2.365, p = 0.006, Table 2). Furthermore, a higher pN-stage and an incomplete resection are independent risk factors for a poorer survival (pN: HR = 2.058, 95% CI 1.434–2.954, p < 0.001; R: HR = 1.408, 95% CI 1.042–1.903, p = 0.026, Table 2).
Classical and basal-like subtypes of PDAC are characterized by different gene expression clusters. The immunohistochemical standard to identify the basal-like subtype is a CK5/6-positive staining (O’Kane et al. 2020). Therefore, we wanted to further investigate the morphologic growth patterns as well as the cellular composition of the microenvironment based on the CK6-expression.
After evaluating all of the CK6-positive and negative tissue samples, no significant difference in the solely morphologic PDAC growth patterns in the H&E stain was registered. From the 87 CK6-positive tumors only two could be identified as an adenosquamous and one tumor as a hepatoid carcinoma subtype. The majority (84 cases) has shown a conventional glandular (ductal) differentiation.
CK5/6 TMA stainings were also performed to measure the correlation with the CK6 TMA stainings. The different levels of staining intensities correlated with each other (p < 0.001). However, 48.1% of negative CK5/6 stainings showed positive staining for CK6. Only 13.3% of negative CK6 stainings showed a low positive staining for CK5/6 and 15.9% high positive staining for CK5/6.
To describe the expression pattern of CK5/6 and CK6 stainings in the tumor, we stained the corresponding whole tissue sections for all CK6-positive TMA samples with CK5/6 and CK6 antibodies. Here, the mean homogeneity of 71% for CK6 and 51.6% for CK5/6 were shown.
Immunohistochemical stainings for CD3, CD20, CD38, CD56, CD66b, CD117, and CD163 as stromal immunity-related cells and FAP, Periostin, PDGFR, and SMA as common markers for fibroblasts were conducted. Again, the stainings were analyzed on microscopy photographs using QuPath v0.3.2 by two independent pathologists. Then, different expression patterns of these markers were correlated between the three above-described CK6 subgroups. Besides no significant differences in most of the stromal immunity-related cell markers, significantly fewer plasma cells were detected in tumor samples with CK6 expression (CD38: p = 0.044, Table 3). On the contrary, significantly more Periostin- and SMA-expression was found in patients with a stronger CK6-expression (Periostin: p = 0.023; SMA: p = 0.006, Table 3).
Summarized, we could show that Cytokeratin 6 is a marker for shorter patients’ overall survival. Multivariate cox proportional hazards model could confirm CK6 as an independent risk factor for poor survival. In addition, we could show differences in the cellular composition of the tumor microenvironment depending on the CK6 expression status. Significantly fewer plasma cells and more Periostin- as well as SMA-positive tumor-associated fibroblasts could be detected in CK6-expressing tumor samples.
Discussion
We have evaluated Cytokeratin 6 as a biomarker in PDAC. Therefore, immunohistochemical stainings in tumor tissue samples of 320 patients were performed. We could show that a higher CK6 expression is an independent risk factor for decreased overall survival. These findings align with the previously described prognostic variables of the cytokeratin 5 positive PDACs (O’Kane et al. 2020). CK5/6 was described to be a marker for the basal-like subtype, which shows a shorter survival in numerous cancer types (Nielsen et al. 2004; Plumb et al. 2004). In most publications, a bispecific antibody against Cytokeratin 5 and 6 was used. Both cytokeratins showcase similarities and the jointed immunohistochemical examination has a clinical utility, since the common antibodies recognize both, Cytokeratin 5 and 6 (Volkel et al. 2022). However, it must be taken into consideration that the bispecific stainings may also have a reduced sensitivity due to the use of different epitopes (Alshareeda et al. 2013; Bhargava et al. 2008; Rakha et al. 2007). Bhargava et al. could show that the CK5 antibody has a sensitivity of 97% compared to 59% of an antibody against CK5/6 in breast carcinoma (Bhargava et al. 2008). We correlated the CK5/6 with the CK6 staining. Here, we could show a significant correlation. However, 48.1% of tissue samples with negative CK5/6 stainings showed a low or high positive tumor staining for CK6. This confirms the previously shown results and questions the accuracy of CK5/6 stainings. Despite similarities between cytokeratin 5 and 6, both proteins show different expression patterns in physiologic tissue as well as in tumors (Moll et al. 1982; Schiller et al. 1982). It could be shown, that CK6 was predominantly expressed in adenocarcinomas, especially in adenocarcinoma of the pancreas (Volkel et al. 2022). However, this project is the first to investigate the prognostic role of CK6 alone in PDAC. Interestingly, cytokeratin 6 was found in 28.7% of the tumor samples in gastric adenocarcinoma. Here, CK6 was correlated with the microsatellite instability, early TNM stages, and a longer overall survival (Kim et al. 2004).
The basal-like subtype was identified in 28.8% of the total study population when primarily observed in PDAC. (Moffitt et al. 2015). In our patient cohort, 26.9% showed a high tumor expression of CK6. We hypothesize, that CK6 is a sufficient marker for the basal-like subtype of PDAC. Nonetheless, further mechanistic investigations are required to fully understand the pathomechanisms behind them. In addition, in further projects, the positivity of CK6 immunohistochemical stainings should be compared to the original genetical definition of the basal-like subtype as described by Moffitt et al. (Moffitt et al. 2015). If the CK6 expression correlates with the genetic definition, CK6 could be used as an easy appliable marker for the basal-like subtype in the daily clinical diagnostic. This evaluation showcased a relatively homogenous expression pattern for CK6, suggesting that CK6 could be evaluated even on pre-treatment biopsy type specimens. This could lead to a personalized chemotherapy regime. Analyses identified that patients with a basal-like subtype of PDAC had a significantly higher chance for a tumor progression under therapy with FOLFIRINOX (O’Kane et al. 2020).
This study could identify that not only the protein expression—as described previously—is different in the basal-like subtype, but so is the cellular microenvironment (Moffitt et al. 2015). Significantly fewer plasma cells could be detected in tumors with a higher CK6 tumor expression. Previous studies could show that an alteration of structural proteins could change the plasma cell infiltration in tumors. A deficiency of Cadherin 11, a cell-to-cell adhesion molecule, leads to an increase of plasma cells in the PDAC mouse model (Martin 2022; Takeichi 1995). Higher amounts of infiltrating plasma cells correlate with a longer overall survival in patients with PDAC (Liu et al. 2020). Higher CD38-positive cell proportion correlated significantly with a better response to immune-checkpoint blockade in hepatocellular carcinoma (Ng, et al. 2020).
In addition, we could show that SMA and Periostin are significantly more frequently detectable in tissues with a high CK6 tumor expression. In line with our results, SMA is known to be expressed in more aggressive tumors of the pancreas and is also an independent risk factor for poor overall survival (Fujita et al. 2010). Periostin demonstrates similar negative effects on survival and seems to be involved in the chemotherapy resistance to gemcitabine in PDAC (Liu et al. 2017; Liu et al. 2016).
Taken all together, CK6 could be used as an easy tool to differentiate between the two subtypes of PDAC with a single immunohistochemical staining and, therefore, contribute to deciding on the best-fitting therapy regime. We demonstrated that strongly CK6-positive PDACs have homogeneous positivity of CK6 across almost all tumor cells in the majority of cases, so that even a preoperative biopsy would be sufficient to correctly diagnose this basal phenotype.
Conclusions
CK6 defines the basal subtype of PDAC. There is good evidence that the basal phenotype of PDAC benefits to a lesser extent from the FOLFIRINOX therapy. We showed in a German study population (PANCALYZE) that CK6 is an independent risk factor for a shorter overall survival in PDAC. In addition, this work showcases for the first time that the composition of the cellular microenvironment differs significantly depending on the CK6 expression. These findings could lead to a wide clinical use to determine a therapy pathway in a personalized manner. However, more preclinical studies are required to identify the best-fitting therapy options for each of the subtypes.
Data availability
The data sets generated and analyzed during the current study are available from the corresponding author on reasonable request.
References
Alshareeda AT et al (2013) Characteristics of basal cytokeratin expression in breast cancer. Breast Cancer Res Treat 139:23–37. https://doi.org/10.1007/s10549-013-2518-x
Aung KL et al (2018) Genomics-driven precision medicine for advanced pancreatic cancer: early results from the COMPASS trial. Clin Cancer Res 24:1344–1354. https://doi.org/10.1158/1078-0432.CCR-17-2994
Bankhead P et al (2017) QuPath: open source software for digital pathology image analysis. Sci Rep 7:16878. https://doi.org/10.1038/s41598-017-17204-5
Bengtsson A, Andersson R, Ansari D (2020) The actual 5-year survivors of pancreatic ductal adenocarcinoma based on real-world data. Sci Rep 10:16425. https://doi.org/10.1038/s41598-020-73525-y
Bhargava R, Beriwal S, McManus K, Dabbs DJ (2008) CK5 is more sensitive than CK5/6 in identifying the “basal-like” phenotype of breast carcinoma. Am J Clin Pathol 130:724–730. https://doi.org/10.1309/AJCP3KFF1LTYWQIY
Conroy T et al (2018) FOLFIRINOX or gemcitabine as adjuvant therapy for pancreatic cancer. N Engl J Med 379:2395–2406. https://doi.org/10.1056/NEJMoa1809775
Conroy T et al (2022) Five-year outcomes of FOLFIRINOX vs gemcitabine as adjuvant therapy for pancreatic cancer: a randomized clinical trial. JAMA Oncol. https://doi.org/10.1001/jamaoncol.2022.3829
De Dosso S et al (2021) Treatment landscape of metastatic pancreatic cancer. Cancer Treat Rev 96:102180. https://doi.org/10.1016/j.ctrv.2021.102180
Fujita H et al (2010) Alpha-smooth muscle actin expressing stroma promotes an aggressive tumor biology in pancreatic ductal adenocarcinoma. Pancreas 39:1254–1262. https://doi.org/10.1097/MPA.0b013e3181dbf647
Gebauer F et al (2021) Study protocol of an open-label, single arm phase II trial investigating the efficacy, safety and quality of life of neoadjuvant chemotherapy with liposomal irinotecan combined with Oxaliplatin and 5-fluorouracil/Folinic acid followed by curative surgical resection in patients with hepatic Oligometastatic adenocarcinoma of the pancreas (HOLIPANC). BMC Cancer 21:1239. https://doi.org/10.1186/s12885-021-08966-3
Grullich C, von Kalle C (2012) Recent developments and future perspectives of personalized oncology. Onkologie 35(Suppl 1):4–7. https://doi.org/10.1159/000334825
Hu JX et al (2021) Pancreatic cancer: a review of epidemiology, trend, and risk factors. World J Gastroenterol 27:4298–4321. https://doi.org/10.3748/wjg.v27.i27.4298
Kalia M (2015) Biomarkers for personalized oncology: recent advances and future challenges. Metabolism 64:S16-21. https://doi.org/10.1016/j.metabol.2014.10.027
Kim MA, Lee HS, Yang HK, Kim WH (2004) Cytokeratin expression profile in gastric carcinomas. Hum Pathol 35:576–581. https://doi.org/10.1016/j.humpath.2003.12.007
Liu Y et al (2016) Periostin promotes the chemotherapy resistance to gemcitabine in pancreatic cancer. Tumour Biol 37:15283–15291. https://doi.org/10.1007/s13277-016-5321-6
Liu Y et al (2017) Role of microenvironmental periostin in pancreatic cancer progression. Oncotarget 8:89552–89565. https://doi.org/10.18632/oncotarget.11533
Liu R, Liao YZ, Zhang W, Zhou HH (2020) Relevance of immune infiltration and clinical outcomes in pancreatic ductal adenocarcinoma subtypes. Front Oncol 10:575264. https://doi.org/10.3389/fonc.2020.575264
Martin KA et al (2022) Abstract 2516: Loss of cadherin 11 in pancreatic cancer induces altered immune cell infiltration. Cancer Res 82:2516
McConkey DJ, Choi W, Dinney CP (2015) Genetic subtypes of invasive bladder cancer. Curr Opin Urol 25:449–458. https://doi.org/10.1097/MOU.0000000000000200
Moffitt RA et al (2015) Virtual microdissection identifies distinct tumor- and stroma-specific subtypes of pancreatic ductal adenocarcinoma. Nat Genet 47:1168–1178. https://doi.org/10.1038/ng.3398
Moll R, Franke WW, Schiller DL, Geiger B, Krepler R (1982) The catalog of human cytokeratins: patterns of expression in normal epithelia, tumors and cultured cells. Cell 31:11–24. https://doi.org/10.1016/0092-8674(82)90400-7
Moll R, Divo M, Langbein L (2008) The human keratins: biology and pathology. Histochem Cell Biol 129:705–733. https://doi.org/10.1007/s00418-008-0435-6
Ng HHM et al (2020) Immunohistochemical scoring of CD38 in the tumor microenvironment predicts responsiveness to anti-PD-1/PD-L1 immunotherapy in hepatocellular carcinoma. J Immunother Cancer 8:e000987. https://doi.org/10.1136/jitc-2020-000987
Nielsen TO et al (2004) Immunohistochemical and clinical characterization of the basal-like subtype of invasive breast carcinoma. Clin Cancer Res 10:5367–5374. https://doi.org/10.1158/1078-0432.CCR-04-0220
O’Kane GM et al (2020) GATA6 expression distinguishes classical and basal-like subtypes in advanced pancreatic cancer. Clin Cancer Res 26:4901–4910. https://doi.org/10.1158/1078-0432.CCR-19-3724
Perou CM et al (2000) Molecular portraits of human breast tumours. Nature 406:747–752. https://doi.org/10.1038/35021093
Plumb SJ, Argenyi ZB, Stone MS, De Young BR (2004) Cytokeratin 5/6 immunostaining in cutaneous adnexal neoplasms and metastatic adenocarcinoma. Am J Dermatopathol 26:447–451. https://doi.org/10.1097/00000372-200412000-00001
Popp FC et al (2017) Protocol of the PANCALYZE trial: a multicenter, prospective study investigating the tumor biomarkers CXCR4, SMAD4, SOX9 and IFIT3 in patients with resected pancreatic adenocarcinoma to predict the pattern of recurrence of the disease. BMC Cancer 17:229. https://doi.org/10.1186/s12885-017-3186-8
Rakha EA et al (2007) Prognostic markers in triple-negative breast cancer. Cancer 109:25–32. https://doi.org/10.1002/cncr.22381
Rebouissou S et al (2014) EGFR as a potential therapeutic target for a subset of muscle-invasive bladder cancers presenting a basal-like phenotype. Sci Transl Med 6:244ra291. https://doi.org/10.1126/scitranslmed.3008970
Schiller DL, Franke WW, Geiger B (1982) A subfamily of relatively large and basic cytokeratin polypeptides as defined by peptide mapping is represented by one or several polypeptides in epithelial cells. EMBO J 1:761–769. https://doi.org/10.1002/j.1460-2075.1982.tb01243.x
Takeichi M (1995) Morphogenetic roles of classic cadherins. Curr Opin Cell Biol 7:619–627. https://doi.org/10.1016/0955-0674(95)80102-2
Volkel C et al (2022) Cytokeratin 5 and cytokeratin 6 expressions are unconnected in normal and cancerous tissues and have separate diagnostic implications. Virchows Arch 480:433–447. https://doi.org/10.1007/s00428-021-03204-4
Acknowledgements
We would like to thank the PANCALYZE study group investigators: Michael Heise (Sana Klinikum Lichtenberg, Berlin), Frank Marusch (Klinikum Ernst von Bergmann, Potsdam), Marco Siech (Ostalb-Klinikum Aalen), Tawfik Mosa (Carl-von-Basedow Klinikum Saalekreis, Merseburg), Bodo Schniewind (Städtisches Klinikum Lüneburg), Jürgen Tepel (Klinikum Osnabrück), Werner Hartwig (Evangelisches Krankenhaus Düsseldorf), Christoph Prinz (KMG Klinikum Güstrow), Bettina M. Rau (Klinikum Neumarkt), Marco Niedergethmann (Alfried Krupp Krankenhaus, Essen), Rainer Kube (Carl-Thiem-Klinikum Cottbus), George Saada (Klinikum Robert Koch Gehrden), Wolfgang Hiller (Klinikum Lippe, Detmold), and Utz Settmacher (Uniklinikum Jena). The authors thank Magdalene Fielenbach for the construction of the tissue microarrays and Wiebke Jeske for their excellent technical assistance.
Funding
Open Access funding enabled and organized by Projekt DEAL. This research received no external funding.
Author information
Authors and Affiliations
Consortia
Contributions
SL, KK, FP, and AQ contributed to the study’s conception and design. Material preparation and data collection were performed by SL and KK. Analysis was performed by KK and SL. The first draft of the manuscript was written by KK. All authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethical approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Ethics Committee of the University of Cologne (protocol code 16–230, 19th of September 2016).
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent to publish
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Membership of the PANCALYZE Study Group is provided in the Acknowledgments.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Lyu, S., Krey, T., Damanakis, A.I. et al. Cytokeratin 6 identifies basal-like subtypes of pancreatic ductal adenocarcinoma with decreased survival. J Cancer Res Clin Oncol 149, 7539–7546 (2023). https://doi.org/10.1007/s00432-023-04702-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-023-04702-5