Abstract
Purpose
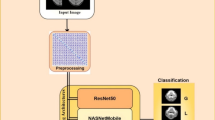
To investigate the application of deep learning combined with traditional radiomics methods for classifying enlarged cervical lymph nodes.
Methods
The clinical and computed tomography (CT) imaging data of 276 patients with enlarged cervical lymph nodes (150 with lymph-node metastasis, 65 with lymphoma, and 61 with benign lymphadenopathy) who were treated at the hospital from January 2015 to January 2021 were retrospectively analysed. The patients were randomly divided into a training group and a test group at a ratio of 8:2. The radiomics features were extracted using one-by-one convolution and neural network activation, filtered with the least absolute shrinkage and selection operator (LASSO) model, and used to construct a discrimination model with PyTorch. Then, the performance of the model was compared with the radiologists’ diagnostic performance. The neural network model was evaluated using the area under the receiver-operator characteristic curve (AUC), and the accuracy, sensitivity, and specificity were analysed.
Results
A total of 102 features, comprising five traditional radiomic features and 97 deep learning features, were selected with LASSO and used to construct a discrimination model, which achieved a total accuracy of 87.50%. The AUC value, specificity, and sensitivity were, respectively, 0.92, 92.30%, and 90.00% for metastatic lymph nodes, 0.87, 95.45%, and 83.33% for benign lymphadenopathy, and 0.88, 90.47%, and 85.71% for lymphoma. The accuracies of the radiologists’ diagnoses were 62.68% and 62.68%. The diagnostic performance of the model was significantly different from that of the radiologists (p < 0.05).
Conclusion
CT-based deep learning combined with the traditional radiomics methods has a high diagnostic value for the classification of cervical enlarged lymph nodes.



Similar content being viewed by others
References
Bayanati H, Thornhill RE, Souza CA et al (2015) Quantitative CT texture and shape analysis: can it differentiate benign and malignant mediastinal lymph nodes in patients with primary lung cancer? Eur Radiol 25(2):480–487. https://doi.org/10.1007/s00330-014-3420-6
Gillies RJ, Kinahan PE, Hricak H (2016) Radiomics: images are more than pictures, they are data. Radiology 278(2):563–577. https://doi.org/10.1148/radiol.2015151169
Kann BH, Hicks DF, Payabvash S et al (2020) Multi-institutional validation of deep learning for pretreatment identification of extranodal extension in head and neck squamous cell carcinoma. J Clin Oncol 38(12):1304–1311. https://doi.org/10.1200/JCO.19.02031
Kuno H, Garg N, Qureshi MM et al (2019) CT texture analysis of cervical lymph nodes on contrast-enhanced [(18)F] FDG-PET/CT images to differentiate nodal metastases from reactive lymphadenopathy in HIV-positive patients with head and neck squamous cell carcinoma. AJNR Am J Neuroradiol 40(3):543–550. https://doi.org/10.3174/ajnr.A5974
Le WT, Maleki F, Romero FP et al (2020) Overview of machine learning: part 2 deep learning for medical image analysis. Neuroimaging Clin North Am 30(4):417. https://doi.org/10.1016/j.nic.2020.06.003
Lee JH, Ha EJ, Kim JH (2019) Application of deep learning to the diagnosis of cervical lymph node metastasis from thyroid cancer with CT. Eur Radiol 29(10):5452–5457. https://doi.org/10.1007/s00330-019-06098-8
Limkin EJ, Sun R, Dercle L et al (2017) Promises and challenges for the implementation of computational medical imaging (radiomics) in oncology. Ann Oncol 28(6):1191–1206. https://doi.org/10.1093/annonc/mdx034
Lubner MG, Smith AD, Sandrasegaran K et al (2017) CT texture analysis: definitions, applications, biologic correlates, and challenges. Radiographics 37(5):1483–1503. https://doi.org/10.1148/rg.2017170056
Mayerhoefer ME, Materka A, Langs G et al (2020) Introduction to radiomics. J Nucl Med 61(4):488–495. https://doi.org/10.2967/jnumed.118.222893
Meador TL, McLarney JK (2000) CT features of Castleman disease of the abdomen and pelvis. AJR Am J Roentgenol 175(1):115–118. https://doi.org/10.2214/ajr.175.1.1750115
Moeckelmann N, Ebrahimi A, Tou YK et al (2018) Prognostic implications of the 8th edition American Joint Committee on Cancer (AJCC) staging system in oral cavity squamous cell carcinoma. Oral Oncol 85:82–86. https://doi.org/10.1016/j.oraloncology.2018.08.013
Nakagawa M, Nakaura T, Namimoto T et al (2018) Machine learning based on multi-parametric magnetic resonance imaging to differentiate glioblastoma multiforme from primary cerebral nervous system lymphoma. Eur J Radiol 108:147–154. https://doi.org/10.1016/j.ejrad.2018.09.017
Park VY, Han K, Kim HJ et al (2020) Radiomics signature for prediction of lateral lymph node metastasis in conventional papillary thyroid carcinoma. PLoS ONE 15(1):e0227315. https://doi.org/10.1371/journal.pone.0227315
Seidler M, Forghani B, Reinhold C et al (2019) Dual-energy CT texture analysis with machine learning for the evaluation and characterization of cervical lymphadenopathy. Comput Struct Biotechnol J 17:1009–1015. https://doi.org/10.1016/j.csbj.2019.07.004
van den Brekel MW, Stel HV, Castelijns JA et al (1990) Cervical lymph node metastasis: assessment of radiologic criteria. Radiology 177(2):379–384. https://doi.org/10.1148/radiology.177.2.2217772
Wang H, Wang L, Lee EH et al (2021) Decoding COVID-19 pneumonia: comparison of deep learning and radiomics CT image signatures. Eur J Nucl Med Mol Imaging 48(5):1478–1486. https://doi.org/10.1007/s00259-020-05075-4
Wu WL, Li JW, Ye JY et al (2021) Differentiation of glioma mimicking encephalitis and encephalitis using multiparametric MR-based deep learning. Front Oncol. https://doi.org/10.3389/fonc.2021.639062
Yang R, Chen Y, Sa G et al (2021) CT classification model of pancreatic serous cystic neoplasms and mucinous cystic neoplasms based on a deep neural network. Abdom Radiol (NY). https://doi.org/10.1007/s00261-021-03230-5
Yi CA, Lee KS, Kim EA et al (2004) Solitary pulmonary nodules: dynamic enhanced multi-detector row CT study and comparison with vascular endothelial growth factor and microvessel density. Radiology 233(1):191–199. https://doi.org/10.1148/radiol.2331031535
Zhou C, Duan X, Lan B et al (2015) Prognostic CT and MR imaging features in patients with untreated extranodal non-Hodgkin lymphoma of the head and neck region. Eur Radiol 25(10):3035–3042. https://doi.org/10.1007/s00330-015-3708-1
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No authors have any conflicts of interest to disclose.
Ethical approval
Ethical approval was waived by the Ethics Committee of the First Affiliated Hospital of Chongqing Medical University (Approval No. 2019-178) in view of the retrospective nature of the study, and all the procedures performed were part of routine care.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Zhang, W., Peng, J., Zhao, S. et al. Deep learning combined with radiomics for the classification of enlarged cervical lymph nodes. J Cancer Res Clin Oncol 148, 2773–2780 (2022). https://doi.org/10.1007/s00432-022-04047-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-022-04047-5