Abstract
Introduction
We aimed to develop a diagnostic deep learning model using contrast-enhanced CT images and to investigate whether cervical lymphadenopathies can be diagnosed with these deep learning methods without radiologist interpretations and histopathological examinations.
Material method
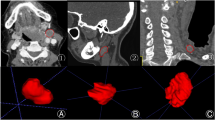
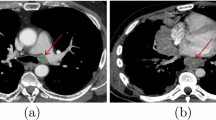
A total of 400 patients who underwent surgery for lymphadenopathy in the neck between 2010 and 2022 were retrospectively analyzed. They were examined in four groups of 100 patients: the granulomatous diseases group, the lymphoma group, the squamous cell tumor group, and the reactive hyperplasia group. The diagnoses of the patients were confirmed histopathologically. Two CT images from all the patients in each group were used in the study. The CT images were classified using ResNet50, NASNetMobile, and DenseNet121 architecture input.
Results
The classification accuracies obtained with ResNet50, DenseNet121, and NASNetMobile were 92.5%, 90.62, and 87.5, respectively.
Conclusion
Deep learning is a useful diagnostic tool in diagnosing cervical lymphadenopathy. In the near future, many diseases could be diagnosed with deep learning models without radiologist interpretations and invasive examinations such as histopathological examinations. However, further studies with much larger case series are needed to develop accurate deep-learning models.






Similar content being viewed by others
References
Ariji Y, Sugita Y, Nagao T, Nakayama A, Fukuda M, Kise Y, Nozawa M, Nishiyama M, Katumata A, Ariji E (2020) CT evaluation of extranodal extension of cervical lymph node metastases in patients with oral squamous cell carcinoma using deep learning classification. Oral Radiol 36(2):148–155. https://doi.org/10.1007/s11282-019-00391-4
McBee MP, Awan OA, Colucci AT, Ghobadi CW, Kadom N, Kansagra AP, Tridandapani S, Auffermann WF (2018) Deep learning in radiology. Acad Radiol 25(11):1472–1480. https://doi.org/10.1016/j.acra.2018.02.018
Langlotz CP, Allen B, Erickson BJ, Kalpathy-Cramer J, Bigelow K, Cook TS, Flanders AE, Lungren MP, Mendelson DS, Rudie JD, Wang G, Kandarpa K (2019) A roadmap for foundational research on artificial intelligence in medical imaging: from the 2018 NIH/RSNA/ACR/The Academy Workshop. Radiology 291(3):781–791. https://doi.org/10.1148/radiol.2019190613
Kann BH, Aneja S, Loganadane GV, Kelly JR, Smith SM, Decker RH, Yu JB, Park HS, Yarbrough WG, Malhotra A, Burtness BA, Husain ZA (2018) Pretreatment identification of head and neck cancer nodal metastasis and extranodal extension using deep learning neural networks. Sci Rep 8(1):1–11. https://doi.org/10.1038/s41598-018-32441-y
LeCun Y, Bengio Y, Hinton GJ (2015) Deep learning. Nature 521(7553):436–444. https://doi.org/10.1038/nature14539
Simonyan K, Zisserman AJ (2014) Very deep convolutional networks for large-scale image recognition. Cornell University. arXiv:1409.1556
Moeckelmann N, Ebrahimi A, Tou YK, Gupta R, Low T-HH, Ashford B, Ch’ng S, Palme CS, Clark JR (2018) Prognostic implications of the 8th edition American Joint Committee on Cancer (AJCC) staging system in oral cavity squamous cell carcinoma. Oral Oncol 85:82–86. https://doi.org/10.1016/j.oraloncology.2018.08.013
Zoumalan R, Kleinberger A, Morris L, Ranade A, Yee H, DeLacure M, Myssiorek D (2010) Lymph node central necrosis on computed tomography as predictor of extracapsular spread in metastatic head and neck squamous cell carcinoma: pilot study. J Laryngol Otol 124(12):1284–1288. https://doi.org/10.1017/S0022215110001453
Som PM, Curtin HD (2011). Head and neck imaging E-Book: Elsevier Health Sciences. ISBN 978-0-323-05355-6
Zhao X, Xie P, Wang M, Li W, Pickhardt PJ, Xia W, Xiong F, Zhang R, Xie Y, Jian J, Bai H, Ni C, Gu J, Yu T, Tang Y, Gao X, Meng X (2020) Deep learning–based fully automated detection and segmentation of lymph nodes on multiparametric-mri for rectal cancer: a multicentre study. EBioMedicine 56:102780. https://doi.org/10.1016/j.ebiom.2020.102780
Tekchandani H, Verma S, Londhe ND, Jain RR, Tiwari AJBSP (2022) Computer aided diagnosis system for cervical lymph nodes in CT images using deep learning. Biomed Signal Process Control 71:103158. https://doi.org/10.1016/j.bspc.2021.103158
Tharwat AJA (2021) Classification assessment methods. Emerald insight. Informatics 17(1):168–92. https://www.emerald.com/insight/2210-8327.htm
Weiss K, Khoshgoftaar TM, Wang D (2016) A survey of transfer learning. J Big Data 3(1):1–40. https://doi.org/10.1186/s40537-016-0043-6
Sokolova M, Japkowicz N, Szpakowicz S (eds) (2006) Beyond accuracy, F-score and ROC: a family of discriminant measures for performance evaluation. AI 2006: advances in artificial intelligence: 19th Australian joint conference on artificial intelligence, Hobart, Australia, December 4–8, 2006 Proceedings 19. Springer
Torrey L, Shavlik J (2010) Transfer learning. Handbook of research on machine learning applications and trends: algorithms, methods, and techniques. IGI Glob. https://doi.org/10.4018/978-1-60566-766-9.ch011
Selvaraju RR, Cogswell M, Das A, Vedantam R, Parikh D, Batra D (eds) (2017) Grad-cam: visual explanations from deep networks via gradient-based localization. In: Proceedings of the IEEE international conference on computer vision (ICCV), pp 618-626
Castelijns JA, van den Brekel MW (2002) Imaging of lymphadenopathy in the neck. Eur Radiol 12:727–738. https://doi.org/10.1007/s003300101102
Lukić S, Marjanović G, Živanović J (2011) Palpable Lymphadenopathy in primary care. Acta Fac Med Naissensis 28(1):17–23
Friedmann AM (2008) Evaluation and management of lymphadenopathy in children. Pediatr Rev 29(2):53. https://doi.org/10.1542/pir.29-2-53
Ludwig BJ, Wang J, Nadgir RN, Saito N, Castro-Aragon I, Sakai OJ (2012) Imaging of cervical lymphadenopathy in children and young adults. Am J Roentgenol 199(5):1105–1113. https://doi.org/10.2214/AJR.12.8629
Twist CJ, Link MP (2002) Assessment of lymphadenopathy in children. Pediatr Clin N Am 49(5):1009–1025. https://doi.org/10.1016/S0031-3955(02)00038-X
Neff L, Newland JG, Sykes KJ, Selvarangan R, Wei JL (2013) Microbiology and antimicrobial treatment of pediatric cervical lymphadenitis requiring surgical intervention. Int J Pediatr Otorhinolaryngol 77(5):817–820. https://doi.org/10.1016/j.ijporl.2013.02.018
Zhang W, Peng J, Zhao S, Wu W, Yang J, Ye J, Xu S (2022) Deep learning combined with radiomics for the classification of enlarged cervical lymph nodes. J Cancer Res Clin Oncol 148(10):2773–2780. https://doi.org/10.1007/s00432-022-04047-5
Ariji Y, Kise Y, Fukuda M, Kuwada C, Ariji E (2022) Segmentation of metastatic cervical lymph nodes from CT images of oral cancers using deep-learning technology. Dentomaxillofac Radiol 51(4):20210515. https://doi.org/10.1259/dmfr.20210515
Zhou Z, Chen L, Sher D, Zhang Q, Shah J, Pham N-L, Jiang S, Wang J (eds) (2018) Predicting lymph node metastasis in head and neck cancer by combining many-objective radiomics and 3-dimensioal convolutional neural network through evidential reasoning. 2018 40th annual international conference of the IEEE engineering in medicine and biology society (EMBC). IEEE
Seidler M, Forghani B, Reinhold C, Pérez-Lara A, Romero-Sanchez G, Muthukrishnan N, Wichmann JL, Melki G, Yu E, Forghani R (2019) Dual-energy CT texture analysis with machine learning for the evaluation and characterization of cervical lymphadenopathy. Comput Struct Biotechnol J 17:1009–1015. https://doi.org/10.1016/j.csbj.2019.07.004
Courot A, Cabrera DL, Gogin N, Gaillandre L, Rico G, Zhang-Yin J, Elhaik M, Bidault F, Bousaid I, Lassau N (2021) Automatic cervical lymphadenopathy segmentation from CT data using deep learning. Diagn Interv Imaging 102(11):675–681. https://doi.org/10.1016/j.diii.2021.04.009
Tomita H, Yamashiro T, Heianna J, Nakasone T, Kobayashi T, Mishiro S, Hirahara D, Takaya E, Mimura H, Murayama S, Kobayashi Y (2021) Deep learning for the preoperative diagnosis of metastatic cervical lymph nodes on contrast-enhanced computed tomography in patients with oral squamous cell carcinoma. Cancers 13(4):600. https://doi.org/10.3390/cancers13040600
Kann BH, Aneja S, Loganadane GV, Kelly JR, Smith SM, Decker RH, Yu JB, Park HS, Yarbrough WG, Malhotra A, Burtness BA, Husain ZA (2018) Pretreatment identification of head and neck cancer nodal metastasis and extranodal extension using deep learning neural networks. Sci Rep 8(1):14036. https://doi.org/10.1038/s41598-018-32441-y
Onoue K, Fujima N, Andreu-Arasa VC, Setty BN, Sakai OJ (2021) Cystic cervical lymph nodes of papillary thyroid carcinoma, tuberculosis and human papillomavirus positive oropharyngeal squamous cell carcinoma: utility of deep learning in their differentiation on CT. Am J Otolaryngol 42(5):103026. https://doi.org/10.1016/j.amjoto.2021.103026
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no funding, financial relationships, or conflicts of interest to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Can, S., Türk, Ö., Ayral, M. et al. Can deep learning replace histopathological examinations in the differential diagnosis of cervical lymphadenopathy?. Eur Arch Otorhinolaryngol 281, 359–367 (2024). https://doi.org/10.1007/s00405-023-08181-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-023-08181-9