Abstract
Purpose
To assess risk factors of patients with oropharyngeal squamous cell carcinoma in the Munich area of Southern Germany in relation to human papillomavirus (HPV) association of the tumors. To demonstrate differences in tumor characteristics and their impact on adjuvant treatment.
Methods
Between November 2010 and July 2013, patients were prospectively interviewed for risk factors before they underwent surgical resection of their tumors. HPV association was evaluated by p16 immunohistochemistry; tumor characteristics and type of adjuvant treatment were recorded. Follow-up data were collected after a median follow-up of 12.1 month.
Results
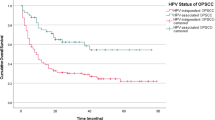
In contrast to many recent studies, we could not detect any difference in overall age and age at sexual debut between p16-positive and p16-negative patients. P16-negative patients are characterized by a more intensive tobacco and alcohol use, a more abusive way of consumption, less nonoral and less oral sex partners. P16-positive patients had a significantly higher risk of lymph node metastases, but nevertheless a significant lower risk to recur or to die. No difference in the incidence of synchronous second primary tumors was seen. P16-positive patients generally received a more aggressive adjuvant treatment because of more frequently involved lymph nodes.
Conclusion
Lifestyle risk factors such as smoking, drinking, and sexual habits were independent from age, but showed marked differences between the p16-positive and p16-negative group. Since p16-positive patients were treated more aggressively, it is not possible to distinguish whether the better outcome of HPV-positive patients is a result of less aggressive cancers or more aggressive treatment. With regard to the ongoing debate about treatment deintensification, we should keep in mind that the survival of HPV-positive cancer patients is not 100 %.

Similar content being viewed by others
References
Alicandri-Ciufelli M, Bonali M, Piccinini A, Marra L, Ghidini A, Cunsolo EM, Maiorana A, Presutti L, Conte PF (2013) Surgical margins in head and neck squamous cell carcinoma: what is ‘close’? Eur Arch Otorhinolaryngol 270:2603–2609
Ang KK, Sturgis EM (2012) Human papillomavirus as a marker of the natural history and response to therapy of head and neck squamous cell carcinoma. Semin Radiat Oncol 22:128–142
Attner P, Du J, Näsman A, Hammarstedt L, Ramqvist T, Lindholm J, Marklund L, Dalianis T, Munck-Wikland E (2010) The role of human papillomavirus in the increased incidence of base of tongue cancer. Int J Cancer 126:2879–2884
Auluck A, Hslop G, Bajdik C, Poh C, Zhang L, Rosin M (2010) Trends in oropharyngeal and oral cavity cancer incidences of human papillomavirus (HPV)-related and HPV-unrelated sites in a multicultural population: the British Columbia experience. Cancer 116:2635–2644
Bajos N, Bozon M, Beltzer N, Laborde C, Andro A, Ferrand M, Goulet V, Laporte A, Le Van C, Leridon H, Levinson S, Razafindratsima N, Toulemon L, Warszawski J, Wellings K (2010) Changes in sexual behaviours: from secular trends to public health policies. AIDS 24:1185–1191
Benard VB, Johnson CJ, Thompson TD, Roland KB, Lai SM, Cokkinides V, Tangka F, Hawkins NA, Lawson H, Weir HK (2008) Examining the association between socioeconomic status and potential human papillomavirus-associated cancers. Cancer 113:2910–2918
Boscolo-Rizzo P, Del Mistro A, Bussu F, Lupato V, Baboci L, Almadori G, Da Mosto MC, Paludetti G (2013) New insights into human papillomavirus-associated head and neck squamous cell carcinoma. Acta Otorhinolaryngol Ital 33:77–87
Brotherston DC, Poon I, Le T, Leung M, Kiss A, Ringash J, Balogh J, Lee J, Wright JR (2013) Patient preferences for oropharyngeal cancer treatment de-escalation. Head Neck 35:151–159
Chaturvedi AK (2012) Epidemiology and clinical aspects of HPV in head and neck cancers. Head Neck Pathol 6:S16–S24
Chaturvedi AK, Engels EA, Anderson WF, Gillison ML (2008) Incidence trends form human papillomavirus-related and -unrelated oral squamous cell carcinomas in the United States. J Clin Oncol 26:612–619
Chaturvedi AK, Engels EA, Pfeiffer RM, Hernandez BY, Xiao W, Kim E, Jiang B, Goodman MT, Sibug-Saber M, Cozen W, Liu L, Lynch CF, Wentzensen N, Jordan RC, Altekruse S, Anderson WF, Rosenberg PS, Gillison ML (2011) Human papillomavirus and rising oropharyngeal cancer incidence in the United States. J Clin Oncol 29:4294–4301
Chung CH, Gillison ML (2009) Human papillomavirus in head and neck cancer: its role in pathogenesis and clinical implications. Clin Cancer Res 15:6758–6762
D’Souza G, Kreimer AR, Viscidi R, Pawlita M, Fakhry C, Koch WM, Westra WH, Gillison ML (2007) Case-control study of human papillomavirus and oropharyngeal cancer. N Engl J Med 356:1944–1956
Fischer CA, Zlobec I, Green E, Probst S, Storck C, Lugli A, Tornillo L, Wolfensberger M, Terracciano LM (2010) Is the improved prognosis of p16 positive oropharyngeal squamous cell carcinoma dependent of the treatment modality? Int J Cancer 126:1256–1262
Gillison ML, Koch WM, Capone RB, Spafford M, Westra WH, Wu L, Zahurak ML, Daniel RW, Viglione M, Symer DE, Shah KV, Sidransky D (2000) Evidence for a causal association between human papillomavirus and a subset of head and neck cancers. J Natl Cancer Inst 92:709–720
Hammarstedt L, Lindquist D, Dahlstrand H, Romanitan M, Dahlgren LO, Joneberg J, Creson N, Lindholm J, Ye W, Dalianis T, Munck-Wikland E (2006) Human papillomavirus as a risk factor for the increase in incidence of tonsillar cancer. Int J Cancer 119:2620–2623
Haughey BH, Sinha P (2012) Prognostic factors and survival unique to surgically treated p16+ oropharyngeal cancer. Laryngoscope 122:S13–S33
Herbenick D, Reece M, Schick V, Sanders SA, Dodge B, Fortenberry JD (2010) Sexual behavior in the United States: results from a national probability sample of men and women ages 14–94. J Sex Med 7:S255–S265
Hocking JS, Stein A, Conway EL, Regan D, Grulich A, Law M, Brotherton JM (2011) Head and neck cancer in Australia between 1982 and 2005 show increasing incidence of potentially HPV-associated oropharyngeal cancers. Br J Cancer 104:886–891
Huang SH, Perez-Ordonez B, Weinreb I, Hope A, Massey C, Waldron JN, Kim J, Bayley AJ, Cummings B, Cho BC, Ringash J, Dawson LA, Siu LL, Chen E, Irish J, Gullane P, Hui A, Liu FF, Shen X, Xu W, O’Sullivan B (2013) Natural course of distant metastases following radiotherapy or chemoradiotherapy in HPV-related oropharyngeal cancer. Oral Oncol 49:79–85
Jain KS, Sikora AG, Baxi SS, Morris LG (2013) Synchronous cancers in patients with head and neck cancer: risks in the era of human papillomavirus-associated oropharyngeal cancer. Cancer 119:1832–1837
Joseph AW, Ogawa T, Bishop JA, Lyford-Pike S, Chang X, Phelps TH, Westra WH, Pai SI (2013) Molecular etiology of second primary tumors in contralateral tonsils of human papillomavirus-associated index tonsillar carcinomas. Oral Oncol 49:244–248
Klozar J, Koslabova E, Kratochvil V, Salakova M, Tachezy R (2013) Nodal status is not a prognostic factor in patients with HPV-positive oral/oropharyngeal tumors. J Surg Oncol 107:625–633
Klussmann JP, Weissenborn SJ, Wieland U, Dries V, Kolligs J, Jungehuelsing M, Eckel HE, Dienes HP, Pfister HJ, Fuchs PG (2001) Prevalence, distribution, and viral load of human papillomavirus 16 DNA in tonsillar carcinomas. Cancer 92:2875–2884
Kreimer AR, Alberg AJ, Daniel R, Gravitt PE, Viscidi R, Garrett ES, Shah KV, Gillison ML (2004) Oral human papillomavirus infection in adults is associated with sexual behavior and HIV serostatus. J Infect Dis 189:686–698
Kreimer AR, Clifford GM, Boyle P, Franceschi S (2005) Human papillomavirus in head and neck squamous cell carcinoma worldwide: a systematic review. Cancer Epidemiol Biomarkers Prev 14:467–475
Lewis JS Jr (2012) p16 Immunohistochemistry as a standalone test for risk stratification in oropharyngeal squamous cell carcinoma. Head Neck Pathol 6:S75–S82
Mackay J (2001) Global sex: sexuality and sexual practices around the world. Sex Relation Ther 16:71–82
Maxwell JH, Kumar B, Feng FY, Worden FP, Lee JS, Eisbruch A, Wolf GT, Prince ME, Moyer JS, Teknos TN, Chepeha DB, McHugh JB, Urba SG, Stoerker J, Walline HM, Kurnit DM, Cordell KG, Davis SJ, Ward PD, Bradford CR, Carey TE (2010) Tobacco use in human papillomavirus-positive advanced oropharynx cancer patients related to increased risk of distant metastases and tumor recurrence. Clin Cancer Res 16:1226–1235
Moody CA, Laimins LA (2010) Human papillomavirus oncoproteins: pathways to transformation. Nat Rev Cancer 10:550–560
Näsman A, Attner P, Hammarstedt L, Du J, Eriksson M, Giraud G, Ahrlund-Richter S, Marklund L, Romanitan M, Lindquist D, Ramqvist T, Lindholm J, Sparén P, Ye W, Dahlstrand H, Munck-Wikland E, Dalianis T (2009) Incidence of human papillomavirus (HPV) positive tonsillar carcinoma in Stockholm, Sweden: an epidemic of viral-induced carcinoma? Int J Cancer 125:362–366
O’Brien CJ, Smith HW, Soong SJ, Urist MM, Maddox WA (1986) Neck dissection with and without radiotherapy—prognostic factors, patterns of recurrence and survival. Am J Surg 152:456–463
O’Sullivan B, Huang SH, Siu LL, Waldron J, Zhao H, Perez-Ordonez B, Weinreb I, Kim J, Ringash J, Bayley A, Dawson LA, Hope A, Cho J, Irish J, Gilbert R, Gullane P, Hui A, Liu FF, Chen E, Xu W (2013) Deintensification candidate subgroups in human papillomavirus-related oropharyngeal cancer according to minimal risk of distant metastasis. J Clin Oncol 31:543–550
Peck BW, Dahlstrom KR, Gan SJ, Caywood W, Li G, Wei Q, Zafereo ME, Sturgis EM (2013) Low risk of second primary malignancies among never smokers with human papillomavirus-associated index oropharyngeal cancers. Head Neck 35:151–159
Rosenquist K, Wennerberg J, Schildt EB, Bladström A, Göran Hansson B, Andersson G (2005) Oral status, oral infections and some lifestyle factors as risk factors for oral and oropharyngeal squamous cell carcinoma: a population-based case-control study in southern Sweden. Acta Otolaryngol 125:1327–1336
Rowe Price KA, Okuno SH, Garcia JJ, Molina JR, Olsen KD, Kasperbauer JC, Price DL, Garces YI, Ma D, Nebe-Wittich MA, Shull SE, Foote RL, Moore EJ (2013) Survival in patients with HPV-positive oropharynx squamous cell carcinoma with distant metastases. J Clin Oncol 31(suppl; abstr.6095)
Sinha P, Lewis JS Jr, Piccirillo JF, Kallogjeri D, Haughey BH (2012) Extracapsular spread and adjuvant therapy in human papillomavirus-related, p16-positive oropharyngeal carcinoma. Cancer 118:3519–3530
Sinha P, Thorstad WT, Nussenbaum B, Haughey BH, Adkins DR, Kallogjeri D, Lewis JS Jr (2014) Distant metastasis in p16-positive oropharyngeal squamous cell carcinoma: a critical analysis of patterns and outcomes. Oral Oncol 50:45–51
Slaughter DO, Southwick HW, Smejkal W (1953) Field cancerization in oral stratified squamous epithelium; clinical implications of multicentric origin. Cancer 6:963–968
Tribius S, Hoffmann M (2013) Human papilloma virus infection in head and neck cancer. Dtsch Arztebl Int 110:184–190
Ukpo OC, Flanagan JJ, Ma XJ, Luo Y, Thorstad WL, Lewis JS Jr (2011) High-risk human papillomavirus E6/E7 mRNA detection by a novel in situ hybridization assay strongly correlates with p16 expression and patient outcomes in oropharyngeal squamous cell carcinoma. Am J Surg Pathol 35:1343–1350
Vent J, Haidle B, Wedemeyer I, Huebbers C, Siefer O, Semrau R, Preuss SF, Klussmann J (2013) p16 expression in carcinoma of unknown primary: diagnostic indicator and prognostic marker. Head Neck 35:1521–1526
Vermorken JB, Specenier P (2010) Optimal treatment for recurrent/metastatic head and neck cancer. Ann Oncol 21:S252–S261
Xu CC, Biron VL, Puttagunta L, Seikaly H (2013) HPV status and second primary tumours in oropharyngeal squamous cell carcinoma. J Otolaryngol Head Neck Surg 42:36
Zengel P, Assmann G, Mollenhauer M, Jung A, Sotlar K, Kirchner T, Ihrler S (2012) Cancer of unknown primary originating from oropharyngeal carcinomas are strongly correlated to HPV positivity. Virchows Arch 461:283–290
Conflict of interest
No conflicts of interest to be stated.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Baumeister, P., Reiter, M., Welz, C. et al. Surgically treated oropharyngeal cancer: risk factors and tumor characteristics. J Cancer Res Clin Oncol 140, 1011–1019 (2014). https://doi.org/10.1007/s00432-014-1631-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-014-1631-5