Abstract
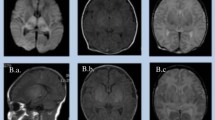
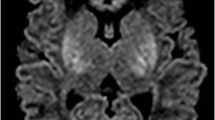
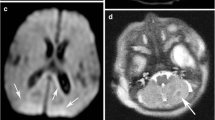
Hypoglycemia is common among neonates and can cause neurological dysfunction. This study aimed to identify the specific time window to perform diffusion-weighted imaging (DWI) for detecting early brain injury in neonatal hypoglycemia and assess the clinical characteristics and neurological outcomes of different patterns of brain injury in neonatal hypoglycemia. We conducted a retrospective analysis of the changes in conventional magnetic resonance imaging (MRI) and DWI at different time points and clinical characteristics in 86 neonates with hypoglycemic brain injury. Among 139 DWI scans, 84 showed injury site hyperintensities within 7 days after hypoglycemia. Thirty-nine scans revealed low DWI and abnormal T1-/T2-weighted imaging signals within 11–23 days after onset, of which 21 showed DWI hyperintensities in the corpus callosum. Abnormal signals were undetected in the second scans of 13 infants within 9–20 days after onset. Vulnerable sites comprised the occipital lobe (98%), splenium of the corpus callosum (60%), and parietal lobe (30%). Compared with focal injury (n = 66), extensive injury (n = 20) had higher involvement of the internal capsule, basal ganglia, and thalamus (P < 0.05); higher incidence of recurrent convulsions, respiratory failure, and coma (P < 0.01); and a higher proportion of death and severe neurodevelopmental impairment (P < 0.05).
Conclusions: Neonatal hypoglycemic brain injury was most common in the occipital lobes. Severe clinical symptoms were significantly associated with extensive brain injury involving the internal capsule, basal ganglia, and thalamus, which could be attributed to hypoxia–ischemia and lead to a poor prognosis.
What is Known: • There is no clear neurological safe threshold for hypoglycemia in neonates. Studies suggest that symptomatic hypoglycemia can be related to brain injury. | |
What is New: • Severe clinical symptoms are significantly associated with extensive brain injury on MRI scans. Extensive brain injuries involving the internal capsule, basal ganglia, and thalamus, which could be due to associated hypoxia–ischemia and lead to a poor prognosis. |



Similar content being viewed by others
Data availability
The original contributions generated for this study are included in the article/supplementary materials; further inquiries can be directed to the corresponding author.
Abbreviations
- DWI:
-
Diffusion-weighted imaging
- HIE:
-
Hypoxic–ischemic encephalopathy
- MRI:
-
Magnetic resonance imaging
- NDI:
-
Neurodevelopmental impairment
References
Dani C, Corsini I (2020) Guidelines for management of neonatal hypoglycemia: are they actually applicable? JAMA Pediatr 174:638–639. https://doi.org/10.1001/jamapediatrics.2020.0632
McKinlay CJD, Alsweiler JM, Anstice NS, Burakevych N, Chakraborty A, Chase JG, Gamble GD, Harris DL, Jacobs RJ, Jiang Y, Paudel N, San Diego RJ, Thompson B, Wouldes TA, Harding JE (2017) Children With Hypoglycemia and Their Later Development (CHYLD) Study Team. Association of neonatal glycemia with neurodevelopmental outcomes at 4.5 Years. JAMA Pediatr 171:972–983. https://doi.org/10.1001/jamapediatrics.2017.1579
Tin W (2014) Defining neonatal hypoglycaemia: a continuing debate. Semin Fetal Neonatal Med 19:27–32. https://doi.org/10.1016/j.siny.2013.09.003
Tam EW, Widjaja E, Blaser SI, Macgregor DL, Satodia P, Moore AM (2008) Occipital lobe injury and cortical visual outcomes after neonatal hypoglycemia. Pediatrics 122:507–512. https://doi.org/10.1542/peds.2007-2002
Filan PM, Inder TE, Cameron FJ, Kean MJ, Hunt RW (2006) Neonatal hypoglycemia and occipital cerebral injury. J Pediatr 148:552–555. https://doi.org/10.1016/j.jpeds.2005.11.015
Yalnizoglu D, Haliloglu G, Turanli G, Cila A, Topcu M (2007) Neurologic outcome in patients with MRI pattern of damage typical for neonatal hypoglycemia. Brain Dev 29:285–292. https://doi.org/10.1016/j.braindev.2006.09.011
Alkalay AL, Flores-Sarnat L, Sarnat HB, Moser FG, Simmons CF (2005) Brain imaging findings in neonatal hypoglycemia: case report and review of 23 cases. Clin Pediatr (Phila) 44:783–790. https://doi.org/10.1177/000992280504400906
Banker BQ (1967) The neuropathological effects of anoxia and hypoglycemia in the newborn. Dev Med Child Neurol 9:544–550. https://doi.org/10.1111/j.1469-8749.1967.tb02323.x
Burns CM, Rutherford MA, Boardman JP, Cowan FM (2008) Patterns of cerebral injury and neurodevelopmental outcomes after symptomatic neonatal hypoglycemia. Pediatrics 122:65–74. https://doi.org/10.1542/peds.2007-2822
Inder T (2008) How low can I go? The impact of hypoglycemia on the immature brain. Pediatrics 122:440–441. https://doi.org/10.1542/peds.2008-1417
Parmentier CEJ, de Vries LS, van der Aa NE, Eijsermans MJC, Harteman JC, Lequin MH, Swanenburg de Veye HFN, Koopman-Esseboom C, Groenendaal F (2022) Hypoglycemia in infants with hypoxic-ischemic encephalopathy is associated with additional brain injury and worse neurodevelopmental outcome. J Pediatr 245:30-38.e1. https://doi.org/10.1016/j.jpeds.2022.01.051
Boardman JP, Hawdon JM (2015) Hypoglycaemia and hypoxic-ischaemic encephalopathy. Dev Med Child Neurol 57(Suppl 3):29–33. https://doi.org/10.1111/dmcn.12729
Wong DS, Poskitt KJ, Chau V, Miller SP, Roland E, Hill A, Tam EW (2013) Brain injury patterns in hypoglycemia in neonatal encephalopathy. AJNR Am J Neuroradiol 34:1456–1461. https://doi.org/10.3174/ajnr.A3423
De Angelis LC, Brigati G, Polleri G, Malova M, Parodi A, Minghetti D, Rossi A, Massirio P, Traggiai C, Maghnie M, Ramenghi LA (2021) Neonatal hypoglycemia and brain vulnerability. Front Endocrinol (Lausanne) 12:634305. https://doi.org/10.3389/fendo.2021.634305
Bayley N (1993) Manual for the Bayley scales of infant development, 2nd edn. Psychological Corporation, San Antonio, TX
Onder H (2016) Reversible diffusion restriction in the splenium of the corpus callosum due to severe hypoglycemia: a case report and literature review. J Neuroradiol 43:419–421. https://doi.org/10.1016/j.neurad.2016.05.005
Maruya J, Endoh H, Watanabe H, Motoyama H, Abe H (2007) Rapid improvement of diffusion-weighted imaging abnormalities after glucose infusion in hypoglycaemic coma. J Neurol Neurosurg Psychiatry 78:102–103. https://doi.org/10.1136/jnnp.2006.096776
Landais A (2015) Reversible splenium diffusion weighted MRI changes associated with hypoglycemia. J Diabetes Complications 29:607–610. https://doi.org/10.1016/j.jdiacomp.2015.02.012
Kim JH, Koh SB (2007) Extensive white matter injury in hypoglycemic coma. Neurology 68:1074. https://doi.org/10.1212/01.wnl.0000258546.83251.36
Righini A, Doneda C, Parazzini C, Arrigoni F, Matta U, Triulzi F (2010) Diffusion tensor imaging of early changes in corpus callosum after acute cerebral hemisphere lesions in newborns. Neuroradiology 52:1025–1035. https://doi.org/10.1007/s00234-010-0745-y
Epelman M, Daneman A, Halliday W, Whyte H, Blaser SI (2012) Abnormal corpus callosum in neonates after hypoxic-ischemic injury. Pediatr Radiol 42:321–330. https://doi.org/10.1007/s00247-011-2238-5
Wagenaar N, Chau V, Groenendaal F, Kersbergen KJ, Poskitt KJ, Grunau RE, Synnes A, Duerden EG, de Vries LS, Miller SP, Benders MJNL (2017) Clinical risk factors for punctate white matter lesions on early magnetic resonance imaging in preterm newborns. J Pediatr 182:34-40.e1. https://doi.org/10.1016/j.jpeds.2016.11.073
Kelly CJ, Arulkumaran S, Tristão Pereira C, Cordero-Grande L, Hughes EJ, Teixeira RPAG, Steinweg JK, Victor S, Pushparajah K, Hajnal JV, Simpson J, Edwards AD, Rutherford MA, Counsell SJ (2019) Neuroimaging findings in newborns with congenital heart disease prior to surgery: an observational study. Arch Dis Child 104:1042–1048. https://doi.org/10.1136/archdischild-2018-314822
de Courten-Myers GM, Xi G, Hwang JH, Dunn RS, Mills AS, Holland SK, Wagner KR, Myers RE (2000) Hypoglycemic brain injury: potentiation from respiratory depression and injury aggravation from hyperglycemic treatment overshoots. J Cereb Blood Flow Metab 20:82–92. https://doi.org/10.1097/00004647-200001000-00012
Auer RN, Siesjö BK (1993) Hypoglycaemia: brain neurochemistry and neuropathology. Baillieres Clin Endocrinol Metab 7:611–625. https://doi.org/10.1016/s0950-351x(05)80210-1
Kim DE, Park SH, Kim SK, Nam HW, Lee YS, Chung JK, Roh JK (2000) Hypoglycemia-induced cerebellar dysfunction and quantitative positron emission tomography study. Neurology 55:418–422. https://doi.org/10.1212/wnl.55.3.418
Johkura K, Nakae Y, Kudo Y, Yoshida TN, Kuroiwa Y (2012) Early diffusion MR imaging findings and short-term outcome in comatose patients with hypoglycemia. AJNR Am J Neuroradiol 33:904–909. https://doi.org/10.3174/ajnr.A2903
Yoneda Y, Yamamoto S (2005) Cerebral cortical laminar necrosis on diffusion-weighted MRI in hypoglycaemic encephalopathy. Diabet Med 22:1098–1100. https://doi.org/10.1111/j.1464-5491.2005.01568.x
Thompson-Branch A, Havranek T (2017) Neonatal hypoglycemia. Pediatr Rev 38:147–157. https://doi.org/10.1542/pir.2016-0063
Thornton PS, Stanley CA, De Leon DD, Harris D, Haymond MW, Hussain K, Levitsky LL, Murad MH, Rozance PJ, Simmons RA, Sperling MA, Weinstein DA, White NH, Wolfsdorf JI (2015) Pediatric Endocrine Society. Recommendations from the pediatric endocrine society for evaluation and management of persistent hypoglycemia in neonates, infants, and children. J Pediatr 167:238–245. https://doi.org/10.1016/j.jpeds.2015.03.057
Stanley CA, Rozance PJ, Thornton PS, De Leon DD, Harris D, Haymond MW, Hussain K, Levitsky LL, Murad MH, Simmons RA, Sperling MA, Weinstein DA, White NH, Wolfsdorf JI (2015) Re-evaluating “transitional neonatal hypoglycemia”: mechanism and implications for management. J Pediatr 166:1520–5.e1. https://doi.org/10.1016/j.jpeds.2015.02.045
Acknowledgements
We want to appreciate the radiologists of the Shengjing Hospital for their support and help in reassessing the head magnetic resonance imaging scans.
Author information
Authors and Affiliations
Contributions
Yi Zhang and Jian Mao contributed to the study conception and design. Yi Zhang, Dan Chen, Yalian Ji, and Wenting Yu performed the material preparation, data collection, and analysis. Yi Zhang wrote the first draft of the manuscript, and all authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki. The study design was approved by the ethics committee of Shengjing Hospital (approval no: 2020PS609K).
Consent to participate
The need for informed consent was waived because of the study’s retrospective nature. Parental consent was obtained for the magnetic resonance imaging examinations.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Communicated by Daniele De Luca
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhang, Y., Chen, D., Ji, Y. et al. Dynamic magnetic resonance imaging findings in the early stages of neonatal hypoglycemic brain injury. Eur J Pediatr 181, 4167–4174 (2022). https://doi.org/10.1007/s00431-022-04637-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-022-04637-y