Abstract
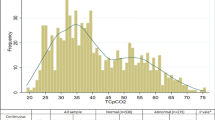
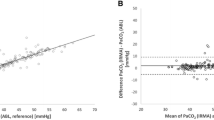
Our objective was to assess within a feasibility study the correlation and agreement of transcutaneous carbon dioxide (PtcCO2) monitoring with venous carbon dioxide (PvCO2) in infants with bronchiolitis in the emergency room (ER) and pediatric department. Sixty infants (aged 3.6 ± 3.3 months) admitted to our ER with bronchiolitis were included. PtcCO2 measurements (SenTec Digital Monitoring System) collected prospectively were compared with simultaneous PvCO2 drawn for patient care. Analysis included 100 measurements. The correlation of PtcCO2 and PvCO2 (r = 0.71, p < 0.001) was good, and the agreement (mean difference ± standard deviation of the differences 1.9 ± 7.0 mmHg) was adequate; average PtcCO2 was slightly lower than PvCO2. Changes in PtcCO2 and PvCO2 for consecutive measurements within each patient correlated (r = 0.41, p < 0.01). The level of PtcCO2 correlated with disease severity clinical score (p < 0.001).
Conclusions: PtcCO2 monitoring was feasible in the ER and pediatric department and was found to have a good correlation and adequate agreement with PvCO2 in infants with bronchiolitis. Because the standard deviation of the differences was relatively high, though comparable to the literature, we suggest that PtcCO2 should not replace blood gas but rather serve as a complementary tool for trending and for real-time continuous assessment of the CO2 levels.


Similar content being viewed by others
Abbreviations
- ABG:
-
Arterial blood gas
- PtcCO2 :
-
Transcutaneous carbon dioxide
- VBG:
-
Venous blood gas
References
Abboud PA, Roth PJ, Skiles CL, Stolfi A, Rowin ME (2012) Predictors of failure in infants with viral bronchiolitis treated with high-flow, high-humidity nasal cannula therapy*. Pediatr Criti Care Med 13:e343–e349. doi:10.1097/PCC.0b013e31825b546f
Bar A, Srugo I, Amirav I, Tzverling C, Naftali G, Kugelman A (2008) Inhaled furosemide in hospitalized infants with viral bronchiolitis: a randomized, double-blind, placebo-controlled pilot study. Pediatr Pulmonol 43:261–267. doi:10.1002/ppul.20765
Bernet V, Doell C, Cannizzaro V, Ersch J, Frey B, Weiss M (2008) Longtime performance and reliability of two different PtcCO2 and SpO2 sensors in neonates. Pediatr Anesth 18:872–877
Bland MJ, Altman D (1986) Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 327:307–310
Bressan S, Balzani M, Krauss B, Pettenazzo A, Zanconato S, Baraldi E (2013) High-flow nasal cannula oxygen for bronchiolitis in a pediatric ward: a pilot study. Eur J Pediatr 172:1649–1656. doi:10.1007/s00431-013-2094-4
Carter B, Wiwczarukt D, Hochmann M, Osborne A, Henning R (2001) Performance of transcutaneous PCO2 and pulse oximetry monitors in newborns and infants after cardiac surgery. Anaesth Intens Care 29:260–265
Dullenkopf A, Bernardo SD, Berger F, Fasnacht M, Gerber AC, Weiss M (2003) Evaluation of a new combined SpO2/PtcCO2 sensor in anaesthetized paediatric patients. Pediatr Anesth 13:777–784
Gennis PR, Skovron ML, Aronson ST, Gallagher EJ (1985) The usefulness of peripheral venous blood in estimating acid-base status in acutely III patients. Ann Emerg Med 14:845–849
Hagerty JJ, Kleinman ME, Zurakowski D, Lyons AC, Krauss B (2002) Accuracy of a new low-flow sidestream capnography technology in newborns: a pilot study. J Perinatol 22:219–225. doi:10.1038/sj.jp.7210672
Harrison AM, Lynch JM, Dean JM, Witte MK (1997) Comparison of simultaneously obtained arterial and capillary blood gases in pediatric intensive care unit patients. Crit Care Med 25:1904–1908
Holmgren D, Sixt R (1992) Transcutaneous and arterial blood gas monitoring during acute asthmatic symptoms in older children. Pediat Pulmonol 14:80–84
Kelly GS, Simon HK, Sturm JJ (2013) High-flow nasal cannula use in children with respiratory distress in the emergency department: predicting the need for subsequent intubation. Pediatr Emerg Care 29:888–892. doi:10.1097/PEC.0b013e31829e7f2f
Kneyber MC, Brandenburg AH, de Groot R, Joosten KF, Rothbarth PH, Ott A, Moll HA (1998) Risk factors for respiratory syncytial virus associated apnoea. Eur J Pediatr 157:331–335
Kugelman A, Zeiger-Aginsky D, Bader D, Shoris I, Riskin A (2008) A novel method of distal end-tidal CO2 capnography in intubated infants: comparison with arterial CO2 and with proximal mainstream end-tidal CO2. Pediatrics 122:e1219–e1224. doi:10.1542/peds.2008-1300
Lacerenza S, De Carolis MP, Fusco FP, La Torre G, Chiaradia G, Romagnoli C (2008) An evaluation of a new combined Spo2/PtcCO2 sensor in very low birth weight infants. Anesth Analg 107:125–129. doi:10.1213/ane.0b013e3181733e47
Lashkeri T, Howell JM, Place R (2012) Capnometry as a predictor of admission in bronchiolitis. Pediatr Emerg Care 28:895–897
Lazner MR, Basu AP, Klonin H (2012) Non-invasive ventilation for severe bronchiolitis: analysis and evidence. Pediatr Pulmonol 47:909–916. doi:10.1002/ppul.22513
Lowell DI, Lister G, Von Koss H, McCarthy P (1987) Wheezing in infants: the response to epinephrine. Pediatrics 79:939–945
Marsden D, Chiu M, Paky F, Helms P (1985) Transcutaneous oxygen and carbon dioxide monitoring in intensive care. Arch Dis Child 60:1158–1161
Mayfield S, Bogossian F, O’Malley L, Schibler A (2014) High-flow nasal cannula oxygen therapy for infants with bronchiolitis: pilot study. J Paediatr Child Health 50:373–378. doi:10.1111/jpc.12509
Paiva R, Krivec U, Aubertin G, Cohen E, Clément A, Fauroux B (2009) Carbon dioxide monitoring during long-term noninvasive respiratory support in children. Intens Care Med 35:1068–1074
Palmisano BW, Severinghaus JW (1990) Transcutaneous PCO2 and PO2: a multicenter study of accuracy. J Clin Monit 6:189–195
Rozycki HJ, Sysyn GD, Marshall MK, Malloy R, Wiswell TE (1998) Mainstream end-tidal carbon dioxide monitoring in the neonatal intensive care unit. Pediatrics 101:648–653
Storre JH, Steurer B, Kabitz H-J, Dreher M, Windisch W (2007) Transcutaneous PCO2 monitoring during initiation of noninvasive ventilation. CHEST 132:1810–1816
Urbano J, Cruzado V, Lopez-Herce J, del Castillo J, Bellon JM, Carrillo A (2010) Accuracy of three transcutaneous carbon dioxide monitors in critically ill children. Pediatr Pulmonol 45:481–486. doi:10.1002/ppul.21203
Wennergren G, Engström I, Bjure J (1986) Transcutaneous oxygen and carbon dioxide levels and a clinical symptom scale for monitoring the acute asthmatic state in infants and young children. Acta Paediatr 75:465–469
Wilson J, Russo P, Russo J, Tobias JD (2005) Noninvasive monitoring of carbon dioxide in infants and children with congenital heart disease: end-tidal versus transcutaneous techniques. J Intens Care Med 20:291–295
Yıldızdaş D, Yapıcıoğlu H, Yılmaz H, Sertdemir Y (2004) Correlation of simultaneously obtained capillary, venous, and arterial blood gases of patients in a paediatric intensive care unit. Arch Dis Child 89:176–180
Acknowledgments
Funding source
No external funding was secured for this study.
Financial disclosure
SenTec Inc. supported the study by supplying a SenTec monitor and supplies for the study.
Conflict of interest
We have no conflicts of interest to disclose, and we had no financial relationship with the organization that sponsored the research.
Author information
Authors and Affiliations
Corresponding author
Additional information
Communicated by Peter de Winter
Rights and permissions
About this article
Cite this article
Gal, S., Riskin, A., Chistyakov, I. et al. Transcutaneous PCO2 monitoring in infants hospitalized with viral bronchiolitis. Eur J Pediatr 174, 319–324 (2015). https://doi.org/10.1007/s00431-014-2407-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-014-2407-2