Abstract
In chronic kidney disease (CKD), hyperphosphatemia promotes medial vascular calcification, a process augmented by osteogenic transdifferentiation of vascular smooth muscle cells (VSMCs). VSMC function is regulated by sympathetic innervation, and these cells express α- and β-adrenergic receptors. The present study explored the effects of β2-adrenergic stimulation by isoproterenol on VSMC calcification. Experiments were performed in primary human aortic VSMCs treated with isoproterenol during control or high phosphate conditions. As a result, isoproterenol dose dependently up-regulated the expression of osteogenic markers core-binding factor α-1 (CBFA1) and tissue-nonspecific alkaline phosphatase (ALPL) in VSMCs. Furthermore, prolonged isoproterenol exposure augmented phosphate-induced calcification of VSMCs. Isoproterenol increased the activation of PKA and CREB, while knockdown of the PKA catalytic subunit α (PRKACA) or of CREB1 genes was able to suppress the pro-calcific effects of isoproterenol in VSMCs. β2-adrenergic receptor silencing or inhibition with the selective antagonist ICI 118,551 blocked isoproterenol-induced osteogenic signalling in VSMCs. The present observations imply a pro-calcific effect of β2-adrenergic overstimulation in VSMCs, which is mediated, at least partly, by PKA/CREB signalling. These observations may support a link between sympathetic overactivity in CKD and vascular calcification.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
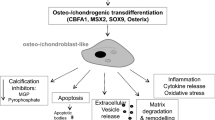
Chronic kidney disease (CKD) is associated with high mortality due to cardiovascular disease [23, 71]. The excessive cardiovascular risk in CKD patients may be fostered by medial vascular calcification [45, 71, 73], which promotes stiffening of vessels, subsequently leading to cardiac and circulatory dysfunctions [45, 71]. Vascular calcification is an active process involving transdifferentiation of vascular smooth muscle cells (VSMCs) into cells with some osteo-/chondroblast-like properties, characterized by expression of osteogenic transcription factors and enzymes [4, 15, 73]. Core-binding factor α-1 (CBFA1/RUNX2) is an osteogenic transcription factor essential for vascular calcification [60, 62], which induces expression of osteogenic enzymes, including tissue-nonspecific alkaline phosphatase (ALPL) [21, 62], a key effector of vascular mineralization [21, 73]. In CKD, hyperphosphatemia is considered the key pathological factor triggering osteogenic transdifferentiation of VSMCs and vascular calcification [73]. Nonetheless, additional pathological factors contribute to the regulation of vascular calcification in CKD [1,2,3, 28, 29, 56, 69, 75].
CKD has been considered a hyperadrenergic state [41] with sympathetic overactivity [13, 22, 42]. Sympathetic overactivity may be involved in the progression of renal disease and its cardiovascular complications [25, 34, 40, 55]. Chronic high sympathetic activity leads to overstimulation of adrenergic receptors promoting the development of cardiac and vascular diseases [52, 58, 66, 70]. Sympathetic blockade by stellate ganglion block reduces vascular calcification in a rat model [26]. Norepinephrine augments the calcification of VSMCs [26]. Besides α-adrenergic receptors associated with vasoconstriction, β-adrenergic receptors are expressed in VSMCs [18, 57, 63]. β2-adrenergic stimulation plays an important role in VSMC physiology and vascular dilation [12, 63]. β2-adrenergic signalling declines with increasing age, which has been discussed as a putative contributing factor for cardiovascular diseases in the elderly [57]. Furthermore, β2-adrenergic stimulation exhibits reno-protective effects [5]. However, the role of β-adrenergic overstimulation in the vasculature is less studied [68]. Chronic overstimulation of vascular β2-adrenergic receptors may induce oxidative stress and vascular dysfunction [16, 18].
Therefore, the present study explores a putative modulating role of β2-adrenergic activation by isoproterenol during phosphate-induced osteogenic transdifferentiation and calcification of VSMCs in vitro.
Materials and methods
Primary human aortic smooth muscle cells (HAoSMCs)
HAoSMCs (Fisher Scientific and Sigma-Aldrich) were routinely cultured as described previously [1, 28, 75] and used in experiments up to passage 12. N indicates the number of independent experiments performed at different passages of the cells. HAoSMCs were treated with the indicated concentrations or 1 μM isoproterenol (stock in PBS; Sigma-Aldrich) [70], 2 mM β-glycerophosphate (Sigma-Aldrich) [69, 74] or 1 μM ICI 118,551 (stock in DMSO; MedChemExpress) [78]. Equal amounts of vehicle were used as control. For calcification analysis, HAoSMCs were treated with calcification medium supplemented with 10 mM β-glycerophosphate and 1.5 mM CaCl2 (Sigma-Aldrich) [28, 75]. For long-term treatments, fresh medium with agents was added every 2–3 days. Where indicated, HAoSMCs were transfected with 10 nM PRKACA siRNA (ID:s11066), 10 nM CREB1 siRNA (ID:s3490), 10 nM ADRB2 siRNA (ID:s1122), or 10 nM negative control siRNA (ID:4390843) by using siPORT amine transfection agent (all from Fisher Scientific) [28].
RNA isolation and RT-PCR
Total RNA was isolated from HAoSMCs by using Trizol reagent (Fisher Scientific). cDNA was synthesized with SuperScript III Reverse Transcriptase and oligo(dT)12–18 primers (Fisher Scientific). RT-PCR was performed in duplicate with iQ™ Sybr Green Supermix (Bio-Rad Laboratories) and CFX96 Real-Time PCR Detection System (Bio-Rad Laboratories). The specificity of the PCR products was confirmed by analysis of the melting curves. Relative mRNA expression was calculated by the 2−ΔΔCt method using GAPDH as housekeeping gene, normalized to the control group. The following human primers were used (Fisher Scientific) [1, 28, 56, 76]:
-
ACTA2 fw: AAAAGACAGCTACGTGGGTGA
-
ACTA2 rev: GCCATGTTCTATCGGGTACTTC
-
ADRB1 fw: ATCGAGACCCTGTGTGTCATT
-
ADRB1 rev: GTAGAAGGAGACTACGGACGAG
-
ADRB2 fw: TGGTGTGGATTGTGTCAGGC
-
ADRB2 rev: GGCTTGGTTCGTGAAGAAGTC
-
ADRB3 fw: GACCAACGTGTTCGTGACTTC
-
ADRB3 rev: GCACAGGGTTTCGATGCTG
-
ALPL fw: GGGACTGGTACTCAGACAACG
-
ALPL rev: GTAGGCGATGTCCTTACAGCC
-
CBFA1 fw: GCCTTCCACTCTCAGTAAGAAGA
-
CBFA1 rev: GCCTGGGGTCTGAAAAAGGG
-
CD68 fw: CTTCTCTCATTCCCCTATGGACA
-
CD68 rev: GAAGGACACATTGTACTCCACC
-
CREB1 fw: CCACTGTAACGGTGCCAACT
-
CREB1 rev: GCTGCATTGGTCATGGTTAATGT
-
GAPDH fw: GAGTCAACGGATTTGGTCGT
-
GAPDH rev: GACAAGCTTCCCGTTCTCAG
-
LGALS3 fw: GTGAAGCCCAATGCAAACAGA
-
LGALS3 rev: AGCGTGGGTTAAAGTGGAAGG
-
PRKACA fw: ACCCTGAATGAAAAGCGCATC
-
PRKACA rev: CGTAGGTGTGAGAACATCTCCC
-
TAGLN fw: CCGTGGAGATCCCAACTGG
-
TAGLN rev: CCATCTGAAGGCCAATGACAT
Protein isolation and Western blotting
HAoSMCs were lysed with ice-cold Pierce IP lysis buffer (Fisher Scientific; 25 mM Tris•HCl pH 7.4, 150 mM NaCl, 1% NP-40, 1 mM EDTA, 5% glycerol) supplemented with complete protease and phosphatase inhibitors cocktail (Fisher Scientific). Protein concentration was measured by the Bradford assay (Bio-Rad Laboratories). Equal amounts of proteins were boiled in Roti-Load1 Buffer (Carl Roth) at 100 °C for 10 min, separated on SDS–polyacrylamide gels and transferred to PVDF membranes. The membranes were incubated with primary rabbit: anti-ALPL (1:1000; Abcam, ab65834), anti-phospho-PKA substrate (RRXS*/T*)(1:1000; Cell Signalling, 9624), anti-phospho-CREB (Ser133)(1:1000; Cell Signalling, 9198), anti-CREB (1:1000; Cell Signalling, 9197), or anti-GAPDH (1:1000; Cell Signalling, 2118) antibodies at 4 °C overnight and then with secondary anti-rabbit HRP-conjugated antibody (1:1000, Cell Signalling) at room temperature for 1 h. The membranes were stripped in stripping buffer (Fisher Scientific) at room temperature. Bands were detected with Clarity Western ECL substrate (Bio-Rad Laboratories) and ChemiDoc MP imaging system (Bio-Rad Laboratories) and quantified by using the ImageJ software. For quantification of the phospho-PKA substrate signal, all bands per lane were used. Results are shown as the ratio of phosphorylated proteins/GAPDH, of phosphorylated/total protein, and of total protein/GAPDH, normalized to the control group [28, 74, 75].
ALP activity assay
ALP activity in HAoSMCs was determined by using a colorimetric assay kit (Abcam). Results are shown normalized to total protein concentration measured by the Bradford assay (Bio-Rad Laboratories) [69] and to the control group.
Calcium content analysis
HAoSMCs were decalcified in 0.6 M HCl at 4 °C overnight, and calcium content in the supernatant was determined by using the QuantiChrom Calcium assay kit (BioAssay Systems). HAoSMCs were lysed with 0.1 M NaOH/0.1% SDS, and protein concentration was measured by the Bradford assay (Bio-Rad Laboratories) [14, 44, 46, 64]. Results are shown normalized to total protein concentration [1, 28, 56] and to the control group.
Calcium near-infrared (NIR) fluorescent imaging and Alizarin red staining
HAoSMCs were stained with OsteoSense 680 EX (1:100 dilution in medium, Perkin Elmer) overnight at 37 °C [49]. Images were collected using the ChemiDoc MP imaging system (Bio-Rad Laboratories) with excitation/emission (bandpass) wavelengths of 680/715(30) nm for detecting the calcium NIR signal (red) and with excitation/emission (bandpass) wavelengths of 488/532(28) nm as control (green, plate autofluorescence). HAoSMCs were fixed with 4% paraformaldehyde/PBS and stained with 2% Alizarin red (pH 4.5). The calcified areas are shown as red staining.
Statistics
Data are shown as scatter dot plots and arithmetic means ± SEM. Normality was tested with Shapiro–Wilk test. Non-normal datasets were transformed (log, reciprocal, or sqrt) prior to statistical testing to provide normality. Statistical testing was performed by one-way ANOVA followed by Tukey (homoscedastic data) or Games-Howell (heteroscedastic data) post hoc test and by the Steel–Dwass method (non-normal data). Two groups were compared by unpaired two-tailed t-test or Mann–Whitney U-test. p < 0.05 was considered statistically significant.
Results
A first series of experiments investigated the effects of chronic β-adrenergic stimulation on markers of osteogenic transdifferentiation of VSMCs. To this end, HAoSMCs were treated with increasing concentrations of isoproterenol, a nonspecific β-adrenergic receptor agonist, and the expression of osteogenic transcription factor CBFA1 and osteogenic enzyme ALPL was determined. As shown in Fig. 1a and b, isoproterenol treatment up-regulated CBFA1 and ALPL mRNA expression in HAoSMCs in a concentration-dependent manner, effects reaching statistical significance at 1 μM isoproterenol concentration. Accordingly, prolonged isoproterenol treatment significantly increased ALPL protein abundance in HAoSMCs (Fig. 1c). In contrast, exposure of HAoSMCs to isoproterenol did not significantly modify macrophage markers CD68 and LGALS3 or smooth muscle markers ACTA2 and TAGLN mRNA expression (Fig. 1d–g).
Isoproterenol up-regulates the expression of osteogenic markers in HAoSMCs. a, b Scatter dot plots and arithmetic means ± SEM (n = 6; arbitrary units, a.u.) of CBFA1 (a) and ALPL (b) relative mRNA expression in HAoSMCs following treatment for 24 h with the indicated concentrations of isoproterenol (ISO, 0–1 μM). c Representative Western blots and scatter dot plots and arithmetic means ± SEM (n = 10; a.u.) of normalized ALPL/GAPDH protein ratio in HAoSMCs following treatment for 7 days with 1 μM isoproterenol (ISO). d–g Scatter dot plots and arithmetic means ± SEM (n = 8; a.u.) of CD68 (d), LGALS3 (e), ACTA2 (f), and TAGLN (g) relative mRNA expression in HAoSMCs following treatment for 24 h with 1 μM isoproterenol (ISO). *(p < 0.05), **(p < 0.01) statistically significant vs control HAoSMCs
Next experiments explored the effects of isoproterenol on osteogenic markers CBFA1 and ALPL expression as well as calcification of HAoSMCs during elevated phosphate conditions. Isoproterenol treatment up-regulated osteogenic markers mRNA expression in HAoSMCs to similarly high levels as following exposure to the phosphate donor β-glycerophosphate (Fig. 2a, b). Additional treatment with isoproterenol tended to enhance β-glycerophosphate-induced CBFA1 mRNA expression, a difference, however, not reaching statistical significance (p = 0.057; Fig. 2a), and significantly augmented β-glycerophosphate-induced ALPL mRNA expression in HAoSMCs (Fig. 2b). Similarly, isoproterenol significantly increased ALP activity in HAoSMCs during control as well as elevated phosphate conditions (Fig. 2c). As shown by quantification of calcium content, isoproterenol did not significantly modify calcification of HAoSMCs during control conditions, but significantly aggravated mineralization induced by a calcification medium (Fig. 2d). These effects were confirmed by Alizarin red staining (Fig. 2e) and calcium NIR fluorescent imaging (Fig. 2f) showing an enhancement of calcification induced by calcification medium in the presence of isoproterenol. Taken together, β-adrenergic stimulation with isoproterenol aggravated phosphate-induced HAoSMC osteogenic marker expression and calcification in vitro.
Isoproterenol aggravates calcification of HAoSMCs during high phosphate conditions. a, b Scatter dot plots and arithmetic means ± SEM (n = 9; arbitrary units, a.u.) of CBFA1 (a) and ALPL (b) relative mRNA expression in HAoSMCs following treatment for 24 h with control (CTR) or 1 μM isoproterenol (ISO) without and with 2 mM β-glycerophosphate (Pi). c Scatter dot plots and arithmetic means ± SEM (n = 10; a.u.) of normalized ALP activity in HAoSMCs following treatment for 7 days with control (CTR) or 1 μM isoproterenol (ISO) without and with 2 mM β-glycerophosphate (Pi). d Scatter dot plots and arithmetic means ± SEM (n = 6; a.u.) of normalized calcium content in HAoSMCs following treatment for 11 days with control (CTR) or 1 μM isoproterenol (ISO) without and with calcification medium (Calc.; 10 mM β-glycerophosphate + 1.5 mM CaCl2). **(p < 0.01), ***(p < 0.001) statistically significant vs control HAoSMCs; †(p < 0.05), †††(p < 0.001) statistically significant vs Pi-/Calc.-treated HAoSMCs. e Representative images showing Alizarin red staining in HAoSMCs following treatment for 11 days with control (CTR) or 1 μM isoproterenol (ISO) without and with calcification medium (Calc.; 10 mM β-glycerophosphate + 1.5 mM CaCl2). Calcified areas: red staining. f Representative images showing calcium NIR fluorescent staining in HAoSMCs following treatment for 11 days with control (CTR) or 1 μM isoproterenol (ISO) without and with calcification medium (Calc.; 10 mM β-glycerophosphate + 1.5 mM CaCl2). Calcified areas: red; plate autofluorescence: green
To elucidate the underlying mechanisms of the pro-calcific effects of isoproterenol, the possible involvement of protein kinase A (PKA)/cAMP-responsive element-binding protein (CREB) signalling was investigated. As shown by Western blotting, isoproterenol significantly up-regulated the phosphorylation at RRXS*/T* substrate motif for PKA (where R refers to arginine, X refers to any amino acid, and S and T represent serine and threonine residue, respectively) of total cellular proteins and, thus, PKA activity in HAoSMCs following 5 min of treatment, levels remaining significantly higher up to 1 h of treatment (Fig. 3a). Similarly, isoproterenol increased the activation of CREB in HAoSMCs, as shown by increased phosphorylation at Ser133, following 5 min and up to 30 min of treatment without significantly affecting total CREB protein abundance (Fig. 3b).
Isoproterenol increases PKA and CREB activation in HAoSMCs. Representative Western blots and scatter dot plots and arithmetic means ± SEM (n = 7; arbitrary units, a.u.) of normalized phospho-PKA substrate/GAPDH protein ratio (a) and phospho-CREB/CREB and CREB/GAPDH protein ratios (b) in HAoSMCs following treatment for the indicated times (0–2 h) with 1 μM isoproterenol (ISO). *(p < 0.05) statistically significant vs control HAoSMCs
Furthermore, suppressing the endogenous expression in HAoSMCs of the PKA catalytic subunit α by silencing of the PRKACA gene using small interfering RNA (siRNA) (Fig. 4a) was able to significantly blunt isoproterenol-induced CBFA1 and ALPL mRNA expression (Fig. 4b, c). In addition, knockdown of the CREB1 gene by siRNA (Fig. 4d) significantly suppressed isoproterenol-induced osteogenic markers mRNA expression in HAoSMCs (Fig. 4e, f). PRKACA (Fig. 4a), or CREB1 (Fig. 4d) mRNA expression was not significantly affected by isoproterenol treatment. More importantly, silencing of the PRKACA or CREB1 genes significantly reduced calcification of HAoSMCs induced by isoproterenol together with calcification medium (Fig. 4g). Thus, PKA and CREB are activated by isoproterenol and participate in isoproterenol-induced osteogenic signalling and augmentation of calcification in HAoSMCs.
Silencing of PKA or CREB suppresses the pro-calcific effects of isoproterenol in HAoSMCs. a Scatter dot plots and arithmetic means ± SEM (n = 8; arbitrary units, a.u.) of PRKACA relative mRNA expression in HAoSMCs following transfection with negative control (Negsi) or PRKACA (PKAsi) siRNA and treatment for 24 h with control or 1 μM isoproterenol (ISO). **(p < 0.01), ***(p < 0.001) statistically significant vs Negsi-transfected HAoSMCs. b, c Scatter dot plots and arithmetic means ± SEM (n = 8; a.u.) of CBFA1 (b) and ALPL (c) relative mRNA expression in HAoSMCs following transfection with negative control (Negsi) or PRKACA (PKAsi) siRNA and treatment for 24 h with control or 1 μM isoproterenol (ISO). *(p < 0.05), **(p < 0.01) statistically significant vs Negsi-transfected HAoSMCs; †(p < 0.05) statistically significant vs Negsi-transfected ISO-treated HAoSMCs. d Scatter dot plots and arithmetic means ± SEM (n = 6; a.u.) of CREB1 relative mRNA expression in HAoSMCs following transfection with negative control (Negsi) or CREB1 (CREBsi) siRNA and treatment for 24 h with control or 1 μM isoproterenol (ISO). **(p < 0.01) statistically significant vs Negsi-transfected HAoSMCs. e, f Scatter dot plots and arithmetic means ± SEM (n = 6; a.u.) of CBFA1 (e) and ALPL (f) relative mRNA expression in HAoSMCs following transfection with negative control (Negsi) or CREB1 (CREBsi) siRNA and treatment for 24 h with control or 1 μM isoproterenol (ISO). *(p < 0.05), **(p < 0.01) statistically significant vs Negsi-transfected HAoSMCs; †(p < 0.05) statistically significant vs Negsi-transfected ISO-treated HAoSMCs. g Scatter dot plots and arithmetic means ± SEM (n = 8; a.u.) of normalized calcium content in HAoSMCs following transfection with negative control (Negsi), PRKACA (PKAsi), or CREB1 (CREBsi) siRNA and treatment for 11 days with control (CTR) or 1 μM isoproterenol (ISO) and calcification medium (Calc.; 10 mM β-glycerophosphate + 1.5 mM CaCl2). ***(p < 0.001) statistically significant vs Negsi-transfected HAoSMCs; †††(p < 0.001) statistically significant vs Negsi-transfected Calc. + ISO-treated HAoSMCs
To identify the β-adrenergic receptor mediating the osteoinductive effects of isoproterenol in HAoSMCs, the mRNA levels of the β-adrenergic receptor subtypes were determined. In accordance with the previous reports [57], the β2-adrenergic receptor, encoded by the ADRB2 gene, had the highest relative expression in HAoSMCs (Fig. 5a). Next, the endogenous expression of the β2-adrenergic receptor in HAoSMCs was suppressed by silencing of the ADRB2 gene using siRNA followed by additional treatment without or with isoproterenol. As a result, ADRB2 mRNA expression was significantly reduced in ADRB2 siRNA-transfected HAoSMCs as compared to negative control siRNA-transfected HAoSMCs, levels not significantly affected by additional isoproterenol treatment (Fig. 5b). Moreover, isoproterenol significantly up-regulated osteogenic markers mRNA expression in control-transfected HAoSMCs, effects significantly suppressed by ADRB2 silencing (Fig. 5c, d). Furthermore, additional treatment with the highly selective β2-adrenergic receptor antagonist ICI 118,551 significantly blunted isoproterenol-induced osteogenic markers mRNA expression (Fig. 5e, f) and significantly reduced calcification of HAoSMCs induced by isoproterenol together with calcification medium (Fig. 5g). Thus, the β2-adrenergic receptor mediated, at least partly, the pro-calcific effects of isoproterenol in HAoSMCs.
Knockdown or blockade of the β2-adrenergic receptor blunts the pro-calcific effects of isoproterenol in HAoSMCs. a Scatter dot plots and arithmetic means ± SEM (n = 4; arbitrary units, a.u.) of β-adrenergic receptors ADRB1, ADRB2, and ADRB3 relative mRNA expression in HAoSMCs. b Scatter dot plots and arithmetic means ± SEM (n = 6; a.u.) of ADRB2 relative mRNA expression in HAoSMCs following transfection with negative control (Negsi) or ADRB2 (ADRB2si) siRNA and treatment for 24 h with control or 1 μM isoproterenol (ISO). *(p < 0.05) statistically significant vs Negsi-transfected HAoSMCs. c, d Scatter dot plots and arithmetic means ± SEM (n = 6; a.u.) of CBFA1 (c) and ALPL (d) relative mRNA expression in HAoSMCs following transfection with negative control (Negsi) or ADRB2 (ADRB2si) siRNA and treatment for 24 h with control or 1 μM isoproterenol (ISO). *(p < 0.05), ***(p < 0.001) statistically significant vs Negsi-transfected HAoSMCs; †(p < 0.05), †††(p < 0.001) statistically significant vs Negsi-transfected ISO-treated HAoSMCs. e, f Scatter dot plots and arithmetic means ± SEM (n = 10; a.u.) of CBFA1 (e) and ALPL (f) relative mRNA expression in HAoSMCs following treatment for 24 h with control (CTR) or 1 μM isoproterenol (ISO) without and with 1 μM β2-adrenergic receptor antagonist ICI 118,551 (ICI). g Scatter dot plots and arithmetic means ± SEM (n = 8; a.u.) of normalized calcium content in HAoSMCs following treatment for 11 days with control (CTR) or 1 μM isoproterenol (ISO) and calcification medium (Calc.; 10 mM β-glycerophosphate + 1.5 mM CaCl2) without and with 1 μM β2-adrenergic receptor antagonist ICI 118,551 (ICI). *(p < 0.05), **(p < 0.01), ***(p < 0.001) statistically significant vs control HAoSMCs; ††(p < 0.01), statistically significant vs ISO-/Calc. + ISO-treated HAoSMCs
Discussion
The present study identifies a promoting effect of chronic β-adrenergic stimulation by isoproterenol through the β2-adrenergic receptor on osteogenic marker expression and calcification of VSMCs. These observations seem surprising, since β2-adrenergic activation ameliorates calcification in valvular cells [53]. Furthermore, acute β2-adrenergic receptor activation induces vasodilation [11], an effect that may be impaired by aging or atherosclerosis [36, 57]. In contrast, chronic isoproterenol exposure augments vasoconstrictor responses and induces vascular dysfunction [18, 19, 68]. Injections of high doses of adrenaline induce microcrystalline calcifications in aortic mitochondria of rabbits [7]. Also, repeated isoproterenol injections in rabbits induce oxidative stress and DNA damage in cerebral artery VSMCs [39]. Although further studies on the vascular effects of β-adrenergic activation are required, β-adrenergic overstimulation has been discussed as a putative factor in sympathetic overactivity [68].
Isoproterenol treatment of VSMCs promotes the expression of osteogenic markers CBFA1 and ALPL. These effects appear to be mediated through the β2-adrenergic receptor and are blocked by a selective antagonist. The pro-calcifying effects of isoproterenol can also be abrogated by silencing of the β2-adrenergic receptor, which did not abolish, but only reduce ADRB2 expression. Thus, it is tempting to speculate that not physiological activation but unphysiological overactivation of the downstream signalling pathways may be responsible for the pro-calcific effects of the β2-adrenergic receptor. These downstream effects of β2-adrenergic stimulation on osteogenic marker expression involve PKA and CREB. Although β2-adrenergic signalling events in VSMC are complex, sustained PKA activation has been identified after isoproterenol exposure [31]. Activation of PKA by TNF-α induces VSMC calcification, suggesting a detrimental role of chronic PKA activation in vascular calcification [32, 33, 65]. PKA has also been implied in the osteogenic effects of uremic serum on VSMC calcification [9]. Accordingly, PKA inhibition attenuates osteogenic transdifferentiation and calcification of VSMCs [37, 65] or aortic rings [67]. However, the role of PKA may be more complex, since also anti-calcific effects of PKA due to inhibition of endoplasmic reticulum stress are described [8].
A downstream target of PKA, activated by Ser133 phosphorylation, is the transcription factor CREB [48]. CREB has been shown to activate CBFA1/RUNX2 [79], and activation of the PKA/CREB pathway plays an important role in osteogenic differentiation of bone marrow stromal cells [59] and mesenchymal stem cells [80]. CREB has also been implied as a factor downstream of PKA-promoting vascular calcification [6, 65]. Furthermore, CREB mediates the pro-calcific effects of low potassium conditions in VSMCs [61]. CREB may also be involved in the pro-calcific effects of transforming growth factor β1 [27]. The present observations show a transient activation of PKA/CREB after isoproterenol exposure. The subsequent downstream effects of this CREB activation to induce a pro-calcific phenotype after isoproterenol exposure are currently unclear. CREB may modulate autophagy, which inherits a complex and important role in VSMC calcification [61]. CREB is further involved in pro-inflammatory signalling pathways in VSMCs [43]. After isoproterenol exposure, no alterations of the macrophage markers LGALS3 and CD68 or smooth muscle markers ACTA2 and TAGLN are detectable. Nonetheless, the PKA/CREB pathway seems to be required for the full pro-calcific effects of isoproterenol, since silencing of CREB or PKA abrogates these effects. These observations cannot rule out other putative mechanisms of isoproterenol exposure on VSMC calcification. β-adrenergic stimulation may induce intracellular signalling leading to RANKL release [35], ERK1/2 activation [58], PI3K pathway activation [10], oxidative stress [54], inflammation [18, 30, 58], or apoptosis [30, 54], all known as regulators of VSMC osteogenic transdifferentiation and vascular calcification [51, 72, 73].
The effects of β2-adrenergic stimulation on VSMC calcification may be a relevant aspect in conditions of sympathetic hyperactivity, such as CKD [25, 40, 55], but more complex mechanisms may play a significant role. The current study is clearly limited by artificial VSMC culture conditions with isoproterenol administration, a condition different from the adrenergic system in the vasculature in vivo [47]. Isoproterenol treatment in cell culture would not mimic a rhythmicity of the sympathetic nervous system and its co-transmitters [47]. β2-adrenergic receptors are involved in the circadian oscillations of vascular adhesion molecules after TNF-α stimulation [20]. In endothelial cells, isoproterenol promotes nitric oxide (NO) release, an important inhibitor of vascular calcification [24, 73]. Mice deficient for the β2-adrenergic receptor exhibit reduced aortic NO production [17]. Overexpression of the β2-adrenergic receptor in endothelial progenitor cells improves vascular repair after vascular injury [38]. However, overstimulation with isoproterenol induces endothelial synthase uncoupling [68] and up-regulates expression of inflammatory cytokines in endothelial cells [50]. A complex immunomodulatory role of the β2-adrenergic receptor has been discussed [77]. Clearly, caution is warranted when interpreting the current results, especially for mechanisms of vascular calcification in human patients.
In conclusion, β-adrenergic overstimulation by isoproterenol aggravates phosphate-induced VSMC calcification in vitro, effects mediated, at least in part, by the β2-adrenergic receptor and involving PKA/CREB signalling activation. Further studies are required to determine a possible association of adrenergic stimulation and vascular calcification.
References
Alesutan I, Luong TTD, Schelski N, Masyout J, Hille S, Schneider MP, Graham D, Zickler D, Verheyen N, Estepa M, Pasch A, Maerz W, Tomaschitz A, Pilz S, Frey N, Lang F, Delles C, Muller OJ, Pieske B, Eckardt KU, Scherberich J, Voelkl J (2020) Circulating uromodulin inhibits vascular calcification by interfering with pro-inflammatory cytokine signaling. Cardiovasc Res. https://doi.org/10.1093/cvr/cvaa081
Alesutan I, Tuffaha R, Auer T, Feger M, Pieske B, Lang F, Voelkl J (2017) Inhibition of osteo/chondrogenic transformation of vascular smooth muscle cells by MgCl2 via calcium-sensing receptor. J Hypertens 35:523–532. https://doi.org/10.1097/HJH.0000000000001202
Alesutan I, Voelkl J, Feger M, Kratschmar DV, Castor T, Mia S, Sacherer M, Viereck R, Borst O, Leibrock C, Gawaz M, Kuro OM, Pilz S, Tomaschitz A, Odermatt A, Pieske B, Wagner CA, Lang F (2017) Involvement of vascular aldosterone synthase in phosphate-induced osteogenic transformation of vascular smooth muscle cells. Sci Rep 7:2059. https://doi.org/10.1038/s41598-017-01882-2
Alves RD, Eijken M, van de Peppel J, van Leeuwen JP (2014) Calcifying vascular smooth muscle cells and osteoblasts: independent cell types exhibiting extracellular matrix and biomineralization-related mimicries. BMC Genomics 15:965. https://doi.org/10.1186/1471-2164-15-965
Arif E, Nihalani D (2019) Beta2-adrenergic receptor in kidney biology: a current prospective. Nephrology (Carlton) 24:497–503. https://doi.org/10.1111/nep.13584
Beazley KE, Eghtesad S, Nurminskaya MV (2013) Quercetin attenuates warfarin-induced vascular calcification in vitro independently from matrix Gla protein. J Biol Chem 288:2632–2640. https://doi.org/10.1074/jbc.M112.368639
Cavallero C, Spagnoli LG, Di Tondo U (1974) Early mitochondrial calcifications in the rabbit aorta after adrenaline. Virchows Arch A Pathol Anat Histol 362:23–39. https://doi.org/10.1007/BF00433772
Chang JR, Duan XH, Zhang BH, Teng X, Zhou YB, Liu Y, Yu YR, Zhu Y, Tang CS, Qi YF (2013) Intermedin1-53 attenuates vascular smooth muscle cell calcification by inhibiting endoplasmic reticulum stress via cyclic adenosine monophosphate/protein kinase A pathway. Exp Biol Med (Maywood) 238:1136–1146. https://doi.org/10.1177/1535370213502619
Chen NX, Duan D, O’Neill KD, Wolisi GO, Koczman JJ, Laclair R, Moe SM (2006) The mechanisms of uremic serum-induced expression of bone matrix proteins in bovine vascular smooth muscle cells. Kidney Int 70:1046–1053. https://doi.org/10.1038/sj.ki.5001663
Chesley A, Lundberg MS, Asai T, Xiao RP, Ohtani S, Lakatta EG, Crow MT (2000) The beta(2)-adrenergic receptor delivers an antiapoptotic signal to cardiac myocytes through G(i)-dependent coupling to phosphatidylinositol 3’-kinase. Circ Res 87:1172–1179. https://doi.org/10.1161/01.res.87.12.1172
Chruscinski A, Brede ME, Meinel L, Lohse MJ, Kobilka BK, Hein L (2001) Differential distribution of beta-adrenergic receptor subtypes in blood vessels of knockout mice lacking beta(1)- or beta(2)-adrenergic receptors. Mol Pharmacol 60:955–962. https://doi.org/10.1124/mol.60.5.955
Conti V, Russomanno G, Corbi G, Izzo V, Vecchione C, Filippelli A (2013) Adrenoreceptors and nitric oxide in the cardiovascular system. Front Physiol 4:321. https://doi.org/10.3389/fphys.2013.00321
Converse RL Jr, Jacobsen TN, Toto RD, Jost CM, Cosentino F, Fouad-Tarazi F, Victor RG (1992) Sympathetic overactivity in patients with chronic renal failure. N Engl J Med 327:1912–1918. https://doi.org/10.1056/NEJM199212313272704
Cui RR, Li SJ, Liu LJ, Yi L, Liang QH, Zhu X, Liu GY, Liu Y, Wu SS, Liao XB, Yuan LQ, Mao DA, Liao EY (2012) MicroRNA-204 regulates vascular smooth muscle cell calcification in vitro and in vivo. Cardiovasc Res 96:320–329. https://doi.org/10.1093/cvr/cvs258
da Silva RA, da SFG, da CFCJ, Zambuzzi WF (2020) Osteogenic gene markers are epigenetically reprogrammed during contractile-to-calcifying vascular smooth muscle cell phenotype transition. Cell Signal 66:109458. https://doi.org/10.1016/j.cellsig.2019.109458
Davel AP, Brum PC, Rossoni LV (2014) Isoproterenol induces vascular oxidative stress and endothelial dysfunction via a Gialpha-coupled beta2-adrenoceptor signaling pathway. PLoS ONE 9:e91877. https://doi.org/10.1371/journal.pone.0091877
Davel AP, Ceravolo GS, Wenceslau CF, Carvalho MH, Brum PC, Rossoni LV (2012) Increased vascular contractility and oxidative stress in beta(2)-adrenoceptor knockout mice: the role of NADPH oxidase. J Vasc Res 49:342–352. https://doi.org/10.1159/000337486
Davel AP, Fukuda LE, De Sa LL, Munhoz CD, Scavone C, Sanz-Rosa D, Cachofeiro V, Lahera V, Rossoni LV (2008) Effects of isoproterenol treatment for 7 days on inflammatory mediators in the rat aorta. Am J Physiol Heart Circ Physiol 295:H211-219. https://doi.org/10.1152/ajpheart.00581.2007
Davel AP, Kawamoto EM, Scavone C, Vassallo DV, Rossoni LV (2006) Changes in vascular reactivity following administration of isoproterenol for 1 week: a role for endothelial modulation. Br J Pharmacol 148:629–639. https://doi.org/10.1038/sj.bjp.0706749
de Juan A, Ince LM, Pick R, Chen CS, Molica F, Zuchtriegel G, Wang C, Zhang D, Druzd D, Hessenauer MET, Pelli G, Kolbe I, Oster H, Prophete C, Hergenhan SM, Albrecht U, Ripperger J, Montanez E, Reichel CA, Soehnlein O, Kwak BR, Frenette PS, Scheiermann C (2019) Artery-associated sympathetic innervation drives rhythmic vascular inflammation of arteries and veins. Circulation 140:1100–1114. https://doi.org/10.1161/CIRCULATIONAHA.119.040232
Demer LL, Tintut Y (2008) Vascular calcification: pathobiology of a multifaceted disease. Circulation 117:2938–2948. https://doi.org/10.1161/CIRCULATIONAHA.107.743161
Dziedzic M, Orlowska E, Petkowicz B, Bednarek-Skublewska A, Solski J, Gozdziewska M (2017) Levels of renalase and advanced oxidation protein products with regard to catecholamines in haemodialysed patients. Ann Agric Environ Med 24:453–458. https://doi.org/10.5604/12321966.1233567
Eckardt KU, Coresh J, Devuyst O, Johnson RJ, Kottgen A, Levey AS, Levin A (2013) Evolving importance of kidney disease: from subspecialty to global health burden. Lancet 382:158–169. https://doi.org/10.1016/S0140-6736(13)60439-0
Ferro A, Queen LR, Priest RM, Xu B, Ritter JM, Poston L, Ward JP (1999) Activation of nitric oxide synthase by beta 2-adrenoceptors in human umbilical vein endothelium in vitro. Br J Pharmacol 126:1872–1880. https://doi.org/10.1038/sj.bjp.0702512
Grassi G, Bertoli S, Seravalle G (2012) Sympathetic nervous system: role in hypertension and in chronic kidney disease. Curr Opin Nephrol Hypertens 21:46–51. https://doi.org/10.1097/MNH.0b013e32834db45d
Hao W, Yang R, Yang Y, Jin S, Li Y, Yuan F, Guo Q, Xiao L, Wang X, Wang F, Wu Y, Teng X (2018) Stellate ganglion block ameliorates vascular calcification by inhibiting endoplasmic reticulum stress. Life Sci 193:1–8. https://doi.org/10.1016/j.lfs.2017.12.002
He F, Li L, Li PP, Deng Y, Yang YY, Deng YX, Luo HH, Yao XT, Su YX, Gan H, He BC (2020) Cyclooxygenase-2/sclerostin mediates TGF-beta1-induced calcification in vascular smooth muscle cells and rats undergoing renal failure. Aging (Albany NY) 12:21220–21235. https://doi.org/10.18632/aging.103827
Henze LA, Luong TTD, Boehme B, Masyout J, Schneider MP, Brachs S, Lang F, Pieske B, Pasch A, Eckardt KU, Voelkl J, Alesutan I (2019) Impact of C-reactive protein on osteo-/chondrogenic transdifferentiation and calcification of vascular smooth muscle cells. Aging (Albany NY) 11:5445–5462. https://doi.org/10.18632/aging.102130
Herrmann J, Babic M, Tolle M, van der Giet M, Schuchardt M (2020) Research models for studying vascular calcification. Int J Mol Sci 21. https://doi.org/10.3390/ijms21062204
Herrmann JE, Heale J, Bieraugel M, Ramos M, Fisher RL, Vickers AE (2014) Isoproterenol effects evaluated in heart slices of human and rat in comparison to rat heart in vivo. Toxicol Appl Pharmacol 274:302–312. https://doi.org/10.1016/j.taap.2013.11.011
Hogarth DK, Sandbo N, Taurin S, Kolenko V, Miano JM, Dulin NO (2004) Dual role of PKA in phenotypic modulation of vascular smooth muscle cells by extracellular ATP. Am J Physiol Cell Physiol 287:C449-456. https://doi.org/10.1152/ajpcell.00547.2003
Hsu JJ, Lu J, Huang MS, Geng Y, Sage AP, Bradley MN, Tontonoz P, Demer LL, Tintut Y (2009) T0901317, an LXR agonist, augments PKA-induced vascular cell calcification. FEBS Lett 583:1344–1348. https://doi.org/10.1016/j.febslet.2009.03.039
Huang MS, Sage AP, Lu J, Demer LL, Tintut Y (2008) Phosphate and pyrophosphate mediate PKA-induced vascular cell calcification. Biochem Biophys Res Commun 374:553–558. https://doi.org/10.1016/j.bbrc.2008.07.062
Jang HS, Kim J, Padanilam BJ (2019) Renal sympathetic nerve activation via alpha2-adrenergic receptors in chronic kidney disease progression. Kidney Res Clin Pract 38:6–14. https://doi.org/10.23876/j.krcp.18.0143
Jiao K, Niu LN, Li QH, Ren GT, Zhao CM, Liu YD, Tay FR, Wang MQ (2015) beta2-Adrenergic signal transduction plays a detrimental role in subchondral bone loss of temporomandibular joint in osteoarthritis. Sci Rep 5:12593. https://doi.org/10.1038/srep12593
Jones BA, Aly HM, Forsyth EA, Sidawy AN (1996) Phenotypic characterization of human smooth muscle cells derived from atherosclerotic tibial and peroneal arteries. J Vasc Surg 24:883–891. https://doi.org/10.1016/s0741-5214(96)70027-7
Kang JH, Toita R, Asai D, Yamaoka T, Murata M (2014) Reduction of inorganic phosphate-induced human smooth muscle cells calcification by inhibition of protein kinase A and p38 mitogen-activated protein kinase. Heart Vessels 29:718–722. https://doi.org/10.1007/s00380-013-0427-x
Ke X, Shu XR, Wu F, Hu QS, Deng BQ, Wang JF, Nie RQ (2016) Overexpression of the beta2AR gene improves function and re-endothelialization capacity of EPCs after arterial injury in nude mice. Stem Cell Res Ther 7:73. https://doi.org/10.1186/s13287-016-0335-y
Kim HK, Park WS, Warda M, Park SY, Ko EA, Kim MH, Jeong SH, Heo HJ, Choi TH, Hwang YW, Lee SI, Ko KS, Rhee BD, Kim N, Han J (2012) Beta adrenergic overstimulation impaired vascular contractility via actin-cytoskeleton disorganization in rabbit cerebral artery. PLoS ONE 7:e43884. https://doi.org/10.1371/journal.pone.0043884
Kiuchi MG, Ho JK, Nolde JM, Gavidia LML, Carnagarin R, Matthews VB, Schlaich MP (2019) Sympathetic activation in hypertensive chronic kidney disease - a stimulus for cardiac arrhythmias and sudden cardiac death? Front Physiol 10:1546. https://doi.org/10.3389/fphys.2019.01546
Kiuchi MG, Mion D Jr (2016) Chronic kidney disease and risk factors responsible for sudden cardiac death: a whiff of hope? Kidney Res Clin Pract 35:3–9. https://doi.org/10.1016/j.krcp.2015.11.003
Klein IH, Ligtenberg G, Neumann J, Oey PL, Koomans HA, Blankestijn PJ (2003) Sympathetic nerve activity is inappropriately increased in chronic renal disease. J Am Soc Nephrol 14:3239–3244. https://doi.org/10.1097/01.asn.0000098687.01005.a5
Lee GL, Wu JY, Yeh CC, Kuo CC (2016) TLR4 induces CREB-mediated IL-6 production via upregulation of F-spondin to promote vascular smooth muscle cell migration. Biochem Biophys Res Commun 473:1205–1210. https://doi.org/10.1016/j.bbrc.2016.04.040
Liao XB, Zhou XM, Li JM, Yang JF, Tan ZP, Hu ZW, Liu W, Lu Y, Yuan LQ (2008) Taurine inhibits osteoblastic differentiation of vascular smooth muscle cells via the ERK pathway. Amino Acids 34:525–530. https://doi.org/10.1007/s00726-007-0003-8
London GM, Guerin AP, Marchais SJ, Metivier F, Pannier B, Adda H (2003) Arterial media calcification in end-stage renal disease: impact on all-cause and cardiovascular mortality. Nephrol Dial Transplant 18:1731–1740. https://doi.org/10.1093/ndt/gfg414
Mackenzie NC, Zhu D, Longley L, Patterson CS, Kommareddy S, MacRae VE (2011) MOVAS-1 cell line: a new in vitro model of vascular calcification. Int J Mol Med 27:663–668. https://doi.org/10.3892/ijmm.2011.631
Malpas SC (2010) Sympathetic nervous system overactivity and its role in the development of cardiovascular disease. Physiol Rev 90:513–557. https://doi.org/10.1152/physrev.00007.2009
Naqvi S, Martin KJ, Arthur JS (2014) CREB phosphorylation at Ser133 regulates transcription via distinct mechanisms downstream of cAMP and MAPK signalling. Biochem J 458:469–479. https://doi.org/10.1042/BJ20131115
O’Rourke C, Shelton G, Hutcheson JD, Burke MF, Martyn T, Thayer TE, Shakartzi HR, Buswell MD, Tainsh RE, Yu B, Bagchi A, Rhee DK, Wu C, Derwall M, Buys ES, Yu PB, Bloch KD, Aikawa E, Bloch DB, Malhotra R (2016) Calcification of vascular smooth muscle cells and imaging of aortic calcification and inflammation. J Vis Exp. https://doi.org/10.3791/54017
Oliveira BC, Marques VB, Brun BF, de Oliveira ESHM, Freitas Soares Melo S, Oliveira EM, Dos Santos L, Barauna VG (2019) Dipeptidyl peptidase-4 inhibition prevents vascular dysfunction induced by beta-adrenergic hyperactivity. Biomed Pharmacother 113:108733. https://doi.org/10.1016/j.biopha.2019.108733
Opdebeeck B, D'Haese PC, Verhulst A (2020) Molecular and cellular mechanisms that induce arterial calcification by indoxyl sulfate and P-cresyl sulfate. Toxins (Basel) 12. https://doi.org/10.3390/toxins12010058
Osadchii OE (2007) Cardiac hypertrophy induced by sustained beta-adrenoreceptor activation: pathophysiological aspects. Heart Fail Rev 12:66–86. https://doi.org/10.1007/s10741-007-9007-4
Osman L, Chester AH, Sarathchandra P, Latif N, Meng W, Taylor PM, Yacoub MH (2007) A novel role of the sympatho-adrenergic system in regulating valve calcification. Circulation 116:I282-287. https://doi.org/10.1161/CIRCULATIONAHA.106.681072
Remondino A, Kwon SH, Communal C, Pimentel DR, Sawyer DB, Singh K, Colucci WS (2003) Beta-adrenergic receptor-stimulated apoptosis in cardiac myocytes is mediated by reactive oxygen species/c-Jun NH2-terminal kinase-dependent activation of the mitochondrial pathway. Circ Res 92:136–138. https://doi.org/10.1161/01.res.0000054624.03539.b4
Salman IM (2015) Cardiovascular autonomic dysfunction in chronic kidney disease: a comprehensive review. Curr Hypertens Rep 17:59. https://doi.org/10.1007/s11906-015-0571-z
Schelski N, Luong TTD, Lang F, Pieske B, Voelkl J, Alesutan I (2019) SGK1-dependent stimulation of vascular smooth muscle cell osteo-/chondrogenic transdifferentiation by interleukin-18. Pflugers Arch 471:889–899. https://doi.org/10.1007/s00424-019-02256-5
Schutzer WE, Mader SL (2012) Biochemical and molecular aspects of vascular adrenergic regulation of blood pressure in the elderly. Int J Hypertens 2012:915057. https://doi.org/10.1155/2012/915057
Shin E, Ko KS, Rhee BD, Han J, Kim N (2014) Different effects of prolonged beta-adrenergic stimulation on heart and cerebral artery. Integr Med Res 3:204–210. https://doi.org/10.1016/j.imr.2014.10.002
Siddappa R, Martens A, Doorn J, Leusink A, Olivo C, Licht R, van Rijn L, Gaspar C, Fodde R, Janssen F, van Blitterswijk C, de Boer J (2008) cAMP/PKA pathway activation in human mesenchymal stem cells in vitro results in robust bone formation in vivo. Proc Natl Acad Sci U S A 105:7281–7286. https://doi.org/10.1073/pnas.0711190105
Steitz SA, Speer MY, Curinga G, Yang HY, Haynes P, Aebersold R, Schinke T, Karsenty G, Giachelli CM (2001) Smooth muscle cell phenotypic transition associated with calcification: upregulation of Cbfa1 and downregulation of smooth muscle lineage markers. Circ Res 89:1147–1154. https://doi.org/10.1161/hh2401.101070
Sun Y, Byon CH, Yang Y, Bradley WE, Dell'Italia LJ, Sanders PW, Agarwal A, Wu H, Chen Y (2017) Dietary potassium regulates vascular calcification and arterial stiffness. JCI Insight 2. https://doi.org/10.1172/jci.insight.94920
Sun Y, Byon CH, Yuan K, Chen J, Mao X, Heath JM, Javed A, Zhang K, Anderson PG, Chen Y (2012) Smooth muscle cell-specific runx2 deficiency inhibits vascular calcification. Circ Res 111:543–552. https://doi.org/10.1161/CIRCRESAHA.112.267237
Tanaka Y, Horinouchi T, Koike K (2005) New insights into beta-adrenoceptors in smooth muscle: distribution of receptor subtypes and molecular mechanisms triggering muscle relaxation. Clin Exp Pharmacol Physiol 32:503–514. https://doi.org/10.1111/j.1440-1681.2005.04222.x
Tanikawa T, Okada Y, Tanikawa R, Tanaka Y (2009) Advanced glycation end products induce calcification of vascular smooth muscle cells through RAGE/p38 MAPK. J Vasc Res 46:572–580. https://doi.org/10.1159/000226225
Tintut Y, Patel J, Parhami F, Demer LL (2000) Tumor necrosis factor-alpha promotes in vitro calcification of vascular cells via the cAMP pathway. Circulation 102:2636–2642. https://doi.org/10.1161/01.cir.102.21.2636
Touyz RM, Alves-Lopes R, Rios FJ, Camargo LL, Anagnostopoulou A, Arner A, Montezano AC (2018) Vascular smooth muscle contraction in hypertension. Cardiovasc Res 114:529–539. https://doi.org/10.1093/cvr/cvy023
Varennes O, Mentaverri R, Duflot T, Kauffenstein G, Objois T, Lenglet G, Avondo C, Morisseau C, Brazier M, Kamel S, Six I, Bellien J (2020) The metabolism of epoxyeicosatrienoic acids by soluble epoxide hydrolase is protective against the development of vascular calcification. Int J Mol Sci 21. https://doi.org/10.3390/ijms21124313
Victorio JA, Clerici SP, Palacios R, Alonso MJ, Vassallo DV, Jaffe IZ, Rossoni LV, Davel AP (2016) Spironolactone prevents endothelial nitric oxide synthase uncoupling and vascular dysfunction induced by beta-adrenergic overstimulation: role of perivascular adipose tissue. Hypertension 68:726–735. https://doi.org/10.1161/HYPERTENSIONAHA.116.07911
Voelkl J, Alesutan I, Leibrock CB, Quintanilla-Martinez L, Kuhn V, Feger M, Mia S, Ahmed MS, Rosenblatt KP, Kuro OM, Lang F (2013) Spironolactone ameliorates PIT1-dependent vascular osteoinduction in klotho-hypomorphic mice. J Clin Invest 123:812–822. https://doi.org/10.1172/JCI64093
Voelkl J, Castor T, Musculus K, Viereck R, Mia S, Feger M, Alesutan I, Lang F (2015) SGK1-sensitive regulation of cyclin-dependent kinase inhibitor 1b (p27) in cardiomyocyte hypertrophy. Cell Physiol Biochem 37:603–614. https://doi.org/10.1159/000430380
Voelkl J, Cejka D, Alesutan I (2019) An overview of the mechanisms in vascular calcification during chronic kidney disease. Curr Opin Nephrol Hypertens 28:289–296. https://doi.org/10.1097/MNH.0000000000000507
Voelkl J, Egli-Spichtig D, Alesutan I, Wagner CA (2021) Inflammation: a putative link between phosphate metabolism and cardiovascular disease. Clin Sci (Lond) 135:201–227. https://doi.org/10.1042/CS20190895
Voelkl J, Lang F, Eckardt KU, Amann K, Kuro OM, Pasch A, Pieske B, Alesutan I (2019) Signaling pathways involved in vascular smooth muscle cell calcification during hyperphosphatemia. Cell Mol Life Sci 76:2077–2091. https://doi.org/10.1007/s00018-019-03054-z
Voelkl J, Luong TT, Tuffaha R, Musculus K, Auer T, Lian X, Daniel C, Zickler D, Boehme B, Sacherer M, Metzler B, Kuhl D, Gollasch M, Amann K, Muller DN, Pieske B, Lang F, Alesutan I (2018) SGK1 induces vascular smooth muscle cell calcification through NF-kappaB signaling. J Clin Invest 128:3024–3040. https://doi.org/10.1172/JCI96477
Voelkl J, Tuffaha R, Luong TTD, Zickler D, Masyout J, Feger M, Verheyen N, Blaschke F, Kuro OM, Tomaschitz A, Pilz S, Pasch A, Eckardt KU, Scherberich JE, Lang F, Pieske B, Alesutan I (2018) Zinc inhibits phosphate-induced vascular calcification through TNFAIP3-mediated suppression of NF-kappaB. J Am Soc Nephrol 29:1636–1648. https://doi.org/10.1681/ASN.2017050492
Wang X, Seed B (2003) A PCR primer bank for quantitative gene expression analysis. Nucleic Acids Res 31:e154. https://doi.org/10.1093/nar/gng154
Wu L, Tai Y, Hu S, Zhang M, Wang R, Zhou W, Tao J, Han Y, Wang Q, Wei W (2018) Bidirectional role of beta2-adrenergic receptor in autoimmune diseases. Front Pharmacol 9:1313. https://doi.org/10.3389/fphar.2018.01313
Yang J, Sun H, Zhang J, Hu M, Wang J, Wu G, Wang G (2015) Regulation of beta-adrenergic receptor trafficking and lung microvascular endothelial cell permeability by Rab5 GTPase. Int J Biol Sci 11:868–878. https://doi.org/10.7150/ijbs.12045
Yu W, Chen FC, Xu WN, Ding SL, Chen PB, Yang L, Jiang SD, Pan XY (2020) Inhibition of Y1 receptor promotes osteogenesis in bone marrow stromal cells via cAMP/PKA/CREB pathway. Front Endocrinol (Lausanne) 11:583105. https://doi.org/10.3389/fendo.2020.583105
Zhang H, Li L, Dong Q, Wang Y, Feng Q, Ou X, Zhou P, He T, Luo J (2015) Activation of PKA/CREB signaling is involved in BMP9-induced osteogenic differentiation of mesenchymal stem cells. Cell Physiol Biochem 37:548–562. https://doi.org/10.1159/000430376
Acknowledgements
The authors gratefully acknowledge the technical assistance of J. Brosch and M. Kiminezhadmalaie.
Funding
Open access funding provided by Johannes Kepler University Linz. This work was supported by the Deutsche Forschungsgemeinschaft (AL2054/1–1, VO2259/2–1).
Author information
Authors and Affiliations
Contributions
J.V. and I.A. designed research; B.M., F.P., M.E., T.T.D.L., and I.A. performed experiments; B.M., B.P., F.L., I.A., and J.V. analysed and interpreted data; J.V. and I.A. wrote the manuscript with comments and edits from all authors.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Moser, B., Poetsch, F., Estepa, M. et al. Increased β-adrenergic stimulation augments vascular smooth muscle cell calcification via PKA/CREB signalling. Pflugers Arch - Eur J Physiol 473, 1899–1910 (2021). https://doi.org/10.1007/s00424-021-02621-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00424-021-02621-3