Abstract
Introduction
Robotic-assisted surgery (RAS) offers potential advantages over traditional surgical approaches. This study aimed to assess outcomes from a district general hospital (DGH) robotic colorectal programme against published data.
Materials and methods
The robotic programme was established following simulator, dry/wet lab training, and proctoring. We performed a case series analysing technical, patient, and oncological outcomes extracted from a prospective database of colorectal RAS cases (2015–2022). A registered systematic review (PROSPERO CRD42022300773; PubMed, Web of Science, EMBASE) of single-centre colorectal series from established robotic centres (n>200 cases) was completed and compared to local data using descriptive summary statistics. Risk of bias assessment was performed using an adapted version of the Cochrane ROBINS-I tool.
Results
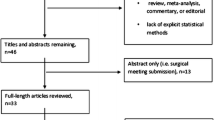
Two hundred thirty-two RAS cases were performed including 122 anterior resections, 56 APERs, 19 rectopexies, and 15 Hartmann’s procedures. The median duration was 325 (IQR 265–400) min. Blood loss was < 100 ml in 97% of cases with 2 (0.9%) cases converted to open. Complications (Clavien-Dindo 3–5) occurred in 19 (8%) patients, with 3 (1.3%) deaths in < 30 days. Length of stay was 7 (IQR 5–11) days. In 169 rectal cancer cases, there were 9 (5.3%) cases with a positive circumferential or distal margin and lymph node yield of 17 (IQR 13–24). A systematic review of 1648 abstracts identified 13 studies from established robotic centres, totaling 4930 cases, with technical, patient, and oncological outcomes comparable to our own case series.
Conclusions
Outcomes from our robotic colorectal programme at a UK DGH are comparable with the largest published case series from world-renowned centres. Training and proctoring together with rolling audit must accompany the expansion of robotic surgery to safeguard outcomes.

Similar content being viewed by others
Data availability
Extracted data and meta-analysis code available on request
References
Hashizume M, Shimada M, Tomikawa M, Ikeda Y, Takahashi I, Abe R et al (2002) Early experiences of endoscopic procedures in general surgery assisted by a computer-enhanced surgical system. Surg Endosc 16(8):1187–1191
Giulianotti PC, Coratti A, Angelini M, Sbrana F, Cecconi S, Balestracci T et al (2003) Robotics in general surgery: personal experience in a large community hospital. Arch Surg 138(7):777–784
NBOCAP. The National Bowel Cancer Audit (NBOCA) Annual Report 2021. Viewed at https://www.nboca.org.uk/content/uploads/2022/02/NBOCA-2021-AR-Final.pdf. Accessed 01/12/2021
Spinoglio G, Summa M, Priora F, Quarati R, Testa S (2008) Robotic colorectal surgery: first 50 cases experience. Dis Colon Rectum 51(11):1627–1632
Baek SJ, Kim SH, Cho JS, Shin JW, Kim J (2012) Robotic versus conventional laparoscopic surgery for rectal cancer: a cost analysis from a single institute in Korea. World J Surg 36(11):2722–2729
Katsuno H, Hanai T, Masumori K, Koide Y, Matsuoka H, Tajima Y et al (2020) Short- and long-term outcomes of robotic surgery for rectal cancer: a single-center retrospective cohort study. Surg Today 50(3):240–247
Huang YJ, Kang YN, Huang YM, Wu AT, Wang W, Wei PL (2019) Effects of laparoscopic vs robotic-assisted mesorectal excision for rectal cancer: an update systematic review and meta-analysis of randomized controlled trials. Asian J Surg 42(6):657–666
Li L, Zhang W, Guo Y, Wang X, Yu H, Du B et al (2019) Robotic versus laparoscopic rectal surgery for rectal cancer: a meta-analysis of 7 randomized controlled trials. Surg Innov 26(4):497–504
Katsuno H, Hanai T, Masumori K, Koide Y, Ashida K, Matsuoka H et al (2020) Robotic surgery for rectal cancer: operative technique and review of the literature. J Anus Rectum Colon 4(1):14–24
Jayne D, Pigazzi A, Marshall H, Croft J, Corrigan N, Copeland J et al (2017) Effect of robotic-assisted vs conventional laparoscopic surgery on risk of conversion to open laparotomy among patients undergoing resection for rectal cancer: the ROLARR randomized clinical trial. JAMA 318(16):1569–1580
Kim MJ, Park SC, Park JW, Chang HJ, Kim DY, Nam BH et al (2018) Robot-assisted versus laparoscopic surgery for rectal cancer: a phase II open label prospective randomized controlled trial. Ann Surg 267(2):243–251
Phan K, Kahlaee HR, Kim SH, Toh JWT (2019) Laparoscopic vs. robotic rectal cancer surgery and the effect on conversion rates: a meta-analysis of randomized controlled trials and propensity-score-matched studies. Tech Coloproctol 23(3):221–230
Scarpinata R, Aly EH (2013) Does robotic rectal cancer surgery offer improved early postoperative outcomes? Dis Colon Rectum 56(2):253–62
Speicher PJ, Englum BR, Ganapathi AM, Nussbaum DP, Mantyh CR, Migaly J (2015) Robotic low anterior resection for rectal cancer: a national perspective on short-term oncologic outcomes. Ann Surg 262(6):1040–1045
Zhang X, Wei Z, Bie M, Peng X, Chen C (2016) Robot-assisted versus laparoscopic-assisted surgery for colorectal cancer: a meta-analysis. Surg Endosc 30(12):5601–5614
Ackerman SJ, Daniel S, Baik R, Liu E, Mehendale S, Tackett S et al (2018) Comparison of complication and conversion rates between robotic-assisted and laparoscopic rectal resection for rectal cancer: which patients and providers could benefit most from robotic-assisted surgery? J Med Econ 21(3):254–261
Baek JH, McKenzie S, Garcia-Aguilar J, Pigazzi A (2010) Oncologic outcomes of robotic-assisted total mesorectal excision for the treatment of rectal cancer. Ann Surg 251(5):882–886
D'Annibale A, Pernazza G, Monsellato I, Pende V, Lucandri G, Mazzocchi P et al (2013) Total mesorectal excision: a comparison of oncological and functional outcomes between robotic and laparoscopic surgery for rectal cancer. Surg Endosc 27(6):1887–1895
Baik SH, Kim NK, Lim DR, Hur H, Min BS, Lee KY (2013) Oncologic outcomes and perioperative clinicopathologic results after robot-assisted tumor-specific mesorectal excision for rectal cancer. Ann Surg Oncol 20(8):2625–2632
Felix EL (2021)Robotic surgery: Deja Vu all over again. General Surgery News 2021 09/03/2021. Viewed at https://www.generalsurgerynews.com/Opinion/Article/03-21/Robotic-Surgery-D-j-agrave-Vu-All-Over-Again-/62765
Khani MH, Smedh K (2010) Centralization of rectal cancer surgery improves long-term survival. Color Dis 12(9):874–879
Prades J, Manchon-Walsh P, Sola J, Espinas JA, Guarga A, Borras JM (2016) Improving clinical outcomes through centralization of rectal cancer surgery and clinical audit: a mixed-methods assessment. Eur J Pub Health 26(4):538–542
Miskovic D, Ahmed J, Bissett-Amess R, Gomez Ruiz M, Luca F, Jayne D et al (2019) European consensus on the standardization of robotic total mesorectal excision for rectal cancer. Color Dis 21(3):270–276
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240(2):205–213
Cochrane (2011) Cochrane handbook for systematic reviews of interventions Version 5.1.0 The Cochrane Collaboration [cited 2016 10/01]. Available from: www.cochrane-handbook.org <http://www.cochrane-handbook.org
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P (2009) Reprint--preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Phys Ther 89(9):873–880
PUBMED: NCBI National Center for Biotechnology Information; 2015 [17.11.2015]. Available from: http://www.ncbi.nlm.nih.gov/pubmed/advanced. Accessed 01/11/2021
Web of Science (2015) Available from: http://wok.mimas.ac.uk/. Accessed 01/11/2021
Sterne JA, Hernán MA, McAleenan A, Reeves BC, Higgins JP (2022) Chapter 25: Assessing risk of bias in a non-randomized study. In: Higgins JPTTJ, Chandler J, Cumpston M, Li T, Page MJ, Welch VA (eds) Cochrane handbook for systematic reviews of interventions 63, Cochrane. Viewed at https://training.cochrane.org/handbook/current/chapter-25. Accessed 01/11/2021
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. Bmj 327(7414):557–560
Sterne JA, Egger M (2001) Funnel plots for detecting bias in meta-analysis: guidelines on choice of axis. J Clin Epidemiol 54(10):1046–1055
R Development Core Team (2013) R: a language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria
Viechtbauer W, Cheung MW (2010) Outlier and influence diagnostics for meta-analysis. Res Synth Methods 1(2):112–125
Tang B, Zhang C, Li C, Chen J, Luo H, Zeng D et al (2017) Robotic total mesorectal excision for rectal cancer: a series of 392 cases and mid-term outcomes from a single center in China. J Gastrointest Surg 21(3):569–576
Chang W, Wei Y, Ren L, Jian M, Chen Y, Chen J et al (2020) Short-term and long-term outcomes of robotic rectal surgery-from the real word data of 1145 consecutive cases in China. Surg Endosc 34(9):4079–4088
Law WL, Foo DCC (2017) Comparison of short-term and oncologic outcomes of robotic and laparoscopic resection for mid- and distal rectal cancer. Surg Endosc 31(7):2798–2807
Lee JM, Yang SY, Han YD, Cho MS, Hur H, Min BS et al (2021) Can better surgical outcomes be obtained in the learning process of robotic rectal cancer surgery? A propensity score-matched comparison between learning phases. Surg Endosc 35(2):770–778
Lei X, Yang L, Huang Z, Shi H, Zhou Z, Tang C et al (2021) No beneficial effect on survival but a decrease in postoperative complications in patients with rectal cancer undergoing robotic surgery: a retrospective cohort study. BMC Surg 21(1):355
Parascandola SA, Horsey ML, Hota S, Paull JO, Graham A, Pudalov N et al (2021) The robotic colorectal experience: an outcomes and learning curve analysis of 502 patients. Color Dis 23(1):226–236
Polat F, Willems LH, Dogan K, Rosman C (2019) The oncological and surgical safety of robot-assisted surgery in colorectal cancer: outcomes of a longitudinal prospective cohort study. Surg Endosc 33(11):3644–3655
Rohila J, Kammar P, Pachaury A, de’Souza A, Saklani A (2020) Evolution of robotic surgery in a colorectal cancer unit in India. Indian. J Surg Oncol 11(4):633–641
Rouanet P, Bertrand MM, Jarlier M, Mourregot A, Traore D, Taoum C et al (2018) Robotic versus laparoscopic total mesorectal excision for sphincter-saving surgery: results of a single-center series of 400 consecutive patients and perspectives. Ann Surg Oncol 25(12):3572–3579
Sammour T, Malakorn S, Bednarski BK, Kaur H, Shin US, Messick C et al (2018) Oncological outcomes after robotic proctectomy for rectal cancer: analysis of a prospective database. Ann Surg 267(3):521–526
Tilney HS, Huddy JR, Nizar AS, Smith R, Gudgeon AM (2021) Minimal access rectal cancer surgery: an observational study of patient outcomes from a district general hospital with over a decade of experience with robotic rectal cancer surgery. Color Dis 23(8):1961–1970
Yamaguchi T, Kinugasa Y, Shiomi A, Kagawa H, Yamakawa Y, Furuatni A et al (2018) Short- and long-term outcomes of robotic-assisted laparoscopic surgery for rectal cancer: results of a single high-volume center in Japan. Int J Color Dis 33(12):1755–1762
Shin JK, Kim HC, Yun SH, Park YA, Cho YB, Huh JW et al (2021) Comparison of transanal total mesorectal excision and robotic total mesorectal excision for low rectal cancer after neoadjuvant chemoradiotherapy. Surg Endosc 35(12):6998–7004
Bonjer HJ, Deijen CL, Abis GA, Cuesta MA, van der Pas MH, de Lange-de Klerk ES et al (2015) A randomized trial of laparoscopic versus open surgery for rectal cancer. N Engl J Med 372(14):1324–1332
Stevenson AR, Solomon MJ, Lumley JW, Hewett P, Clouston AD, Gebski VJ et al (2015) Effect of laparoscopic-assisted resection vs open resection on pathological outcomes in rectal cancer: the ALaCaRT randomized clinical trial. JAMA 314(13):1356–1363
Jayne DG, Guillou PJ, Thorpe H, Quirke P, Copeland J, Smith AM et al (2007) Randomized trial of laparoscopic-assisted resection of colorectal carcinoma: 3-year results of the UK MRC CLASICC Trial Group. J Clin Oncol 25(21):3061–3068
Jeong SY, Park JW, Nam BH, Kim S, Kang SB, Lim SB et al (2014) Open versus laparoscopic surgery for mid-rectal or low-rectal cancer after neoadjuvant chemoradiotherapy (COREAN trial): survival outcomes of an open-label, non-inferiority, randomised controlled trial. Lancet Oncol 15(7):767–774
Sihler KC, Napolitano LM (2010) Complications of massive transfusion. Chest 137(1):209–220
Ferraris VA, Davenport DL, Saha SP, Austin PC, Zwischenberger JB (2012) Surgical outcomes and transfusion of minimal amounts of blood in the operating room. Arch Surg 147(1):49–55
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by Peter Vaughan-Shaw, Abraham Joel, and Mohamed Farah. The first draft of the manuscript was written by Peter Vaughan-Shaw, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript
Corresponding author
Ethics declarations
Ethics approval
This is an observational study. The study was approved as a service evaluation project by the Clinical Governance and Clinical Effectiveness Department and considered exempt from ethical approval. Informed consent was not deemed necessary.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Peter G Vaughan-Shaw and Abraham S Joel are joint first authors.
Previous communications: Accepted for poster presentation at ACPGBI 2022
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Vaughan-Shaw, P.G., Joel, A.S., Farah, M. et al. Evaluation of an established colorectal robotic programme at an NHS district general hospital: audit of outcomes and systematic review of published data. Langenbecks Arch Surg 408, 416 (2023). https://doi.org/10.1007/s00423-023-03152-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00423-023-03152-4