Abstract
Purpose
Laparoscopic surgery for low rectal cancer is often challenging. Transanal total mesorectal excision (TaTME) and robotic surgery have been introduced to overcome the technical difficulties in laparoscopic surgery and achieve more favorable outcomes. Hybrid robotic surgery, which combines TaTME with the abdominal robotic approach, incorporates the advantages of each of these surgical techniques and might achieve less invasive and safer surgery. This study evaluated the safety and feasibility of hybrid robotic surgery with TaTME (hybrid TaTME).
Methods
We retrospectively reviewed 162 TaTME cases performed at our department from September 2016 to May 2022. Among them, 92 cases of conventional TaTME and 30 of hybrid TaTME were eligible. We used propensity score matching analysis (PSM) to adjust for patients’ characteristics and compared the short-term outcomes of the two treatment groups.
Results
Twenty-seven cases in each group were extracted using PSM. The operation time in hybrid TaTME was comparable to that in conventional TaTME. There was no significant difference in the postoperative hospital stay between the two groups. Other intra- and post-operative outcomes were also comparable between the two groups. Furthermore, no significant differences were observed between the two groups in the curative resection and recurrence rates.
Conclusion
Hybrid TaTME for low rectal cancer was as favorable as conventional TaTME in producing satisfactory short-term outcomes. However, furthermore, larger-scale studies conducted over longer study periods are needed to evaluate the validity of the findings.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Total mesorectal excision (TME), which was first documented by Heald in 1982, has become the standard surgical technique for rectal cancer [1, 2]. Complete TME and a secure circumferential resection margin (CRM) have been considered very important in and have contributed to reduced local recurrence [3,4,5,6]. Although laparoscopic surgery for rectal cancer was introduced, complete TME has been challenging in cases such as patients with obesity and male patients with a narrow pelvis [7,8,9]. Although two large randomized control trials (RCTs) had found that laparoscopic surgery was not inferior to open surgery in oncological outcomes, two large subsequent RCTs refuted that laparoscopic surgery was not non-inferior to open surgery in terms of securing CRM, which thus raised concerns regarding laparoscopic surgery [10,11,12,13]. Robotic surgery and transanal TME (TaTME) have recently emerged as independent attempts to overcome these technical difficulties.
Robotic surgery provides three-dimensional vision, articulated function, and image stabilization, enabling safer and more meticulous manipulation in the complex pelvis [14, 15]. In the large-scale ROLARR trial, no statistically significant differences were found between robotic-assisted laparoscopic surgery and laparoscopic surgery in the overall conversion rate, positive CRM, and perioperative complications [15]. However, the conversion rate in robotic-assisted surgery was significantly lower in male patients, patients with obesity, and patients who underwent low anterior resection [15]. These results suggest that robotic surgery may be indicated for cases that are difficult to treat with laparoscopic surgery.
TaTME is a transanal TME procedure performed in a down-to-up fashion. TaTME provides a better view in lower rectal cancer and secures the distal margin (DM), leading to better oncological outcomes [16, 17]. However, issues have been raised concerning pelvic organ injuries, such as urethral injury, and a high local recurrence rate in TaTME because of technical difficulties; thus, technical proficiency is required in TaTME [17,18,19,20].
We have performed TaTME in more than 160 cases since its first introduction in September 2016. TaTME is currently the first-line surgical procedure for low rectal cancer at our department. Since June 2020, we have performed TaTME in combination with the abdominal robotic approach (hybrid TaTME) for a safer, less invasive surgery. Because reports on this technique are scarce, the feasibility and safety of hybrid TaTME are unclear [21,22,23,24]. Therefore, this study evaluated the feasibility and safety of hybrid TaTME compared with conventional TaTME for low rectal cancer.
Materials and methods
Patients
A database of prospectively managed rectal cancer cases at Kobe University was reviewed. We retrospectively examined 162 TaTME cases performed by our department from September 2016 to May 2022. Patients aged 20 years or older with preoperatively histologically proven malignant tumors, such as adenocarcinoma, squamous cell carcinoma, neuroendocrine tumor, or malignant melanoma, located below the peritoneal reflection, were eligible for this study. Five cases of robotic TaTME (in which robot-assisted anal manipulation was performed), 4 of total pelvic exenteration, 6 of inguinal lymph node dissection, 6 of total colectomy, 2 of perineal reconstruction, and 1 of laparotomy were excluded. Two patients diagnosed with gastrointestinal stromal tumors, 2 with benign tumors, 2 with double cancers, and 10 with preoperative recurrence were also excluded. In total, 92 cases of conventional laparoscopic TaTME and 30 of hybrid TaTME were included in the study. Patient characteristics; surgical, postoperative, and pathological outcomes; and recurrence data were extracted from electronic medical records in this study.
As described above, we introduced TaTME for low rectal cancer in 2016, and all patients with low rectal cancer were indicated for TaTME. Hybrid TaTME was introduced in June 2020. However, the availability of robot was limited in our institution, and hybrid TaTME was performed depending on its availability.
This study was approved by the Institutional Review Board and Ethics Committee of Kobe University Graduate School of Medicine (IRB reference no.: B220001).
Preoperative management
All patients were diagnosed based on imaging studies, including colonoscopy, computed tomography, magnetic resonance imaging, and positron emission computed tomography. Patients diagnosed as cT3/4- or cN-positive without distant metastasis were eligible for preoperative treatment. Preoperative treatment consisted of neoadjuvant chemoradiotherapy (NACRT) using oral 5-FU and radiation therapy (45–50 Gy) or neoadjuvant chemotherapy (NAC). Surgery was performed 6–8 weeks after the completion of NACRT. The patients who received NAC underwent surgery 2–8 weeks after 6 courses of FOLFOXIRI and bevacizumab.
Surgical techniques
Two teams performed the TaTME with simultaneous abdominal and perineal manipulation, except for the first six cases of conventional TaTME and the first of hybrid TaTME. The surgery was performed according to the procedure described by Lacy et al. [16].
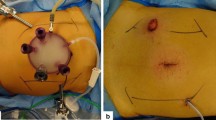
For perineal manipulation in low anterior resection, the GelPOINT path (Applied Medical, USA) was applied through the anus, and CO2 was insufflated using an AirSeal (SurgiQuest, USA) to achieve a pressure of 13 mmHg. After confirming the DM of the tumor, the rectum was closed by applying a purse-string suture to the submucosa to secure a sufficient DM. The rectum was washed to prevent the contamination of the surgical field and tumor implantation. Then, the perineal team initiated a full-thickness rectal incision and performed TaTME in a down-to-up fashion, as described previously [25].
Perineal manipulation in abdominoperineal resection was performed as described previously [26]. Briefly, the anus was tightly closed by a double purse-string suture, and the skin was incised circumferentially around the anus. The GelPOINT Mini (Applied Medical, USA) was placed subcutaneously, and the perineal subcutaneous cavity was insufflated by CO2 at a pressure of 12–15 mmHg. The levator ani muscle was widely exposed and its transection was started at 6 o’clock. After exposure of the mesorectal plane, the dissection of the levator ani muscle was extended bilaterally. Then, the puborectal sling was dissected, and the dorsal surface of the prostate (or the vagina) was identified by dissecting between the neurovascular bundle and mesorectum. The rectourethral muscle (or the rectovaginal septum) was divided using the prostate (or the vagina) as a landmark. Finally, TME was performed in a down-to-up manner.
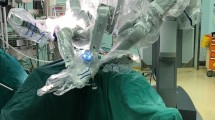
In the conventional surgery, the standard abdominal manipulations, including the ligation of the inferior mesenteric artery and transabdominal TME, were performed using a conventional 5-port system in parallel. In the hybrid surgery, the same surgical procedures as above were performed using the da Vinci Xi Surgical System (Intuitive Surgical, Sunnyvale, CA, USA).
When both the abdominal and perineal teams reached the peritoneal reflection, the peritoneum was incised, and the TME was completed. Then, the specimen was extracted through a mini-laparotomy. After the perineal team performed purse-string suturing on the distal rectal stump, they created an anastomosis using the single stapling technique. After confirming the presence of anastomotic bleeding and anastomotic leakage by colonoscopy, a drain was placed on the pelvic floor. A diverting ileostomy was subsequently created.
In the hybrid surgery, the entire process was performed as described in Fig. 1.
Statistical analysis
Propensity score matching analysis (PSM) was performed to reduce confounding bias between the conventional and hybrid TaTME groups. A propensity score was calculated by logistic regression analysis using age, sex, American Society of Anesthesiology score, body mass index, distance from the anal verge, clinical T stage, surgical procedure, preoperative treatment, and lateral pelvic lymph node dissection (LLND) as covariates. Nearest neighbor matching was performed so that the two groups were at a 1:1 ratio without replacement, and the width of the caliper was within 0.2 standard deviation (SD). Then, 27 patients each from the hybrid and conventional TaTME groups were matched.
Categorical variables were compared using the chi-square test or Fisher’s exact test. Non-parametric continuous variables were compared using the Mann–Whitney test and expressed as median and range. Local recurrence-free survival rate (LRFS) and recurrence-free survival rate (RFS) were calculated using the Kaplan–Meier method, and the log-rank test was performed to compare the survival curves of the two treatment groups. The results were considered statistically significant when the P-value < 0.05. All statistical data were analyzed using EZR version 1.54 (Saitama Medical Center, Jichi Medical University, Saitama, Japan), which is a graphical user interface for R (The R Foundation for Statistical Computing, Vienna, Austria).
Results
Patient backgrounds and tumor characteristics are summarized in Table 1. The patients in the hybrid group were younger than those in the conventional group. The distance from the anal verge was shorter in the hybrid group than in the conventional group. The patient and tumor characteristics after PSM were similar between the two groups.
The surgical outcomes are shown in Table 2. The surgical procedure, lymphadenectomy, and LLND were performed approximately equally between the two groups. The median operation time, blood loss, and the number of lymph nodes harvested were also comparable between the two groups. No patients were converted to open surgery in either group.
The postoperative complications are summarized in Table 3. The rate of complications of grade II or higher on the Clavien–Dindo classification system was similar in both groups. The median postoperative hospital stay in the hybrid group tended to be shorter than that in the conventional group; however, no significant difference was noted between the two groups (P = 0.076). One case in the conventional group received re-operation for anastomotic leakage. Two and one in the hybrid group underwent re-operation due to anastomotic leakage and bowel obstruction, respectively.
The pathological outcomes are shown in Table 4. In one case of intersphincteric resection in the hybrid group, both DM and radial margin (RM) were 450 µm, resulting in an R1 resection. However, all the other cases were negative for both DM and RM. In the conventional group, a positive RM was observed in only one case.
The recurrence data are summarized in Table 5. Three patients in the conventional group and five in the hybrid group with stage IV rectal cancer were excluded, and the remaining patients were examined for recurrence. The median follow-up period was 24.0 months in the conventional group and 7.5 in the hybrid group. No significant differences were observed between the two groups concerning the recurrence, distant metastasis, and local recurrence rates.
The Kaplan–Meier curves for LRFS and RFS are shown in Fig. 2. No significant difference was found in LRFS (P = 0.37) and RFS (P = 0.876) between the two groups.
Discussion
The application of TaTME has expanded globally since it was first described by Sylla et al. [27]. TaTME provides a better view under direct vision in low rectal cancer, secures DM and CRM, and helps preserve the pelvic nerves [16, 17]. Robotic surgery also has several important features not found in laparoscopic surgery, such as a three-dimensional stabilized camera, motion scaling, and articulating functions, allowing for more meticulous manipulation in the complex pelvis. The potential advantages of both techniques are lower rates of conversion and the consequent postoperative complications, as well as better specimen quality, leading to favorable oncologic outcomes [14, 17, 18, 28,29,30,31,32,33]. In addition, these surgical techniques are especially beneficial in patients with obesity and male patients with a narrow pelvis, which present difficulties for laparoscopy [7,8,9, 15, 34]. Based on the belief that incorporating the advantages of each of these techniques could achieve a safer and less invasive surgery and, consequently, better oncological outcomes, we established hybrid TaTME at our institution. To our knowledge, few reports of this technique have been published [21,22,23,24], and the present study is the first to compare it with conventional TaTME regarding safety and feasibility. We found that the short-term outcomes of hybrid TaTME were comparable to those of conventional TaTME, which was considered acceptable.
Robotic surgery has a longer operation time compared with open or laparoscopic surgery [29, 30]. Although performing hybrid TaTME would also presumably take longer in the present study, the operation time was similar to that of conventional TaTME. The operation time in the present study was also comparable to that in a previous report, although about half of the patients underwent LLND [34]. This result may be because the surgeon’s progress in robotic surgery, which enabled safer and more precise manipulation from early on, could shorten the operation time, despite the surgeon’s limited experience with robotic surgery in the present study. The operation time in hybrid surgery could also be shortened by standardizing the procedure and adhering to the time course shown in Fig. 1 through close collaboration between the two surgical teams. The accumulation of more cases is expected to eliminate the influence of the learning curve, allowing the operation time in this technique to be further shortened.
The advantages of hybrid TaTME are the improved visibility and ergonomics compared with conventional TaTME due to the various features of robotic surgery. Furthermore, the TilePro function allows the surgeon of the abdominal team to share the surgical field with the perineal team, enhancing the collaboration between both teams. These advantages may have allowed for safer and more meticulous manipulation at the various surgical stages, even in cases of a confined pelvis, ultimately leading to fewer complications. In the present study, however, while fewer complications were observed in the hybrid group than in the conventional group, no significant difference was found in the complication rate due to the small number of cases. Furthermore, the complication rate was comparable to those of previous reports, ranging from 20 to 45%, suggesting that hybrid surgery is as safe and feasible as conventional surgery [16,17,18,19, 34]. However, as this technique is still in its infancy, it is expected that further refinement through the accumulation of cases could provide more favorable short-term outcomes in complex rectal cancers.
Enhancing specimen quality to reduce local recurrence is of great importance [3,4,5,6]. While a low local recurrence rate of 0–4% has been reported for TaTME, certain concerns have been raised regarding local recurrence after TaTME, as reported in a 2019 Norwegian study, due to the complexity and difficulty of the procedure [17, 20, 31, 35]. In the hybrid group in the present study, local recurrence was observed in only one patient (4.5%), and no local recurrence was observed in patients who achieved R0 resection. These recurrence cases may be due to the positive DM or RM at the time of the initial surgery, which may not present a serious concern regarding recurrence in hybrid TaTME if the quality of the resection is maintained. In the present study, all but one patient achieved R0 resection (96.3%), and the median number of lymph nodes harvested was 12 or more in the hybrid group, which is comparable to that in the conventional group.
These pathological results were also comparable to those in previous reports on TaTME [17, 18]. Therefore, hybrid TaTME could also adequately maintain the quality of radical resection as conventional TaTME, leading to acceptable outcomes in local recurrence, despite the high proportion of cT3/4-positive, preoperatively treated, and male patients in the present study.
Another important issue is whether TaTME is still needed in the times of robotic surgery. It is well known that successful TME can be achieved by robotic surgery alone even in the obese or male patients [15]. However, TaTME is only one down-to-up approach which is completely different from the other transabdominal approaches including robotic and laparoscopic TME and should have its unique advantages. TaTME may be beneficial for the patients with bulky tumors, recurrent tumors, and positive lateral pelvic lymph nodes. Although future randomized trials of TaTME vs. robotic surgery are necessary to determine which patients benefit from TaTME, we believe that TaTME is worth learning for colorectal surgeons and that hybrid TaTME could be a useful option in the future.
This study has several limitations. First, since this is a retrospective cohort study, a bias in patient selection remains, despite performing PSM to minimize it. Second, a risk of overestimation concerning RM may exist because, in Japan, the lymph nodes in the mesorectum are generally separated from the specimen before submission to the pathology department. Finally, due to the short follow-up duration, the recurrence rate may be underestimated, thus necessitating a longer follow-up period.
In conclusion, hybrid TaTME, which incorporates the advantages of abdominal robotic surgery and TaTME, is as favorable as conventional TaTME in producing suitable short-term outcomes in low rectal cancer. Further larger-scale studies conducted over a longer period are needed to verify the current findings on this surgical technique.
Data availability
The data presented in this study are available on request from the corresponding author.
References
Heald RJ, Husband EM, Ryall RD (1982) The mesorectum in rectal cancer surgery–the clue to pelvic recurrence? Br J Surg 69:613–616
Campa-Thompson M, Weir R, Calcetera N, Quirke P, Carmack S (2015) Pathologic processing of the total mesorectal excision. Clin Colon Rectal Surg 28:43–52
Quirke P, Steele R, Monson J, Grieve R, Khanna S, Couture J, O’Callaghan C, Myint AS, Bessell E, Thompson LC, Parmar M, Stephens RJ, Sebag-Montefiore D (2009) Effect of the plane of surgery achieved on local recurrence in patients with operable rectal cancer: a prospective study using data from the MRC CR07 and NCIC-CTG CO16 randomised clinical trial. Lancet 373:821–828
Quirke P, Durdey P, Dixon MF, Williams NS (1986) Local recurrence of rectal adenocarcinoma due to inadequate surgical resection. Histopathological study of lateral tumour spread and surgical excision. Lancet 2:996–999
Wibe A, Rendedal PR, Svensson E, Norstein J, Eide TJ, Myrvold HE, Søreide O (2002) Prognostic significance of the circumferential resection margin following total mesorectal excision for rectal cancer. Br J Surg 89:327–334
Birbeck KF, Macklin CP, Tiffin NJ, Parsons W, Dixon MF, Mapstone NP, Abbott CR, Scott N, Finan PJ, Johnston D, Quirke P (2002) Rates of circumferential resection margin involvement vary between surgeons and predict outcomes in rectal cancer surgery. Ann Surg 235:449–457
Targarona EM, Balague C, Pernas JC, Martinez C, Berindoague R, Gich I, Trias M (2008) Can we predict immediate outcome after laparoscopic rectal surgery? Multivariate analysis of clinical, anatomic, and pathologic features after 3-dimensional reconstruction of the pelvic anatomy. Ann Surg 247:642–649
Akiyoshi T, Kuroyanagi H, Oya M, Konishi T, Fukuda M, Fujimoto Y, Ueno M, Miyata S, Yamaguchi T (2009) Factors affecting the difficulty of laparoscopic total mesorectal excision with double stapling technique anastomosis for low rectal cancer. Surgery 146:483–489
Fung A, Trabulsi N, Morris M, Garfinkle R, Saleem A, Wexner SD, Vasilevsky CA, Boutros M (2017) Laparoscopic colorectal cancer resections in the obese: a systematic review. Surg Endosc 31:2072–2088
Jeong SY, Park JW, Nam BH, Kim S, Kang SB, Lim SB, Choi HS, Kim DW, Chang HJ, Kim DY, Jung KH, Kim TY, Kang GH, Chie EK, Kim SY, Sohn DK, Kim DH, Kim JS, Lee HS, Kim JH, Oh JH (2014) Open versus laparoscopic surgery for mid-rectal or low-rectal cancer after neoadjuvant chemoradiotherapy (COREAN trial): survival outcomes of an open-label, non-inferiority, randomised controlled trial. Lancet Oncol 15:767–774
Bonjer HJ, Deijen CL, Abis GA, Cuesta MA, van der Pas MH, de Lange-de Klerk ES, Lacy AM, Bemelman WA, Andersson J, Angenete E, Rosenberg J, Fuerst A, Haglind E (2015) A randomized trial of laparoscopic versus open surgery for rectal cancer. N Engl J Med 372:1324–1332
Stevenson AR, Solomon MJ, Lumley JW, Hewett P, Clouston AD, Gebski VJ, Davies L, Wilson K, Hague W, Simes J (2015) Effect of laparoscopic-assisted resection vs open resection on pathological outcomes in rectal cancer: the ALaCaRT randomized clinical trial. JAMA 314:1356–1363
Fleshman J, Branda M, Sargent DJ, Boller AM, George V, Abbas M, Peters WR Jr, Maun D, Chang G, Herline A, Fichera A, Mutch M, Wexner S, Whiteford M, Marks J, Birnbaum E, Margolin D, Larson D, Marcello P, Posner M, Read T, Monson J, Wren SM, Pisters PW, Nelson H (2015) Effect of laparoscopic-assisted resection vs open resection of stage II or III rectal cancer on pathologic outcomes: the ACOSOG Z6051 randomized clinical trial. JAMA 314:1346–1355
Yamaguchi T, Kinugasa Y, Shiomi A, Tomioka H, Kagawa H, Yamakawa Y (2016) Robotic-assisted vs. conventional laparoscopic surgery for rectal cancer: short-term outcomes at a single center. Surg Today 46:957–962
Jayne D, Pigazzi A, Marshall H, Croft J, Corrigan N, Copeland J, Quirke P, West N, Rautio T, Thomassen N, Tilney H, Gudgeon M, Bianchi PP, Edlin R, Hulme C, Brown J (2017) Effect of robotic-assisted vs conventional laparoscopic surgery on risk of conversion to open laparotomy among patients undergoing resection for rectal cancer: the ROLARR randomized clinical trial. JAMA 318:1569–1580
de Lacy AM, Rattner DW, Adelsdorfer C, Tasende MM, Fernández M, Delgado S, Sylla P, Martínez-Palli G (2013) Transanal natural orifice transluminal endoscopic surgery (NOTES) rectal resection: “down-to-up” total mesorectal excision (TME)–short-term outcomes in the first 20 cases. Surg Endosc 27:3165–3172
Deijen CL, Tsai A, Koedam TW, Veltcamp Helbach M, Sietses C, Lacy AM, Bonjer HJ, Tuynman JB (2016) Clinical outcomes and case volume effect of transanal total mesorectal excision for rectal cancer: a systematic review. Tech Coloproctol 20:811–824
Penna M, Hompes R, Arnold S, Wynn G, Austin R, Warusavitarne J, Moran B, Hanna GB, Mortensen NJ, Tekkis PP (2019) Incidence and risk factors for anastomotic failure in 1594 patients treated by transanal total mesorectal excision: results from the international TaTME registry. Ann Surg 269:700–711
Veltcamp Helbach M, van Oostendorp SE, Koedam TWA, Knol JJ, Stockmann H, Oosterling SJ, Vuylsteke R, de Graaf EJR, Doornebosch PG, Hompes R, Bonjer HJ, Sietses C, Tuynman JB (2020) Structured training pathway and proctoring; multicenter results of the implementation of transanal total mesorectal excision (TaTME) in the Netherlands. Surg Endosc 34:192–201
Larsen SG, Pfeffer F, Kørner H (2019) Norwegian moratorium on transanal total mesorectal excision. Br J Surg 106:1120–1121
Bravo R, Trépanier JS, Arroyave MC, Fernández-Hevia M, Pigazzi A, Lacy AM (2017) Combined transanal total mesorectal excision (taTME) with laparoscopic instruments and abdominal robotic surgery in rectal cancer. Tech Coloproctol 21:233–235
Nikolic A, Waters PS, Peacock O, Choi CC, Rajkomar A, Heriot AG, Smart P, Warrier S (2020) Hybrid abdominal robotic approach with conventional transanal total mesorectal excision (TaTME) for rectal cancer: feasibility and outcomes from a single institution. J Robot Surg 14:633–641
Inoue Y, Ng JY, Chu CH, Lai YL, Huang IP, Yang SH, Chen CC (2022) Robotic or transanal total mesorectal excision (TaTME) approach for rectal cancer, how about both? Feasibility and outcomes from a single institution. J Robot Surg 16:149–157
Oshio H, Oshima Y, Yunome G, Okazaki S, Kawamura I, Ashitomi Y, Musha H, Kawai M, Motoi F (2021) Transanal total mesorectal excision and transabdominal robotic surgery for rectal cancer: a retrospective study. Ann Med Surg (Lond) 70:102902
Matsuda T, Yamashita K, Hasegawa H, Fujikawa M, Sakamoto H, Yamamoto M, Kanaji S, Oshikiri T, Nakamura T, Suzuki S, Kakeji Y (2021) Clinical outcomes of transanal total mesorectal excision using a lateral-first approach for low rectal cancer: a propensity score matching analysis. Surg Endosc 35:971–978
Matsuda T, Yamashita K, Hasegawa H, Takiguchi G, Urakawa N, Yamamoto M, Kanaji S, Oshikiri T, Nakamura T, Suzuki S, Kakeji Y (2021) Transperineal minimally invasive abdominoperineal resection for low rectal cancer: standardized technique and clinical outcomes. Surg Endosc 35:7236–7245
Sylla P, Rattner DW, Delgado S, Lacy AM (2010) NOTES transanal rectal cancer resection using transanal endoscopic microsurgery and laparoscopic assistance. Surg Endosc 24:1205–1210
Sun Y, Xu H, Li Z, Han J, Song W, Wang J, Xu Z (2016) Robotic versus laparoscopic low anterior resection for rectal cancer: a meta-analysis. World J Surg Oncol 14:61
Crippa J, Grass F, Dozois EJ, Mathis KL, Merchea A, Colibaseanu DT, Kelley SR, Larson DW (2021) Robotic surgery for rectal cancer provides advantageous outcomes over laparoscopic approach: results from a large retrospective cohort. Ann Surg 274:e1218–e1222
Prete FP, Pezzolla A, Prete F, Testini M, Marzaioli R, Patriti A, Jimenez-Rodriguez RM, Gurrado A, Strippoli GFM (2018) Robotic versus laparoscopic minimally invasive surgery for rectal cancer: a systematic review and meta-analysis of randomized controlled trials. Ann Surg 267:1034–1046
Roodbeen SX, Spinelli A, Bemelman WA, Di Candido F, Cardepont M, Denost Q, D’Hoore A, Houben B, Knol JJ, Martín-Pérez B, Rullier E, Sands D, Setton I, Van de Steen K, Tanis PJ, Wexner SD, Hompes R, Wolthuis AM (2021) Local recurrence after transanal total mesorectal excision for rectal cancer: a multicenter cohort study. Ann Surg 274:359–366
Ma B, Gao P, Song Y, Zhang C, Zhang C, Wang L, Liu H, Wang Z (2016) Transanal total mesorectal excision (taTME) for rectal cancer: a systematic review and meta-analysis of oncological and perioperative outcomes compared with laparoscopic total mesorectal excision. BMC Cancer 16:380
Deijen CL, Velthuis S, Tsai A, Mavroveli S, de Lange-de Klerk ES, Sietses C, Tuynman JB, Lacy AM, Hanna GB, Bonjer HJ (2016) COLOR III: a multicentre randomised clinical trial comparing transanal TME versus laparoscopic TME for mid and low rectal cancer. Surg Endosc 30:3210–3215
Penna M, Hompes R, Arnold S, Wynn G, Austin R, Warusavitarne J, Moran B, Hanna GB, Mortensen NJ, Tekkis PP (2017) Transanal total mesorectal excision: international registry results of the first 720 cases. Ann Surg 266:111–117
Muratore A, Mellano A, Marsanic P, De Simone M (2015) Transanal total mesorectal excision (taTME) for cancer located in the lower rectum: short- and mid-term results. Eur J Surg Oncol 41:478–483
Acknowledgements
The authors thank Enago (www.enago-jp) for the English language editing.
Funding
Open access funding provided by Kobe University.
Author information
Authors and Affiliations
Contributions
Study conception and design: T.M. Acquisition of data: M.A., R.S., and H.H. Analysis and interpretation of data: M.A., K.Y., H.G., H.H., and N.U. Drafting of the manuscript: M.A. Critical revision of the manuscript: T.M., S.K., T.O., and Y.K.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ando, M., Matsuda, T., Sawada, R. et al. Feasibility and safety of robotic surgery for low rectal cancer combined with transanal total mesorectal excision. Langenbecks Arch Surg 408, 129 (2023). https://doi.org/10.1007/s00423-023-02870-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00423-023-02870-z