Abstract
Purpose
To analyze short-term outcomes of curative-intent cancer surgery in all adult patients diagnosed with colorectal cancer undergoing surgery from January 2010 to December 2019 and determine risk factors for postoperative complications and mortality.
Methods
Retrospective study conducted at a single tertiary university institution. Patients were stratified by age into two groups: < 75 years and ≥ 75 years. Primary outcome was the influence of age on 30-day complications and mortality. Independent risk factors for postoperative adverse events or mortality were analyzed, and two novel nomograms were constructed.
Results
Of the 1486 patients included, 580 were older (≥ 75 years). Older subjects presented more comorbidities and tumors were located mainly in right colon (45.7%). After matching, no between-group differences in surgical postoperative complications were observed. The 30-day mortality rate was 5.3% for the older and 0.8% for the non-older group (p < 0.001). In multivariable analysis, the independent risk factors for postoperative complications were peripheral vascular disease, chronic pulmonary disease, severe liver disease, postoperative transfusion, and surgical approach. Independent risk factors for 30-day mortality were age ≥ 80 years, cerebrovascular disease, severe liver disease, and postoperative transfusion. The model was internally and externally validated, showing high accuracy.
Conclusion
Patients aged ≥ 75 years had similar postoperative complications but higher 30-day mortality than their younger counterparts. Patients with peripheral vascular disease, chronic pulmonary disease, or severe liver disease should be informed of higher postoperative complications. But patients aged ≥ 80 suffering cerebrovascular disease, severe liver disease, or needing postoperative transfusion should be warned of significantly increased risk of postoperative mortality.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Against the background of the progressive ageing of the European population, currently 9.84% of the Spanish population is ≥ 75 years old, and Spain is estimated to become one of the longest-living countries in Europe within 40 years [1]. This trend has serious implications, as older patients needing a surgical resection for colorectal cancer (CRC) are more likely than the non-older to present with medical and surgical postoperative complications [2, 3], probably due to the fact that comorbidities are more frequent and serious in older age patients [4,5,6]. Surgeons are therefore faced with difficult decisions when managing increasingly older patients. It is estimated that postoperative adverse outcomes in this patient subgroup could be substantial, ranging from 6 to 50% [7,8,9,10,11,12]. Higher postoperative mortality rates of up to 20% have also been reported in older patients, mainly during the first 30 days after surgery [4, 5, 9, 11,12,13,14,15,16].
However, age may not be the only variable influencing surgical outcomes in the older. Indeed, some studies found no significant differences in rates of postoperative complications, reoperations, or mortality between patients over or under 80 years of age [6, 13, 17,18,19]. Several factors have been identified that could increase the risk of postoperative adverse events in older patients: comorbidities, male sex, tumor location, operation time, open surgery, and emergent surgery. Interestingly, age has not appeared as a factor increasing postoperative complications or mortality rate [12, 14, 17,18,19,20,21]. Some authors have reported comorbidities as the strongest predictors of postoperative complications in aged patients [8]. Preoperative identification of predictors of surgical complications in older patients could be useful for implementing additional optimization bundles before major surgery.
The aim of this study was to assess postoperative outcomes after curative-intent oncologic surgery for CRC and determine independent risk factors for complications or mortality during the first 30 post-surgery days.
Materials and methods
Study design and setting
This observational study included all adult patients diagnosed with CCR from January 2010 to December 2019 at the Colorectal Surgery Department in a tertiary university institution (University Clinic Hospital of Valencia, Spain). The STROBE guidelines were followed [22]. Tumors were staged according to the 8th edition of the American Joint Committee on Cancer classification. The inclusion criteria were age over 18 years, histological diagnosis of stages I-III colon or rectal adenocarcinoma, indication for elective oncological surgery with curative intent and minimum follow-up of 1 year. Exclusion criteria were appendicular tumor and local rectal excision. Patients were stratified according to significant age-specific cut-off points for this series. The older cohort was matched to the young cohort by propensity score analysis to obtain two comparable patient groups.
Data source and study variables
Patient data were acquired from hospital and primary care clinical records. Patient variables were age, sex, American Society of Anesthesiologists (ASA) score, and comorbid conditions. Patients with severe comorbidities were those with an ASA score of III-IV. Surgery-related variables were surgical procedure (right colectomy, left colectomy, segmental splenic flexure resection, total colectomy, low anterior resection, abdominoperineal resection), surgical approach (laparoscopic or open surgery), duration of operation, anastomosis, and diverting stoma. Tumor variables were tumor location, TNM classification, stage, and grade of differentiation.
Study endpoints and outcome variables
The study endpoint was the impact of age on short-term postoperative results. Outcome variables were complications and mortality during 30 days after the intervention, comparing patient cohorts according to the age-specific cut-off point, including analysis of possible risk factors for postoperative adverse events or mortality. The variable Any complication was defined as any deviation from the normal postoperative course. Adverse outcomes were divided into medical and surgical complications. Clavien-Dindo classification was used to stratify postoperative complications (severe complications were those with a score ≥ III).
Ethics
The study was approved by the local Research Ethics Committee. Informed consent was waived because of the retrospective nature of the study, and the analysis used anonymous clinical data.
Statistical analysis
A descriptive analysis of each variable of the sample was carried out. The normality of the variables was determined by graphic methods. The description of the series was conducted according to age groups. Quantitative variables were expressed as median and range and qualitative variables as percentages. The ASA score was dichotomized to assess the risk factors of the outcome variables. Cut-off points were determined with ROC curves, considering the maximum sensibility and specificity value. Propensity score matching (PSM) was used to minimize potential selection bias. The cohort of older patients was matched to the younger cohort with a ratio 1:1. The confounding variables to calculate the PSM were sex, ASA score, tumor location, surgical procedure, laparoscopic surgery, duration of operation, and diverting stoma. Logistic regression without substitution as an estimation and nearest-neighbor pairing algorithm was performed, using 0.2 of the logarithm of the PSM standard deviation as the caliber (Supplementary File 1). After the PSM, Fisher’s exact test or χ2 tests were used to find possible differences between qualitative variables, while the Mann–Whitney U test was used for quantitative variables. Multivariable analysis with logistic binary regression was conducted to identify independent risk factors for postoperative complications or mortality. Internal validation of the model was performed. External validation was conducted with a sample division validation technique that randomly assigned patients into two subgroups. The model was performed with the training subset, which was 70% of the sample randomly selected, and the test subset was the remaining 30%. ROC curves and forest plots were obtained from the model. Finally, a nomogram was built according to the validated model. P value < 0.05 was considered statistically significant. Statistical analysis was performed using IBM SPSS Statistics for Macintosh, version 25 (IBM Corp., Armonk, N.Y., USA) and R Core Team, 2020 (R Foundation for Statistical Computing, Vienna, Austria).
Results
Descriptive analysis
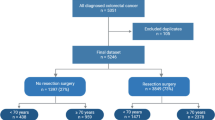
A total of 1486 patients diagnosed with CCR were included in the study across a period of 10 years. Median patient age was 71.0 years (range: 31–95 years). Two different significant age-specific cut-off points were obtained by analyzing the influence of age on postoperative outcomes: 75 years for postoperative complications and 80 years for postoperative mortality. Patients were therefore stratified up to age 75 for sample description and analysis of complications and clustered according to age 80 for mortality assessment. Patients’ characteristics and surgery details are outlined in Tables 1 and 2 by age group. Patients aged over 75 years presented with comorbidities more frequently than non-older subjects. The tumor was more frequently located in the rectum in patients under 75 years (43.3%), whereas the ascending and transverse colon was the most frequent tumor location in the over-75s cohort (45.7%, p < 0.001). Consequently, the non-older group predominantly underwent low anterior resection of the rectum (36.1%), while in the older the main intervention was right colectomy (44.8%, p < 0.001). Anastomosis and diverting stoma were more frequently performed in the under-75s patient subset (89.4% vs. 84.8%; p < 0.001 and 20.1% vs. 9.8%, p < 0.001; respectively). Regarding tumor staging, stages II and III were more common among older patients. Given the significant differences found between the two cohorts, PSM was performed and two completely comparable groups of 438 patients were obtained.
Surgery outcomes
In the cohort of non-older patients, a total of 263 patients (29.0%) presented postoperative complications during the 30 postoperative days, while 39.0% of the older patients suffered any postoperative adverse event (p < 0.001). Table 3 shows surgery outcomes. After matching the two age cohorts, the only differences found between them were in respiratory and cardiac complications. Only cases with anastomosis were included in the analysis of anastomotic failure, without between-group differences. Postoperative transfusion was needed more frequently in patients aged ≥ 75 years. According to the Clavien-Dindo classification, older patients suffered severe complications (≥ III) more often than the younger subset (16.2% vs 11.9%, p < 0.001). The postoperative mortality rate was 2.5% across the whole series. Patients aged ≥ 80 years presented a higher mortality rate during the first 30 postoperative days than those aged under that cutoff (5.3% vs. 0.8%, respectively; p < 0.001) and after matching the two cohorts, these differences remained (p = 0.024).
Risk factors for postoperative complications
We conducted univariable and multivariable analysis of factors associated with postoperative complications. As depicted in the forest plot (Fig. 1), binary logistic regression revealed independent risk factors for presenting any complication to be peripheral vascular disease, chronic pulmonary disease, severe liver disease, and postoperative transfusion. However, the laparoscopic approach was an independent factor predicting a lower postoperative complication rate. All these factors showed a variance inflation factor under 1.5. The model had an area under the curve of 0.69 (IC 95% = 0.65–0.73) and 70.3% accuracy. Age was not an independent risk factor for postoperative complications and moreover showed no association with surgical site infection (p = 0.181), anastomotic leak (p = 0.636), or reoperation rate (p = 0.195).
Risk factors for postoperative mortality
The forest plot of Fig. 2 represents independent risk factors for postoperative mortality obtained from multivariable analysis with binary logistic regression: age ≥ 80 years, cerebrovascular disease, severe liver disease, and postoperative transfusion. Variance inflation factor was lower than 1.3 in all factors. The model presented an area under the curve of 0.90 (IC 95% = 0.83–0.95) and an accuracy of 93.9%.
Nomograms
Two nomograms were constructed to predict the risk of complications and mortality during the postoperative period (Figs. 3, 4). The value of each risk factor is obtained from the upper percentile line, and their sum gives an overall score indicating the probability of postoperative complications or 30-day mortality in the risk line at the bottom. The prognostic nomogram of postoperative complications after colorectal cancer surgery showed an accuracy of 68.4% with an area under the ROC curve of 70%, and the prognostic nomogram of 30-day mortality was able to predict postoperative mortality with an accuracy of 90.2% and an area under the ROC curve of 91%.
Discussion
This is one of the few studies to focus on analysis of independent risk factors for postoperative complications and mortality, employing a substantial sample size with detailed perioperative data and providing a novel nomogram to predict short-term outcomes.
To establish two age groups, the age-specific cut-off point of ≥ 75 years was fitted for the present series, thus providing non-arbitrary sample stratification. In most previous published studies, there is great variability between the age thresholds selected for postoperative outcomes in older patients; they are usually standard cut-off points, not representing inflection points in the series and without medical or biological evidence to support the choice. Some authors also found that age ≥ 75 years could be an optimal cut-off, and age has also been stated as a significant risk factor for postoperative complications in colorectal surgery [12]. After analyzing data on physical and psychological health in the older, the Japanese Geriatrics Society proposed that elderly should be defined as those aged 75 years and older [23]. Nevertheless, other authors classified older patients into three groups: youngest-old (65 to 74 years), middle-old (75 to 84 years) and oldest-old (≥ 85 years) [24].
Comparing the two age groups, older patients had a greater number of comorbidities, which were more also severe. Improvements in perioperative multidisciplinary care have made colorectal surgery feasible in the older despite the fact that they frequently present with serious comorbidities [4,5,6]. Similar to other available studies, in the aged cohort, the tumor was more frequently located in the ascending colon, resulting in a higher ratio of right colectomies [6, 16]. As the two subsets differed in their baseline features, PSM was conducted to obtain two homogeneous groups in order to compare postoperative outcomes. Note that all study patients included received the same perioperative bundle of enhanced recovery after surgery protocols, regardless of age.
Similarly to other authors, we found no differences between older and younger patients in postoperative complication rates, including anastomotic leak [6, 13]. These results support that in patients eligible for colorectal resection, a primary anastomosis can be performed safely without excess risk. A recent systematic review and meta-analysis conducted by Hoshino et al,. focusing on the outcomes of laparoscopic surgery for CCR in older patients, reported slightly higher incidence of postoperative complications in the older, but without differences in anastomotic leak or mortality rates [10].
Our findings revealed that severe postoperative complications were mainly due to worsening of previous comorbidities. Cardiopulmonary complications were more frequent among patients aged ≥ 75 years. Chan et al. also reported pneumonia with respiratory failure as the most common postoperative complication and the leading cause of mortality [17]. In a study of over 1200 CCR patients aged ≥ 85 years undergoing surgical resection, Verweij et al. found high rates of cardiopulmonary complications and excess mortality, particularly in the first year after surgery [11].
The mortality rate for older patients during the postoperative period was 5.3%, in line with outcomes obtained in other studies on octogenarians (2%–13%) and nonagenarians (2%–20%) [4, 5, 9, 11,12,13,14,15,16]. Although older patients may present more comorbidities, several studies found no differences in short-term postoperative reoperations or mortality after colorectal surgery [17,18,19]. Improvements in mortality rates are likely because of advances in perioperative care, safe standardized minimally invasive procedures and better patient selection for surgery. In our experience, although colorectal resection did not involve higher postoperative complication rates in older patients, it did entail higher mortality rates, predominantly in patients with associated comorbidities. Prehabilitation programs could help to optimize preoperative patient status, minimize postoperative risks, and improve surgical outcomes. Furthermore, aged patients without concurrent diseases can be successfully treated by curative-intent surgery. Comorbidities may therefore have more impact on postoperative outcomes than age itself.
Age has long been considered among the predominant risk factors for postoperative complications, but essentially due to an increased number of comorbid conditions and worse functional status [4, 11, 12]. Likewise, multivariable analysis revealed that several comorbidities, but not age, were independent predictors of postoperative complications. Moreover, age did not present any association with surgical site infection, anastomotic leak, or with reoperation rate. These findings are consistent with those obtained from other large series, where age was not predictive of in-hospital complications or mortality, suggesting that other conditions may impact more significantly in surgical outcomes [8, 12, 14, 19, 20, 25]. Therefore, it would be more appropriate to consider a frailty index rather than age in preoperative decision-making. Identification of predictors for surgical complications in elderly frail patients could be useful to implement further optimization bundles before major surgery.
Chronic pulmonary disease was an independent risk factor for postoperative adverse events. In other studies, preoperative cardiopulmonary function was determinant in postoperative outcomes [11, 17]. Respiratory physiotherapy is a good measure to incorporate in perioperative care for older patients, given that it could decrease incidence of postoperative pulmonary complications and 30-day mortality [26].
Severe liver disease is a serious comorbidity and was found to be independently associated with adverse postoperative outcomes. Similarly, a recent meta-analysis concluded that pre-existing liver cirrhosis was associated with higher postoperative major complication and mortality rates following CRC surgery [27]. One reason for this could be that abnormal liver metabolism leads to hepatic coagulopathy, lower albumin levels, reduced drug metabolism, and weakened immune function, increasing postoperative adverse events.
Laparoscopic surgery is safe in older patients, and moreover, postoperative complications including wound infection, ileus, and pneumonia are less frequent than in open surgery [8, 12, 18, 19, 28]. In the present series, laparoscopic approach was found to be independently associated with a lower postoperative complication rate. Similarly, a Dutch population-based study found that compared with open surgery, laparoscopic surgery was independently associated with a lower risk of cardiopulmonary complications and reduced risk of postoperative mortality in elective CCR surgery [21]. Older patients could benefit from laparoscopic surgery despite their limited life expectancy and comorbidities.
Undoubtedly one of the most interesting aspects of our study is the determination of factors influencing postoperative death. In recent years, various prognostic factors for 30-day postoperative mortality have been outlined in older patients, such as age ≥ 85 years, anemia, ASA score IV, and palliative cancer surgery [13]. We found that age ≥ 80 years, cerebrovascular disease, severe liver disease, and need for postoperative transfusion increased the risk of 30-day mortality. Interestingly, advanced age was not predictive of complications, but was revealed as a predictor for postoperative mortality. A possible explanation could be that although older patients present a similar postoperative complication rate to younger ones, recovery is more hazardous in the former group due to their limited physiological reserve, which could entail a higher risk of mortality. These outcomes are in line with those obtained by Youl et al. in a population-based study in Australia which analyzed postoperative outcomes in 18,339 patients aged over 65 years diagnosed with CRC. Among other factors such as advanced tumor stage, open procedure, and emergency surgery, age ≥ 75 years was found to be independently related with an increased risk of postoperative death [12]. Other studies have also concluded that comorbidities were the main factors influencing mortality after surgery, but age itself was not [14, 17, 25].
Another aspect frequently associated with worse postoperative complications potentially leading to increased mortality is the need for postoperative transfusion. As expected, therefore, blood transfusion was revealed as a prognostic factor for 30-day complications and mortality, consistent with the results reported in other studies [16]. Postoperative transfusion may reveal intraoperative bleeding. However, in the present series, the main indication for transfusion was the worsening of preoperative preexisting anemia. Many studies reported worse outcomes when blood transfusion was needed during the postoperative period, particularly in elderly patients. Some authors found that perioperative blood transfusion was a very good predictor of postoperative mortality [29, 30]. Older patients have limited physiological reserve, making this subset of patients especially vulnerable to the consequences of anemia, therefore preoperative optimization of hemoglobin level should be recommended.
Similarly, emergent surgery is known to negatively affect surgical outcomes and has been widely proposed as a predictor of postoperative mortality in older patients [4, 11,12,13,14, 17]. In the present series, however, we included elective surgery only to diminish confounding factors in the analysis and avoid heterogeneity between groups.
The nomograms constructed in the present study are in line with the few that have previously been published. As in Kiran et al., our model was built with a 70% randomly selected study population, and the remaining 30% used to validate it. This ratio was used to avoid overfitting the model. In the multicenter national study conducted by Anaco Study Group, however, the ratio was 60/40 [31, 32]. The models presented similar areas under the curve and share some risk factors. The predictive novel nomograms developed in the present study confirm that prior severe comorbid conditions are the main factors in postoperative short-term outcomes. The nomograms presented herein are useful tools in our setting, as they easily provide individualized risk prediction of postoperative complications or mortality, can help clinicians in preoperative evaluation by providing accurate information about postoperative risks, and could facilitate enhanced, tailored multidisciplinary care to minimize complications.
The study included a relatively large sample with non-arbitrary age cut-off points and two homogeneous patient groups obtained through PSM that received the same perioperative care. The prediction model constructed obtained high accuracy and satisfactory internal and external validation and was presented in the form of a nomogram to facilitate its application by clinicians in outpatient clinics. Nonetheless, this study has some limitations, arising from its observational and retrospective design at a single institution. Patients diagnosed with rectal cancer were included in the study because after the PSM, this subgroup of patients was equally distributed between the two age groups; however, this could be a potential source of bias given that rectal surgery is more complex and time consuming than colon surgery. Data about performance status, frailty, sarcopenia, or nutritional status were not recorded, so accurate information about the functional status of the patients was limited.
Conclusion
Patients aged over 75 years with CCR who underwent oncologic surgery presented a similar complication rate but higher mortality rate than younger patients during the postoperative period. Patients with severe comorbidities (peripheral vascular disease, chronic pulmonary disease, or severe liver disease) should be informed of higher postoperative complications, regardless of age, but patients aged over 80 suffering cerebrovascular disease, or severe liver disease, or needing postoperative transfusion should be warned of a significantly increased risk of postoperative mortality. The novel nomogram proposed herein could help tailor management of patient comorbidities and target perioperative care to improve outcomes.
Data sharing
Data supporting the findings of this study are available from the corresponding author upon reasonable request.
References
GBD (2013) Mortality and Causes of Death Collaborators (2015) Global, regional, and national age–sex specific all-cause and cause-specific mortality for 240 causes of death, 1990–2013: a systematic analysis for the Global Burden of Disease Study 2013. The Lancet 385:117–171. https://doi.org/10.1016/S0140-6736(14)61682-2
Handforth C, Clegg A, Young C et al (2015) The prevalence and outcomes of frailty in older cancer patients: a systematic review. Ann Oncol 26:1091–1101. https://doi.org/10.1093/annonc/mdu540
Baré M, Mora L, Pera M et al (2020) Type and consequences of short-term complications in colon cancer surgery, focusing on the oldest old. Clin Colorectal Cancer 19:e18–e25. https://doi.org/10.1016/j.clcc.2019.11.003
Colorectal Cancer Collaborative Group (2000) Surgery for colorectal cancer in elderly patients: a systematic review. Lancet 356:968–974
Arenal JJ, Tinoco C, Labarga F et al (2012) Colorectal cancer in nonagenarians: colorectal cancer in nonagenarians. Colorectal Dis 14:44–47. https://doi.org/10.1111/j.1463-1318.2011.02596.x
Tokuhara K, Nakatani K, Ueyama Y et al (2016) Short- and long-term outcomes of laparoscopic surgery for colorectal cancer in the elderly: a prospective cohort study. Int J Surg 27:66–71. https://doi.org/10.1016/j.ijsu.2016.01.035
Johnston S, Louis M, Churilov L et al (2020) Health costs of post-operative complications following rectal resection: a systematic review. ANZ J Surg 90:1270–1276. https://doi.org/10.1111/ans.15708
Zeng W-G, Liu M-J, Zhou Z-X et al (2021) Outcomes of colorectal cancer surgery in nonagenarian patients: a multicenter retrospective study. J Gastrointest Oncol 12:1568–1576. https://doi.org/10.21037/jgo-21-324
Tamura K, Matsuda K, Fujita Y et al (2021) Optimal assessment of frailty predicts postoperative complications in older patients with colorectal cancer surgery. World J Surg 45:1202–1209. https://doi.org/10.1007/s00268-020-05886-4
Hoshino N, Fukui Y, Hida K, Sakai Y (2019) Short-term outcomes of laparoscopic surgery for colorectal cancer in the elderly versus non-elderly: a systematic review and meta-analysis. Int J Colorectal Dis 34:377–386. https://doi.org/10.1007/s00384-019-03234-0
Verweij NM, Schiphorst AHW, Maas HA et al (2016) Colorectal cancer resections in the oldest old between 2011 and 2012 in The Netherlands. Ann Surg Oncol 23:1875–1882. https://doi.org/10.1245/s10434-015-5085-z
Youl PH, Theile DE, Moore J et al (2021) Outcomes following major resection for colorectal cancer in patients aged 65+ years: a population-based study in Queensland, Australia. ANZ J Surg 91:932–937. https://doi.org/10.1111/ans.16631
Duron J-J, Duron E, Dugue T et al (2011) Risk factors for mortality in major digestive surgery in the elderly: a multicenter prospective study. Ann Surg 254:375–382. https://doi.org/10.1097/SLA.0b013e318226a959
Ihedioha U, Gravante G, Lloyd G et al (2013) Curative colorectal resections in patients aged 80 years and older: clinical characteristics, morbidity, mortality and risk factors. Int J Colorectal Dis 28:941–947. https://doi.org/10.1007/s00384-012-1626-0
Bessems SAM, Konsten JLM, Vogelaar JFJ et al (2021) Frailty screening by Geriatric-8 and 4-meter gait speed test is feasible and predicts postoperative complications in elderly colorectal cancer patients. J Geriatr Oncol 12:592–598. https://doi.org/10.1016/j.jgo.2020.10.012
Roque-Castellano C, Fariña-Castro R, Nogués-Ramia EM et al (2020) Colorectal cancer surgery in selected nonagenarians is relatively safe and it is associated with a good long-term survival: an observational study. World J Surg Onc 18:120. https://doi.org/10.1186/s12957-020-01895-8
Chan TY, Foo CC, Law WL, Lo O (2019) Outcomes of colorectal cancer surgery in the nonagenarians: 20-year result from a tertiary center. BMC Surg 19:155. https://doi.org/10.1186/s12893-019-0623-4
Peltrini R, Imperatore N, Carannante F et al (2021) Age and comorbidities do not affect short-term outcomes after laparoscopic rectal cancer resection in elderly patients. A multi-institutional cohort study in 287 patients. Updates Surg 73:527–537. https://doi.org/10.1007/s13304-021-00990-z
Utsumi M, Matsuda T, Yamashita K et al (2021) Short-term and long-term outcomes after laparoscopic surgery for elderly patients with colorectal cancer aged over 80 years: a propensity score matching analysis. Int J Colorectal Dis 36:2519–2528
Michaud Maturana M, English WJ, Nandakumar M et al (2021) The impact of frailty on clinical outcomes in colorectal cancer surgery: a systematic literature review. ANZ J Surg 91:2322–2329. https://doi.org/10.1111/ans.16941
Gietelink L, Wouters MWJM, Bemelman WA et al (2016) Reduced 30-day mortality after laparoscopic colorectal cancer surgery: a population based study from the Dutch Surgical Colorectal Audit (DSCA). Ann Surg 264:135–140. https://doi.org/10.1097/SLA.0000000000001412
von Elm E, Altman DG, Egger M et al (2014) The strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. Int J Surg 12:1495–1499. https://doi.org/10.1016/j.ijsu.2014.07.013
Ouchi Y, Rakugi H, Arai H et al (2017) Redefining the elderly as aged 75 years and older: proposal from the Joint Committee of Japan Gerontological Society and the Japan Geriatrics Society: redefining elderly: proposal from Japan. Geriatr Gerontol Int 17:1045–1047. https://doi.org/10.1111/ggi.13118
Lee SB, Oh JH, Park JH et al (2018) Differences in youngest-old, middle-old, and oldest-old patients who visit the emergency department. Clin Exp Emerg Med 5:249–255. https://doi.org/10.15441/ceem.17.261
Tan KY, Kawamura Y, Mizokami K et al (2009) Colorectal surgery in octogenarian patients—outcomes and predictors of morbidity. Int J Colorectal Dis 24:185–189. https://doi.org/10.1007/s00384-008-0615-9
Odor PM, Bampoe S, Gilhooly D, Creagh-Brown B, Moonesinghe SR (2020) Perioperative interventions for prevention of postoperative pulmonary complications: systematic review and meta-analysis. BMJ 368:m540. https://doi.org/10.1136/bmj.m540
Cheng Y-X, Tao W, Zhang H et al (2021) Does liver cirrhosis affect the surgical outcome of primary colorectal cancer surgery? A meta-analysis. World J Surg Onc 19:167. https://doi.org/10.1186/s12957-021-02267-6
Son IT, Kim JY, Kim MJ et al (2021) Clinical and oncologic outcomes of laparoscopic versus open surgery in elderly patients with colorectal cancer: a retrospective multicenter study. Int J Clin Oncol 26:2237–2245. https://doi.org/10.1007/s10147-021-02009-4
Wu W-C, Smith TS, Henderson WG et al (2010) Operative blood loss, blood transfusion, and 30-day mortality in older patients after major noncardiac surgery. Ann Surg 252:11–17. https://doi.org/10.1097/SLA.0b013e3181e3e43f
Roque-Castellano C, Marchena-Gómez J, Fariña-Castro R et al (2016) Perioperative blood transfusion is associated with an increased mortality in older surgical patients. World J Surg 40:1795–1801. https://doi.org/10.1007/s00268-016-3521-2
Sánchez-Guillén L, Frasson M, Pellino G et al (2020) Nomograms for morbidity and mortality after oncologic colon resection in the enhanced recovery era: results from a multicentric prospective national study. Int J Colorectal Dis 35:2227–2238. https://doi.org/10.1007/s00384-020-03692-x
Kiran RP, Attaluri V, Hammel J, Church J (2013) A novel nomogram accurately quantifies the risk of mortality in elderly patients undergoing colorectal surgery. Ann Surg 257:905–908. https://doi.org/10.1097/SLA.0b013e318269d337
Funding
Open Access funding provided thanks to the CRUE-CSIC agreement with Springer Nature.
Author information
Authors and Affiliations
Contributions
Study conception and design: David Moro-Valdezate, José Martín-Arévalo, Óscar Ferro-Echevarría. Acquisition of data: José Martín-Arévalo, Leticia Pérez-Santiago, Óscar Ferro-Echevarría. Analysis and interpretation of data: José Martín-Arévalo, Vicente Pla-Martí, Stephanie García-Botello, Alejandro Espí-Macías. Drafting of manuscript: David Moro-Valdezate, Ricardo Gadea-Mateo, Noelia Tarazona. Critical revision of manuscript: Susana Roselló-Keränen, Alejandro Espí-Macías.
Corresponding author
Ethics declarations
Ethics approval
The study was approved by the local Research Ethics Committee. Informed consent was waived because of the retrospective nature of the study, and the analysis used anonymous clinical data.
Conflict of interest
-
1.
David Moro-Valdezate (MD, PhD, Professor)
Payment or honoraria for lectures, presentations, speaker bureaus or educational events from Johnson & Johnson. Support for attending meetings and/or travel from Takeda.
-
2.
José Martín-Arévalo (MD, PhD, Professor)
Payment or honoraria for lectures, presentations, speaker bureaus or educational events from Johnson & Johnson. Support for attending meetings and/or travel from Takeda.
-
3.
Óscar Ferro-Echevarría (MD)
Declares no relationships, conditions or circumstances that present potential conflict of interest.
-
4.
Vicente Pla-Martí (MD, PhD, Professor)
Payment or honoraria for lectures, presentations, speaker bureaus or educational events from Johnson & Johnson, Medtronic and Braun Medical. Support for attending meetings and/or travel from Takeda.
-
5.
Stephanie García-Botello (MD, PhD, Professor)
Payment or honoraria for lectures, presentations, speaker bureaus or educational events from Johnson & Johnson.
-
6.
Leticia Pérez-Santiago (MD)
Declares no relationships, conditions or circumstances that present potential conflict of interest.
-
7.
Ricardo Gadea-Mateo (MD)
Declares no relationships, conditions or circumstances that present potential conflict of interest.
-
8.
Noelia Tarazona (MD, PhD)
Declares no relationships, conditions or circumstances that present potential conflict of interest.
-
9.
Roda Desamparados (MD, PhD)
Declares no relationships, conditions or circumstances that present potential conflict of interest.
-
10.
Susana Roselló-Keränen (MD, PhD)
Declares no relationships, conditions or circumstances that present potential conflict of interest.
-
11.
Alejandro Espí-Macías (MD, PhD, Professor)
Payment or honoraria for lectures, presentations, speaker bureaus or educational events from Johnson & Johnson, Medtronic and Braun Medical. Support for attending meetings and/or travel from Takeda.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Moro-Valdezate, D., Martín-Arévalo, J., Ferro-Echevarría, Ó. et al. Short-term outcomes of colorectal cancer surgery in older patients: a novel nomogram predicting postoperative morbi-mortality. Langenbecks Arch Surg 407, 3587–3597 (2022). https://doi.org/10.1007/s00423-022-02688-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-022-02688-1