Abstract
Introduction
Intraabdominal visceral obesity may increase technical challenges during laparoscopic rectal resection and hypothetically therefore increase the risk of perioperative complications. The aim of this study was to analyze intraabdominal obesity by means of perirenal fat against risk of adverse outcomes in patients undergoing laparoscopic rectal cancer surgery.
Methods
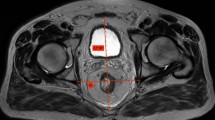
This study was a single-institution retrospective analysis of consecutive patients undergoing laparoscopic total mesorectal surgery for rectal cancer between January 2009 and January 2013. Abdominal CT scans with intravenous contrast were assessed in a blinded manner to estimate the perirenal fat area (cm2).
Result
A total of 195 patients were included (median age 70 years (range 27–87), 58 women and 137 men) for analysis. There was a moderate correlation between BMI and perirenal fat area (r = 0.499, p = 0.001). Perirenal fat area was not associated with any of the measured adverse outcomes. Patients with BMI ≥ 30 had significantly higher intraoperative blood loss (191 mL, p = 0.001).
Conclusion
Perirenal fat area was not an important predictor of adverse outcomes in patients undergoing laparoscopic rectal cancer surgery.

Similar content being viewed by others
References
Kim JY, Kim YW, Kim NK et al (2011) Pelvic anatomy as a factor in laparoscopic rectal surgery: a prospective study. Surg Laparosc Endosc Percutan Tech 21:334–339. https://doi.org/10.1097/SLE.0b013e31822b0dcb
Jung M, Volonté F, Buchs NC et al (2014) Perirenal fat surface area as a risk factor for morbidity after elective colorectal surgery. Dis Colon Rectum 57:201–209. https://doi.org/10.1097/DCR.0000000000000029
Kang J, Baek S-E, Kim T et al (2012) Impact of fat obesity on laparoscopic total mesorectal excision: more reliable indicator than body mass index. Int J Color Dis 27:497–505. https://doi.org/10.1007/s00384-011-1333-2
Ballian N, Lubner MG, Munoz A et al (2012) Visceral obesity is associated with outcomes of total mesorectal excision for rectal adenocarcinoma. J Surg Oncol 105:365–370. https://doi.org/10.1002/jso.22031
Tsujinaka S, Konishi F, Kawamura YJ, et al. (2008) Visceral obesity predicts surgical outcomes after laparoscopic colectomy for sigmoid colon cancer. Dis Colon Rectum 51:1757–65–7. doi: https://doi.org/10.1007/s10350-008-9395-0
Ishii Y, Hasegawa H, Nishibori H et al (2005) Impact of visceral obesity on surgical outcome after laparoscopic surgery for rectal cancer. Br J Surg 92:1261–1262. https://doi.org/10.1002/bjs.5069
Singh A, Muthukumarasamy G, Pawa N et al (2011) Laparoscopic colorectal cancer surgery in obese patients. Color Dis 13:878–883. https://doi.org/10.1111/j.1463-1318.2010.02348.x
Kawasaki S, Aoki K, Hasegawa O et al Sonographic evaluation of visceral fat by measuring para- and perirenal fat. J Clin Ultrasound 36:129–133. https://doi.org/10.1002/jcu.20426
Bulut O, Aslak KK, Levic K et al (2015) A randomized pilot study on single-port versus conventional laparoscopic rectal surgery: effects on postoperative pain and the stress response to surgery. Tech Coloproctol 19:11–22. https://doi.org/10.1007/s10151-014-1237-6
Dindo D, Muller MK, Weber M, Clavien P-A (2003) Obesity in general elective surgery. Lancet (London, England) 361:2032–2035. https://doi.org/10.1016/S0140-6736(03)13640-9
Ballian N, Yamane B, Leverson G et al (2010) Body mass index does not affect postoperative morbidity and oncologic outcomes of total mesorectal excision for rectal adenocarcinoma. Ann Surg Oncol 17:1606–1613. https://doi.org/10.1245/s10434-010-0908-4
Leroy J, Ananian P, Rubino F et al (2005) The impact of obesity on technical feasibility and postoperative outcomes of laparoscopic left colectomy. Ann Surg 241:69–76
Senagore AJ, Delaney CP, Madboulay K et al Laparoscopic colectomy in obese and nonobese patients. J Gastrointest Surg 7:558–561
Delaney CP, Pokala N, Senagore AJ et al (2005) Is laparoscopic colectomy applicable to patients with body mass index >30? A case-matched comparative study with open colectomy. Dis Colon Rectum 48:975–981. https://doi.org/10.1007/s10350-004-0941-0
Manilich E, Vogel JD, Kiran RP et al (2013) Key factors associated with postoperative complications in patients undergoing colorectal surgery. Dis Colon Rectum 56:64–71. https://doi.org/10.1097/DCR.0b013e31827175f6
Benoist S, Panis Y, Alves A, Valleur P (2000) Impact of obesity on surgical outcomes after colorectal resection. Am J Surg 179:275–281
Schwandner O, Farke S, Schiedeck THK, Bruch H-P (2004) Laparoscopic colorectal surgery in obese and nonobese patients: do differences in body mass indices lead to different outcomes? Surg Endosc 18:1452–1456. https://doi.org/10.1007/s00464-003-9259-6
Makino T, Shukla PJ, Rubino F, Milsom JW (2012) The impact of obesity on perioperative outcomes after laparoscopic colorectal resection. Ann Surg 255:228–236. https://doi.org/10.1097/SLA.0b013e31823dcbf7
Thorpe H, Jayne DG, Guillou PJ et al (2008) Patient factors influencing conversion from laparoscopically assisted to open surgery for colorectal cancer. Br J Surg 95:199–205. https://doi.org/10.1002/bjs.5907
Expert Consultation WHO (2004) Appropriate body-mass index for Asian populations and its implications for policy and intervention strategies. Lancet (London, England) 363:157–163. https://doi.org/10.1016/S0140-6736(03)15268-3
Examination Committee of Criteria for “Obesity Disease” in Japan, Japan Society for the Study of Obesity (2002) New criteria for “obesity disease” in Japan. Circ J 66:987–992
Poll L, Wittsack H-J, Willers R et al (2004) Correlation between anthropometric parameters and abdominal fat volumes assessed by a magnetic resonance imaging method in patients with diabetes. Diabetes Technol Ther 6:844–849. https://doi.org/10.1089/dia.2004.6.844
Camhi SM, Bray GA, Bouchard C et al (2011) The relationship of waist circumference and BMI to visceral, subcutaneous, and total body fat: sex and race differences. Obesity (Silver Spring) 19:402–408. https://doi.org/10.1038/oby.2010.248
Keller DS, Madhoun N, Flores-Gonzalez JR et al (2016) Effect of BMI on short-term outcomes with robotic-assisted laparoscopic surgery: a case-matched study. J Gastrointest Surg 20:488–493. https://doi.org/10.1007/s11605-015-3016-8
Kartheuser AH, Leonard DF, Penninckx F et al (2013) Waist circumference and waist/hip ratio are better predictive risk factors for mortality and morbidity after colorectal surgery than body mass index and body surface area. Ann Surg 258:722–730. https://doi.org/10.1097/SLA.0b013e3182a6605a
Rasulov AO, Mamedli ZZ, Gordeyev SS et al (2016) Short-term outcomes after transanal and laparoscopic total mesorectal excision for rectal cancer. Tech Coloproctol 20:227–234. https://doi.org/10.1007/s10151-015-1421-3
Morris K, Tuorto S, Gönen M et al (2010) Simple measurement of intra-abdominal fat for abdominal surgery outcome prediction. Arch Surg 145:1069–1073. https://doi.org/10.1001/archsurg.2010.222
Eisner BH, Zargooshi J, Berger AD et al (2010) Gender differences in subcutaneous and perirenal fat distribution. Surg Radiol Anat 32:879–882. https://doi.org/10.1007/s00276-010-0692-7
Acknowledgements
The authors thank Merete Friis, M.D., at the Department of Radiology, Copenhagen University Hospital Hvidovre, for her help with reviewing and assessing the thoracoabdominal CT scans.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants performed by any of the authors (retrospective study).
Rights and permissions
About this article
Cite this article
Levic, K., Bulut, O., Schødt, M. et al. Increased perirenal fat area is not associated with adverse outcomes after laparoscopic total mesorectal excision for rectal cancer. Langenbecks Arch Surg 402, 1205–1211 (2017). https://doi.org/10.1007/s00423-017-1636-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-017-1636-z