Abstract
Purpose
There is no consensus on how to quantify indocyanine green (ICG) fluorescence angiography. The aim of the present study was to establish and gather validity evidence for a method of quantifying fluorescence angiography, to assess organ perfusion.
Methods
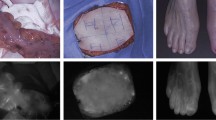
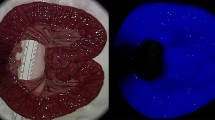
Laparotomy was performed on seven pigs, with two regions of interest (ROIs) marked. ICG and neutron-activated microspheres were administered and the stomach was illuminated in the near-infrared range, parallel to continuous recording of fluorescence signal. Tissue samples from the ROIs were sent for quantification of microspheres to calculate the regional blood flow. A software system was developed to assess the fluorescent recordings quantitatively, and each quantitative parameter was compared with the regional blood flow. The parameter with the strongest correlation was then compared with results from an independently developed algorithm, to evaluate reproducibility.
Results
A strong correlation was found between regional blood flow and the slope of the fluorescence curves (ROI I: Pearson r = 0.97, p < 0.001; ROI II: 0.96, p < 0.001) as the normalized slope (ROI I: Pearson r = 0.92, p = 0.004; ROI II: r = 0.96, p = 0.001). There was acceptable correlation of the slope of the curve between two independently developed algorithms (ROI I+II: Pearson r = 0.83, p < 0.001), and good resemblance was found with the Bland-Altman method, with no proportional bias.
Conclusions
Perfusion assessment with quantitative indocyanine green fluorescence angiography is not only feasible but easy to perform with commercially available equipment and readily accessible software.




Similar content being viewed by others
References
Owens SL (1996) Indocyanine green angiography. Br J Ophthalmol 80:263–266
Raabe A, Beck J, Gerlach R, Zimmermann M, Seifert V (2003) Near-infrared indocyanine green video angiography: a new method for intraoperative assessment of vascular flow. Neurosurgery 52:132–139 discussion 139
Alander JT, Kaartinen I, Laakso A et al (2012) A review of indocyanine green fluorescent imaging in surgery. Int J Biomed Imaging 2012:940585
Boni L, David G, Mangano A et al (2015) Clinical applications of indocyanine green (ICG) enhanced fluorescence in laparoscopic surgery. Surg Endosc 29:2046–2055
Diana M, Halvax P, Dallemagne B et al (2014) Real-time navigation by fluorescence-based enhanced reality for precise estimation of future anastomotic site in digestive surgery. Surg Endosc 28:3108–3118
Toens C, Krones CJ, Blum U et al (2006) Validation of IC-VIEW fluorescence videography in a rabbit model of mesenteric ischaemia and reperfusion. Int J Color Dis 21:332–338
Towle EL, Richards LM, Kazmi SM, Fox DJ, Dunn AK (2012) Comparison of indocyanine green angiography and laser speckle contrast imaging for the assessment of vasculature perfusion. Neurosurgery 71:1023–1030 discussion 1030-1021
Yuasa Y, Seike J, Yoshida T et al (2012) Sentinel lymph node biopsy using intraoperative indocyanine green fluorescence imaging navigated with preoperative CT lymphography for superficial esophageal cancer. Ann Surg Oncol 19:486–493
Ishizawa T, Bandai Y, Ijichi M et al (2010) Fluorescent cholangiography illuminating the biliary tree during laparoscopic cholecystectomy. Br J Surg 97:1369–1377
Degett TH, Andersen HS, and Gogenur I (2016) Indocyanine green fluorescence angiography for intraoperative assessment of gastrointestinal anastomotic perfusion: a systematic review of clinical trials. Langenbecks Arch Surg.
Thompson SK, Chang EY, Jobe BA (2006) Clinical review: healing in gastrointestinal anastomoses, part I. Microsurgery 26:131–136
Chadi SA, Fingerhut A, Berho M, et al. (2016) Emerging trends in the etiology, prevention, and treatment of gastrointestinal anastomotic leakage. J Gastrointest Surg.
Markar S, Gronnier C, Duhamel A et al (2015) The impact of severe anastomotic leak on long-term survival and cancer recurrence after surgical resection for esophageal malignancy. Ann Surg 262:972–980
Mirnezami A, Mirnezami R, Chandrakumaran K et al (2011) Increased local recurrence and reduced survival from colorectal cancer following anastomotic leak: systematic review and meta-analysis. Ann Surg 253:890–899
Karliczek A, Harlaar NJ, Zeebregts CJ et al (2009) Surgeons lack predictive accuracy for anastomotic leakage in gastrointestinal surgery. Int J Color Dis 24:569–576
Urbanavicius L, Pattyn P, de Putte DV, Venskutonis D (2011) How to assess intestinal viability during surgery: a review of techniques. World J Gastrointest Surg 3:59–69
Heymann MA, Payne BD, Hoffman JI, Rudolph AM (1977) Blood flow measurements with radionuclide-labeled particles. Prog Cardiovasc Dis 20:55–79
Lange M, Hamahata A, Traber DL et al (2013) Multiple versus single injections of fluorescent microspheres for the determination of regional organ blood flow in septic sheep. Lab Anim 47:203–209
Reinhardt CP, Dalhberg S, Tries MA, Marcel R, Leppo JA (2001) Stable labeled microspheres to measure perfusion: validation of a neutron activation assay technique. Am J Physiol Heart Circ Physiol 280:H108–H116
Levesque E, Martin E, Dudau D et al (2016) Current use and perspective of indocyanine green clearance in liver diseases. Anaesth Crit Care Pain Med 35:49–57
Diana M, Noll E, Diemunsch P et al (2014) Enhanced-reality video fluorescence: a real-time assessment of intestinal viability. Ann Surg 259:700–707
Woitzik J, Pena-Tapia PG, Schneider UC, Vajkoczy P, Thome C (2006) Cortical perfusion measurement by indocyanine-green videoangiography in patients undergoing hemicraniectomy for malignant stroke. Stroke 37:1549–1551
Altman DG, Bland JM (1983) Measurement in medicine: the analysis of method comparison studies. The Statistician 32:307
James DR, Ris F, Yeung TM et al (2015) Fluorescence angiography in laparoscopic low rectal and anorectal anastomoses with pinpoint perfusion imaging—a critical appraisal with specific focus on leak risk reduction. Color Dis 17(Suppl 3):16–21
Jafari MD, Wexner SD, Martz JE et al (2015) Perfusion assessment in laparoscopic left-sided/anterior resection (PILLAR II): a multi-institutional study. J Am Coll Surg 220(82–92):e81
Guillou PJ, Quirke P, Thorpe H et al (2005) Short-term endpoints of conventional versus laparoscopic-assisted surgery in patients with colorectal cancer (MRC CLASICC trial): multicentre, randomised controlled trial. Lancet 365:1718–1726
Krarup PM, Jorgensen LN, Andreasen AH, Harling H, Danish Colorectal Cancer G (2012) A nationwide study on anastomotic leakage after colonic cancer surgery. Color Dis 14:e661–e667
Protyniak B, Dinallo AM, Boyan WP Jr, Dressner RM, Arvanitis ML (2015) Intraoperative indocyanine green fluorescence angiography—an objective evaluation of anastomotic perfusion in colorectal surgery. Am Surg 81:580–584
Kudszus S, Roesel C, Schachtrupp A, Hoer JJ (2010) Intraoperative laser fluorescence angiography in colorectal surgery: a noninvasive analysis to reduce the rate of anastomotic leakage. Langenbeck’s Arch Surg 395:1025–1030
Acknowledgements
Equipment was kindly provided during the experiments by Karl Storz (Karl Storz GmbH and Co. KG, Tüttlingen, Germany). The study was supported by the Danish Cancer Research Foundation. The study sponsors had no role in the design of the study; the collection, analysis, or interpretation of the data; the writing of the manuscript; or the decision to submit the manuscript for publication.
Author contributions
Study conception and design: NN, HSA, RA, RBS, MBSS, MHM, LBS, and MA. Acquisition of data: NN, HSA, RA, RBS, MBSS, and MHM. Analysis and interpretation of data: NN, HSA, RA, RBS, MBSS, MHM, LBS, and MA. Drafting of manuscript: NN. Critical revision of manuscript: NN, HSA, RA, RBS, MBSS, MHM, LBS, and MA
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All applicable international, national, and/or institutional guidelines for the care and use of animals were followed. All procedures performed in animals were in accordance with the ethical standards of the institution, at which the studies were conducted. The study was conducted under the supervision of research veterinarians at the Department of Experimental Medicine, Panum Institute, University of Copenhagen and was approved by the Danish Animal Experiments Inspectorate (No. 2012-15-2934-00186).
Electronic supplementary material
ESM 1
(DOCX 47 kb)
Rights and permissions
About this article
Cite this article
Nerup, N., Andersen, H.S., Ambrus, R. et al. Quantification of fluorescence angiography in a porcine model. Langenbecks Arch Surg 402, 655–662 (2017). https://doi.org/10.1007/s00423-016-1531-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-016-1531-z