Abstract
Background and aims
There have been many supportive data that the pylorus-preserving pancreatoduodenectomy (PPPD) might be equal to the classic Whipple pancreatoduodenectomy (PD) in terms of oncological radicality. However, few reports are available on the early postoperative and enduring functional changes, nutritional status, body composition, and quality of life years after surgery. The aim of this study was to compare nutritional and functional results of the different techniques in a retrospective evaluation and prospective cohort study.
Patients and methods
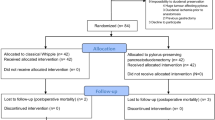
In May 1998, the standard surgical approach in the Department of Surgery, University-Hospital Mannheim, changed from PD to PPPD. The early postoperative and enduring functional changes, quality of life, oncological radicality, and nutritional status after years were compared between 128 patients after PD and 111 patients after PPPD. In a retrospective manner, the intra- and postoperative course was evaluated. In survivors, we prospectively analyzed the functional, nutritional, and oncological outcomes after 54 months (mean) in PD and after 24 months (mean) in PPPD patients.
Results
The PPPD and PD groups did not differ according to age, gender, preoperative condition, or tumor localization. The PPPD group demonstrated favorable results (p<0.05) for operation time (PPPD 341±74 vs PD 386±89 min), blood loss (793±565 vs 1,000±590 ml), blood transfusions (416±691 vs 653±776 ml), delayed gastric emptying (6 vs 13%), and hospital stay (20 vs 24 days). However, a possible bias has to be mentioned since more T4 stages were diagnosed in the PD group (3 vs 11%), and even more extended (venous) resections were performed in the PD group (7 vs 24%). Morbidity (32 vs 30%) and mortality (5 vs 3%) did not differ between the two groups. After 24 months (PPPD, n=22) and 54 months (PD, n=16), there was no difference in global quality of life in recurrence-free patients. While the preoperative body weight was reached after 4 months (median) in the PPPD group, it was reached after 6 months (p<0.05) in the PD group. Bioelectrical impedance analysis (BIA) revealed a significantly (p<0.05) lower total body water (55 vs 60%) and significantly higher total body fat (26 vs 18%) in PPPD than in PD patients. Long-term follow-up showed no significant statistical differences in survival between both groups.
Conclusion
Besides favorable postoperative outcome in specific aspects and equal oncological outcome of PPPD, pylorus preservation seems to have advantages in enduring functional and nutritional status years after surgery for pancreatic cancer.



Similar content being viewed by others
References
Sener SF, Fremgen A, Menck HR, Winchester DP (1999) Pancreatic cancer: a report of treatment and survival trends for 100,313 patients diagnosed from 1985–1995, using the National Cancer Database. J Am Coll Surg 189:1–7
Richter A, Niedergethmann M, Hartel M, Sturm JW, Lorenz D, Trede M, Post S (2002) Resection for malignancies of the pancreatic head in patients over 70 years. Eur J Surg 168:6
Trede M, Schwall G, Saeger HD (1990) Survival after pancreatduodenectomy. 118 consecutive resections without an operative mortality. Ann Surg 211:447–451
Trede M, Richter A, Wendl K (2001) Personal observations, opinions, and approaches to cancer of the pancreas and the periampullary area. Surg Clin North Am 81:595–610
Gebhardt C, Meyer W, Reichel M, Wünsch PH (2000) Prognostic factors in the operative treatment of ductal pancreatic carcinoma. Langenbecks Arch Surg 385:14
Yeo CJ, Cameron JL, Sohn TA, Lillemoe KD, Pitt HA, Talamini MA et al (1997) Six hundred fifty consecutive pancreaticoduodenectomies in the 1990s: pathology, complications, and outcomes. Ann Surg 226:248–257
Oettle H, Riess H (2002) Gemcitabine in combination with 5-fluorouracil with or without folinic acid in the treatment of pancreatic cancer. Cancer 15(95):912–922
Neoptolemos JP, Stocken DD, Dunn JA, Almond J, Beger HG, Pederzoli P et al (2001) Influence of resection margins on survival for patients with pancreatic cancer treated by adjuvant chemoradiation and/or chemotherapy in the ESPAC-1 randomized controlled trial. Ann Surg 234:758–768
Niedergethmann M, Farag-Soliman M, Post S (2004) Postoperative complications of pancreatic cancer surgery. Minerva Chir 59:175–183
Gouma DJ, van Geenen RC, van Gulik TM, de Haan RJ, de Wit LT, Busch OR et al (2000) Rates of complications and death after pancreaticoduodenectomy: risk factors and the impact of hospital volume. Ann Surg 232:786–795
Ohtsuka T, Yamaguchi K, Ohuchida J, Inoue K, Nagai E, Chijiwa K, Tanaka M (2003) Comparison of quality of life after pylorus-preserving pancreatoduodenectomy and Whipple resection. Hepatogastroenterology 50:846–850
Horstmann O, Markus P, Ghadimi M, Becker H (2004) Pylorus preservation has no impact on delayed gastric emptying after pancreatic head resection. Pancreas 28:69–74
Kozuscheck W, Reith HB, Waleczek H, Haarmann W, Edelmann M, Sonntag D (1994) A comparison of long-term results of the standard Whipple procedure and the pylorus preserving pancreatoduodenectomy. J Am Coll Surg 178:443
Wenger FA, Jacobi CA, Haubold K, Zieren HU, Müller JM (1999) Gastrointestinal quality of life after duodenopancreatectomy in pancreatic carcinoma. Preliminary results of a prospective randomized study: pancreatoduodenectomy or pylorus-preserving pancreatoduodenectomy. Chirurg 70:1454–1459
Bassi C, Falconi M, Salvia R, Mascetta G, Molinari E, Pederzoli P (2001) Management of complications after pancreaticoduodectomy in a high volume centre: results on 150 consecutive patients. Dig Surg 18:453–458
Yeo CJ, Cameron JL, Maher MM, Sauter PK, Zahurak ML, Talamini MA et al (1995) A prospective randomized trial of pancreaticogastrostomy versus pancreaticojejunostomy after pancreaticoduodenectomy. Ann Surg 222:580–588
Tran KT, Smeenk HG, van Eijck CH, Kazemier G, Hop WC, Greve JW, Terpstra OT, Zijlstra JA, Klinkert P, Jeekel H (2004) Pylorus preserving pancreaticoduodenectomy versus standard Whipple procedure: a prospective, randomized, multicenter analysis of 170 patients with pancreatic and periampullary tumors. Ann Surg 240:738–745
Di Carlo V, Zerbi A, Balzano G, Corso V (1999) Pylorus-preserving pancreaticoduodenectomy versus conventional Whipple operation. World J Surg 23:920–929
Klinkenbijl JHG, van der Schelling GP, Hop WCJ, van Pel R, Bruining HA, Jeekel J (1992) The advantages of pylorus preserving pancreatoduodenectomy in malignant disease of the pancreas and periampullary region. Ann Surg 216:142–147
Lin PW, Lin YJ (1999) Prospective randomized comparison between pylorus-preserving and standard pancreaticoduodenectomy. Br J Surg 86:603–607
Seiler CA, Wagner M, Sadowski C, Kulli C, Büchler MW (2000) Randomized prospective trial of pylorus-preserving vs. classic duodenopancreatectomy (Whipple procedure): initial clinical results. J Gastrointest Surg 4:443–452
Horstmann O, Becker H, Post S, Nustede R (1999) Is delayed gastric emptying following pancreaticoduodenectomy related to pylorus preservation? Langenbecks Arch Surg 384:354–359
Watson K (1944) Carcinoma of ampulla of Vater. Successful radical resection. Br J Surg 31:368
Traverso LW, Longmire WP (1978) Preservation of the pylorus in pancreaticoduodenectomy. Surg Gynecol Obstet 146:959–962
Post S, Niedergethmann M (2003) Die Resektion des Pankreaskopftumors. In: Büchler MW, Löhr JM (eds) Das Pankreaskarzinom. Unimed Verlag, Bremen, pp 124–140
Seiler CA, Wagner M, Büchler MW (1994) The role of pylorus-preserving duodenopancreatectomy in pancreatic cancer. Dig Surg 11:390–396
Bell RH (2004) Save the pylori. Ann Surg 240:746–747
Warshaw AL, Torchiana DL (1985) Delayed gastric emptying after pylorus preserving pancreaticoduodenectomy. Surg Gynecol Obstet 160:1
Roder JD, Stein HJ, Huttl W, Siewert JR (1995) Pylorus preserving versus standard pancreatoduodenectomy. Br J Surg 82:975
Murakami H, Suzuki H, Nakamura T (2002) Pancreatic fibrosis correlates with delayed gastric emptying after pylorus-preserving pancreaticoduodenectomy with pancreaticogastrostomy. Ann Surg 235:240–245
Riediger H, Makowiec F, Schareck WD, Hopt UT, Adam U (2003) Delayed gastric emptying after pylorus-preserving pancreaticoduodenectomy is strongly related to other postoperative complications. J Gastrointest Surg 7:758–765
Abrams RA, Lillemoe KD, Piantadosi S (2001) Continuing controversy over adjuvant therapy of pancreatic cancer. Lancet 10(358):1565–1566
Van Berge Henegouwen MI, van Gulik TM, DeWit LT, Allema JH, Rauws EA, Obertop H (1997) Delayed gastric emptying after standard pancreaticoduodenectomy versus pylorus-preserving pancreaticoduodenectomy: an analysis of 200 consecutive patients. J Am Coll Surg 185:373–379
Cameron JL, Pitt HA, Yeo CJ, Lillemoe KD, Kaufman HS, Coleman J (1993) One hundred and forty-five consecutive pancreaticoduodenectomies without mortality. Ann Surg 217:430–435
Tanaka M, Sarr MG (1987) Total duodenectomy: effect on canine gastrointestinal motility. J Surg Res 42:483–493
Grace PA, Pitt HA, Longmire WP (1986) Pancreaticoduodenectomy with pylorus preservation for adenocarcinoma of the head of the pancreas. Br J Surg 73:647–650
Itani KM, Coleman RE, Meyers WC (1986) Pylorus-preserving pancreaticoduodenectomy. A clinical and physiological appraisal. Ann Surg 204:655–664
Ohwada S, Satoh Y, Kawate S, Yamada T, Kawamura O, Koyama T et al (2001) Low-dose erythromycin reduces delayed gastric emptying and improves gastric motility after Billroth I pylorus-preserving-pancreaticoduodenectomy. Ann Surg 234:668–674
Boettger TC, Engelmann R, Junginger T (2002) Ante-oder retrokolische Duodenojejunostomie nach pyloruserhaltender Duodenopankreatektomie—eine prospektiv randomisierte Studie. Langenbecks Arch Surg
Ohta T, Nagakawa Z, Ueno K (1993) The mode of lymphatic and local spread of pancreatic carcinoma less than 4.0 in size. Int Surg 78:208
Gupta R, Ihmaidat H (2003) Nutritional effects of oesophageal, gastric and pancreatic carcinoma. Eur J Surg Oncol 29(8):634–643
Wigmore SJ, Plester CE, Richardson RA, Fearon KC (1997) Changes in nutritional status associated with unresectable pancreatic cancer. Br J Cancer 75(1):106–109
De Wys WD (1980) Nutritional care of the cancer patient. JAMA 244(4):374–376
Brennan MF, Pisters PW, Posner M et al (1994) A prospective randomized trial of total parenteral nutrition after major pancreatic resection for malignancy. Ann Surg 220:436–441
Giacosa A, Frascio F, Sukkar SG, Roncella S (1996) Food intake and body composition in cancer cachexia. Nutrition 12:20–23
Kern KA, Norton JA (1988) Cancer cachexia. JPEN J Parenter Enteral Nutr 12(3):286–298
Author information
Authors and Affiliations
Corresponding author
Additional information
Marco Niedergethmann, M.D. and Edward Shang, M.D., contributed to this work equally.
Rights and permissions
About this article
Cite this article
Niedergethmann, M., Shang, E., Farag Soliman, M. et al. Early and enduring nutritional and functional results of pylorus preservation vs classic Whipple procedure for pancreatic cancer. Langenbecks Arch Surg 391, 195–202 (2006). https://doi.org/10.1007/s00423-005-0015-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-005-0015-3