Abstract
Purpose
To investigate the impact of soccer training on cardiac adaptations in mildly hypertensive middle-aged women.
Methods
Hypertensive premenopausal women (n = 41; age (mean ± SD): 44 ± 7 years; height: 166 ± 6 cm; weight: 78.6 ± 11.6 kg; body fat: 43.3 ± 5.2%) were randomized to soccer training (SOC, n = 21) or control (CON, n = 20). SOC performed three weekly training sessions for 15 weeks, whereas CON had no training or lifestyle changes during the same period. Cardiac structure and function were assessed by echocardiography pre-intervention and post-intervention.
Results
Soccer training increased (P = 0.001) left ventricular mass index by 10% [95% CI 4; 15], while no changes occurred in CON (time × group interaction, P = 0.005). In addition, only SOC demonstrated a within-group increase (P = 0.01) of 8% [95% CI 2; 14] in left ventricular septum diameter. For markers of right ventricular remodelling, a within-group increase (P = 0.02) occurred for tricuspid annulus plane systolic excursion of 8% [95% CI 1; 14] in SOC only. Left atrial diameter index increased (P < 0.001) by 6% [95% CI 3; 10] after SOC, while it was unaffected in CON (time × group interaction, P = 0.02). For makers of diastolic function, SOC demonstrated a within-group increase (P = 0.02) in the average early diastolic mitral annulus velocity of 10% [95% CI 2; 19]. In addition, a reduction (P < 0.001) in mitral valve A velocity of − 19% [95% CI − 29; − 10] was observed following soccer training, which manifested in increased (P < 0.001) mitral valve E/A ratio of 34% [95% CI 16; 53] in SOC. No within-group changes were apparent in CON.
Conclusion
In sedentary, mildly hypertensive, middle-aged women, 15 weeks of soccer training increases left ventricular mass and left atrial diameter and improves indices of left ventricular diastolic function.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In developed countries, cardiovascular disease (CVD) remains the leading cause of mortality (Townsend et al. 2022). The burden of CVD can be largely explained by means of the traditional risk factors affecting both genders, including smoking, elevated cholesterol levels, physical inactivity, overweight, diabetes and arterial hypertension (Jagannathan et al. 2019; Appelman et al. 2014). However, compelling evidence indicates robust and independent CVD risk factors that are exclusive to women (Sattar and Greer 2002; Rosano et al. 2007), including disorders of pregnancy, polycystic ovarian syndrome, premature menopause and menopause (Appelman et al. 2014; Harvey et al. 2015; Cho et al. 2020), which emphasizes the importance of gender-specific guidelines for CVD prevention and treatment.
In 1999, women-specific guidelines for CVD prevention were developed by the American Heart Association (AHA) (Mosca et al. 1999), which emphasized the importance of regular physical exercise as an adjunct to the pharmacological treatment and prevention of CVD. Specifically, the most recent women-specific guidelines from AHA (Arnett et al. 2019) recommend at least 150 min per week of moderate-intensity physical activity or 75 min of vigorous-intensity physical activity weekly. However, the optimal characteristics of the training programme to reduce CVD risk factors including health-beneficial changes in cardiac structure and function have not been clearly defined or identified.
Recent studies from our group indicate that soccer training can be an effective tool in the primary and secondary prevention of CVD by reducing numerous cardiovascular risk factors in both healthy and hypertensive individuals (Krustrup et al. 2018, 2010; Milanović et al. 2019; Andersen et al. 2010). For instance, Andersen et al. (2010) demonstrated that 16 weeks of soccer training induced substantial changes in cardiac dimensions and improved both left ventricular systolic and diastolic function in sedentary healthy premenopausal females, and Krustrup et al. (2010) reported that 16 weeks of recreational soccer training resulted in improved pulse pressure wave augmentation index, a marker of arterial stiffness in untrained healthy premenopausal women.
Thus, the main purpose of the present study was to investigate the effects of 15 weeks of recreational soccer training on cardiac structure and function in sedentary, mildly hypertensive, middle-aged women using conventional echocardiography, TDI and speckle tracking analysis. We hypothesized that the applied soccer training protocol would induce robust cardiac adaptations due to substantial cardiovascular loading during the training sessions.
Materials and methods
Compliance with ethical standards
The experimental protocol conformed to the standards set by the Declaration of Helsinki and was approved by the ethical committee of the Faroe Islands and the Sport and Health Sciences Research Ethics Committee at the University of Exeter, Exeter, United Kingdom. After being informed verbally and in writing of the experimental procedures and associated risks, all the participants gave their written consent to take part in the study.
Participants
Sedentary, mildly hypertensive, premenopausal women (n = 41) with average (± SD) age, height, weight, body fat and systolic/diastolic blood pressure of 44 ± 7 years, 166 ± 6 cm, 78.6 ± 11.6 kg, 43.3 ± 5.2% and 137 ± 7/84 ± 5 mmHg, respectively, were recruited for the study.
Experimental design
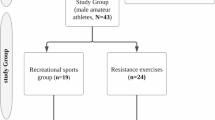
The study was designed as a randomized controlled trial and parts of the obtained data have been reported elsewhere (Mohr et al. 2014, 2015; Nordsborg et al. 2015). After an initial screening of 262 women volunteers, the participants were enrolled in the study based on selection criteria of a sedentary lifestyle for at least 2 years, mild hypertension (mean arterial pressure of 96–110 mmHg) and body mass index of at least 25 kg/m2. Moreover, solely premenopausal women were included. The participants were randomized into one of two intervention groups: a soccer training group (SOC, n = 21; age: 45 ± 5 years; height: 165 ± 7 cm; weight: 79.8 ± 12.8 kg) or a control group (CON, n = 20; age: 43 ± 4 years; height: 166 ± 6 cm; weight: 77.3 ± 10.4 kg). Soccer training was performed three times a week for 15 weeks, whereas CON had no training or lifestyle changes during the same period. Within 10 days before initiation of the intervention and 48–72 h after the last training session, all participants underwent echocardiography. Dietary intake was not controlled during the intervention, and the experimental days were not timed in relation to the menstrual cycle.
Training intervention
SOC completed a total of 45 ± 3 training sessions over the 15-week intervention period. All SOC training sessions lasted 1 h and consisted of small-sided soccer games (4 vs 4 to 8 vs 8) as previously described (Krustrup et al. 2018). A trained soccer coach was present during all sessions to control the duration of the training and ensure competitive games. Heart rate was measured during a training session in the 1st and 15th week of training in order to describe the cardiovascular loading during the training sessions.
Echocardiography
Echocardiography was performed by a single experienced cardiologist, who was blinded to the experimental groups and pre-/post measurements on a GE Vivid E9 ultrasound (GE Medical System, Horten, Norway) with a 2.5 MHz transducer and subjects in the left lateral supine position as described previously (Hansen et al. 2013; Sjúrðarson et al. 2022). Analysis was performed offline using a commercially available software program (EchoPac, GE Medical System, Norway). In brief, two-dimensional (2D) ultrasound imaging, M-mode imaging, and pulsed-wave conventional and tissue Doppler measurements were produced, with measurements of LV and RV dimensions and interventricular septum thickness in parasternal long-axis 2D recordings at mid-ventricular level, and LV volumes and ejection fraction were calculated using Simpson’s biplane method (Schiller et al. 1989). Left atrium (LA) diameter was also measured in parasternal long-axis 2D recordings. Pulsed Doppler measurements of mitral inflow were performed in the apical four-chamber view to determine peak transmitral flows in early diastole (E) and during LA contraction (A), E/A ratio and deceleration time of early filling velocity curves. RV systolic function was assessed by TAPSE using M-mode echocardiography in the apical four-chamber view and TAPSE measured as the total displacement of the tricuspid annulus in the longitudinal direction from end diastole to end systole. In addition, pulsed-wave tissue Doppler imaging was performed in four-chamber apical projections of the medial and lateral myocardial wall to assess average early diastolic mitral annulus velocity (E′) (Sjúrðarson et al. 2022). For speckle tracking analysis, 2D images recorded with a frame rate of > 80 Hz from the standard apical view were analysed to track movements of “speckles” over the cardiac cycle. LV global longitudinal strain was calculated as an average of maximal systolic strains in all myocardial segments determined from apical projections as performed previously (Leitman et al. 2004; Reisner et al. 2004). Examples of representative original echocardiography images are shown in Fig. 1. Finally, indexed values were adjusted for body surface area (BSA) calculated with the Mosteller equation (BSA = square root of the height (cm) multiplied by the weight (kg) divided by 3600).
Representative Doppler echocardiographic images from before and after the intervention. Top: pulsed Doppler mitral inflow before (left) and after (right) the intervention indicating early (E wave) and late (A wave) diastolic transmitral flow. Bottom: pulsed-wave tissue Doppler measurement in the lateral mitral annulus before (left) and after (right) the intervention used to evaluate E′
Statistical analysis
Data are presented as means with 95% confidence intervals. Specific statistical analyses (using SPSS v. 27.0.0, IBM) were applied to answer the primary hypothesis. Continuous endpoints were analysed by a linear mixed model repeated measures approach by means of the SPSS mixed method (Cnaan et al. 2005). ‘Participant number’ specified random variation, and a repeated effect for time was included in the model. Main effects for ‘time’ (pre vs. post), ‘group’ (SOC and CON) and ‘time’ × ‘group’ interactions were further explored by Sidak-adjusted pairwise comparisons. Homogeneity of residual variance and the normality of the residuals were visually checked for all of the obtained data. The level of statistical significance was set at P < 0.05.
Results
Cardiac adaptions
All obtained cardiac measures were similar between SOC and CON at baseline (Table 1).
Left ventricular remodelling
Soccer training increased (P = 0.001) left ventricular mass index by 10% [4;15], whereas no changes were observed in CON (time × group, P = 0.005; Fig. 2). In addition, a main effect of time was observed for left ventricular septum diameter index. The pairwise comparison revealed a within-group increase (P = 0.01) of 8% [2;14] in left ventricular septum diameter index after SOC only (Table 1), but no significant between-group effect existed (time × group, P = 0.16; Table 1). No within-group or between-group change was observed for left ventricular internal dimension index at end diastole or end systole (Table 1).
Mean values for left ventricular diastolic mass index in histograms with individual participants as dotted lines in the soccer group and the control group measured pre-intervention (white bars) and post-intervention (grey bars). *denotes a “time × group” interaction at P < 0.05. The result of the post hoc analysis is indicated by ##P < 0.01 compared with pre-intervention
Right ventricular remodelling
No time × group interaction was observed for markers of right ventricular adaptations, but a main effect of time existed for tricuspid annulus plane systolic excursion. The post hoc analysis revealed a within-group increase (P = 0.02) in tricuspid annulus plane systolic excursion of 8% [1; 14] in SOC only (Table 1).
Markers of diastolic function
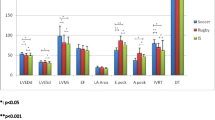
For markers of diastolic function, a main effect of time existed for the mitral valve E/A ratio, the average early diastolic mitral annulus velocity E′ and the mitral valve A velocity. Specifically, the pairwise comparisons revealed a within-group increase (P < 0.001) in the mitral valve E/A ratio of 34% [16;53] (P < 0.001) and in the average early diastolic mitral annulus velocity E′ of 10% [2;19] (P = 0.02) in SOC only, but no statistical differences between groups existed (Fig. 3A, B). Furthermore, a reduction (P < 0.001) in mitral valve A velocity of − 19% [− 29; − 10] was observed after SOC only, resulting in a 19% [4;34] lower (P = 0.02) mitral valve A velocity in SOC compared to CON post-intervention (Table 1). Finally, soccer training increased (P < 0.001) left atrial diameter index by 6% [3;10], whereas it was unaffected in CON (time × group, P = 0.02; Fig. 3D).
Mean values for the mitral valve E/A ratio (A), the average early diastolic mitral annulus velocity (B), the ratio of average E to E′ (C) and the left atrial diameter index (D) in histograms with individual participants as dotted lines in the soccer group and the control group measured pre-intervention (white bars) and post-intervention (grey bars). *denotes a “time × group” interaction at P < 0.05. The result of the post hoc analysis is indicated by #P < 0.05, ###P < 0.001 compared with pre-intervention
Markers of systolic function
No between-group or within-group effect existed for global longitudinal strain or left ventricular ejection fraction (Table 1).
Discussion
The present study investigated the effect of 15 weeks of soccer training on cardiac function and structure in middle-aged, sedentary, hypertensive women. Notably, 15 weeks of soccer training induced substantial increases in left ventricular mass and left atrial diameter compared to habitually active controls. In addition, significant within-group adaptations were observed for left ventricular septum diameter, tricuspid annulus plane systolic excursion, the average early diastolic mitral annulus E′, mitral valve A velocity and mitral valve E/A ratio in response to the soccer training only. Thus, our findings, which are supported by long-term trials in men (Andersen et al. 2014), indicate beneficial effects of 15 weeks of soccer training on key components for cardiac health in middle-aged sedentary hypertensive women.
Several randomized controlled trials have shown broad-spectrum health effects of 3–4 months of soccer training for untrained women (Krustrup et al. 2018). These findings are additionally supported by meta-analysis evidence that demonstrated beneficial effects on cardiovascular disease risk factors (Milanović et al. 2019, 2015) and superior effects of complex or hybrid training regimes compared to conventional endurance, high-intensity interval and resistance training protocols (Batrakoulis et al., 2022). However, few studies have investigated the impact of recreational soccer training on cardiac health.
The applied soccer training intervention effectively increased left ventricular mass compared to the control group. This observation, in conjunction with the within-group increase in left ventricular septum diameter in SOC, indicates that 15 weeks of soccer training with 3 weekly 1-h sessions is potent enough to induce concentric cardiac remodelling in sedentary, mildly hypertensive women. In accordance with this, Arbab-Zadeh et al. (2014) demonstrated that 3 months of endurance training generates concentric remodelling, including a ~ 12% and ~ 15% increase in left ventricular mass and left ventricular mean wall thickness, respectively, in previously sedentary, healthy individuals. In addition, a ~ 6% increase in left ventricular posterior wall thickness has been reported after 16 weeks of soccer training in healthy, previously sedentary women (Andersen et al. 2010). In contrast, no training-induced change existed for the left ventricular internal dimension at end diastole in the present study, which may require long-term exercise protocols to expose. Indeed, Arbab-Zadeh et al. (2014) reported no significant change in left ventricular end-diastolic volume after 3 months of endurance training, but reported a significant 8% increase after 6 months of endurance training. In contrast, Andersen et al. (2010) reported a 13% and 12% increase in left ventricular end-diastolic volume and right ventricle diastolic diameter, respectively, after 16 weeks of soccer training in healthy, previously sedentary women.
Although no time × group interaction existed for tricuspid annulus plane systolic excursion, a marker of right ventricular systolic function (Meluzín et al. 2001; Aloia et al. 2016), it should be pointed out that tricuspid annulus plane systolic excursion increased after soccer training. Accordingly, Andersen et al. (2010) demonstrated a substantial 16% increase in tricuspid annulus plane systolic excursion in response to 16 weeks of soccer training in healthy, previously sedentary women, and a study in untrained men reported augmented tricuspid annular plane systolic excursion after 3 months of soccer training (Andersen et al. 2014). Studies have demonstrated that the time course of the adaptive response in different cardiac variables to exercise training differs (Arbab-Zadeh et al. 2014; Fujimoto et al. 2010). Thus, our training intervention may have been too short to induce a significant between-group interaction.
In relation to markers of diastolic cardiac function, the applied soccer training protocol provoked a pronounced increase in left atrial diameter compared to the control group. Enlarged atrial diameter is an expected adaptation to endurance exercise training in healthy individuals (Sjúrðarson et al. 2022; Mahjoub et al. 2019), but even though enlarged cardiac chamber volumes are seen as typical observations amongst endurance-trained athletes (Maron and Pelliccia 2006), the clinical impact of left atrial expansion in borderline hypertensive women is unknown. While no time × group effect was observed for any of the other markers of diastolic function, it should be noted that the soccer training induced marked within-group decreases in mitral valve A velocity and thereby an increase in mitral valve E/A ratio promoting a shift towards a more passive filling of the left ventricle during diastole in the soccer group. Furthermore, a within-group increase in E′ supports an improved diastolic left ventricular function in the soccer group. In support, Andersen et al. (2010) reported that 16 weeks of soccer training in healthy, sedentary women induced substantial improvements in left ventricular diastolic function in terms of mitral valve A velocity, mitral valve E/A ratio and E′. Collectively, these findings indicate that short-term soccer training, and hence, the combination of fast accelerations in heart loading and time spent in high heart rate zones can induce health-beneficial adaptations in diastolic function. The observed adaptations were, however, relatively small, and future studies should aim to further elucidate the long-term clinical effects.
Although CVD accounts for the majority of deaths amongst women, epidemiological studies have shown that premenopausal women are somewhat protected against developing CVD compared to males, which is demonstrated by a delayed presentation of CVD (Rosano et al. 2007; Vitale et al. 2009; Khoudary et al. 2020; Kannel et al. 1976; Iorga et al. 2017). The later onset of CVD in premenopausal women is attributed at least in part to the levels of the female hormone, oestrogen, which confers cardioprotection through a plethora of mechanisms that reduce oxidative stress, augment angiogenesis and improve vascular function (Rosano et al. 2007; Iorga et al. 2017). In support, the incidence of CVD increases considerably after the menopause, which coincides with an increase in numerous traditional CVD risk factors, including elevated blood pressure, endothelial dysfunction and vascular inflammation (Rosano et al. 2007). Thus, studies investigating the impact on cardiac health in women approaching the menopause such as the present study are highly warranted. Despite a somewhat unclear adaptive response in some of the obtained cardiac measures, the present findings indicate that sedentary premenopausal women with moderate arterial hypertension can benefit from 15 weeks of soccer training with respect to both cardiac structure and function. Future studies using longer training interventions should explore this further. It should be noted that blood pressure, total body weight, body composition and blood lipid profile were also measured pre- and post-intervention, and these data have been reported elsewhere (Mohr et al. 2014). Briefly, 15 weeks of soccer training induced marked reductions in systolic blood pressure (− 12 mmHg) and diastolic blood pressure (-6 mmHg), whereas no changes were apparent in CON. The change in total body weight was not statistically different between groups, but the change in total body fat mass was significantly different in SOC (− 2.3 kg) compared to CON (0.4 kg), and the changes in both total cholesterol (SOC: − 0.4 mmol/L vs. CON: 0.1 mmol/L) and triglycerides (SOC: − 0.2 mmol/L vs. CON: 0.3 mmol/L) were statistically different between SOC and CON (Mohr et al. 2014).
Our study has some limitations. Firstly, the cardiovascular effects of exercise training in our population of sedentary, mildly hypertensive middle-aged women might affect other parameters than the ones examined, including vascular stiffness that has been proven to increase before the manifestation of left ventricular hypertrophic remodelling (Kyhl et al. 2021).
The strength of strain analysis is that it is an objective measure that is able to detect miniscule changes in cardiac performance on a continuous scale. However, only GLS was available in the present study. Radial, circumferential, and transverse strain, which might have added information to the present study, were not performed. Finally, adjustment for multiple tests using the Sidak correction might lead to an increased risk of type II errors, and thus, it should be taken into account that an actual effect might have been missed.
In conclusion, 15 weeks of soccer training induces marked increases in left ventricular mass and left atrial volume in middle-aged, sedentary, hypertensive women and promotes signs of improved left ventricular filling. Thus, the present findings indicate a substantial cardiac plasticity to short-term soccer training in sedentary, mildly hypertensive women.
Data availability
The data sets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Aloia E, Cameli M, D’Ascenzi F, Sciaccaluga C, Mondillo S (2016) TAPSE: an old but useful tool in different diseases. Int J Cardiol 225:177–183
Andersen LJ, Hansen PR, Søgaard P, Madsen JK, Bech J, Krustrup P (2010) Improvement of systolic and diastolic heart function after physical training in sedentary women. Scand J Med Sci Sports 20(Suppl 1):50–57. https://doi.org/10.1111/j.1600-0838.2009.01088.x
Andersen LJ, Randers MB, Hansen PR, Hornstrup T, Schmidt JF, Dvorak J, Søgaard P, Krustrup P, Bangsbo J (2014) Structural and functional cardiac adaptations to 6 months of football training in untrained hypertensive men. Scand J Med Sci Sport 24:27–35. https://doi.org/10.1111/sms.12237
Appelman Y, van Rijn BB, ten Haaf ME, Boersma E, Peters SAE (2014) Sex differences in cardiovascular risk factors and disease prevention. Atherosclerosis 241:211–218. https://doi.org/10.1016/j.atherosclerosis.2015.01.027
Arbab-Zadeh A, Perhonen M, Howden E, Peshock RM, Zhang R, Adams-Huet B, Haykowsky MJ, Levine BD (2014) Cardiac remodeling in response to 1 year of intensive endurance training. Circulation 130:2152–2161. https://doi.org/10.1161/CIRCULATIONAHA.114.010775
Arnett DK, Blumenthal RS, Albert MA, Buroker AB, Goldberger ZD, Hahn EJ, Himmelfarb CD, Khera A, Lloyd-Jones D, McEvoy JW, Michos ED, Miedema MD, Muñoz D, Smith SC, Virani SS, Williams KA, Yeboah J, Ziaeian B (2019) 2019 ACC/AHA guideline on the primary prevention of cardiovascular disease: executive summary: a Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J Am Coll Cardiol 74:1376–1414. https://doi.org/10.1016/j.jacc.2019.03.009
Cho L, Davis M, Elgendy I, Epps K, Lindley KJ, Mehta PK, Michos ED, Minissian M, Pepine C, Vaccarino V, Volgman AS (2020) Summary of updated recommendations for primary prevention of cardiovascular disease in women: JACC state-of-the-art review. J Am Coll Cardiol 75:2602–2618
Cnaan A, Laird NM, Slasor P (2005) Using the general linear mixed model to analyse unbalanced repeated measures and longitudinal data. Stat Med 16:2349–2380. https://doi.org/10.1002/0470023724.ch1c(i)
El Khoudary SR, Aggarwal B, Beckie TM, Hodis HN, Johnson AE, Langer RD, Limacher MC, Manson JE, Stefanick ML, Allison MA (2020) Menopause transition and cardiovascular disease risk: implications for timing of early prevention: a scientific statement from the American Heart Association. Circulation 142:E506–E532
Fujimoto N, Prasad A, Hastings JL, Arbab-Zadeh A, Bhella PS, Shibata S, Palmer D, Levine BD (2010) Cardiovascular effects of 1 year of progressive and vigorous exercise training in previously sedentary individuals older than 65 years of age. Circulation 122:1797–1805. https://doi.org/10.1161/CIRCULATIONAHA.110.973784
Hansen PR, Andersen LJ, Rebelo AN, Brito J, Hornstrup T, Schmidt JF, Jackman SR, Mota J, Rêgo C, Oliveira J, Seabra A, Krustrup P (2013) Cardiovascular effects of 3 months of football training in overweight children examined by comprehensive echocardiography: a pilot study. J Sports Sci 31:1432–1440. https://doi.org/10.1080/02640414.2013.792951
Harvey RE, Coffman KE, Miller VM (2015) Women-specific factors to consider in risk, diagnosis and treatment of cardiovascular disease. Womens Health 11:239–257
Iorga A, Cunningham CM, Moazeni S, Ruffenach G, Umar S, Eghbali M (2017) The protective role of estrogen and estrogen receptors in cardiovascular disease and the controversial use of estrogen therapy. Biol Sex Differ 8:33
Jagannathan R, Patel SA, Ali MK, Narayan KMV (2019) Global updates on cardiovascular disease mortality trends and attribution of traditional risk factors. Curr Diab Rep 19:1–12
Kannel WB, Hjortland MC, McNamara P, Gordon T (1976) Menopause and risk of cardiovascular disease. The Framingham Study. Ann Intern Med 85:447–452. https://doi.org/10.7326/0003-4819-85-4-447
Krustrup P, Hansen PR, Randers MB, Nybo L, Martone D, Andersen LJ, Bune LT, Junge A, Bangsbo J (2010) Beneficial effects of recreational football on the cardiovascular risk profile in untrained premenopausal women. Scand J Med Sci Sports 20(Suppl 1):40–49. https://doi.org/10.1111/j.1600-0838.2010.01110.x
Krustrup P, Helge EW, Hansen PR, Aagaard P, Hagman M, Randers MB, de Sousa M, Mohr M (2018) Effects of recreational football on women’s fitness and health: adaptations and mechanisms. Eur J Appl Physiol 118:11–32. https://doi.org/10.1007/s00421-017-3733-7
Kyhl K, von Huth S, Bojer A, Thomsen C, Engstrøm T, Vejlstrup N, Madsen PL (2021) Conductance artery stiffness impairs atrio-ventriculo-arterial coupling before manifestation of arterial hypertension or left ventricular hypertrophic remodelling. Sci Rep 11:14467. https://doi.org/10.1038/s41598-021-93614-w
Leitman M, Lysyansky P, Sidenko S, Shir V, Peleg E, Binenbaum M, Kaluski E, Krakover R, Vered Z (2004) Two-dimensional strain—a novel software for real-time quantitative echocardiographic assessment of myocardial function. J Am Soc Echocardiogr 17:1021–1029. https://doi.org/10.1016/j.echo.2004.06.019
Mahjoub H, Le Blanc OL, Paquette M, Imhoff S, Labrecque L, Drapeau A, Poirier P, Bédard É, Pibarot P, Brassard P (2019) Cardiac remodeling after six weeks of high-intensity interval training to exhaustion in endurance-trained men. Am J Physiol—Hear Circ Physiol 317:H685–H694. https://doi.org/10.1152/ajpheart.00196.2019
Maron BJ, Pelliccia A (2006) The heart of trained athletes: Cardiac remodeling and the risks of sports, including sudden death. Circulation 114:1633–1644
Meluzín J, Špinarová L, Bakala J, Toman J, Krejči J, Hude P, Kára T, Souček M (2001) Pulsed Doppler tissue imaging of the velocity of tricuspid annular systolic motion. A new, rapid, and non-invasive method of evaluating right ventricular systolic function. Eur Heart J 22:340–348. https://doi.org/10.1053/euhj.2000.2296
Milanović Z, Pantelić S, Čović N, Sporiš G, Krustrup P (2015) Is recreational soccer effective for improving VO2max? A systematic review and meta-analysis. Sport Med 45:1339–1353
Milanović Z, Pantelić S, Čović N, Sporiš G, Mohr M, Krustrup P (2019) Broad-spectrum physical fitness benefits of recreational football: a systematic review and meta-analysis. Br J Sports Med 53:926–939. https://doi.org/10.1136/bjsports-2017-097885
Mohr M, Lindenskov A, Holm PM, Nielsen HP, Mortensen J, Weihe P, Krustrup P (2014) Football training improves cardiovascular health profile in sedentary, premenopausal hypertensive women. Scand J Med Sci Sport 24:36–42. https://doi.org/10.1111/sms.12278
Mohr M, Helge EW, Petersen LF, Lindenskov A, Weihe P, Mortensen J, Jørgensen NR, Krustrup P (2015) Effects of soccer vs swim training on bone formation in sedentary middle-aged women. Eur J Appl Physiol 115:2671–2679. https://doi.org/10.1007/s00421-015-3231-8
Mosca L, Grundy SM, Judelson D, King K, Limacher M, Oparil S, Pasternak R, Pearson TA, Redberg RF, Smith SC, Winston M, Zinberg S (1999) Guide to preventive cardiology for women. J Am Coll Cardiol 33:1751–1755
Nordsborg NB, Connolly L, Weihe P, Iuliano E, Krustrup P, Saltin B, Mohr M (2015) Oxidative capacity and glycogen content increase more in arm than leg muscle in sedentary women after intense training. J Appl Physiol 119:116–123. https://doi.org/10.1152/japplphysiol.00101.2015
Reisner SA, Lysyansky P, Agmon Y, Mutlak D, Lessick J, Friedman Z (2004) Global longitudinal strain: a novel index of left ventricular systolic function. J Am Soc Echocardiogr 17:630–633. https://doi.org/10.1016/j.echo.2004.02.011
Rosano GMC, Vitale C, Marazzi G, Volterrani M (2007) Menopause and cardiovascular disease: the evidence. Climacteric 10:19–24. https://doi.org/10.1080/13697130601114917
Sattar N, Greer IA (2002) Pregnancy complications and maternal cardiovascular risk: opportunities for intervention and screening? Br Med J 325:157–160
Schiller NB, Shah PM, Crawford M, DeMaria A, Devereux R, Feigenbaum H, Gutgesell H, Reichek N, Sahn D, Schnittger I, Silverman NH, Tajik AJ (1989) Recommendations for quantitation of the left ventricle by two-dimensional echocardiography. J Am Soc Echocardiogr 2:358–367. https://doi.org/10.1016/S0894-7317(89)80014-8
Sjúrðarson T, Bejder J, Andersen AB, Bonne T, Kyhl K, Róin T, Patursson P, Gregersen NO, Skoradal M-B, Schliemann M, Lindegaard M, Weihe P, Mohr M, Nordsborg NB (2022) Effect of angiotensin-converting enzyme inhibition on cardiovascular adaptation to exercise training. Physiol Rep 10:e15382. https://doi.org/10.14814/PHY2.15382
Townsend N, Kazakiewicz D, Lucy Wright F, Timmis A, Huculeci R, Torbica A, Gale CP, Achenbach S, Weidinger F, Vardas P (2022) Epidemiology of cardiovascular disease in Europe. Nat Rev Cardiol 19:133–143
Vitale C, Mendelsohn ME, Rosano GMC (2009) Gender differences in the cardiovascular effect of sex hormones. Nat Rev Cardiol 6:532–542. https://doi.org/10.1038/nrcardio.2009.105
Acknowledgements
The authors would like to express their appreciation for the outstanding efforts and positive attitude of the participants. In addition, they are extremely grateful for the technical assistance provided by study coordinator Annika Lindenskov and coaches Súsanna Holm, Pætur Mikal Holm, Heðin Joensen, Oluffa á Høvdanum, Pauli Øssursson Mohr, Heini Rasmussen and the late Jákup Mohr. Finally, the authors render thanks to medical assistance of Pál Weihe and Hans Peter Nielsen. The study was supported by a grant from the Faroese Research Council, as well as by the Faroese Confederation of Sports and Olympic Committee (Itrottarsamband Foroya), the Faroese Football Association (FSF) and the Danish Sports Confederation (Danmarks Idrætsforbund). In addition, financial support was obtained from Betri Bank.
Funding
Open access funding provided by University of Southern Denmark.
Author information
Authors and Affiliations
Contributions
MM, PK and NBN conceived and designed the research study. RK, LJA and MM performed the experiments. TS and KK analysed the data. TS, KK, LJA, NBN, PK and MM interpreted the results of the experiments. TS prepared the figures and tables. TS, KK and MM drafted the manuscript. All authors edited and revised the manuscript and approved the final version.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Additional information
Communicated by Westerterp/Westerblad.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Sjúrðarson, T., Kyhl, K., Nordsborg, N.B. et al. 15 weeks of soccer training increases left ventricular mass and improves indices of left ventricular diastolic function in previously sedentary, mildly hypertensive, middle-aged women. Eur J Appl Physiol 124, 1621–1629 (2024). https://doi.org/10.1007/s00421-023-05399-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-023-05399-7