Abstract
Purpose
To investigate whether performing resistance exercise in hypoxia augments physiological and perceptual responses, and if altering work-rate by performing repetitions to failure compared to sub-maximally increases the magnitude of these responses.
Methods
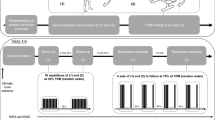
Twenty male university students (minimum of 2 year resistance training experience) completed four sessions, two in hypoxia (fraction of inspired oxygen [FiO2] = 0.13), and two in normoxia (FiO2 = 0.21). For each condition, session one comprised three sets to failure of shoulder press and bench press (high work-rate session), while session two involved the same volume load, distributed over six sets (low work-rate session). Muscle oxygenation (triceps brachii), surface electromyographic activity (anterior deltoid, pectoralis major, and triceps brachii), heart rate (HR), and arterial blood oxygen saturation were recorded. Blood lactate concentration ([Bla−]) was recorded pre-exercise and 2 min after each exercise. Muscle thickness was measured pre- and post-exercise via ultrasound.
Results
Muscle oxygenation values during sets and inter-set rest periods were lower in hypoxia vs normoxia (p = 0.001). Hypoxia caused greater [Bla−] during the shoulder press of failure sessions (p = 0.003) and both shoulder press (p = 0.048) and bench press (p = 0.005) of non-failure sessions. Hypoxia increased HR during non-failure sessions (p < 0.001). There was no effect of hypoxia on muscular swelling, surface electromyographic activity, perceived exertion, or number of repetitions performed.
Conclusions
Hypoxia augmented metabolite accumulation, but had no impact on any other physiological or perceptual response compared to the equivalent exercise in normoxia. Furthermore, the magnitude to which hypoxia increased the measured physiological responses was not influenced by sessional work-rate.




Similar content being viewed by others
Abbreviations
- AOP:
-
Arterial occlusion pressure
- BFR:
-
Blood flow restriction
- [BLa−]:
-
Blood lactate concentration
- EMG:
-
Electromyography
- ESSA:
-
Exercise and Sport Science Australia
- FiO2 :
-
Fraction of inspired oxygen
- HR:
-
Heart rate
- iEMG:
-
Integrated electromyography
- NIRS:
-
Near-infrared spectroscopy
- RM:
-
Repetition max
- RPE:
-
Rating of perceived exertion
- RTH:
-
Resistance training in hypoxia
- SpO2 :
-
Arterial blood oxygen saturation
- sRPE:
-
Sessional rating of perceived exertion
- TSI:
-
Tissue saturation index
References
Allen DG, Lamb GD, Westerblad H (2008) Skeletal muscle fatigue: cellular mechanisms. Physiol Rev 88(1):287–332. https://doi.org/10.1152/physrev.00015.2007
Bird SP, Tarpenning KM, Marino FE (2005) Designing resistance training programmes to enhance muscular fitness. Sports Med 35(10):841–851
Borg G, Borg G, Hassmén P, Hassmen P, Lagerstrom M, Lagerström M (1987) Perceived exertion related to heart rate and blood lactate during arm and leg exercise. Eur J Appl Physiol 56(6):679–685. https://doi.org/10.1007/BF00424810
Britto FA, Gnimassou O, De Groote E, Balan E, Warnier G, Everard A, Cani PD, Deldicque L (2020) Acute environmental hypoxia potentiates satellite cell-dependent myogenesis in response to resistance exercise through the inflammation pathway in human. FASEB J 34(1):1885–1900. https://doi.org/10.1096/fj.201902244R
Cairns SP (2006) Lactic acid and exercise performance: culprit or friend? Sports Med 36(4):279–291. https://doi.org/10.2165/00007256-200636040-00001
Fry CS, Glynn EL, Drummond MJ, Timmerman KL, Fujita S, Abe T, Dhanani S, Volpi E, Rasmussen BB (2010) Blood flow restriction exercise stimulates mTORC1 signaling and muscle protein synthesis in older men. J Appl Physiol 108(5):1199–1209. https://doi.org/10.1152/japplphysiol.01266.2009
Hiscock DJ, Dawson B, Peeling P (2015) Perceived exertion responses to changing resistance training programming variables. J Strength Cond Res 29(6):1564–1569. https://doi.org/10.1519/JSC.0000000000000775
Ho J-Y, Kuo T-Y, Liu K-L, Dong X-Y, Tung K (2014) Combining normobaric hypoxia with short-term resistance training has no additive beneficial effect on muscular performance and body composition. J Strength Cond Res 28(4):935–941. https://doi.org/10.1519/JSC.0000000000000289
Jenkins NDM, Housh TJ, Bergstrom HC, Cochrane KC, Hill EC, Smith CM, Johnson GO, Schmidt RJ, Cramer JT (2015) Muscle activation during three sets to failure at 80 vs. 30% 1RM resistance exercise. Eur J Appl Physiol 115(11):2335–2347. https://doi.org/10.1007/s00421-015-3214-9
Kon M, Ikeda T, Homma T, Akimoto T, Suzuki Y, Kawahara T (2010) Effects of acute hypoxia on metabolic and hormonal responses to resistance exercise. Med Sci Sports Exerc 42(7):1279–1285. https://doi.org/10.1249/MSS.0b013e3181ce61a5
Kon M, Ikeda T, Homma T, Suzuki Y (2012) Effects of low-intensity resistance exercise under acute systemic hypoxia on hormonal responses. J Strength Cond Res 26(3):611–617. https://doi.org/10.1519/JSC.0b013e3182281c69
Krustrup P, Mohr M, Steensberg A, Bencke J, Kjær M, Bangsbo J (2006) Muscle and blood metabolites during a soccer game: implications for sprint performance. Med Sci Sports Exerc 38(6):1165–1174
Li Z (2015) Three dimensional image analysis on movement speed biomechanics based on Myoresearch XP. In: 2015 international conference on automation, mechanical control and computational engineering. Atlantis Press
Lockhart C, Scott BR, Thoseby B, Dascombe BJ (2018) Acute effects of interset rest duration on physiological and perceptual responses to resistance exercise in hypoxia. J Strength Cond Res. https://doi.org/10.1519/JSC.0000000000002755
Loenneke JP, Fahs CA, Rossow LM, Abe T, Bemben MG (2012a) The anabolic benefits of venous blood flow restriction training may be induced by muscle cell swelling. Med Hypotheses 78(1):151–154. https://doi.org/10.1016/j.mehy.2011.10.014
Loenneke JP, Fahs CA, Thiebaud RS, Rossow LM, Abe T, Ye X, Kim D, Bemben MG (2012b) The acute muscle swelling effects of blood flow restriction. Acta Physiol Hung 99(4):400–410. https://doi.org/10.1556/APhysiol.99.2012.4.4
Marston KJ, Peiffer JJ, Newton MJ, Scott BR (2017) A comparison of traditional and novel metrics to quantify resistance training. Sci Rep 7:1. https://doi.org/10.1038/s41598-017-05953-2
McLean BD, Coutts AJ, Kelly V, McGuigan MR, Cormack SJ (2010) Neuromuscular, endocrine, and perceptual fatigue responses during different length between-match microcycles in professional rugby league players. Int J Sports Physiol Perform 5(3):367–383. https://doi.org/10.1123/ijspp.5.3.367
Nishimura A, Sugita M, Kato K, Fukuda A, Sudo A, Uchida A (2010) Hypoxia increases muscle hypertrophy induced by resistance training. Int J Sports Physiol Perform 5(4):497–508
Ramos-Campo DJ, Rubio-Arias JA, Dufour S, Chung L, Ávila-Gandía V, Alcaraz PE (2017) Biochemical responses and physical performance during high-intensity resistance circuit training in hypoxia and normoxia. Eur J Appl Physiol 117(4):809–818. https://doi.org/10.1007/s00421-017-3571-7
Ramos-Campo DJ, Scott BR, Alcaraz PE, Rubio-Arias JA (2018a) The efficacy of resistance training in hypoxia to enhance strength and muscle growth: a systematic review and meta-analysis. Eur J Sport Sci 18(1):92–103. https://doi.org/10.1080/17461391.2017.1388850
Ramos-Campo DJ, Martínez-Guardado I, Olcina G, Marín-Pagán C, Martínez-Noguera FJ, Carlos-Vivas J, Alcaraz PE, Rubio JÁ (2018b) Effect of high-intensity resistance circuit-based training in hypoxia on aerobic performance and repeat sprint ability. Scand J Med Sci Sports 28(10):2135–2143. https://doi.org/10.1111/sms.13223
Reynolds JM, Gordon TJ, Robergs RA (2006) Prediction of one repetition maximum strength from multiple repetition maximum testing and anthropometry. J Strength Cond Res 20(3):584–592. https://doi.org/10.1519/00124278-200608000-00020
Schoenfeld BJ (2013) Potential mechanisms for a role of metabolic stress in hypertrophic adaptations to resistance training. Sports Med 43(3):179–194. https://doi.org/10.1007/s40279-013-0017-1
Scott BR, Slattery KM, Dascombe BJ (2014a) Intermittent hypoxic resistance training: does it provide added benefit? Front Physiol 5:397. https://doi.org/10.3389/fphys.2014.00397
Scott BR, Slattery KM, Sculley DV, Dascombe BJ (2014b) Hypoxia and resistance exercise: a comparison of localized and systemic methods. Sports Med 44(8):1037–1054. https://doi.org/10.1007/s40279-014-0177-7
Scott BR, Slattery KM, Sculley DV, Lockie RG, Dascombe BJ (2014c) Reliability of telemetric electromyography and near-infrared spectroscopy during high-intensity resistance exercise. J Electromyogr Kinesiol 24(5):722–730. https://doi.org/10.1016/j.jelekin.2014.07.008
Scott BR, Slattery KM, Dascombe BJ (2015) Intermittent hypoxic resistance training: is metabolic stress the key moderator? Med Hypotheses 84(2):145–149. https://doi.org/10.1016/j.mehy.2014.12.001
Scott BR, Goods PSR, Slattery KM (2016) High-intensity exercise in hypoxia: is increased reliance on anaerobic metabolism important? Front Physiol. https://doi.org/10.3389/fphys.2016.00637
Scott BR, Slattery KM, Sculley DV, Lockhart C, Dascombe BJ (2017) Acute physiological responses to moderate-load resistance exercise in hypoxia. J Strength Cond Res 31(7):1973–1981. https://doi.org/10.1519/JSC.0000000000001649
Wheatley CM, Snyder EM, Johnson BD, Olson TP (2014) Sex differences in cardiovascular function during submaximal exercise in humans. Springerplus 3(1):445
Yasuda T, Fujita S, Ogasawara R, Sato Y, Abe T (2010) Effects of low-intensity bench press training with restricted arm muscle blood flow on chest muscle hypertrophy: a pilot study. Clin Physiol Funct Imaging 30(5):338–343. https://doi.org/10.1111/j.1475-097X.2010.00949.x
Zając A, Chalimoniuk M, Gołaś A, Lngfort J, Maszczyk A (2015) Central and peripheral fatigue during resistance exercise—a critical review. J Hum Kinet 49(1):159–169. https://doi.org/10.1515/hukin-2015-0118
Acknowledgements
The authors would like to thank the participants for volunteering their time to take part in the study.
Author information
Authors and Affiliations
Contributions
TPW, BRS, and OG conceived and designed research. TPW, AMJ, and KJM conducted experiments. TPW, BRS, OG, AMJ, and ARD analyzed data. All authors interpreted the results of experiments. TPW drafted manuscript and prepared figures/tables. All authors edited and revised manuscript. All authors approved the final version of manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest, source of funding, or financial ties to disclose and no current or past relationship with companies or manufacturers who could benefit from the results of the present study.
Additional information
Communicated by Michael Lindinger.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Walden, T.P., Girard, O., Jonson, A.M. et al. Sessional work-rate does not affect the magnitude to which simulated hypoxia can augment acute physiological responses during resistance exercise. Eur J Appl Physiol 120, 2159–2169 (2020). https://doi.org/10.1007/s00421-020-04440-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-020-04440-3