Abstract
In silico methods and models in the pathology of the blood-brain barrier (BBB) or also called BBB "computational pathology", are based on using mathematical approaches together with complex, high-dimensional experimental data to evaluate and predict disease-related impacts on the CNS. These computational methods and tools have been designed to deal with BBB-linked neuropathology at the molecular, cellular, tissue, and organ levels. The molecular and cellular levels mainly include molecular docking and molecular dynamics simulations (atomistic and coarse-grain) of mutated or misfolded tight junction proteins, receptors, and various BBB transporters. The tissue and organ levels encompass the mechanistic and pharmacokinetic models as well as finite-element method and pathway analyses enriched with multiple sources of raw data (e.g., in vitro and in vivo, histopathological records, "-omics", and imaging data). Overall, this review discusses comprehensive computational techniques and strategies at different levels of complexity, providing new insights and future directions for diagnosis, treatment improvement, and a deeper understanding of BBB-related neuropathological events.
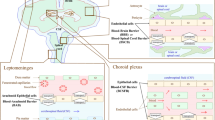
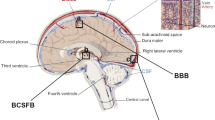
Graphical abstract


(The graphics program ChemDraw® was used to create the artwork)

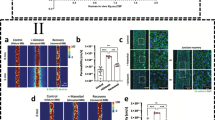
(Reprinted from Ref. Goliaei et al. (2015). Copyright 2015, ACS Chemical Neuroscience). (The graphics program ChemDraw® was used to create the artwork)

(Reprinted from Ref. Bearer et al. (2009). Copyright 2009, Cancer Research). (The graphics program ChemDraw® was used to create the artwork)
Similar content being viewed by others
References
Adhikari U, Goliaei A, Berkowitz ML (2016) Nanobubbles, cavitation, shock waves and traumatic brain injury. Phys Chem Chem Phys 18:32638–32652. https://doi.org/10.1039/c6cp06704b
Banerjee S, Khajanchi S, Chaudhuri S (2015) A mathematical model to elucidate brain tumor abrogation by immunotherapy with T11 target structure. PLoS One 10(5):e0123611
Banks WA (1999) Physiology and pathology of the blood-brain barrier: implications for microbial pathogenesis, drug delivery and neurodegenerative disorders. J Neurovirol 5:538–555
Banks WA (2012) Drug delivery to the brain in Alzheimer’s disease: consideration of the blood-brain barrier. Adv Drug Deliv Rev 64:629–639. https://doi.org/10.1016/j.addr.2011.12.005
Bearer EL et al (2009) Multiparameter computational modeling of tumor invasion. Cancer Res 69:4493–4501. https://doi.org/10.1158/0008-5472.CAN-08-3834
Brodland GW (1994) Finite element methods for developmental biology. Int Rev Cytol 150:95–118
Burek M, Arias-Loza PA, Roewer N, Forster CY (2010) Claudin-5 as a novel estrogen target in vascular endothelium. Arterioscler Thromb Vasc Biol 30:298–304. https://doi.org/10.1161/ATVBAHA.109.197582
Cramer SP, Larsson HBW (2014) Accurate determination of blood brain barrier permeability using dynamic contrast-enhanced T1-weighted MRI: a simulation and in vivo study on healthy subjects and multiple sclerosis patients. J Cerebr Blood Flow Met 34:1655–1665. https://doi.org/10.1038/jcbfm.2014.126
Dahl RH, Berg RMG (2015) A mathematical approach for assessing the transport of large neutral amino acids across the blood-brain barrier in man. Acta Neurobiol Exp 75:446–456
Del Razo MJ et al (2016) Computational and in vitro studies of blast-induced blood-brain barrier disruption siam. J Sci Comput 38:B347-B374. https://doi.org/10.1137/15M1010750
Dodacki A et al (2017) Expression and function of Abcg4 in the mouse blood-brain barrier: role in restricting the brain entry of amyloid-beta peptide. Sci Rep 7:13393. https://doi.org/10.1038/s41598-017-13750-0
Doege H, Schurmann A, Ohnimus H, Monser V, Holman GD, Joost HG (1998) Serine-294 and threonine-295 in the exofacial loop domain between helices 7 and 8 of glucose transporters (GLUT) are involved in the conformational alterations during the transport process. Biochem J 329:289–293 doi. https://doi.org/10.1042/Bj3290289
Dufour S, Atchia Y, Gad R, Ringuette D, Sigal I, Levi O (2013) Evaluation of laser speckle contrast imaging as an intrinsic method to monitor blood brain barrier integrity. Biomed Opt Express 4:1856–1875. https://doi.org/10.1364/Boe.4.001856
Forster C, Silwedel C, Golenhofen N, Burek M, Kietz S, Mankertz J, Drenckhahn D (2005) Occludin as direct target for glucocorticoid-induced improvement of blood-brain barrier properties in a murine in vitro system. J Physiol 565:475–486. https://doi.org/10.1113/jphysiol.2005.084038
Frieboes HB, Zheng X, Sun CH, Tromberg B, Gatenby R, Cristini V (2006) An integrated computational/experimental model of tumor invasion. Cancer Res 66:1597–1604. https://doi.org/10.1158/0008-5472.CAN-05-3166
Gefen A, Gefen N, Zhu Q, Raghupathi R, Margulies SS (2003) Age-dependent changes in material properties of the brain and braincase of the rat. J Neurotrauma 20:1163–1177. https://doi.org/10.1089/089771503770802853
Goiaei A, Adhikari U, Berkowitz ML (2015) Opening of the blood-brain barrier tight junction due to shock wave induced bubble collapse: a molecular dynamics simulation study. ACS Chem Neurosci 6:1296–1301. https://doi.org/10.1021/acschemneuro.5b00116
Hosseinkhah N, Goertz DE, Hynynen K (2015) Microbubbles and blood-brain barrier opening: a numerical study on acoustic emissions and wall stress predictions. IEEE Trans Bio-Med Eng 62:1293–1304. https://doi.org/10.1109/Tbme.2014.2385651
Irudayanathan FJ, Wang N, Wang X, Nangia S (2017) Architecture of the paracellular channels formed by claudins of the blood-brain barrier tight junctions. Ann N Y Acad Sci 1405:131–146. https://doi.org/10.1111/nyas.13378
Kleinschnitz C et al (2011) Glucocorticoid insensitivity at the hypoxic blood-brain barrier can be reversed by inhibition of the proteasome. Stroke 42:1081–1089. https://doi.org/10.1161/STROKEAHA.110.592238
Konrad M et al (2006) Mutations in the tight-junction gene claudin 19 (CLDN19) are associated with renal magnesium wasting, renal failure, and severe ocular involvement. Am J Hum Genet 79:949–957. https://doi.org/10.1086/508617
Lamy M, Baumgartner D, Willinger R, Yoganandan N, Stemper BD (2011) Study of mild traumatic brain injuries using experiments and finite element modeling. Ann Adv Automot Med 55:125–135
Lang GE, Vella D, Waters SL, Goriely A (2017) Mathematical modelling of blood-brain barrier failure and oedema. Math Med Biol 34:391–414. https://doi.org/10.1093/imammb/dqw009
Levchakov A, Linder-Ganz E, Raghupathi R, Margulies SS, Gefen A (2006) Computational studies of strain exposures in neonate and mature rat brains during closed head impact. J Neurotrauma 23:1570–1580. https://doi.org/10.1089/neu.2006.23.1570
Louis DN et al (2016) Computational pathology: a path ahead. Arch Pathol Lab Med 140:41–50. https://doi.org/10.5858/arpa.2015-0093-SA
Lozovaya N et al (2014) Selective suppression of excessive GluN2C expression rescues early epilepsy in a tuberous sclerosis murine model. Nature Commun 5:4563. https://doi.org/10.1038/ncomms5563
Lu GH, Kimura H (2009) A mathematical model of brain glucose homeostasis. Theor Biol Med Model 6 (Artn 26)
Macklin P, Lowengrub J (2007) Nonlinear simulation of the effect of microenvironment on tumor growth. J Theor Biol 245:677–704. https://doi.org/10.1016/j.jtbi.2006.12.004
Maikos JT, Qian Z, Metaxas D, Shreiber DI (2008) Finite element analysis of spinal cord injury in the rat. J Neurotraum 25:795–816. https://doi.org/10.1089/neu.2007.0423
Mang A et al (2012) Biophysical modeling of brain tumor progression: From unconditionally stable explicit time integration to an inverse problem with parabolic PDE constraints for model calibration. Med Phys 39:4444–4459. https://doi.org/10.1118/1.4722749
Miranda A, Cova T, Sousa J, Vitorino C, Pais A (2018) Computational modeling in glioblastoma: from the prediction of blood-brain barrier permeability to the simulation of tumor behavior. Future Med Chem 10:121–131. https://doi.org/10.4155/fmc-2017-0128
Mishra PK, Teale JM (2013) Changes in gene expression of pial vessels of the blood brain barrier during murine neurocysticercosis. Plos Neglect Trop D 7(3):e02099
Olsowski A, Monden I, Krause G, Keller K (2000) Cysteine scanning mutagenesis of helices 2 and 7 in GLUT1 identifies an exofacial cleft in both transmembrane segments. Biochemistry 39:2469–2474. https://doi.org/10.1021/Bi992160x
Panagiotopoulou O (2009) Finite element analysis (FEA): applying an engineering method to functional morphology in anthropology and human biology. Ann Hum Biol 36:609–623. https://doi.org/10.1080/03014460903019879
Papadogiorgaki M, Koliou P, Kotsiakis X, Zervakis ME (2013) Mathematical modelling of spatio-temporal glioma evolution. Theor Biol Med Model 10 (Artn 47)
Park M-S (2015) Molecular dynamics simulations of the human glucose transporter GLUT1. PLoS One 10(4):e0125361
Qosa H, Abuasal BS, Romero IA, Weksler B, Couraud PO, Keller JN, Kaddoumi A (2014) Differences in amyloid-beta clearance across mouse and human blood-brain barrier models Kinetic analysis mechanistic modeling. Neuropharmacology 79:668–678. https://doi.org/10.1016/j.neuropharm.2014.01.023
Rockne R, Alvord EC, Rockhill JK, Swanson KR (2009) A mathematical model for brain tumor response to radiation therapy. J Math Biol 58:561–578. https://doi.org/10.1007/s00285-008-0219-6
Saili KS et al (2017) Blood-brain barrier development: systems modeling and predictive toxicology. Birth Defects Res 109:1680–1710. https://doi.org/10.1002/bdr2.1180
Salvador E, Neuhaus W, Foerster C (2013) Stretch in brain microvascular endothelial cells (cEND) as an in vitro traumatic brain injury model of the blood brain barrier. J Vis Exp JoVE. https://doi.org/10.3791/50928
Shityakov S, Foerster C (2015) Systems biology approaches for discovering new glucocorticoid-mediated pathways at the blood-brain barrier. J Vasc Res 52:33–33
Shityakov S, Forster C (2014) In silico predictive model to determine vector-mediated transport properties for the blood-brain barrier choline transporter. Adv Appl Bioinf Chem AABC 7:23–36. https://doi.org/10.2147/AABC.S63749
Shityakov S, Neuhaus W, Dandekar T, Forster C (2013a) Analysing molecular polar surface descriptors to predict blood-brain barrier permeation. Int J Comput Biol Drug Design 6:146–156. https://doi.org/10.1504/IJCBDD.2013.052195
Shityakov S, Salvador E, Förster C (2013b) In silico, in vitro and in vivo methods to analyse drug permeation across the blood-brain barrier: A critical review. OA Anaesthetics 1(2):13
Shityakov S, Puskas I, Papai K, Salvador E, Roewer N, Forster C, Broscheit JA (2015a) Sevoflurane-sulfobutylether-beta-cyclodextrin complex: preparation, characterization, cellular toxicity, molecular modeling and blood-brain barrier transport studies. Molecules 20:10264–10279. https://doi.org/10.3390/molecules200610264
Shityakov S, Salvador E, Pastorin G, Forster C (2015b) Blood-brain barrier transport studies, aggregation, and molecular dynamics simulation of multiwalled carbon nanotube functionalized with fluorescein isothiocyanate. Int J Nanomed 10:1703–1713. https://doi.org/10.2147/IJN.S68429
Shityakov S, Salmas RE, Salvador E, Roewer N, Broscheit J, Forster C (2016) Evaluation of the potential toxicity of unmodified and modified cyclodextrins on murine blood-brain barrier endothelial cells. J Toxicol Sci 41:175–184. https://doi.org/10.2131/jts.41.175
Shityakov S, Roewer N, Broscheit JA, Förster CY (2017) In silico models for nanotoxicity evaluation and prediction at the blood-brain barrier level: a mini-review. Comp Tox 2:20–27
Suarez C, Maglietti F, Colonna M, Breitburd K, Marshall G (2012) Mathematical modeling of human glioma growth based on brain topological structures: study of two clinical cases. Plos One 7 (ARTN e39616)
Ward NL, Lamanna JC (2004) The neurovascular unit and its growth factors: coordinated response in the vascular and nervous systems. Neurol Res 26:870–883. https://doi.org/10.1179/016164104X3798
Wilson W, van Donkelaar CC, Huyghe JM (2005) A comparison between mechano-electrochemical and biphasic swelling theories for soft hydrated tissues. J Biomech Eng-T Asme 127:158–165. https://doi.org/10.1115/1.1835361
Yan Y-B, Qi W, Wu Z-X, Qiu T-X, Teo E-C, Lei W (2012) Finite element study of the mechanical response in spinal cord during the thoracolumbar burst fracture. Plos One 7:e41397. https://doi.org/10.1371/journal.pone.0041397
Zhu Y et al (2017) Design and evaluation of EphrinA1 mutants with cerebral protective effect. Sci Rep 7:1881. https://doi.org/10.1038/s41598-017-02091-7
Acknowledgements
The authors are also grateful to BMBF (Bundesministerium für Bildung und Forschung), European Commission, and German Research Foundation (DFG) for their support of this work by providing the LIPOTRANS 13N11803, NEUROBID Call HEALTH-2009-2.2.1-4, and DFG Fo315/4-1 grants to Carola Förster. This publication was also funded by the University of Würzburg in the funding program Open Access Publishing.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
Authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Shityakov, S., Förster, C.Y. Computational simulation and modeling of the blood–brain barrier pathology. Histochem Cell Biol 149, 451–459 (2018). https://doi.org/10.1007/s00418-018-1665-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00418-018-1665-x