Abstract
Purpose
To test the hypothesis that development of glaucomatous visual fields can be predicted several years earlier from prior visual field information.
Methods
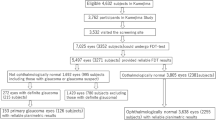
One-hundred and seven eyes with glaucomatous optic neuropathy (n = 47 eyes) or which were suspicious for glaucoma (n = 60) were prospectively enrolled in a longitudinal study. Visual fields were evaluated on an annual basis using standard automated perimetry (SAP), the original version of frequency doubling technology (FDT) perimetry, and a custom version of FDT that used the 24-2 stimulus pattern. All SAP fields were within normal limits at the initial visit. When the SAP glaucoma hemifield test was ‘outside normal limits’ or the pattern standard deviation probability was worse than the lower 5th percentile or more than two clustered locations at the p < 0.05 level were present on the pattern deviation probability plot, an eye was defined as being abnormal. We used a classification tree analysis to predict which eyes would convert, using only baseline test results.
Results
Classification trees that were constructed using only baseline data had excellent specificity (near 100%) but worse sensitivity (25–50%) for predicting which eyes would convert during follow-up.
Conclusions
Predictive information is present in visual field results, even when they are still within normal limits.



Similar content being viewed by others
References
Quigley HA, Dunkelberger GR, Green WR (1989) Retinal ganglion cell atrophy correlated with automated perimetry in human eyes with glaucoma. Am J Ophthalmol 107(5):453–464
Harwerth RS, Carter-Dawson L, Shen F, Smith EL 3rd, Crawford ML (1999) Ganglion cell losses underlying visual field defects from experimental glaucoma. Invest Ophthalmol Vis Sci 40(10):2242–2250
Harwerth RS, Crawford ML, Frishman LJ, Viswanathan S, Smith EL 3rd, Carter-Dawson L (2002) Visual field defects and neural losses from experimental glaucoma. Prog Retin Eye Res 21(1):91–125, Review
Garway-Heath DF, Holder GE, Fitzke FW, Hitchings RA (2002) Relationship between electrophysiological, psychophysical, and anatomical measurements in glaucoma. Invest Ophthalmol Vis Sci 43(7):2213–2220
Swanson WH, Felius J, Pan F (2004) Perimetric defects and ganglion cell damage: interpreting linear relations using a two-stage neural model. Invest Ophthalmol Vis Sci 45(2):466–472
Kass MA, Heuer DK, Higginbotham EJ, Johnson CA, Keltner JL, Miller JP, Parrish RK 2nd, Wilson MR, Gordon MO (2002) The Ocular Hypertension Treatment Study: a randomized trial determines that topical ocular hypotensive medication delays or prevents the onset of primary open-angle glaucoma. Arch Ophthalmol 120(6):701–713, discussion 829–30
Heijl A, Leske MC, Bengtsson B, Hyman L, Bengtsson B, Hussein M, Early Manifest Glaucoma Trial Group (2002) Reduction of intraocular pressure and glaucoma progression: results from the Early Manifest Glaucoma Trial. Arch Ophthalmol 120(10):1268–1279
Sample PA, Weinreb RN (1992) Progressive color visual field loss in glaucoma. Invest Ophthalmol Vis Sci 33(6):2068–2071
Sample PA, Taylor JD, Martinez GA, Lusky M, Weinreb RN (1993) Short-wavelength color visual fields in glaucoma suspects at risk. Am J Ophthalmol 115(2):225–233
Johnson CA, Brandt JD, Khong AM, Adams AJ (1995) Short-wavelength automatedperimetry in low-, medium-, and high-risk ocular hypertensive eyes. Initial baseline results. Arch Ophthalmol 13(1):70–76
Sample PA (2000) Short-wavelength automated perimetry: it’s role in the clinic and for understanding ganglion cell function. Prog Retin Eye Res 19(4):369–383, Review
Sit AJ, Medeiros FA, Weinreb RN (2004) Short-wavelength automated perimetry can predict glaucomatous standard visual field loss by ten years. Semin Ophthalmol 19(3–4):122–124
Bengtsson B, Heijl A (2006) Diagnostic sensitivity of fast blue-yellow and standard automated perimetry in early glaucoma: a comparison between different test programs. Ophthalmology 113(7):1092–1097
Van der Schoot J, Reus NJ, Colen TP, Lemij HG (2010) The ability of short-wavelength automated perimetry to predict conversion to glaucoma. Ophthalmology 117:30–34
Havvas I, Papaconstantinou D, Moschos MM, Theodossiadis PG, Andreanos V, Ekatomatis P, Vergados Ik Andreanos D (2013) Comparison of SWAP and SAP on the point of glaucoma conversion. Clin Ophthalmol 7:1805–1810
Maddess T, Henry GH (1992) Performance of nonlinear visual units in ocular hypertension and glaucoma. Clin Vis Sci 7:371–383
Johnson CA, Samuels SJ (1997) Screening for glaucomatous visual field loss with frequency-doubling perimetry. Invest Ophthalmol Vis Sci 38:413–425
Anderson AJ, Johnson CA (2003) Frequency-doubling technology perimetry. Ophthalmol Clin N Am 16:213–225
White AJ, Sun H, Swanson WH, Lee BB (2002) An examination of physiological mechanisms underlying the frequency-doubling illusion. Invest Ophthalmol Vis Sci 43:3590–3599
Swanson WH, Sun H, Lee BB, Cao D (2011) Responses of primate retinal ganglion cells to perimetric stimuli. Invest Ophthalmol Vis Sci 52:764–771. doi:10.1167/iovs.10-6158
Zeppieri M, Demirel S, Kent K, Johnson CA (2008) Perceived spatial frequency of sinusoidal gratings. Optom Vis Sci 85:318–329. doi:10.1097/OPX0b013e31816be9td
Petruska D, Grivich MI, Sher A, Field GD, Gauthier JL, Greschner M, Shlens J, Chichilnisky EJ, Litke AM (2007) Identification and characterization of a Y-like primate retinal ganglion cell. J Neurosci 27:11019–11027
Crook JD, Peterson BB, Packer OS, Robinson FR, Troy JB, Dacey DM (2008) Y-cell receptive field and collicular projection of parasol ganglion cells in macaque monkey retina. J Neurosci 28:11277–11291
Crook JD, Peterson BB, Packer OS, Robinson FR, Gamlin PD, Troy JB, Dacey DM (2008) The smooth monostratified ganglion cell: Evidence for spatial diversity in the Y-cell pathway to the lateral geniculate nucleus and superior colliculus in the macaque monkey. J Neurosci 28:12654–12671
Rosli Y, Bedford SM, Maddess T (2009) Low-spatial-frequency channels and the spatial frequency doubling illusion. Invest Ophthalmol Vis Sci 50:1956–1963
Johnson CA, Cioffi GA, Van Buskirk EM (1999) Frequency doubling technology perimetry using a 24-2 stimulus presentation pattern. Optom Vis Sci 76:571–581
Lloyd MJ, Mansberger SL, Fortune BA, Nguyen H, Torres R, Demirel S, Gardiner SK, Johnson CA, Cioffi GA (2013) Features of optic disc progression in patients with ocular hypertension and early glaucoma. J Glaucoma 22:343–348. doi:10.1097/IJG.0b013e31824c9251
Tyrrell RA, Owens DA (1988) A rapid technique to assess the resting states of the eyes and other threshold phenomena: the modified binary search (MOBS). Behav Res Methods Instrum Comput 20:137–141
Demirel S, Johnson CA (2001) Incidence and prevalence of short wavelength automated perimetry deficits in ocular hypertensive patients. Am J Ophthalmol 131:709–715
Adams CW, Bullimore MA, Wall M, Fingeret M, Johnson CA (1999) Normal aging effects for frequency doubling technology perimetry. Optom Vis Sci 76:582–587
Bowd C, Zangwill LM, Berry CC et al (2001) Detecting early glaucoma by assessment of retinal nerve fiber layer thickness and visual function. Invest Ophthalmol Vis Sci 42:1993–2003
Johnson CA (2002) Recent developments in automated perimetry in glaucoma diagnosis and management. Curr Opin Ophthalmol 13:77–84
Ihaka R, Gentleman R (1996) R: a language for data analysis and graphics. J Comput Graph Stat 5:299–314
Breiman L, Friedman JH, Olshen RA, Stone CJ. (1984) Classification and regression trees. Wadsworth, Pacific Grove
Bland JM, Altman DG (1986) Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 1:307–310
Johnson CA, Cioffi GA, Liebmann JR, Sample PA, Zangwill L, Weinreb RN (2000) The relationship between structural and functional alterations in glaucoma: A review. Seminars in Ophthalmology 15:221–233
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
Welch Allyn provided financial support in the form of $ 36,000.00 funding. Welch Allyn had no role in the design or conduct of this research.
Conflict of interest
During the time of this research the third author (CAJ) received research support from Welch Allyn and was a consultant for Welch Allyn. The first author (GT) and the second author (SM) have no financial interest related to this study or manuscript.
Ethical approval
All procedures performed in this study were in accordance with the ethical standards of the Institutional Research Board and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The study was approved by the Legacy Health Systems Institutional Review Board in Portland, Oregon.
Informed consent
All participants in this study provided written informed consent prior to participating in this study, and received a copy of their consent form.
Rights and permissions
About this article
Cite this article
Takahashi, G., Demirel, S. & Johnson, C.A. Predicting conversion to glaucoma using standard automated perimetry and frequency doubling technology. Graefes Arch Clin Exp Ophthalmol 255, 797–803 (2017). https://doi.org/10.1007/s00417-016-3573-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-016-3573-x