Abstract
Background
To evaluate the demographic, clinical, and ocular features of patients with Behçet’s disease (BD) who had first symptom onset after 40 years of age and fulfilled the diagnostic criteria afterwards.
Methods
This retrospective study included 42 patients with initial BD symptom onset after 40 years of age who fulfilled the diagnostic criteria afterwards, according to the International Study Group for BD. Patients were divided into two groups based on the presence of ocular involvement: group 1 had uveitis and group 2 did not have uveitis. The ocular characteristics of patients in group 1 were further examined according to age groups. Group 1A included patients between 40–50 years of age, and group 1B included patients older than 50 years of age. Clinical and demographic features of uveitic and non-uveitic patients were compared. Ocular manifestations, treatment protocols, and ocular complications in uveitic patients were noted. The ocular characteristics of group 1A and group 1B were further evaluated.
Results
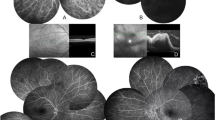
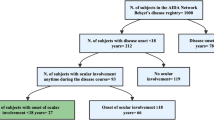
Twenty-six patients (61.9%) had uveitis (group 1) and 16 (39.1%) had no uveitis (group 2). There was no significant difference between groups according to sex, age at initial admission, age at the time of initial symptom of BD, and period between initial symptom and the diagnosis of BD. The most frequent initial manifestation was oral ulcer in both groups. No statistical difference between the groups was detected with regard to the mean age of onset of each symptom. Anterior uveitis (73.1%) was the most frequent type of uveitis followed by panuveitis (19.2%) and sclerouveitis (7.7%). Uveitis was bilateral in 80.8% of patients. The incidence of anterior uveitis was higher in group 1B than in group 1A (P = 0.023). Cataract was the most common ocular complication, followed by macular edema sequelae, glaucoma, optic disc paleness, and branch retinal vein occlusion.
Conclusion
Late-onset BD usually affects both genders equally, and the prognosis of ocular involvement is usually good. The incidence of panuveitis decreases as age increases, while the incidence of anterior uveitis increases. Ocular involvement is usually bilateral and there is no correlation between gender and uveitis type.
Similar content being viewed by others
References
Schirmer M, Calamia KT, Direskeneli H (2001) Ninth International Conference on Behçet’s disease, Seoul, Korea, May 27–29, 2000. J Rheumatol 28:636–639
Mochizuki M, Akduman L, Nussenblatt RB (1996) Behçet’s disease. In: Pepose JS, Holland GN, Wilhelmus KR (eds) Ocular infection and immunity. Mosby, St Louis, pp 663–675
Matsuo T, Itami M, Nakagawa H (2002) The incidence and pathology of conjunctival ulceration in Behçet’s syndrome. Br J Ophthalmol 86:140–143
Nussenblatt RB, Whitcup SM, Palestine AG (1996) Behçet’s disease. In: Nussenblatt RB, Whitcup SM, Palestine AG (eds) Uveitis: fundamentals and clinical practice. Mosby, St Louis, pp 334–353
Colvard DM, Robertson DM, O’Duffy JD (1977) The ocular manifestations of Behçet’s disease. Arch Ophthalmol 95:1813–1817
Zamir E, Bodaghi B, Tugal-Tutkun I, See RF, Charlotte F, Wang RC, Wechsler B, LeHoang P, Anteby I, Rao NA (2003) Conjunctival ulcers in Behçet’s disease. Ophthalmology 110:1137–1141
Atmaca LS (1989) Fundus changes associated with Behçet’s disease. Graefes Arch Clin Exp Ophthalmol 227:340–344
Yazici H, Tuzun Y, Pazarli H, Yurdakul S, Ozyazgan Y, Ozdoğan H, Serdaroğlu S, Ersanli M, Ulkü BY, Müftüoğlu AU (1984) Influence of age of onset and patient’s sex on the prevalence and severity of manifestations of Behçet’s syndrome. Ann Rheum Dis 43:783–789
Bardak Y (1999) Effects of age and sex on Behçet’s disease [letter]. J Rheumatol 26:1008–1009
Fujikawa S, Suemitsu T (1997) Behcet’s disease in children: a nationwide retrospective survey in Japan. Acta Paediatr Jpn 39:285–289
Sarıca R, Azizlerli G, Kose A, Dişçi R, Ovül C, Kural Z (1996) Juvenile Behcet’s disease among 1784 Turkish Behcet’s patients. Int J Dermatol 35:109–111
Krause I, Uziel Y, Guedj D, Mukamel M, Harel L, Molad Y, Weinberger A (1999) Childhood Behçet’s disease: clinical features and comparison with adult-onset disease. Rheumatology (Oxford) 38:457–462
Sungur GK, Hazirolan D, Yalvac I, Ozer PA, Yuksel D, Vural ET, Duman S (2009) Clinical and demographic evaluation of Behçet disease among different paediatric age groups. Br J Ophthalmol 93(1):83–87
International Study Group for Behçet’s Disease (1990) Evaluation of diagnostic (‘classification’) criteria in Behçet’s disease: toward internationally agreed criteria. Lancet 335:1078–1080
Tugal-Tutkun I, Onal S, Altan-Yaycioglu R, Huseyin Altunbas H, Urgancioglu M (2004) Uveitis in Behçet disease: an analysis of 880 patients. Am J Ophthalmol 138:373–380
Saricaoglu H, Karadogan SK, Bayazit N, Yucel A, Dilek K, Tunali S (2006) Clinical features of late-onset Behçet’s disease: report of nine cases. Int J Dermatol 45:1284–1287
Saricaoglu H, Karadogan SK, Bayazit N, Yucel A, Dilek K, Tunali S (2008) Late-onset Behçet’s disease does not correlate with indolent clinical course: report of seven Taiwanese patients. J Eur Acad Dermatol Venereol 2:596–600
Evereklioglu C (2005) Current concepts in the etiology and the treatment of Behçet disease. Surv Ophthalmol 50:297
Demiroglu H, Barista I, Dundar S (1997) Risk factor assessment and prognosis of eye involvement in Behçet’s disease in Turkey. Ophthalmology 104:701–705
Ozdal PC, Ortaç S, Taşkintuna I, Firat E (2002) Posterior segment involvement in ocular Behçet’s disease. Eur J Ophthalmol 12:424–431
Author information
Authors and Affiliations
Corresponding author
Additional information
No financial relationship exists with any organisation that sponsored the research. The authors have full control of all primary data, and they agree to allow Graefe's Archive for Clinical and Experimental Ophthalmology to review their data upon request.
Funding/Support
None.
Financial disclosures
None.
Rights and permissions
About this article
Cite this article
Sungur, G., Hazirolan, D., Hekimoglu, E. et al. Late-onset Behçet’s disease: demographic, clinical, and ocular features. Graefes Arch Clin Exp Ophthalmol 248, 1325–1330 (2010). https://doi.org/10.1007/s00417-010-1399-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-010-1399-5