Abstract
Introduction
A third of frontotemporal dementia (FTD) is caused by an autosomal-dominant genetic mutation in one of three genes: microtubule-associated protein tau (MAPT), chromosome 9 open reading frame 72 (C9orf72) and progranulin (GRN). Prior studies of prodromal FTD have identified impaired executive function and social cognition early in the disease but few have studied naming in detail.
Methods
We investigated performance on the Boston Naming Test (BNT) in the GENetic Frontotemporal dementia Initiative cohort of 499 mutation carriers and 248 mutation-negative controls divided across three genetic groups: C9orf72, MAPT and GRN. Mutation carriers were further divided into 3 groups according to their global CDR plus NACC FTLD score: 0 (asymptomatic), 0.5 (prodromal) and 1 + (fully symptomatic). Groups were compared using a bootstrapped linear regression model, adjusting for age, sex, language and education. Finally, we identified neural correlates of anomia within carriers of each genetic group using a voxel-based morphometry analysis.
Results
All symptomatic groups performed worse on the BNT than controls with the MAPT symptomatic group scoring the worst. Furthermore, MAPT asymptomatic and prodromal groups performed significantly worse than controls. Correlates of anomia in MAPT mutation carriers included bilateral anterior temporal lobe regions and the anterior insula. Similar bilateral anterior temporal lobe involvement was seen in C9orf72 mutation carriers as well as more widespread left frontal atrophy. In GRN mutation carriers, neural correlates were limited to the left hemisphere, and involved frontal, temporal, insula and striatal regions.
Conclusion
This study suggests the development of early anomia in MAPT mutation carriers, likely to be associated with impaired semantic knowledge. Clinical trials focused on the prodromal period within individuals with MAPT mutations should use language tasks, such as the BNT for patient stratification and as outcome measures.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Frontotemporal dementia (FTD) is a heterogeneous neurodegenerative disorder presenting with distinct changes in behaviour, language and motor function [1]. A third of cases are caused by an autosomal-dominant genetic mutation in one of three genes: microtubule-associated protein tau (MAPT), chromosome 9 open reading frame 72 (C9orf72) and progranulin (GRN) [2]. Although mutations in any of these genes can lead to impaired naming ability (anomia), MAPT mutation carriers tend to show the most pronounced deficit with previous studies showing that such difficulties can even be detected before symptom onset [3,4,5]. Importantly, whilst anomia is one of the key manifestations of people with the language variant of FTD [6], a similar pattern of naming deficits, albeit often less severe, has been found in the early stages of people presenting with both behavioural and motor symptoms [7,8,9], suggesting that impairment could potentially be seen in all of the phenotypes of genetic FTD.
Neuroanatomical correlates of naming deficits in FTD have implicated a widespread network of brain regions focused on the left hemisphere [10], which reflects the different components of the language pathway that contribute to naming [11]. In FTD due to C9orf72, GRN or MAPT mutations, there are both shared and distinct networks of atrophy across genetic groups, observable even at the pre-symptomatic stage [12]. This raised our hypothesis that the neuroanatomical correlates underlying naming differ according to the genetic aetiology of FTD.
The current study assessed naming deficits using the short 30-item version of the Boston Naming Test (BNT) [13] in a large cohort of C9orf72, MAPT and GRN mutation carriers. We expected all symptomatic mutation carriers to be impaired compared to mutation-negative controls on the BNT, but that MAPT mutation carriers would be the most impaired, potentially even in pre-symptomatic stages [4]. We also aimed to investigate the neural correlates of the BNT within each genetic group using voxel-based morphometric analyses of grey matter volume derived from structural Magnetic Resonance Imaging (MRI). We expected regions of the left-lateralised language network to be implicated in naming deficits across the groups, with potentially more focal anterior medial temporal structures in MAPT mutation carriers and a wider network in the C9orf72 and GRN groups.
Methods
Participants
Participants were recruited from the fifth data freeze of the GENFI study including sites in the UK, Canada, Sweden, Netherlands, Belgium, Spain, France, Portugal, Italy and Germany with eight different languages. Ethical approval was obtained for the study and all participants provided informed written consent. As well as the 30-item version of the Boston Naming Test in their preferred language [14], all participants underwent a standardised GENFI clinical assessment including a medical history, physical examination, the Mini-Mental State Examination (MMSE), and the Clinical Dementia Rating Scale (CDR) with National Alzheimer’s Coordinating Centre (NACC) FTD-specific modules (CDR plus NACC FTLD). The CDR plus NACC FTLD provides both a summed score (CDR plus NACC FTLD sum of boxes) and a global score, where 0 is asymptomatic, 0.5 is prodromal, 1 is mildly symptomatic, 2 is moderately symptomatic and 3 is severely symptomatic, with the last three scores also being combined to create a 1 + or ‘fully symptomatic’ group [15].
747 GENFI participants completed the BNT and were included in the present study: 248 mutation-negative carriers (controls), 212 C9orf72 expansion carriers, 201 GRN mutation carriers, and 86 MAPT mutation carriers. Mutation carriers were further divided into three groups according to their CDR plus NACC FTLD global score. Within the symptomatic mutation carrier groups, 101 met the diagnostic criteria for behavioural variant FTD (bvFTD: 54 C9orf72, 26 GRN and 21 MAPT), 20 primary progressive aphasia (PPA: 3 C9orf72, 16 GRN and 1 MAPT) and 14 amyotrophic lateral sclerosis with or without FTD (14 C9orf72). Demographic data for the groups are described in Table 1.
Magnetic Resonance Imaging (MRI)
Participants underwent volumetric T1-weighted magnetic resonance imaging (MRI) according to the harmonized GENFI imaging protocol on a 3T scanner, with only mutation carriers included in the neural correlate imaging analysis. From a total of 499 mutation carriers included in the naming study, 94 were excluded from the imaging analysis due to either imaging not being performed or not passing quality control. 405 scans were included: Siemens Trio 3T (n = 111), Siemens Skyra 3T (n = 64), Siemens Prisma 3T (n = 91), Philips Achieva 3T (n = 135) and GE 3T (n = 4).
BNT statistical analysis
Statistical analyses were performed using STATA version 16.0 (Texas, USA). The significance level was set at p < 0.05 across all comparisons. We compared group demographic data with linear regression except for sex which was compared using chi-square tests.
BNT scores in controls were assessed by calculating cumulative frequency (and therefore percentile scores), as well as investigating the effect of sex (Mann–Whitney U test), age (Spearman’s rank correlation), and education (Spearman’s rank correlation).
BNT scores in the mutation carrier groups were compared to each other and to controls using a bootstrapped linear mixed effects model (2000 repetitions) (due to non-normality). The model was adjusted for age, sex, education, language and family clustering with 95% bootstrapped confidence intervals. Post hoc pairwise comparisons were used to assess differences in group performance.
Structural brain imaging analysis
Voxel-based morphometric (VBM) analysis was performed using Statistical Parametric Mapping (SPM) 12 software, version 7219 (www.fil.ion.ucl.ac.uk/spm), running under Matlab R2014b (Mathworks, USA). The T1-weighted images were normalized and segmented into grey matter (GM), white matter (WM) and cerebrospinal fluid (CSF) probability maps, using standard procedures and the fast-diffeomorphic image registration algorithm (DARTEL) [16]. GM segmentations were affine-transformed into the Montreal Neurological Institute (MNI) space, modulated and smoothed using a Gaussian kernel with 6 mm full width, at half maximum, before analysis. Finally, a customised explicit brain mask was applied based on an optimised voxel threshold intensity criterion [17]. All segmentations were visually checked at each stage. Total intracranial volume was calculated using SPM [18].
The relationship of BNT score with GM density in the three mutation carrier groups was explored using a flexible factorial regression model. A main effect of BNT was included in the model and genetic group was included as an interaction. Age, sex, TIV and scanner type were included as covariates in the initial model with a further model additionally including disease severity as measured by the CDR plus NACC FTLD sum of boxes. All comparisons were adjusted for multiple comparisons by applying a Family-Wise Error correction set at p < 0.05. An uncorrected threshold of p < 0.001 was used if no results were found after correcting for multiple comparisons. An empirically determined cluster size threshold was also applied (23 for the initial model, and 62 for the further model).
Results
Demographic data
Differences between groups were seen in age, sex and years of education (Table 1). Compared with controls, all symptomatic groups (p < 0.001) as well as prodromal C9orf72 (p = 0.033) and GRN (p = 0.010) mutation carriers were significantly older, whilst asymptomatic MAPT mutation carriers were significantly younger than controls (p = 0.001). Within each genetic group, all symptomatic groups were significantly older than the prodromal groups (p < 0.003) who were significantly older than the asymptomatic groups (p < 0.033) apart from in MAPT mutations carriers where no difference in age was observed between prodromal and asymptomatic groups. There were significantly more males than females in the symptomatic C9orf72 (p = 0.001) and MAPT (p = 0.027) mutation carriers compared with the control group. With genetic groups, there were significantly more males than females in the symptomatic C9orf72 mutation carriers compared with the prodromal (p = 0.011) and asymptomatic (p = 0.003) groups. There were also more males than females in the symptomatic MAPT mutation carriers compared to the prodromal (p = 0.023) and asymptomatic (p = 0.030) groups. In terms of years of education, symptomatic GRN and C9orf72 mutation carriers had significantly fewer years of education than controls (p < 0.001, p < 0.05). Within genetic groups, symptomatic GRN mutation carriers had fewer years of education compared with the other two groups (p < 0.05) and symptomatic C9orf72 mutation carriers had significantly fewer years of education than the asymptomatic group (p < 0.05).
BNT scores in controls
Calculation of cumulative frequency in controls revealed a 5th percentile cut-off score at 24 (Supplementary Table S1). BNT scores did not correlate with age (rho = − 0.04, p = 0.53), and there was no significant effect of sex on BNT score (U = − 10,590, p = 0.72) (Supplementary Table S2). However, there was a weak positive correlation with education (rho = 0.28, p < 0.001).
BNT scores in genetic groups
All three fully symptomatic mutation carrier groups performed significantly worse than controls on the BNT (all p = < 0.001) (Fig. 1, Table 1, Supplementary Table S3). Asymptomatic and prodromal MAPT mutation carriers also performed significantly worse than controls (p = 0.012 and 0.011 respectively) but neither of the GRN or C9orf72 pre-symptomatic groups performed significantly worse than controls on the task.
Mean scores and standard error on the BNT for each group. Significantly worse performance compared with controls is shown with a star in the bar. Only differences between disease groups and controls, and within each genetic group are shown on the graph. Additional between genetic group differences were seen between MAPT 1 + and both GRN and C9orf72 1 + , between MAPT 0.5 and C9orf72 0.5, and between both MAPT 0 and C9orf72 0 and GRN 0
Within genetic groups, the fully symptomatic groups performed worse than both the prodromal and asymptomatic groups in MAPT, GRN and C9orf72 mutation carriers (all p = < 0.001). Additionally, the GRN prodromal group scored significantly worse than the asymptomatic group (p = 0.018).
Between genetic groups at the same disease stage, symptomatic MAPT mutation carriers performed significantly worse than symptomatic GRN and C9orf72 mutation carriers (p = 0.007 and 0.034 respectively). Prodromal MAPT mutation carriers performed significantly worse than prodromal C9orf72 mutation carriers (p = 0.020), whilst both asymptomatic MAPT and C9orf72 mutation carriers performed significantly worse than asymptomatic GRN carriers (p = 0.003, p = 0.048 respectively).
Neuroanatomical correlates of BNT score
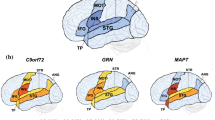
The initial VBM analysis model revealed partially overlapping neural correlates of naming in the three genetic groups (Figs. 2, 3, Supplementary Table S4). In MAPT mutation carriers, the anterior and medial temporal regions were implicated bilaterally as were the bilateral anterior insular cortices. In C9orf72 mutation carriers, the anterior temporal structures were also bilaterally involved. However, more widespread correlates of naming were seen in this group, particularly affecting the left hemisphere, in frontal (inferior, middle and superior) and insular cortices as well as the caudate. In GRN mutation carriers, correlates were only found within the left hemisphere, but were more distributed than the other two groups, affecting frontal (including premotor and supplementary motor cortices), anterior and lateral temporal, anterior parietal and striatal regions.
Overlapping neural correlates of naming across the three genetic groups. Comparative results are shown on a study-specific T1-weighted MRI template in MNI space and at p < 0.05 for Family-Wise error. The C9orf72 group are shown in green, the GRN group are shown in red and the MAPT group are shown in yellow
Adjusting for disease severity found very similar results in the additional VBM analysis model, although at an uncorrected p < 0.001 threshold, with no results found when correcting for multiple comparisons (Supplementary Fig. S1 and Supplementary Table S5): similar neural correlates were seen in each group although with more focal left anterior temporal lobe involvement for the C9orf72 mutation carriers in this analysis.
Discussion
In this study, we found that all genetic groups performed significantly worse on the BNT than controls when people were fully symptomatic, but only in the MAPT mutation group was naming ability impaired pre-symptomatically, being abnormal in both prodromal and asymptomatic mutation carriers. This highlights that naming performance is significantly impaired in people with genetic FTD, particularly in those with MAPT mutations, consistent with the previous literature [3,4,5, 11]. However, here we demonstrate very early naming change in the MAPT genetic group, and with overlapping but distinct neural correlates across the genetic groups: bilateral anterior temporal and anterior insula regions in MAPT mutation carriers, with similar temporal lobe involvement as well as more widespread left hemisphere atrophy in C9orf72 mutation carriers, and only distributed left hemisphere correlates in GRN mutation carriers.
The results in MAPT mutation carriers are consistent with previous work, where more severe deficits are seen on naming tasks cross-sectionally and the most decline over time is seen compared with both C9orf72 and GRN mutation carriers [4, 19]. We also found that both MAPT asymptomatic and prodromal groups performed significantly worse than controls. This finding has not been reported in the literature but is in keeping with previous work showing that MAPT mutation carriers have naming deficits before a formal diagnosis of FTD [4, 20]. Our study provides further evidence for subtle cognitive changes at a pre-symptomatic stage. Clinical trials for MAPT mutation carriers should consider using naming tasks such as the BNT as a marker for patient selection and outcome measure.
In MAPT mutation carriers, focal atrophy within the bilateral anterior and medial temporal lobes was associated with BNT score. The anterior temporal lobe has often been associated with semantic memory, particularly in studies which show that this region is specifically atrophied and hypometabolic in people with the semantic variant of PPA compared with those with Alzheimer’s disease [21]. Symptomatic and late pre-symptomatic MAPT mutation carriers are significantly impaired compared to controls on semantic memory tasks, with performance correlating strongly with bilateral temporal lobe volume [22]. Moreover, semantic deficits are suggested to occur with greater frequency in MAPT mutation carriers than in GRN or C9orf72 mutation carriers [3,4,5]. Thus, a core semantic deficit has been put forward as the defective mechanism underlying MAPT mutation carriers’ anomia, and our imaging results appear in line with such claims. Moreover, in view of the extremely symmetrical neuroanatomical correlates with the BNT, it appears that both verbal and visual semantics are equally likely to be related to MAPT mutation carriers’ poor BNT score.
In C9orf72 and GRN mutation carriers, reduced grey matter volume in the anterior temporal structures was also related to BNT performance. In the C9orf72 group, these extended to include bilateral hippocampi, whilst in the GRN group, these were left hemisphere only. In a recent study of a large cohort of patients, semantic deficits were also found in both C9orf72 and GRN mutation carriers [22]. Thus, semantic memory deficits are likely to underlie at least part of BNT performance. However, our results show that in both C9orf72 and GRN mutation carriers, neuroanatomical correlates of BNT score were more widespread throughout the left hemisphere. Indeed, in C9orf72 mutation carriers, left-predominant frontal regions and the left caudate were implicated, whilst in GRN mutation carriers, left frontal and striatal areas as well as the lateral temporal and parietal cortices were also involved. These findings are consistent with previous studies which have identified different regions to be related to anomia according to the likely linguistic subdomain affecting naming ability. Whilst anterior temporal regions have been found to correlate with naming deficits when semantic impairment is present, such as in the semantic variant of PPA [9, 10, 23], frontal lobe regions may be involved when there is impairment of word generation and motor aspects of speech and language, such as in the non-fluent variant of PPA. These include the inferior frontal lobe, opercular and anterior insula [24,25,26], as was seen here in both GRN and C9orf72 mutation carriers. In GRN mutation carriers alone, more lateral temporal and anterior parietal regions were involved. In the lateral temporal cortex, the superior temporal sulcus was particularly implicated, an area shown to enable audiovisual integration, leading to its implication in semantic processing [27], whilst in the anterior parietal region, classically affected in the logopenic variant of PPA, the angular gyrus was mainly involved, an area usually thought to be associated with semantic processing for both auditory and visual stimuli as well as being involved in concept retrieval and conceptual integration [28]. Finally, the C9orf72 genetic group showed bilateral frontal involvement, albeit left-lateralised. Previous studies show that executive processes can also be involved in naming, as can be seen in people with bvFTD [3, 9], and it may be that this is playing a role here.
A limitation of the present study is that the nature of incorrect answers on the BNT were not recorded. Error analysis could reveal the contributing processes, for example according to whether the participant gives the superordinate name, a wrong name or no name [29, 30]. Distinct error patterns can be seen as a function of left versus right and anterior versus posterior temporal lobe atrophy [9]. Our genetic groups showed left/right as well as anterior/posterior differences which could therefore lead to contrasting error patterns. Thus, future work could examine the nature of naming errors to explore whether such patterns differ across genetic groups and correspond to the different anatomical correlates identified. An alternative way to distinguish between the underlying cognitive processes could be to examine the inter-relationship with other linguistic measures. However, specific language tasks were limited in the GENFI neuropsychological battery.
The strength of this study’s results comes from the use of a large cohort of people with genetic FTD, which enabled gene-specific analyses, compared to control group of mutation-negative family members. We were therefore able to find pre-symptomatic naming deficits in MAPT mutation carriers and reveal different levels of performance in naming, between the three genetic groups. Different processes underlying naming in each genetic group are suggested by the diverse brain regions which appeared related to naming performance.
Conclusion
Overall, our findings are consistent with the hypothesis that large‐scale neural network degeneration underlies the impairment of naming ability in genetic FTD, but with different contributory regions in each genetic form. This study highlights the potential use of a simple naming task as an outcome measure for international clinical trials in pre-symptomatic MAPT mutation carriers, and in helping differential diagnosis and severity staging by understanding the sources of naming difficulty.
Availability of data and material
Some GENFI data are available on reasonable request through application to the GENFI Data Access Committee.
References
Snowden JS (2001) Distinct behavioural profiles in frontotemporal dementia and semantic dementia. J Neurol Neurosurg Psychiatry 70(3):323–332. https://doi.org/10.1136/jnnp.70.3.323
Rohrer JD et al (2009) The heritability and genetics of frontotemporal lobar degeneration. Neurology 73(18):1451–1456. https://doi.org/10.1212/WNL.0b013e3181bf997a
Hardy CJD et al (2016) The language profile of behavioral variant frontotemporal dementia. J Alzheimers Dis 50(2):359–371. https://doi.org/10.3233/JAD-150806
Rohrer JD et al (2015) C9orf72 expansions in frontotemporal dementia and amyotrophic lateral sclerosis. Lancet Neurol 14(3):291–301. https://doi.org/10.1016/S1474-4422(14)70233-9
Snowden JS et al (2015) Distinct clinical and pathological phenotypes in frontotemporal dementia associated with MAPT, PGRN and C9orf72 mutations. Amyotroph Lateral Scler Front Degener 16(7–8):497–505. https://doi.org/10.3109/21678421.2015.1074700
Rogalski EJ, Mesulam MM (2009) Clinical trajectories and biological features of primary progressive aphasia (PPA). Curr Alzheimer Res 6(4):331–336. https://doi.org/10.2174/156720509788929264
Ranasinghe KG et al (2016) Distinct subtypes of behavioral variant frontotemporal dementia based on patterns of network degeneration. JAMA Neurol 73(9):1078–1088. https://doi.org/10.1001/jamaneurol.2016.2016
Saxon JA et al (2017) Examining the language and behavioural profile in FTD and ALS-FTD. J Neurol Neurosurg Psychiatry 88(8):675–680. https://doi.org/10.1136/jnnp-2017-315667
Snowden JS et al (2019) Naming and conceptual understanding in frontotemporal dementia. Cortex 120:22–35. https://doi.org/10.1016/j.cortex.2019.04.027
McMillan C, Gee J, Moore P, Dennis K, DeVita C, Grossman M (2004) Confrontation naming and morphometric analyses of structural mri in frontotemporal dementia. Dement Geriatr Cogn Disord 17(4):320–323. https://doi.org/10.1159/000077163
Grossman M et al (2004) What’s in a name: voxel-based morphometric analyses of MRI and naming difficulty in Alzheimer’s disease, frontotemporal dementia and corticobasal degeneration. Brain 127(3):628–649. https://doi.org/10.1093/brain/awh075
Cash DM et al (2018) Patterns of gray matter atrophy in genetic frontotemporal dementia: results from the GENFI study. Neurobiol Aging 62:191–196. https://doi.org/10.1016/j.neurobiolaging.2017.10.008
Kaplan E, Goodglass H, Weintraub S (2001) The Boston Naming Test: Pro- Ed
Weintraub S et al (2009) The Alzheimer’s disease centers’ uniform data set (UDS): the neuropsychological test battery. Alzheimer Dis Assoc Disord 23(2):91–101. https://doi.org/10.1097/WAD.0b013e318191c7dd
Miyagawa T et al (2020) Utility of the global CDR® plus NACC FTLD rating and development of scoring rules: data from the ARTFL/LEFFTDS Consortium. Alzheimers Dement J Alzheimers Assoc 16(1):106–117. https://doi.org/10.1002/alz.12033
Ashburner J (2007) A fast diffeomorphic image registration algorithm. Neuroimage 38(1):95–113. https://doi.org/10.1016/j.neuroimage.2007.07.007
Ridgway GR, Omar R, Ourselin S, Hill DLG, Warren JD, Fox NC (2009) Issues with threshold masking in voxel-based morphometry of atrophied brains. Neuroimage 44(1):99–111. https://doi.org/10.1016/j.neuroimage.2008.08.045
Malone IB et al (2015) Accurate automatic estimation of total intracranial volume: a nuisance variable with less nuisance. Neuroimage 104:366–372. https://doi.org/10.1016/j.neuroimage.2014.09.034
Jiskoot LC et al (2018) Longitudinal cognitive biomarkers predicting symptom onset in presymptomatic frontotemporal dementia. J Neurol 265(6):1381–1392. https://doi.org/10.1007/s00415-018-8850-7
Cheran G et al (2019) Cognitive indicators of preclinical behavioral variant frontotemporal dementia in MAPT carriers. J Int Neuropsychol Soc 25(2):184–194. https://doi.org/10.1017/S1355617718001005
Nestor PJ, Fryer TD, Hodges JR (2006) Declarative memory impairments in Alzheimer’s disease and semantic dementia. Neuroimage 30(3):1010–1020. https://doi.org/10.1016/j.neuroimage.2005.10.008
Moore K et al (2020) A modified Camel and Cactus Test detects presymptomatic semantic impairment in genetic frontotemporal dementia within the GENFI cohort. Appl Neuropsychol Adult. https://doi.org/10.1080/23279095.2020.1716357
Mion M et al (2010) What the left and right anterior fusiform gyri tell us about semantic memory. Brain 133(11):3256–3268. https://doi.org/10.1093/brain/awq272
Gorno-Tempini ML et al (2004) Cognition and anatomy in three variants of primary progressive aphasia. Ann Neurol 55(3):335–346. https://doi.org/10.1002/ana.10825
Rohrer JD et al (2009) Patterns of cortical thinning in the language variants of frontotemporal lobar degeneration. Neurology 72(18):1562–1569. https://doi.org/10.1212/WNL.0b013e3181a4124e
Rogalski E et al (2011) Anatomy of language impairments in primary progressive aphasia. J Neurosci 31(9):3344–3350. https://doi.org/10.1523/JNEUROSCI.5544-10.2011
Wilson SM, Bautista A, McCarron A (2018) Convergence of spoken and written language processing in the superior temporal sulcus. Neuroimage 171:62–74. https://doi.org/10.1016/j.neuroimage.2017.12.068
Seghier ML (2013) The angular gyrus: multiple functions and multiple subdivisions. Neuroscientist 19(1):43–61. https://doi.org/10.1177/1073858412440596
Hodges JR, Patterson K (2007) Semantic dementia: a unique clinicopathological syndrome. Lancet Neurol 6(11):1004–1014. https://doi.org/10.1016/S1474-4422(07)70266-1
Savage SA, Ballard KJ, Piguet O, Hodges JR (2013) Bringing words back to mind—improving word production in semantic dementia. Cortex 49(7):1823–1832. https://doi.org/10.1016/j.cortex.2012.09.014
Acknowledgements
We would like to thank the research participants for their contribution to the study. Members of the GENFI Consortium are listed as follows. Aitana Sogorb Esteve: Department of Neurodegenerative Disease, Dementia Research Centre, UCL Queen Square Institute of Neurology, London, UK; UK Dementia Research Institute at University College London, UCL Queen Square Institute of Neurology, London, UK. Annabel Nelson: Department of Neurodegenerative Disease, Dementia Research Centre, UCL Queen Square Institute of Neurology, London, UK. Carolin Heller: Department of Neurodegenerative Disease, Dementia Research Centre, UCL Queen Square Institute of Neurology, London, UK. David Cash: Department of Neurodegenerative Disease, Dementia Research Centre, UCL Queen Square Institute of Neurology, London, UK. David L Thomas: Neuroimaging Analysis Centre, Department of Brain Repair and Rehabilitation, UCL Institute of Neurology, Queen Square, London, UK. Emily Todd: Department of Neurodegenerative Disease, Dementia Research Centre, UCL Queen Square Institute of Neurology, London, UK. Hanya Benotmane: UK Dementia Research Institute at University College London, UCL Queen Square Institute of Neurology, London, UK. Henrik Zetterberg: UK Dementia Research Institute at University College London, UCL Queen Square Institute of Neurology, London, UK; Department of Psychiatry and Neurochemistry, the Sahlgrenska Academy at the University of Gothenburg, Mölndal, Sweden. Imogen J Swift: Department of Neurodegenerative Disease, Dementia Research Centre, UCL Queen Square Institute of Neurology, London, UK; UK Dementia Research Institute at University College London, UCL Queen Square Institute of Neurology, London, UK. Jennifer Nicholas: Department of Medical Statistics, London School of Hygiene and Tropical Medicine, London, UK. Kiran Samra: Department of Neurodegenerative Disease, Dementia Research Centre, UCL Queen Square Institute of Neurology, London, UK. Rachelle Shafei: Department of Neurodegenerative Disease, Dementia Research Centre, UCL Queen Square Institute of Neurology, London, UK. Carolyn Timberlake: Department of Clinical Neurosciences, University of Cambridge, Cambridge, UK. Thomas Cope: Department of Clinical Neuroscience, University of Cambridge, Cambridge, UK. Timothy Rittman: Department of Clinical Neurosciences, University of Cambridge, Cambridge, UK. Alberto Benussi, Centre for Neurodegenerative Disorders: Department of Clinical and Experimental Sciences, University of Brescia, Brescia, Italy. Enrico Premi: Stroke Unit, ASST Brescia Hospital, Brescia, Italy. Roberto Gasparotti: Neuroradiology Unit, University of Brescia, Brescia, Italy. Silvana Archetti, Biotechnology Laboratory, Department of Diagnostics, ASST Brescia Hospital, Brescia, Italy. Stefano Gazzina: Neurology, ASST Brescia Hospital, Brescia, Italy. Valentina Cantoni, Centre for Neurodegenerative Disorders, Department of Clinical and Experimental Sciences, University of Brescia, Brescia, Italy. Andrea Arighi: Fondazione IRCCS Ca’ Granda Ospedale Maggiore Policlinico, Neurodegenerative Diseases Unit, Milan, Italy; University of Milan, Centro Dino Ferrari, Milan, Italy. Chiara Fenoglio: Fondazione IRCCS Ca’ Granda Ospedale Maggiore Policlinico, Neurodegenerative Diseases Unit, Milan, Italy; University of Milan, Centro Dino Ferrari, Milan, Italy. Elio Scarpini: Fondazione IRCCS Ca’ Granda Ospedale Maggiore Policlinico, Neurodegenerative Diseases Unit, Milan, Italy; University of Milan, Centro Dino Ferrari, Milan, Italy. Giorgio Fumagalli: Fondazione IRCCS Ca’ Granda Ospedale Maggiore Policlinico, Neurodegenerative Diseases Unit, Milan, Italy; University of Milan, Centro Dino Ferrari, Milan, Italy. Vittoria Borracci. Giacomina Rossi: Fondazione IRCCS Istituto Neurologico Carlo Besta, Milano, Italy. Giorgio Giaccone: Fondazione IRCCS Istituto Neurologico Carlo Besta, Milano, Italy. Giuseppe Di Fede: Fondazione IRCCS Istituto Neurologico Carlo Besta, Milano, Italy. Paola Caroppo: Fondazione IRCCS Istituto Neurologico Carlo Besta, Milano, Italy. Pietro Tiraboschi: Fondazione IRCCS Istituto Neurologico Carlo Besta, Milano, Italy. Sara Prioni: Fondazione IRCCS Istituto Neurologico Carlo Besta, Milano, Italy. Veronica Redaelli: Fondazione IRCCS Istituto Neurologico Carlo Besta, Milano, Italy. David Tang-Wai: The University Health Network, Krembil Research Institute, Toronto, Canada. Ekaterina Rogaeva: Tanz Centre for Research in Neurodegenerative Diseases, University of Toronto, Toronto, Canada. Miguel Castelo-Branco: Faculty of Medicine, University of Coimbra, Coimbra, Portugal. Morris Freedman: Baycrest Health Sciences, Rotman Research Institute, University of Toronto, Toronto, Canada. Ron Keren: The University Health Network, Toronto Rehabilitation Institute, Toronto, Canada. Sandra Black: Sunnybrook Health Sciences Centre, Sunnybrook Research Institute, University of Toronto, Toronto, Canada. Sara Mitchell: Sunnybrook Health Sciences Centre, Sunnybrook Research Institute, University of Toronto, Toronto, Canada. Christen Shoesmith: Department of Clinical Neurological Sciences, University of Western Ontario, London, Ontario, Canada. Robart Bartha: Department of Medical Biophysics, The University of Western Ontario, London, Ontario, Canada; Centre for Functional and Metabolic Mapping, Robarts Research Institute, The University of Western Ontario, London, Ontario, Canada. Rosa Rademakers, Center for Molecular Neurology, University of Antwerp. Jackie Poos: Department of Neurology, Erasmus Medical Center, Rotterdam, Netherlands. Janne M. Papma: Department of Neurology, Erasmus Medical Center, Rotterdam, Netherlands. Lucia Giannini: Department of Neurology, Erasmus Medical Center, Rotterdam, Netherlands. Rick van Minkelen: Department of Clinical Genetics, Erasmus Medical Center, Rotterdam, Netherlands. Yolande Pijnenburg, Amsterdam University Medical Centre, Amsterdam VUmc, Amsterdam, Netherlands. Benedetta Nacmias: Department of Neuroscience, Psychology, Drug Research and Child Health, University of Florence, Florence, Italy. Camilla Ferrari: Department of Neuroscience, Psychology, Drug Research and Child Health, University of Florence, Florence, Italy. Cristina Polito: Department of Biomedical, Experimental and Clinical Sciences “Mario Serio”, Nuclear Medicine Unit, University of Florence, Florence, Italy. Gemma Lombardi: Department of Neuroscience, Psychology, Drug Research and Child Health, University of Florence, Florence, Italy. Valentina Bessi: Department of Neuroscience, Psychology, Drug Research and Child Health, University of Florence, Florence, Italy. Michele Veldsman, Nuffield Department of Clinical Neurosciences, Medical Sciences Division, University of Oxford, Oxford, UK. Christin Andersson: Department of Clinical Neuroscience, Karolinska Institutet, Stockholm, Sweden. Hakan Thonberg, Center for Alzheimer Research, Division of Neurogeriatrics, Karolinska Institutet, Stockholm, Sweden. Linn Öijerstedt, Center for Alzheimer Research, Division of Neurogeriatrics: Department of Neurobiology, Care Sciences and Society, Bioclinicum, Karolinska Institutet, Solna, Sweden; Unit for Hereditary Dementias, Theme Aging, Karolinska University Hospital, Solna, Sweden. Vesna Jelic, Division of Clinical Geriatrics, Karolinska Institutet, Stockholm, Sweden. Paul Thompson, Division of Neuroscience and Experimental Psychology, Wolfson Molecular Imaging Centre, University of Manchester, Manchester, UK. Tobias Langheinrich, Division of Neuroscience and Experimental Psychology, Wolfson Molecular Imaging Centre, University of Manchester, Manchester, UK; Manchester Centre for Clinical Neurosciences: Department of Neurology, Salford Royal NHS Foundation Trust, Manchester, UK. Albert Lladó, Alzheimer’s disease and Other Cognitive Disorders Unit, Neurology Service, Hospital Clínic, Barcelona, Spain. Anna Antonell, Alzheimer’s disease and Other Cognitive Disorders Unit, Neurology Service, Hospital Clínic, Barcelona, SpainJaume Olives, Alzheimer’s disease and Other Cognitive Disorders Unit, Neurology Service, Hospital Clínic, Barcelona, SpainMircea Balasa, Alzheimer’s disease and Other Cognitive Disorders Unit, Neurology Service, Hospital Clínic, Barcelona, SpainNuria Bargalló, Imaging Diagnostic Center, Hospital Clínic, Barcelona, SpainSergi Borrego-Ecija, Alzheimer’s disease and Other Cognitive Disorders Unit, Neurology Service, Hospital Clínic, Barcelona, SpainAna Verdelho: Department of Neurosciences and Mental Health, Centro Hospitalar Lisboa Norte - Hospital de Santa Maria & Faculty of Medicine, University of Lisbon, Lisbon, PortugalCarolina Maruta, Laboratory of Language Research, Centro de Estudos Egas Moniz, Faculty of Medicine, University of Lisbon, Lisbon, PortugalCatarina B. Ferreira, Laboratory of Neurosciences, Faculty of Medicine, University of Lisbon, Lisbon, PortugalGabriel Miltenberger, Faculty of Medicine, University of Lisbon, Lisbon, PortugalFrederico Simões do Couto, Faculdade de Medicina, Universidade Católica Portuguesa Alazne Gabilondo, Cognitive Disorders Unit: Department of Neurology, Donostia University Hospital, San Sebastian, Gipuzkoa, Spain; Neuroscience Area, Biodonostia Health Research Insitute, San Sebastian, Gipuzkoa, SpainAna Gorostidi, Neuroscience Area, Biodonostia Health Research Insitute, San Sebastian, Gipuzkoa, SpainJorge Villanua, OSATEK, University of Donostia, San Sebastian, Gipuzkoa, SpainMarta Cañada, CITA Alzheimer, San Sebastian, Gipuzkoa, SpainMikel Tainta, Neuroscience Area, Biodonostia Health Research Insitute, San Sebastian, Gipuzkoa, SpainMiren Zulaica, Neuroscience Area, Biodonostia Health Research Insitute, San Sebastian, Gipuzkoa, SpainMyriam Barandiaran, Cognitive Disorders Unit: Department of Neurology, Donostia University Hospital, San Sebastian, Gipuzkoa, Spain; Neuroscience Area, Biodonostia Health Research Insitute, San Sebastian, Gipuzkoa, SpainPatricia Alves, Neuroscience Area, Biodonostia Health Research Insitute, San Sebastian, Gipuzkoa, Spain; Department of Educational Psychology and Psychobiology, Faculty of Education, International University of La Rioja, Logroño, SpainBenjamin Bender: Department of Diagnostic and Interventional Neuroradiology, University of Tübingen, Tübingen, GermanyCarlo Wilke: Department of Neurodegenerative Diseases, Hertie-Institute for Clinical Brain Research and Center of Neurology, University of Tübingen, Tübingen, Germany; Center for Neurodegenerative Diseases (DZNE), Tübingen, GermanyLisa Graf: Department of Neurodegenerative Diseases, Hertie-Institute for Clinical Brain Research and Center of Neurology, University of Tübingen, Tübingen, GermanyAnnick Vogels: Department of Human Genetics, KU Leuven, Leuven, BelgiumMathieu Vandenbulcke, Geriatric Psychiatry Service, University Hospitals Leuven, Belgium; Neuropsychiatry: Department of Neurosciences, KU Leuven, Leuven, BelgiumPhilip Van Damme, Neurology Service, University Hospitals Leuven, Belgium; Laboratory for Neurobiology, VIB-KU Leuven Centre for Brain Research, Leuven, BelgiumRose Bruffaerts: Department of Biomedical Sciences, University of Antwerp, Antwerp, Belgium; Biomedical Research Institute, Hasselt University, 3500 Hasselt, BelgiumKoen Poesen, Laboratory for Molecular Neurobiomarker Research, KU Leuven, Leuven, BelgiumPedro Rosa-Neto, Translational Neuroimaging Laboratory, McGill Centre for Studies in Aging, McGill University, Montreal, Québec, CanadaSerge Gauthier, Alzheimer Disease Research Unit, McGill Centre for Studies in Aging: Department of Neurology & Neurosurgery, McGill University, Montreal, Québec, CanadaAgnès Camuzat, Sorbonne Université, Paris Brain Institute – Institut du Cerveau – ICM, Inserm U1127, CNRS UMR 7225, AP-HP - Hôpital Pitié-Salpêtrière, Paris, FranceAlexis Brice, Sorbonne Université, Paris Brain Institute – Institut du Cerveau – ICM, Inserm U1127, CNRS UMR 7225, AP-HP - Hôpital Pitié-Salpêtrière, Paris, France; Reference Network for Rare Neurological Diseases (ERN-RND)Anne Bertrand, Sorbonne Université, Paris Brain Institute – Institut du Cerveau – ICM, Inserm U1127, CNRS UMR 7225, AP-HP - Hôpital Pitié-Salpêtrière, Paris, France; Inria, Aramis project-team, F-75013, Paris, France; Centre pour l'Acquisition et le Traitement des Images, Institut du Cerveau et la Moelle, Paris, FranceAurélie Funkiewiez, Centre de référence des démences rares ou précoces, IM2A, Département de Neurologie, AP-HP - Hôpital Pitié-Salpêtrière, Paris, France; Sorbonne Université, Paris Brain Institute – Institut du Cerveau – ICM, Inserm U1127, CNRS UMR 7225, AP-HP - Hôpital Pitié-Salpêtrière, Paris, FranceDaisy Rinaldi, Centre de référence des démences rares ou précoces, IM2A, Département de Neurologie, AP-HP - Hôpital Pitié-Salpêtrière, Paris, France; Sorbonne Université, Paris Brain Institute – Institut du Cerveau – ICM, Inserm U1127, CNRS UMR 7225, AP-HP - Hôpital Pitié-Salpêtrière, Paris, France; Département de Neurologie, AP-HP - Hôpital Pitié-Salpêtrière, Paris, FranceDario Saracino, Sorbonne Université, Paris Brain Institute – Institut du Cerveau – ICM, Inserm U1127, CNRS UMR 7225, AP-HP - Hôpital Pitié-Salpêtrière, Paris, France; Inria, Aramis project-team, F-75013, Paris, France; Centre de référence des démences rares ou précoces, IM2A, Département de Neurologie, AP-HP - Hôpital Pitié-Salpêtrière, Paris, FranceOlivier Colliot, Sorbonne Université, Paris Brain Institute – Institut du Cerveau – ICM, Inserm U1127, CNRS UMR 7225, AP-HP - Hôpital Pitié-Salpêtrière, Paris, France; Inria, Aramis project-team, F-75013, Paris, France; Centre pour l'Acquisition et le Traitement des Images, Institut du Cerveau et la Moelle, Paris, FranceSabrina Sayah, Sorbonne Université, Paris Brain Institute – Institut du Cerveau – ICM, Inserm U1127, CNRS UMR 7225, AP-HP - Hôpital Pitié-Salpêtrière, Paris, FranceCatharina Prix, Neurologische Klinik, Ludwig-Maximilians-Universität München, Munich, GermanyElisabeth Wlasich, Neurologische Klinik, Ludwig-Maximilians-Universität München, Munich, GermanyOlivia Wagemann, Sandra Loosli, Neurologische Klinik, Ludwig-Maximilians-Universität München, Munich, GermanySonja Schönecker, Neurologische Klinik, Ludwig-Maximilians-Universität München, Munich, GermanyTobias Hoegen, Neurologische Klinik, Ludwig-Maximilians-Universität München, Munich, GermanyJolina Lombardi: Department of Neurology, University of Ulm, UlmSarah Anderl-Straub: Department of Neurology, University of Ulm, Ulm, GermanyAdeline Rollin, CHU, CNR-MAJ, Labex Distalz, LiCEND Lille, FranceGregory Kuchcinski, Univ Lille, France; Inserm 1172, Lille, France; CHU, CNR-MAJ, Labex Distalz, LiCEND Lille, FranceMaxime Bertoux, Inserm 1172, Lille, France; CHU, CNR-MAJ, Labex Distalz, LiCEND Lille, FranceThibaud Lebouvier, Univ Lille, France; Inserm 1172, Lille, France; CHU, CNR-MAJ, Labex Distalz, LiCEND Lille, FranceVincent Deramecourt, Univ Lille, France; Inserm 1172, Lille, France; CHU, CNR-MAJ, Labex Distalz, LiCEND Lille, FranceBeatriz Santiago, Neurology Department, Centro Hospitalar e Universitario de Coimbra, Coimbra, PortugalDiana Duro, Faculty of Medicine, University of Coimbra, Coimbra, PortugalMaria João Leitão, Centre of Neurosciences and Cell Biology, Universidade de Coimbra, Coimbra, PortugalMaria Rosario Almeida, Faculty of Medicine, University of Coimbra, Coimbra, PortugalMiguel Tábuas-Pereira, Neurology Department, Centro Hospitalar e Universitario de Coimbra, Coimbra, PortugalSónia Afonso, Instituto Ciencias Nucleares Aplicadas a Saude, Universidade de Coimbra, Coimbra, Portugal. Annerose Engel, Clinic for Cog+zig, Germany. Maryna Polyakova: Department for Neurology, Max Planck Institute for Human Cognitive and Brain Sciences and Clinic for Cognitive Neurology, University Hospital Leipzig, Leipzig, Germany
Funding
The Dementia Research Centre is supported by Alzheimer's Research UK, Alzheimer's Society, Brain Research UK, and The Wolfson Foundation. This work was supported by the NIHR UCL/H Biomedical Research Centre, the Leonard Wolfson Experimental Neurology Centre (LWENC) Clinical Research Facility, and the UK Dementia Research Institute, which receives its funding from UK DRI Ltd, funded by the UK Medical Research Council, Alzheimer's Society and Alzheimer's Research UK. JDR is supported by the Miriam Marks Brain Research UK Senior Fellowship and has received funding from an MRC Clinician Scientist Fellowship (MR/M008525/1) and the NIHR Rare Disease Translational Research Collaboration (BRC149/NS/MH). This work was also supported by the MRC UK GENFI grant (MR/M023664/1), the Bluefield Project and the JPND GENFI-PROX grant (2019-02248). This research was supported by the NIHR Cambridge Biomedical Research Centre (BRC-1215-20014). The views expressed are those of the authors and not necessarily those of the NIHR or the Department of Health and Social Care. MB is supported by a Fellowship award from the Alzheimer’s Society, UK (AS-JF-19a-004-517). MB’s work is also supported by the UK Dementia Research Institute which receives its funding from DRI Ltd, funded by the UK Medical Research Council, Alzheimer’s Society and Alzheimer’s Research UK. RC/CG are supported by a Frontotemporal Dementia Research Studentships in Memory of David Blechner funded through The National Brain Appeal (RCN 290173). Several authors of this publication are members of the European Reference Network for Rare Neurological Diseases—Project ID No 739510. This work was funded by the Deutsche Forschungsgemeinschaft (DFG, German Research Foundation) under Germany’s Excellence Strategy within the framework of the Munich Cluster for Systems Neurology (EXC 2145 SyNergy—ID 390857198).
Author information
Authors and Affiliations
Consortia
Contributions
AB, JR and LR contributed to the study design, acquisition, analysis and interpretation of the data as well as drafting and revising the manuscript. All other authors contributed to the acquisition of data and study coordination as well as helping to critically review and revise the manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest. Johannes Levin reports speaker fees from Bayer Vital, Biogen and Roche, consulting fees from Axon Neuroscience and Biogen, author fees from Thieme medical publishers and W. Kohlhammer GmbH medical publishers, non-financial support from Abbvie and compensation for duty as part-time CMO from MODAG, outside the submitted work.
Ethical approval
Local ethics committees at each site provided ethical approval in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments.
Consent to participate
All participants provided informed written consent prior to their inclusion.
Consent for publication
Not required.
Additional information
List of Consortium Authors is mentioned in Acknowledgements (The Genetic FTD Initiative, GENFI).
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Bouzigues, A., Russell, L.L., Peakman, G. et al. Anomia is present pre-symptomatically in frontotemporal dementia due to MAPT mutations. J Neurol 269, 4322–4332 (2022). https://doi.org/10.1007/s00415-022-11068-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-022-11068-0