Abstract
Objective
The study aimed to assess the risk of cognitive impairment in patients with epilepsy, the impact of age of epilepsy onset on cognition and the temporal relationship of epilepsy onset and intellectual impairment.
Methods
This longitudinal study analyzed birth cohorts and followed-up children born 2005–2007 up to the age of ten using administrative healthcare data of about 8.9 million members insured by the statutory health insurance “BARMER” in Germany. We compared prevalence of cognitive impairment (ICD-code F7*) in children with epilepsy (ICD-code G40) to controls, and calculated relative risks by age groups at onset of epilepsy and assessed differences in relation to the temporal sequence of the diagnoses.
Results
Of the 142,563 pre-pubertal children included in the analysis, 2728 (1.9%) had an epilepsy diagnosis within the first 10 years of life. 17.4% (475/2728) of children with epilepsy had a diagnosis of cognitive impairment compared to 1.7% (2309/139835) in controls. The relative risk for cognitive impairment compared to age-matched controls was 10.5 (95% CI 9.6, 11.6) and was highest in epilepsy cases with seizure manifestation within the first 2 years of life compared to older children. The prevalence of cognitive impairment before epilepsy diagnosis was slightly increased compared to controls, while it was increased by a factor of nine in children diagnosed with cognitive impairment in the year of onset of epilepsy or afterwards.
Conclusions
Pre-pubertal children with epilepsy have a ten-fold higher risk for intellectual impairment compared to age-matched controls. This risk inversely correlates with the age of epilepsy manifestation. Cognitive impairment was diagnosed after epilepsy manifestation in the majority of patients.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Background
Mental health, developmental and behavioural problems are comorbidities present in some children with epilepsy [1]. These comorbidities might have a higher impact on impaired quality of life for both, patients and caregivers than seizure activity itself [2, 3]. Additionally, adolescents with epilepsy often feel more socially disadvantaged than patients with other, non-neurological chronic diseases [4]. Patients with childhood-onset epilepsies with cognitive problems have a higher rate of unemployment than childhood-onset epilepsy patients without cognitive problems in adulthood [5].
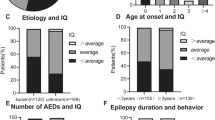
The causes of these epilepsy associated comorbidities are often difficult to dissect as many factors might contribute to impaired mental function [6]. First, epilepsy-related factors as age of seizure onset, seizure frequency and duration might have a significant impact on comorbidities suggesting higher prevalence in patients with earlier seizure onset, higher seizure frequency and longer epilepsy duration. Second, the cause of the underlying epilepsy syndrome impacts to cognitive performance: patients with idiopathic epilepsy syndromes show higher intelligence quotient (IQ) scores than patients with monogenetic epilepsies (i.e. caused by mutations in ion channels encoded by SCN1A) [7]. Some researchers even propose to call the latter epilepsy group ‘Developmental brain disorders with the comorbidity of epilepsy’ in order to pronounce the high impact of cognitive, developmental and behavioral disturbances in theses syndromes beside the burden of seizures [8]. Lastly, significant effects on cognitive performance and behavioral disturbances have been shown for many antiseizure medication (ASM) and commonly reveal cumulative effects when drugs are combined [9, 10].
There is plenty of data about cognitive impairment in children with epilepsy [6, 11, 12]. Most of these data, however, lack a control group of children without epilepsy and even fewer studies focus the pre-pubertal age. Follow-up of birth cohorts in healthcare data allows assessing the absolute risk for cognitive impairment in children with epilepsy and the relative risk compared to children without epilepsy. The longitudinal structure of these data facilitate addressing the assessment of the temporal relation of epilepsy and cognitive impairment.
The study aimed to assess the following questions: how much does epilepsy increase the risk for cognitive impairment for children of pre-pubertal age? Does this risk increment vary by age of onset of epilepsy? Is there a risk that cognitive impairment precedes epilepsy onset?
Methods
Data source
In Germany, there is obligatory statutory health insurance, which covers 90% of the population [13]. Persons with high income are exempt and may opt between none, private or statutory health insurance [14]. There are over 100 different statutory health insurance providers [15]. One of these is BARMER. In terms of the number of insured persons, BARMER is the second largest statutory health insurance in Germany. About 11% of the German population (8.9 million health insurance holders) is BARMER insured [16, 17]. BARMER insured slightly more children aged younger than 15 years than other statutory health insurances on average (13.74% vs 12.77%) [18].
Physicians or clinics claim the treatment fees from the health insurance provider and therefore collect several data, including the ICD codes (International Classification of Diseases) for the diagnoses related to the medical treatment and drug prescriptions. All medical diagnosis are coded in the German Modification of ICD-10 published by the World Health Organization [19]. The insurance thus collects information on physician contacts and diagnoses for each insured person. BARMER provides this data in pseudonymized form for scientific purposes. Data of the present study comprise insured persons from 2005 to 2019 and could, therefore, follow-up birth cohorts in a retrospective cohort study.
Study cohort
This analysis is based on data for children born in 2005–2007 with complete follow-up (= permanently BARMER insured until 2019 or until death). Patients with a diagnosis of epilepsy in the first 10 years of life defined the cases. Patients without a diagnosis of epilepsy in the first 10 years of life served as the control group. Outpatient and inpatient physician visits for epilepsy from birth through the age of ten (means until 2015 for the 2005 birth cohort, until 2016 for the 2006 birth cohort and 2017 for the 2007 birth cohort) and for case validation 2 years beyond were considered.
Case definition
We defined ‘pre-pubertal’ as from birth up to 10 years of age. The ICD code for epilepsy is G40*. All children not meeting the case definition were controls. The case definition used in our analysis was adapted from the recommendations by Reid et al. [20]. We proposed ‘2 physician claims or 1 hospitalization in 2 years coded’ (ICD G40) as the most accurate and ‘1 physician claim or 1 hospitalization or 1 ER visit in 2 years’ as the most sensitive algorithm. In contrast to the suggestion by Reid, we decided not to include G41 (status epilepticus) cases. R56.1 (febrile convulsions) was also not considered within the “epilepsy” group unless the concomitant code of G40 was documented as defined above.
Outpatient and inpatient physician visits for epilepsy from birth through the age of 10 (means until 2015 for the 2005 birth cohort, until 2016 for the 2006 birth cohort and 2017 for the 2007 birth cohort) and for case validation 2 years beyond, respectively, were considered. A confirmed diagnosis of epilepsy requires a diagnose of G40 anytime in the first 10 years of life ‘in at least two outpatient physician claims’ or ‘related to one hospitalization and at least one outpatient physician claim’ or ‘related to more than one hospitalization’ in the year of the first G40 diagnosis and two subsequent years.
Main outcomes
Beyond description of the pre-pubertal incidence rate of epilepsy, the study aimed to investigate the association between epilepsy and cognitive impairment. Cognitive impairment was defined by a diagnosis of ICD-code F7*. Cases with different F7* codes during the first 10 years of life or with code F78 or F79 only were summarized and labeled as “unspecific cognitive impairment”.
Statistical methods
The year of onset of epilepsy was defined as the year with the first G40 diagnosis.
Confidence intervals (CI) of 95% for incidence were calculated according to Agresti Coull [21, 22].
The prevalence of cognitive impairment in epilepsy cases and controls is displayed with 95% CI. Relative risk (RR) were calculated to compare case and control group. Differences between cases and controls were tested using chi-square statistics. The significance level for all analyses was set at 5%. We performed all analyses with SAS Enterprise guide 8.3 Update 2.
Data accessibility and ethics
This is an analysis on healthcare data, not owned by the authors. BARMER gives remote access to their data to scientists with an appropriate research question.
Informed consent is not necessary in retrospective data analysis of pseudonymized healthcare data. The ethics committee of the medical faculty of the Ludwig-Maximilians-University Munich gave ethical approval (Number 17-742 UE until 17-746 UE).
Results
Incidence of epilepsy in pre-pubertal children
We identified 142,563 children born in 2005–2007 with complete follow-up until 2019 or until death. 2728 (1.9%) had an epilepsy diagnosis within the first 10 years of life (Fig. 1). The incidence rate of pre-pubertal epilepsy was 191 [95% CI 185, 200] per 100,000 person years and the highest age-specific incidence of 314 [95% CI 286, 344] per 100,000 children was recorded at the age of one. The age-specific incidence subsequently decreased to 112 (95% CI 96, 131] per 100,000 by the age of eight (Table 1 and Fig. 2). There were slightly more male children in the case group (54%, n = 1484/2728) compared to the control group (51%, n = 71,826/139,835, p = 0.002).
Prevalence and the risk of cognitive impairment in children with epilepsy
Two thousand seven hundred and eighty-four (2.0%) children within the study cohort were identified as having cognitive impairment. Figure 3 summarizes the prevalence of different categories of cognitive impairment in 2728 cases with epilepsy and 139,835 control children and the relative risk for cognitive impairment. The prevalence of cognitive impairment was higher in children with epilepsy than in controls for all categories of severity (RR 10.5, 95% CI 9.6, 11.6). Overall, prevalence of cognitive impairment in the epilepsy group was 17.4% (475/2728), whereas it was 1.7% in the control group (2309/139,835). The incidence rate of cognitive impairment per each age year for both patients with epilepsy and controls is depicted in Table 2.
The risk of cognitive impairment in children with epilepsy compared to age-matched controls. The risk of cognitive impairment was increased by factor 10.5 in patients with epilepsy. Epilepsy patients revealed most likely not further specified (F78, 79) or mild (F70) cognitive impairment. The risk of profound cognitive impairment (F73) was almost increased by factor 50 compared to age-matched controls
The relative risk related to epilepsy increased by severity of cognitive impairment. While the relative risk for mild cognitive impairment in the epilepsy group was 9.4 [95% CI 7.8, 11.4], the RR for profound cognitive impairment was 47.4 [95% CI 27.5, 81.5] (Fig. 3). About half of the cognitive impairment diagnose was coded with ICD F78 or ICD F79 precluding information on the severity level. In the majority of patients with epilepsy, mild cognitive impairment was the most common grade of severity accounting for 120 out of 2728 (4.4%). More severe cases were encountered in 1.4% (moderate impairment), 1.6% (severe impairment) and 0.9% (severest impairment) of the cases. In 8.9% of the epilepsy cases, cognitive impairment was coded without documentation of the grade of severity (Fig. 3).
The impact of age of epilepsy onset on the relative risk for cognitive impairment in epilepsy
To assess the association of cognitive impairment and age of epilepsy onset, we stratified the analysis by age group (Fig. 4). The relative risk for cognitive impairment was highest in epilepsy cases with seizure manifestation within the first 2 years of life than in patients with seizure manifestation in preschool (2–5 years) and school (6–10 years) age (RR 16.9 vs. 9.9 and 6.4, respectively).
The temporal relation of epilepsy onset and cognitive impairment
Considering the temporal sequence of the diagnoses of epilepsy and cognitive impairment, the prevalence of cognitive impairment before epilepsy diagnosis was slightly higher (2.5%, 78/2728) compared to the prevalence of the general population (1.7%, 2309/139,835) with an increased risk of RR 1.7 (95% CI 1.4, 2.2). The risk for cognitive impairment in the years at and after the epilepsy diagnosis was significantly increased (RR 8.8 (95% CI 8.0, 9.7)) compared to cognitive impairment in children without epilepsy (Fig. 5).
Discussion
In the present study, we analyzed a birth cohort of considerable size based on healthcare data. We observed a cumulative incidence of epilepsy up the age of 10 slightly above the upper range of other studies with different approaches for assessment. We found an about ten-fold higher risk for cognitive impairment in children with epilepsy than in children without epilepsy, which was most pronounced for severe cognitive impairment. The risk for cognitive impairment in epilepsy cases was higher in younger children. Though the risk for cognitive impairment was slightly increased prior to the onset of epilepsy compared to controls, cognitive impairment mainly appears to follow the onset of epilepsy.
Epidemiology of epilepsy and cognitive impairment
Reported incidences for epilepsy in children vary from 41/100,000 to 187/100,000 [23]. Our incidence estimates of 191 [95% CI 185, 200] per 100,000 person years in the first 10 years is higher than the previously reported. There are several possible reasons for this: different age ranges [24], different case definitions since some require the use of ASM [25], or potential misclassification, since no individual case validation was possible in our data. The latter would account for an overestimation for prevalence and an underestimation of the risk for cognitive impairment. In accordance with others, we observed the highest risk for onset of epilepsy in the first year of life [26, 27]. Furthermore, higher incidence and prevalence rates for epilepsy are more likely to occur in claims data analyses compared to field data research. This was recently shown in a large claims-based analysis in adults with epilepsy providing different estimates depending on diagnosis criteria [28]. Another explanation for the high incidence rate of epilepsy in the present study might be related to the search strategy which might appear to “loose”. One could argue i.e. to include only G40 patients who receive ASM. However, this could led to false exclusion of patients with mild epilepsy phenotypes as rolandic epilepsy, who might be left untreated in some circumstances [29]. Nevertheless, a selection bias toward false classified patients as epileptic patients cannot be excluded in the present study. Approximately 3% of children of school age are suspected to have cognitive impairment [30], which is slightly higher than our estimate with 2%. Since diagnosis of cognitive impairment requires intelligence testing, the physicians’ diagnostic coding is likely to be valid. Some non-differential under-ascertainment appears possible because of failure to send all cases with developmental delay for IQ testing.
The prevalence and risk of cognitive impairment in epilepsy
Population-based studies in cohorts of children with epilepsy found cognitive impairment or subnormal cognitive function in about one third of the cases [6, 11, 12]. The prevalence of cognitive impairment in children with epilepsy in absence of a control group does not indicate the risk. Assessment of the risk requires a control group of children without epilepsy. Identical ascertainment for cognitive impairment for both the epilepsy cohort and the non-epilepsy cohort is mandatory for valid risk estimates. This is a unique feature in our data. We could not identify previous population-based studies including a contemporary control group in the same health insurance setting. Although only 17.4% of our cases had cognitive impairment, their risk for cognitive impairment compared to children without epilepsy was increased by a factor of about ten. A recent claim-based analysis on developmental speech and language disorders revealed a high prevalence in epileptic patients’ age 0–19 years [31]. Given the close association between language development and cognition, these results supports or our findings.
Age-dependent risk of cognitive impairment in children with epilepsy
Cognitive impairment is more common in children with early epilepsy onset, and in children with high burden epilepsy for example in children, who develop drug-resistant seizures [32,33,34]. In early onset cases, the following factors might impact cognitive function: etiology, seizure frequency, presences and absence of EEG-status and the type and total load of ASM. The latter is supposed to be high in this age group according to high incidence of medically refractory cases due to above mentioned etiologies [35]. The design of the present study does not allow to further dissect the role of these different parameters. Data on genetic epilepsies i.e. Dravet syndrome suggest that epilepsy-specific parameters like seizure frequency contribute less to cognitive decline than the underlying biological cause (= etiology) itself [36].
The temporal relation of cognitive impairment and onset of epilepsy
The risk of cognitive impairment was slightly higher prior to the diagnosis of epilepsy than in children without epilepsy, but further increased during the course of disease suggesting that epilepsy-specific parameters as seizure frequency may increase the risk of cognitive impairment. Nevertheless, this association might also be due to increased awareness to intellectual impairment triggering more systematic cognitive testing once the diagnosis of epilepsy is established. Furthermore, the diagnosis of intellectual impairment by means of an ICD F7* diagnosis cannot be established within the first years of life and these patients might diagnosed instead with the ICD code of global developmental delay (R62.8), which was not considered in our study. Patients with an increased risk of cognitive impairment before seizure onset suggest strong contributing factors on cognitive impairment besides typical epilepsy-related factors (as seizure frequency and drug treatment). Most likely, etiological factors causing cognitive impairment are also responsible for the predisposition of epileptic seizures. For example, patients with structural brain damage, i.e. due to perinatal hypoxemia or malformations of cortical development may reflect cognitive impairment before seizure initiation. For patients with epilepsies associated with mainly monogenetic causes, it was even proposed to call these syndromes ‘Developmental brain disorders with the comorbidity of epilepsy’ to pronounce the high impact of other underlying dysfunction beside epilepsy and to acknowledge the importance of the neurobiological basis in causing both seizures and cognitive impairment [8]. Nevertheless, cognition might deteriorate upon seizure onset in some circumstances. This bidirectional relationship [37] between epilepsy and cognition is especially visible in patients with structural brain damage and new onset West-syndrome: while developmental delay is usually present prior seizure onset, the beginning of epileptic spams and the EEG patterns of hypsarrhythmia coincides with further cognitive deterioration in the patients.
Homogeneity of the analyzed cohort
Ninety percent of the German population is insured by statutory health insurances. There are no obligations with respect to socio-economic status to join either of the statutory insurances suggesting homogeneity of the insured population. Eventually, patients insured by private insurances (10%) have higher income compared to people in statutory insurances. Incidence rates of neurological conditions do not differ between these two types of insurances. Furthermore, there are no differences in the proportion of insured children and adolescents and the amount of utilization of the health care system [38]. External validity is further supported by Hoffman et al., who compared adults with different statutory health insurance in Germany. They did not find a difference regarding educational level, but a slightly higher prevalence of chronic diseases in BARMER insured persons [39].
Case definition
In the present study, we did not use G41 (status epilepticus) as a diagnosis of epilepsy unless G40 was concomitantly coded as described in the method section. Status epilepticus in children is most often caused by acute conditions (most commonly by fever followed by CNS infections, trauma, etc.) [40]. In the case of recurrent status epilepticus in children, an underlying epilepsy is evident in the vast majority of cases [41] and these patients are most likely covered by the G40 case definition we provided within the method section. Accordingly, we considered status epilepticus as a diagnosis of a prolonged (mostly symptomatic) seizure rather than a chronic disease as epilepsy. It could be further argued for excluding patients with G41 and without G40 diagnosis from the control group as they might carry an increased risk of later neurodevelopmental impairment [42]. Consequently, one would have to consider excluding other neurological conditions, too. The term “control” group might be misleading in this context: “control group” means that this group should not contain patients with epilepsy but does not imply the inclusion of solely healthy subjects. The true increase in cognitive impairment by epilepsy might thus be rather underestimated. Febrile convulsions (R56.1) were included in the control group unless the diagnosis of epilepsy (G40) was coded as the majority of cases with febrile convulsions are not associated with epilepsy and have a favorable neurodevelopmental outcome [43].
Strengths and limitations
There are few population-based data on the incidence of epilepsy and diagnoses of cognitive impairment in pre-pubertal children, even fewer with a complete follow-up throughout the first 10 years of life and inclusion of control subjects. Such data allow for valid assessment of the population attributable risk for epilepsy, the temporal sequence of comorbidities and comparison to the risk in children without epilepsy.
Limitation of the analysis is the structure of the dataset, which precludes individual case validation for the diagnosis of epilepsy as well as for the diagnosis of cognitive impairment. Misclassification, therefore, appears possible. Incorrect ICD coding of patients with seizures not fulfilling the criterion of chronic epilepsy as defined by the ILAE might be taken in account [44]. However, the accuracy of identification of epilepsy cases using healthcare administration data based on ICD G40* yielded a positive/negative predictive value, sensitivity and specificity > 80% in the majority of studies [20, 45, 46].
Regarding cognitive impairment, we have no data on whether IQ testing was performed equally often in children with and without epilepsy. The prevalence of cognitive impairment within entire study population studied, however, was comparable with the literature. Although, BARMER is a major statutory health insurer in Germany limitations regarding external validity cannot be definitively ruled out.
The definition of the pre-pubertal period might be misleading in patients with epilepsy. Especially in patients with epilepsy and additional cognitive impairment, puberty might precocious physiologically expected [47].
We did not dissect the epilepsy to further syndromes and etiologies, which is due to the nature of the ICD classification system. Epilepsy classification according to the ILAE has changed significantly over time and although ICD classification divides epilepsy into focal and generalized syndromes, this appears to be only a rough approach of categorizing epilepsy syndromes [48,49,50]. Furthermore, epidemiologic studies as performed here cannot prove causality, and even less a role of specific underlying mechanism. Thus, we describe associations and present possibly explanations rather than proving causality or even certain biological mechanisms.
Conclusions
The strength of the association of epilepsy and cognitive impairment appears to be a factor of about ten. Children with early epilepsy manifestation are especially at high risk for the diagnosis of cognitive impairment. The diagnosis of cognitive impairment was coded after epilepsy diagnosis in the majority of the cases. This might reflect different explanations as (1) an increased awareness of cognitive comorbidities once the epilepsy diagnosis is established, (2) the difficulty in diagnosing the F7* code in very young children, and (3) the impact of epilepsy-specific parameters in cognition itself in some cases or a common cause for both (4).
Data availability
This is an analysis on healthcare data, not owned by the authors. BARMER gives remote access to their data to researchers who provide a methodologically sound proposal for use in achieving the goals of the approved proposal.
Abbreviations
- ICD:
-
International classification of diseases
- IQ:
-
Intelligence quotient
- ATC:
-
Anatomical therapeutic chemical classification
- ASM:
-
Antiseizure medication
- CI:
-
Confidence interval
- RR:
-
Relative risk
- SD:
-
Standard deviation
References
Bourgeois BF, Prensky AL, Palkes HS et al (1983) Intelligence in epilepsy: a prospective study in children. Ann Neurol. https://doi.org/10.1002/ana.410140407
Baca CB, Vickrey BG, Caplan R et al (2011) Psychiatric and medical comorbidity and quality of life outcomes in childhood-onset epilepsy. Pediatrics 128:e1532–e1543. https://doi.org/10.1542/peds.2011-0245
Fayed N, Davis AM, Streiner DL et al (2015) Children’s perspective of quality of life in epilepsy. Neurology 84:1830–1837. https://doi.org/10.1212/WNL.0000000000001536
Cheung C, Wirrell E (2006) Adolescents’ perception of epilepsy compared with other chronic diseases: “through a teenager’s eyes.” J Child Neurol 21:214–222. https://doi.org/10.2310/7010.2006.00053
Berg AT, Baca CB, Rychlik K et al (2016) Determinants of social outcomes in adults with childhood-onset epilepsy. Pediatrics. https://doi.org/10.1542/peds.2015-3944
Nickels KC, Zaccariello MJ, Hamiwka LD et al (2016) Cognitive and neurodevelopmental comorbidities in paediatric epilepsy. Nat Rev Neurol 12:465–476. https://doi.org/10.1038/nrneurol.2016.98
Moorhouse FJ, Cornell S, Gerstl L et al (2020) Cognitive performance and behavior across idiopathic/genetic epilepsies in children and adolescents. Sci Rep 10:21543. https://doi.org/10.1038/s41598-020-78218-0
Berg AT, Tarquinio D, Koh S (2017) Early life epilepsies are a comorbidity of developmental brain disorders. Sem Pediatr Neurol. https://doi.org/10.1016/j.spen.2017.10.008
Andrew T, Milinis K, Baker G et al (2012) Self reported adverse effects of mono and polytherapy for epilepsy. Seizure 21:610–613. https://doi.org/10.1016/j.seizure.2012.06.013
Besag F, Gobbi G, Aldenkamp A et al (2016) Psychiatric and behavioural disorders in children with epilepsy (ILAE task force report): behavioural and psychiatric disorders associated with childhood epilepsy syndromes. Epileptic Disord. https://doi.org/10.1684/epd.2016.0815
Murphy CC, Trevathan E, Yeargin-Allsopp M (1995) Prevalence of epilepsy and epileptic seizures in 10-year-old children: results from the metropolitan Atlanta developmental disabilities study. Epilepsia 36:866–872. https://doi.org/10.1111/j.1528-1157.1995.tb01629.x
Berg AT, Langfitt JT, Testa FM et al (2008) Global cognitive function in children with epilepsy: a community-based study. Epilepsia 49:608–614. https://doi.org/10.1111/j.1528-1167.2007.01461.x
Verband der Ersatzkassen EV (vdek) (2020) Daten zum Gesundheitswesen: Versicherte [Data on health care: Insured persons]. https://www.vdek.com/presse/daten/b_versicherte.html. Accessed 27 Nov 2020
Zentrale Vereinigung für bürgernahe Verbraucherinformationen. The Health Insurance System in Germany. https://www.krankenkassenzentrale.de/wiki/incoming-en#. Accessed 27 Nov 2020
GKV-Spitzenverband Alle gesetzlichen Krankenkassen—GKV-Spitzenverband [All statutory health insurance companies]. https://www.gkv-spitzenverband.de/krankenversicherung/kv_grundprinzipien/alle_gesetzlichen_krankenkassen/alle_gesetzlichen_krankenkassen.jsp. Accessed 27 Nov 2020
Barmer Coredata of BARMER. https://www.barmer.de/presse/infothek/daten-und-fakten/kerndaten-42164. Accessed 27 Nov 2020
Federal Statistical Office Germany Population size Germany: GENESIS-Online: Ergebnis 12411–0001. https://www-genesis.destatis.de/genesis/online?operation=abruftabelleBearbeiten&levelindex=2&levelid=1606484943866&auswahloperation=abruftabelleAuspraegungAuswaehlen&auswahlverzeichnis=ordnungsstruktur&auswahlziel=werteabruf&code=12411-0001&auswahltext=&werteabruf=starten#abreadcrumb. Accessed 27 Nov 2020
Wittig R, Albers L, Koletzko S et al (2019) Pediatric chronic inflammatory bowel disease in a german statutory health INSURANCE-incidence rates from 2009 to 2012. J Pediatr Gastroenterol Nutr 68:244–250. https://doi.org/10.1097/MPG.0000000000002162
Bundesinstitut für Arzneimittel und Medizinprodukte Deutsches Institut für medizinische Dokumentation und Information (DIMDI) [German Institute for Medical Documentation and Information ] ICD-10-GM Version 2020. https://www.dimdi.de/static/de/klassifikationen/icd/icd-10-gm/kode-suche/htmlgm2020/. Accessed 27 Nov 2020
Reid AY, St G-SC, Liu M et al (2012) Development and validation of a case definition for epilepsy for use with administrative health data. Epilepsy Res. https://doi.org/10.1016/j.eplepsyres.2012.05.009
Agresti A, Coull BA (1998) Approximate is better than “exact” for interval estimation of binomial proportions. Am Stat 52:119–126. https://doi.org/10.1080/00031305.1998.10480550
Brown LD, Cai TT, DasGupta A (2001) Interval estimation for a binomial proportion. Stat Sci 16:101–117
Camfield P, Camfield C (2015) Incidence, prevalence and aetiology of seizures and epilepsy in children. Epileptic Disord 17:117–123. https://doi.org/10.1684/epd.2015.0736
Sillanpää M, Lastunen S, Helenius H et al (2011) Regional differences and secular trends in the incidence of epilepsy in Finland: a nationwide 23-year registry study. Epilepsia 52:1857–1867. https://doi.org/10.1111/j.1528-1167.2011.03186.x
Saarinen MM, Sillanpää M, Schmidt D et al (2016) Long-term changes in the incidence of childhood epilepsy. A population study from Finland. Epilepsy Behav 58:81–85. https://doi.org/10.1016/j.yebeh.2016.02.040
Doose H, Sitepu B (1983) Childhood epilepsy in a German city. Neuropediatrics 14:220–224. https://doi.org/10.1055/s-2008-1059582
Durá-Travé T, Yoldi-Petri ME, Gallinas-Victoriano F (2008) Incidence of epilepsies and epileptic syndromes among children in Navarre, Spain: 2002 through 2005. J Child Neurol 23:878–882. https://doi.org/10.1177/0883073808314898
Ertl J, Hapfelmeier J, Peckmann T et al (2016) Guideline conform initial monotherapy increases in patients with focal epilepsy: a population-based study on German health insurance data. Seizure 41:9–15. https://doi.org/10.1016/j.seizure.2016.07.001
Hughes JR (2010) Benign epilepsy of childhood with centrotemporal spikes (BECTS): to treat or not to treat, that is the question. Epilepsy Behav 19:197–203. https://doi.org/10.1016/j.yebeh.2010.07.018
Roeleveld N, Zielhuis GA, Gabreëls F (1997) The prevalence of mental retardation: a critical review of recent literature. Dev Med Child Neurol 39:125–132. https://doi.org/10.1111/j.1469-8749.1997.tb07395.x
Sommer M, Waltersbacher A, Schlotmann A et al (2021) Prevalence and therapy rates for stuttering, cluttering, and developmental disorders of speech and language: evaluation of german health insurance data. Front Hum Neurosci 15:645292. https://doi.org/10.3389/fnhum.2021.645292
Symonds JD, Zuberi SM, Stewart K et al (2019) Incidence and phenotypes of childhood-onset genetic epilepsies: a prospective population-based national cohort. Brain 142:2303–2318. https://doi.org/10.1093/brain/awz195
Berg AT, Zelko FA, Levy SR et al (2012) Age at onset of epilepsy, pharmacoresistance, and cognitive outcomes: a prospective cohort study. Neurology 79:1384–1391. https://doi.org/10.1212/WNL.0b013e31826c1b55
Wirrell E, Wong-Kisiel L, Mandrekar J et al (2012) Predictors and course of medically intractable epilepsy in young children presenting before 36 months of age: a retrospective, population-based study. Epilepsia. https://doi.org/10.1111/j.1528-1167.2012.03562.x
Berg AT, Wusthoff C, Shellhaas RA et al (2019) Immediate outcomes in early life epilepsy: a contemporary account. Epilepsy Behav 97:44–50. https://doi.org/10.1016/j.yebeh.2019.05.011
Nabbout R, Chemaly N, Chipaux M et al (2013) Encephalopathy in children with Dravet syndrome is not a pure consequence of epilepsy. Orphanet J Rare Dis 8:176. https://doi.org/10.1186/1750-1172-8-176
Helmstaedter C, Witt J-A (2017) Epilepsy and cognition—a bidirectional relationship? Seizure 49:83–89. https://doi.org/10.1016/j.seizure.2017.02.017
Ochmann R, Albrecht M, Schiffhorst et al. Geteilter Geteilter Krankenversicherungsmarkt: Risikoselektion und regionale Verteilung der Ärzte. https://www.bertelsmann-stiftung.de/fileadmin/files/BSt/Publikationen/GrauePublikationen/VV_Studie_Geteilter_Krankenversicherungsmarkt.pdf. Accessed 01 Feb 2022
Hoffmann F, Icks A (2012) Unterschiede in der Versichertenstruktur von Krankenkassen und deren Auswirkungen für die Versorgungsforschung: Ergebnisse des Bertelsmann-Gesundheitsmonitors (structural differences between health insurance funds and their impact on health services research: results from the Bertelsmann health-care monitor). Gesundheitswesen 74:291–297. https://doi.org/10.1055/s-0031−1275711
Chin RFM, Neville BGR, Peckham C et al (2006) Incidence, cause, and short-term outcome of convulsive status epilepticus in childhood: prospective population-based study. The Lancet 368:222–229. https://doi.org/10.1016/S0140-6736(06)69043-0
Shinnar S, Maytal J, Krasnoff L et al (1992) Recurrent status epilepticus in children. Ann Neurol 31:598–604. https://doi.org/10.1002/ana.410310606
Martinos MM, Yoong M, Patil S et al (2013) Early developmental outcomes in children following convulsive status epilepticus: a longitudinal study. Epilepsia 54:1012–1019. https://doi.org/10.1111/epi.12136
Verity CM, Greenwood R, Golding J (1998) Long-term intellectual and behavioral outcomes of children with febrile convulsions. N Engl J Med 338:1723–1728. https://doi.org/10.1056/NEJM199806113382403
Fisher RS, Acevedo C, Arzimanoglou A et al (2014) ILAE official report: a practical clinical definition of epilepsy. Epilepsia 55:475–482. https://doi.org/10.1111/epi.12550
Mbizvo GK, Bennett KH, Schnier C et al (2020) The accuracy of using administrative healthcare data to identify epilepsy cases: a systematic review of validation studies. Epilepsia 61:1319–1335. https://doi.org/10.1111/epi.16547
Fonferko-Shadrach B, Lacey AS, White CP et al (2017) Validating epilepsy diagnoses in routinely collected data. Seizure 52:195–198. https://doi.org/10.1016/j.seizure.2017.10.008
Winter S, Durand A, Brauner R (2019) Precocious and early central puberty in children with pre-existing medical conditions: a single center study. Front Pediatr 7:35. https://doi.org/10.3389/fped.2019.00035
Engel J (2001) A proposed diagnostic scheme for people with epileptic seizures and with epilepsy: report of the ILAE task force on classification and terminology. Epilepsia 42:796–803. https://doi.org/10.1046/j.1528-1157.2001.10401.x
Berg AT, Berkovic SF, Brodie MJ et al (2010) Revised terminology and concepts for organization of seizures and epilepsies: report of the ILAE commission on classification and terminology, 2005–2009. Epilepsia 51:676–685. https://doi.org/10.1111/j.1528-1167.2010.02522.x
Scheffer IE, Berkovic S, Capovilla G et al (2017) ILAE classification of the epilepsies: position paper of the ILAE commission for classification and terminology. Epilepsia 58:512–521. https://doi.org/10.1111/epi.13709
Acknowledgements
The authors thank the BARMER health insurance, in particular Dr. Ursula Marshall, for providing access to the BARMER health insurance data.
Funding
Open Access funding enabled and organized by Projekt DEAL. The project was conducted with no specific support or funding.
Author information
Authors and Affiliations
Contributions
IB and RvK conceptualized and designed the study, drafted the initial manuscript, and reviewed and revised the manuscript. A-LS carried out the analyses, conceptualized and designed the study, drafted the initial manuscript, and reviewed and revised the manuscript. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflicts of interest
None of the authors has any conflict of interests to disclose.
Ethical statement
The ethics committee of the medical faculty of the Ludwig-Maximilians-University Munich gave ethical approval (Number 17–742 UE until 17–746 UE).
Consent to participate
Data were obtained from administrative healthcare data. Informed consent is not necessary in retrospective data analysis of pseudonymized healthcare data.
Consent for publication
All authors have approved the manuscript for submission, accordingly the manuscript conforms to the journal’s policies. The authors take full responsibility for the data, the analyses and interpretation, and the conduct of the research. They have full access to all of the data, and the right to publish any and all data.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Sorg, AL., von Kries, R. & Borggraefe, I. Cognitive disorders in childhood epilepsy: a comparative longitudinal study using administrative healthcare data. J Neurol 269, 3789–3799 (2022). https://doi.org/10.1007/s00415-022-11008-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-022-11008-y