Abstract
Purpose
We aimed to investigate the ability of MRI radiomics features-based machine learning (ML) models to classify the time since stroke onset (TSS), which could aid in stroke assessment and treatment options.
Methods
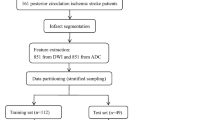
This study involved 84 patients with acute ischemic stroke due to anterior circulation artery occlusion (51 in the training cohort and 33 in the independent test cohort). Region of infarct segmentation was manually outlined by 3D-slicer software. Image processing including registration, normalization and radiomics features calculation were done in R (version 3.6.1). A total of 4312 radiomic features from each image sequence were captured and used in six ML models to estimate stroke onset time for binary classification (≤ 4.5 h). Receiver-operating characteristic curve (ROC) and other parameters were calculated to evaluate the performance of the models in both training and test cohorts.
Results
Twelve radiomics and six clinic features were selected to construct the ML models for TSS classification. The deep learning model-based DWI/ADC radiomic features performed the best for binary TSS classification in the independent test cohort, with an AUC of 0.754, accuracy of 0.788, sensitivity of 0.952, specificity of 0.500, positive predictive value of 0.769, and negative predictive value of 0.857, respectively. Furthermore, adding clinical information did not improve the performance of the DWI/ADC-based deep learning model. The TSS prediction models can be visited at: http://123.57.65.199:3838/deeptss/.
Conclusions
A unique deep learning model based on DWI/ADC radiomic features was constructed for TSS classification, which could aid in decision making for thrombolysis in patients with unknown stroke onset.





Similar content being viewed by others
Availability of data and material
All data generated or analyzed during this study are included in this published article.
References
Sivanandy P, Thomas B, Krishnan V, Arunachalam S (2011) Safety and efficacy of thrombolytic therapy using rt-PA (alteplase) in acute ischemic stroke. ISRN Neurol 2011:618624. https://doi.org/10.5402/2011/618624
Wang Y, Liao X, Zhao X, Wang DZ, Wang C, Nguyen-Huynh MN, Zhou Y, Liu L, Wang X, Liu G, Li H, Wang Y, Registry CNS, I, (2011) Using recombinant tissue plasminogen activator to treat acute ischemic stroke in China: analysis of the results from the Chinese National Stroke Registry (CNSR). Stroke 42(6):1658–1664. https://doi.org/10.1161/STROKEAHA.110.604249
Li X, Wu L, Xie H, Bao Y, He D, Luo X (2020) Endovascular treatment for ischemic stroke beyond the time window: a meta-analysis. Acta Neurol Scand 141(1):3–13. https://doi.org/10.1111/ane.13161
Peter-Derex L, Derex L (2019) Wake-up stroke: from pathophysiology to management. Sleep Med Rev 48:101212. https://doi.org/10.1016/j.smrv.2019.101212
Rimmele DL, Thomalla G (2014) Wake-up stroke: clinical characteristics, imaging findings, and treatment option—an update. Front Neurol 5:35. https://doi.org/10.3389/fneur.2014.00035
Thomalla G, Rossbach P, Rosenkranz M, Siemonsen S, Krutzelmann A, Fiehler J, Gerloff C (2009) Negative fluid-attenuated inversion recovery imaging identifies acute ischemic stroke at 3 hours or less. Ann Neurol 65(6):724–732. https://doi.org/10.1002/ana.21651
Koga M, Yamamoto H, Inoue M, Asakura K, Aoki J, Hamasaki T, Kanzawa T, Kondo R, Ohtaki M, Itabashi R, Kamiyama K, Iwama T, Nakase T, Yakushiji Y, Igarashi S, Nagakane Y, Takizawa S, Okada Y, Doijiri R, Tsujino A, Ito Y, Ohnishi H, Inoue T, Takagi Y, Hasegawa Y, Shiokawa Y, Sakai N, Osaki M, Uesaka Y, Yoshimura S, Urabe T, Ueda T, Ihara M, Kitazono T, Sasaki M, Oita A, Yoshimura S, Fukuda-Doi M, Miwa K, Kimura K, Minematsu K, Toyoda K, TT Investigators (2020) Thrombolysis with alteplase at 0.6 mg/kg for stroke with unknown time of onset: a randomized controlled trial. Stroke 51(5):1530–1538. https://doi.org/10.1161/STROKEAHA.119.028127
Campbell BCV, Ma H, Ringleb PA, Parsons MW, Churilov L, Bendszus M, Levi CR, Hsu C, Kleinig TJ, Fatar M, Leys D, Molina C, Wijeratne T, Curtze S, Dewey HM, Barber PA, Butcher KS, De Silva DA, Bladin CF, Yassi N, Pfaff JAR, Sharma G, Bivard A, Desmond PM, Schwab S, Schellinger PD, Yan B, Mitchell PJ, Serena J, Toni D, Thijs V, Hacke W, Davis SM, Donnan GA, EXTEND, ECASS-4, and EPITHET Investigators (2019) Extending thrombolysis to 4.5–9 h and wake-up stroke using perfusion imaging: a systematic review and meta-analysis of individual patient data. Lancet 394(10193):139–147. https://doi.org/10.1016/S0140-6736(19)31053-0
Thomalla G, Simonsen CZ, Boutitie F, Andersen G, Berthezene Y, Cheng B, Cheripelli B, Cho TH, Fazekas F, Fiehler J, Ford I, Galinovic I, Gellissen S, Golsari A, Gregori J, Gunther M, Guibernau J, Hausler KG, Hennerici M, Kemmling A, Marstrand J, Modrau B, Neeb L, Perez de la Ossa N, Puig J, Ringleb P, Roy P, Scheel E, Schonewille W, Serena J, Sunaert S, Villringer K, Wouters A, Thijs V, Ebinger M, Endres M, Fiebach JB, Lemmens R, Muir KW, Nighoghossian N, Pedraza S, Gerloff C, W-U Investigators (2018) MRI-guided thrombolysis for stroke with unknown time of onset. N Engl J Med 379(7):611–622. https://doi.org/10.1056/NEJMoa1804355
Thomalla G, Fiebach JB, Ostergaard L, Pedraza S, Thijs V, Nighoghossian N, Roy P, Muir KW, Ebinger M, Cheng B, Galinovic I, Cho TH, Puig J, Boutitie F, Simonsen CZ, Endres M, Fiehler J, Gerloff C, WAKE-UP Investigators (2014) A multicenter, randomized, double-blind, placebo-controlled trial to test efficacy and safety of magnetic resonance imaging-based thrombolysis in wake-up stroke (WAKE-UP). Int J Stroke 9(6):829–836. https://doi.org/10.1111/ijs.12011
Scheldeman L, Wouters A, Boutitie F, Dupont P, Christensen S, Cheng B, Ebinger M, Endres M, Fiebach JB, Gerloff C, Muir KW, Nighoghossian N, Pedraza S, Simonsen CZ, Thijs V, Thomalla G, Lemmens R, WAKE-UP Investigators (2020) Different mismatch concepts for magnetic resonance imaging-guided thrombolysis in unknown onset stroke. Ann Neurol 87(6):931–938. https://doi.org/10.1002/ana.25730
Emeriau S, Serre I, Toubas O, Pombourcq F, Oppenheim C, Pierot L (2013) Can diffusion-weighted imaging-fluid-attenuated inversion recovery mismatch (positive diffusion-weighted imaging/negative fluid-attenuated inversion recovery) at 3 Tesla identify patients with stroke at <4.5 hours. Stroke 44(6):1647–1651. https://doi.org/10.1161/STROKEAHA.113.001001
Thomalla G, Cheng B, Ebinger M, Hao Q, Tourdias T, Wu O, Kim JS, Breuer L, Singer OC, Warach S, Christensen S, Treszl A, Forkert ND, Galinovic I, Rosenkranz M, Engelhorn T, Kohrmann M, Endres M, Kang DW, Dousset V, Sorensen AG, Liebeskind DS, Fiebach JB, Fiehler J, Gerloff C, the STIR and VISTA Imaging Investigators (2011) DWI-FLAIR mismatch for the identification of patients with acute ischaemic stroke within 4.5 h of symptom onset (PRE-FLAIR): a multicentre observational study. Lancet Neurol 10(11):978–986. https://doi.org/10.1016/S1474-4422(11)70192-2
Ziegler A, Ebinger M, Fiebach JB, Audebert HJ, Leistner S (2012) Judgment of FLAIR signal change in DWI-FLAIR mismatch determination is a challenge to clinicians. J Neurol 259(5):971–973. https://doi.org/10.1007/s00415-011-6284-6
Kim BJ, Kim HJ, Lee DH, Kwon SU, Kim SJ, Kim JS, Kang DW (2014) Diffusion-weighted image and fluid-attenuated inversion recovery image mismatch: unclear-onset versus clear-onset stroke. Stroke 45(2):450–455. https://doi.org/10.1161/STROKEAHA.113.002830
Ogata T, Nagakane Y, Christensen S, Ma H, Campbell BC, Churilov L, Olivot JM, Desmond PM, Albers GW, Davis SM, Donnan GA, Epithet ID (2011) A topographic study of the evolution of the MR DWI/PWI mismatch pattern and its clinical impact: a study by the EPITHET and DEFUSE Investigators. Stroke 42(6):1596–1601. https://doi.org/10.1161/STROKEAHA.110.609016
Odland A, Saervoll P, Advani R, Kurz MW, Kurz KD (2015) Are the current MRI criteria using the DWI-FLAIR mismatch concept for selection of patients with wake-up stroke to thrombolysis excluding too many patients? Scand J Trauma Resusc Emerg Med 23:22. https://doi.org/10.1186/s13049-015-0101-7
Bianconi F, Fravolini ML, Bello-Cerezo R, Minestrini M, Scialpi M, Palumbo B (2018) Evaluation of shape and textural features from CT as prognostic biomarkers in non-small cell lung cancer. Anticancer Res 38(4):2155–2160. https://doi.org/10.21873/anticanres.12456
Chung JW, Kim YC, Cha J, Choi EH, Kim BM, Seo WK, Kim GM, Bang OY (2019) Characterization of clot composition in acute cerebral infarct using machine learning techniques. Ann Clin Transl Neurol 6(4):739–747. https://doi.org/10.1002/acn3.751
Rehme AK, Volz LJ, Feis DL, Bomilcar-Focke I, Liebig T, Eickhoff SB, Fink GR, Grefkes C (2015) Identifying neuroimaging markers of motor disability in acute stroke by machine learning techniques. Cereb Cortex 25(9):3046–3056. https://doi.org/10.1093/cercor/bhu100
Panayides AS, Pattichis MS, Leandrou S, Pitris C, Constantinidou A, Pattichis CS (2019) Radiogenomics for precision medicine with a big data analytics perspective. IEEE J Biomed Health Inform 23(5):2063–2079. https://doi.org/10.1109/JBHI.2018.2879381
Holzinger A, Haibe-Kains B, Jurisica I (2019) Why imaging data alone is not enough: AI-based integration of imaging, omics, and clinical data. Eur J Nucl Med Mol Imaging 46(13):2722–2730. https://doi.org/10.1007/s00259-019-04382-9
Kolossvary M, Karady J, Szilveszter B, Kitslaar P, Hoffmann U, Merkely B, Maurovich-Horvat P (2017) Radiomic features are superior to conventional quantitative computed tomographic metrics to identify coronary plaques with napkin-ring sign. Circ Cardiovasc Imaging. https://doi.org/10.1161/CIRCIMAGING.117.006843
Kamal H, Lopez V, Sheth SA (2018) Machine learning in acute ischemic stroke neuroimaging. Front Neurol 9:945. https://doi.org/10.3389/fneur.2018.00945
Sheth SA, Lopez-Rivera V, Barman A, Grotta JC, Yoo AJ, Lee S, Inam ME, Savitz SI, Giancardo L (2019) Machine learning-enabled automated determination of acute ischemic core from computed tomography angiography. Stroke 50(11):3093–3100. https://doi.org/10.1161/STROKEAHA.119.026189
Feng R, Badgeley M, Mocco J, Oermann EK (2018) Deep learning guided stroke management: a review of clinical applications. J Neurointerv Surg 10(4):358–362. https://doi.org/10.1136/neurintsurg-2017-013355
Lee H, Lee EJ, Ham S, Lee HB, Lee JS, Kwon SU, Kim JS, Kim N, Kang DW (2020) Machine learning approach to identify stroke within 4.5 hours. Stroke 51(3):860–866. https://doi.org/10.1161/STROKEAHA.119.027611
Straka M, Albers GW, Bammer R (2010) Real-time diffusion-perfusion mismatch analysis in acute stroke. J Magn Reson Imaging 32(5):1024–1037. https://doi.org/10.1002/jmri.22338
Funding
This study was supported by the grants from National Key Basic Research Program of China (973 program) (Grant No. 2013CB733805), and the National Natural Science Foundation of China (Grant Nos. 81871464, and 61671440).
Author information
Authors and Affiliations
Contributions
WJJ, YQZ, AFL, and JL conceived and designed the experiments, YQZ and AFL performed the experiments, JL, YYZ, YDZ and AFL analyzed the data, YYZ, YDZ, CL, YEL, YQZ and JZ contributed reagents/materials/analysis tools, APZ, YYZ and JL drafted the manuscript, JL and WJJ revised the draft. All authors reviewed the manuscript. FYM made substantial contribution to the conception and interpretation of data, and involved in revising it critically for important intellectual content.
Corresponding authors
Ethics declarations
Conflicts of interest
The authors declare that they have no competing interests.
Ethical approval
This study was approved by the institutional ethics committee at the PLA Rocket Force Characteristic Medical Center (Approval No. KeYan 2013031).
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Zhang, YQ., Liu, AF., Man, FY. et al. MRI radiomic features-based machine learning approach to classify ischemic stroke onset time. J Neurol 269, 350–360 (2022). https://doi.org/10.1007/s00415-021-10638-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-021-10638-y