Abstract
Objective
To study the diagnostic value of salivary pepsin measurement (Peptest) for detecting gastroesophageal reflux disease (GERD) in laryngopharyngeal reflux (LPR) patients.
Methods
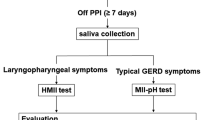
Patients with reflux symptoms were consecutively recruited from January 2020 to November 2022. Patients benefited from hypopharyngeal–esophageal impedance-pH monitoring (HEMII-pH), fasting and bedtime saliva collections to measure pepsin. Sensitivity, specificity, positive (PPV) and negative (NPV) predictive values were evaluated for GERD and LPR patients considering the highest values of pepsin tests at ≥ 16, ≥ 75, and ≥ 216 ng/mL cutoffs. The relationship between HEMII-pH, endoscopic and clinical findings, and pepsin measurements was studied.
Results
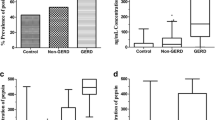
Saliva was collected in 109 LPR patients and 30 individuals with both LPR and GERD. The total number of pharyngeal reflux events was significantly higher in GERD-LPR patients compared with LPR patients (p = 0.008). The mean fasting and bedtime pepsin saliva concentrations were similar between groups. The sensitivity of Peptest in LPR patients was 30.5%, 70.2%, and 84.0% at cutoffs ≥ 16, ≥ 75 and ≥ 216 ng/mL. In GERD-LPR group, Peptest was 80.0%, 70.0%, and 30.0% sensitive. At cutoff 16 ng/mL, Peptest reported PPV of 20.7% and 94.8% in LPR-GERD and LPR groups, respectively. NPV were 73.9% and 8.7% in GERD-LPR and LPR groups, respectively. The consistency analysis between Peptest and HEMII-pH was not significant. Peptest was significantly associated with the number of acid pharyngeal reflux events (rs = 0.182; p = 0.032).
Conclusion
Pepsin saliva measurements appear to be not a reliable diagnostic tool for the detection of GERD in LPR patients. Future studies are needed to determine the place of Peptest in laryngopharyngeal reflux and gastroesophageal reflux diseases.
Similar content being viewed by others

Data availabiity
Data are available on request.
References
Kim SI, Jeong SJ, Kwon OE, Park JM, Doo JG, Park SI, Kim BH, Lee YC, Eun YG, Ko SG (2021) Pharyngeal reflux episodes in patients with suspected laryngopharyngealreflux versus healthy subjects: a prospective cohort study. Eur Arch Otorhinolaryngol 278(9):3387–3392. https://doi.org/10.1007/s00405-021-06865-8
Pizzorni N, Ambrogi F, Eplite A, Rama S, Robotti C, Lechien J, Schindler A (2022) Magnesium alginate versus proton pump inhibitors for the treatment of laryngopharyngeal reflux: a non-inferiority randomized controlled trial. Eur Arch Otorhinolaryngol 279(5):2533–2542. https://doi.org/10.1007/s00405-021-07219-0
Perry KA, Enestvedt CK, Lorenzo CS et al (2008) The integrity of esophagogastric junction anatomy in patients with isolated laryngopharyngeal reflux symptoms. J Gastrointest Surg 12(11):1880–1887
Hoppo T, Sanz AF, Nason KS et al (2012) How much pharyngeal exposure is “normal”? Normative data for laryngopharyngeal reflux events using hypopharyngeal multichannel intraluminal impedance (HMII). J Gastrointest Surg 16:16–24
Lechien JR, Bobin F, Muls V, Eisendrath P, Horoi M, Thill MP, Dequanter D, Durdurez JP, Rodriguez A, Saussez S (2020) Gastroesophageal reflux in laryngopharyngeal reflux patients: Clinical features and therapeutic response. Laryngoscope 130(8):E479–E489. https://doi.org/10.1002/lary.28482
Hirano I (2006) Review article: modern technology in the diagnosis of gastro-oesophageal reflux disease–Bilitec, intraluminal impedance and Bravo capsule pH monitoring. Aliment Pharmacol Ther 23(Suppl 1):12–24. https://doi.org/10.1111/j.1365-2036.2006.02800.x
Calvo-Henríquez C, Ruano-Ravina A, Vaamonde P, Martínez-Capoccioni G, Martín-Martín C (2017) Is pepsin a reliable marker of laryngopharyngeal reflux? A systematic review. Otolaryngol Head Neck Surg 157(3):385–391. https://doi.org/10.1177/0194599817709430
Zeleník K, Hránková V, Vrtková A, Staníková L, Komínek P, Formánek M (2021) Diagnostic value of the Peptest™ in detecting laryngopharyngeal reflux. J Clin Med 10(13):2996. https://doi.org/10.3390/jcm10132996
Lechien JR, Chan WW, Akst LM, Hoppo T, Jobe BA, Chiesa-Estomba CM, Muls V, Bobin F, Saussez S, Carroll TL, Vaezi MF, Bock JM (2022) Normative ambulatory reflux monitoring metrics for laryngopharyngeal reflux: a systematic review of 720 healthy individuals. Otolaryngol Head Neck Surg 166(5):802–819. https://doi.org/10.1177/01945998211029831
Gyawali CP, Kahrilas PJ, Savarino E, Zerbib F, Mion F, Smout AJPM, Vaezi M, Sifrim D, Fox MR, Vela MF, Tutuian R, Tack J, Bredenoord AJ, Pandolfino J, Roman S (2018) Modern diagnosis of GERD: the Lyon Consensus. Gut 67(7):1351–1362. https://doi.org/10.1136/gutjnl-2017-314722
Bobin F, Journe F, Lechien JR (2019) Saliva pepsin level of laryngopharyngeal reflux patients is not correlated with reflux episodes. Laryngoscope. https://doi.org/10.1002/lary.28260
Lechien JR, Bobin F, Rodriguez A, Dequanter D, Muls V, Huet K, Harmegnies B, Crevier-Buchman L, Hans S, Saussez S, Carroll TL (2021) Development and validation of the short version of the reflux symptom score: reflux symptom score-12. Otolaryngol Head Neck Surg 164(1):166–174. https://doi.org/10.1177/0194599820941003
Lechien JR, Bobin F, Muls V et al (2019) Validity and reliability of the reflux sign assessment (RSA). Ann Otol Rhinol Laryngol. https://doi.org/10.1177/0003489419888947
Zhang M, Chia C, Stanley C, Phyland DJ, Paddle PM (2021) Diagnostic utility of salivary pepsin as compared with 24-hour dual pH/impedance probe in laryngopharyngeal reflux. Otolaryngol Head Neck Surg 164(2):375–380. https://doi.org/10.1177/0194599820951183
Wang J, Zhao Y, Ren J, Xu Y (2018) Pepsin in saliva as a diagnostic biomarker in laryngopharyngeal reflux: a meta-analysis. Eur Arch Otorhinolaryngol 275(3):671–678. https://doi.org/10.1007/s00405-017-4845-8
Wang J, Li J, Nie Q, Zhang R (2022) Are multiple tests necessary for salivary pepsin detection in the diagnosis of laryngopharyngeal reflux? Otolaryngol Head Neck Surg 166(3):477–481. https://doi.org/10.1177/01945998211026837
Bobin F, Journe F, Lechien JR (2020) Saliva pepsin level of laryngopharyngeal reflux patients is not correlated with reflux episodes. Laryngoscope 130(5):1278–1281. https://doi.org/10.1002/lary.28260
Fortunato JE, D’Agostino RB Jr, Lively MO (2017) Pepsin in saliva as a biomarker for oropharyngeal reflux compared with 24-hour esophageal impedance/pH monitoring in pediatric patients. Neurogastroenterol Motil. https://doi.org/10.1111/nmo.12936
Haddad HA, He Z, Shaffer SE, Molle-Rios ZL (2020) Salivary pepsin A detection related to gastro-oesophageal reflux episodes in children undergoing impedance probe monitoring. Acta Paediatr 109(11):2374–2379. https://doi.org/10.1111/apa.15276
Lechien JR (2023) Pediatric laryngopharyngeal reflux: an evidence-based review. Children (Basel). https://doi.org/10.3390/children10030583. (In revision)
Yu L, Li R, Du L, Zhao Y (2022) The diagnostic value of pepsin concentration in saliva for laryngopharyngeal reflux disease. Eur Arch Otorhinolaryngol 279(12):5783–5789. https://doi.org/10.1007/s00405-022-07472-x
Lechien JR, Bobin F, Muls V, Horoi M, Thill MP, Dequanter D, Finck C, Rodriguez A, Saussez S (2021) Saliva pepsin concentration of laryngopharyngeal reflux patients is influenced by meals consumed before the samples. Laryngoscope 131(2):350–359. https://doi.org/10.1002/lary.28756
Sasaki CT, Doukas SG, Costa J, Vageli DP (2019) Biliary reflux as a causal factor in hypopharyngeal carcinoma: new clinical evidence and implications. Cancer 125(20):3554–3565. https://doi.org/10.1002/cncr.32369
De Corso E, Baroni S, Salonna G, Marchese M, Graziadio M, Di Cintio G, Paludetti G, Costamagna G, Galli J (2021) Impact of bile acids on the severity of laryngo-pharyngeal reflux. Clin Otolaryngol 46(1):189–195. https://doi.org/10.1111/coa.13643
Sereg-Bahar M, Jerin A, Jansa R, Stabuc B, Hocevar-Boltezar I (2015) Pepsin and bile acids in saliva in patients with laryngopharyngeal reflux—a prospective comparative study. Clin Otolaryngol 40(3):234–239. https://doi.org/10.1111/coa.12358
Aviv JE, Liu H, Parides M, Kaplan ST, Close LG (2000) Laryngopharyngeal sensory deficits in patients with laryngopharyngeal refluxand dysphagia. Ann Otol Rhinol Laryngol 109(11):1000–1006. https://doi.org/10.1177/000348940010901103
Acknowledgements
None.
Funding
Vesale Grant & IRIS-Recherche Grant (Foundation Roi Baudouin). The study is funded by the Groupement de Coopération Sanitaire ELSAN, 58 bis rue de la Boétie, 75008 Paris, France.
Author information
Authors and Affiliations
Contributions
JRL: design, acquisition of data, data analysis and interpretation, drafting, final approval, and accountability for the work; final approval of the version to be published; agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. FB: design, acquisition of data, data analysis and interpretation, drafting, final approval, and accountability for the work; final approval of the version to be published; agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest.
Informed consent
Patients consented to the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lechien, J.R., Bobin, F. Saliva pepsin measurements in the detection of gastroesophageal reflux disease in laryngopharyngeal reflux patients: a cohort study. Eur Arch Otorhinolaryngol 280, 3765–3771 (2023). https://doi.org/10.1007/s00405-023-08000-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-023-08000-1