Abstract
Background
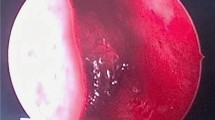
Hemangiopericytoma is a rare tumor of the sino-nasal tract. Its clinical behavior is controversial. Whereas some describe an indolent course, others consider it to be an aggressive lesion with a tendency toward rapid local recurrence. Here, we describe our experience in the management of sino-nasal hemangiopericytoma (SN-HPC), comparing our experience with the current literature, and evaluating signs and tools to improve diagnosis and treatment.
Methods
All cases of SN-HPC between 2010 and 2020 were extracted and reviewed from our institutional electronic medical records. SN-HPC cases from PubMed and EMBASE between 2010 and 2020 were analyzed in a systematic literature review using the preferred reporting items for systematic review and meta-analysis (PRISMA) guidelines. Data regarding demographics, presentation, diagnosis, treatment, and outcome were collected.
Results
We identified four cases of SN-HPC in the nasal cavity in our institution and an additional 53 cases in previous reports. The mean age at the time of diagnosis was 59 years, with a 1.2:1 male to female ratio. SN-HPC mostly appears unilaterally, arising in the ethmoid sinus (42.1%). The most common presenting symptoms were epistaxis (47.3) and nasal obstruction (47.3%). Both computed tomography (CT) and magnetic resonance imaging (MRI) were required for diagnosis and for tailoring the treatment plan. Endoscopic surgical excision was used in 85.9% of the patients, and in 15.7%, an additional preoperative embolization was performed, which was associated with septal necrosis in one patient (2.6%). The recurrence rate was 7%.
Conclusion
Although previous reports attribute an aggressive tumoral behavior to SN-HPC, our experience and the literature review support a more indolent course with low recurrence rates following complete endoscopic resection. Preoperative embolization can be useful in certain cases, but due to potential complications, it should not be routinely indicated.




Similar content being viewed by others
References
Stout AP, Murray MR (1942) Hemagiopericytoma a vascular tumor featuring Zimmermann’s pericytes. Ann Surg 116:26–33. https://doi.org/10.1097/00000658-194207000-00004
Simmonds JC, Rebeiz EE (2017) Surgical resection of sinonasal hemangiopericytoma involving anterior skull base: case reports and literature review. Am J Otolaryngol 38:87–91. https://doi.org/10.1016/j.amjoto.2016.09.003
Lee GG, Dhong H-J, Park Y-S, Ko YH (2014) Sinonasal glomangiopericytoma causing oncogenic osteomalacia. Clin Exp Otorhinolaryngol 7:145. https://doi.org/10.3342/ceo.2014.7.2.145
Kim J, Jeon J, Kim D-H, Park ES, Maeng L-S, Jun S-Y (2016) Glomangiopericytoma and glomus tumor of the sinonasal tract: a report of two cases with emphasis on the differential diagnosis: Glomangiopericytoma and glomus tumor. Pathol Int 66:348–350. https://doi.org/10.1111/pin.12399
Chen Q, Chen X-Z, Wang J-M, Li S-W, Jiang T, Dai J-P (2012) Intracranial meningeal hemangiopericytomas in children and adolescents: CT and MR imaging findings. Am J Neuroradiol 33:195–199. https://doi.org/10.3174/ajnr.A2721
Park ES, Kim J, Jun S-Y (2017) Characteristics and prognosis of glomangiopericytomas: a systematic review. Head Neck 39:1897–1909. https://doi.org/10.1002/hed.24818
Bignami M, Dallan I, Battaglia P, Lenzi R, Pistochini A, Castelnuovo P (2010) Endoscopic, endonasal management of sinonasal haemangiopericytoma: 12-year experience. J Laryngol Otol 124:1178–1182. https://doi.org/10.1017/S0022215110000952
Thompson LDR, Miettinen M, Wenig BM (2003) Sinonasal-type hemangiopericytoma: a clinicopathologic and immunophenotypic analysis of 104 cases showing perivascular myoid differentiation. Am J Surg Pathol 27:737–749. https://doi.org/10.1097/00000478-200306000-00004
Watanabe K, Saito A, Suzuki M, Yamanobe S, Suzuki T (2001) True hemangiopericytoma of the nasal cavity. Arch Pathol Lab Med 125:686–690. https://doi.org/10.5858/2001-125-0686-THOTNC
Mena H, Ribas JL, Pezeshkpour GH, Cowan DN, Parisi JE (1991) Hemangiopericytoma of the central nervous system: a review of 94 cases. Hum Pathol 22:84–91. https://doi.org/10.1016/0046-8177(91)90067-Y
Schiariti M, Goetz P, El-Maghraby H, Tailor J, Kitchen N (2011) Hemangiopericytoma: long-term outcome revisited: clinical article. J Neurosurg 114:747–755. https://doi.org/10.3171/2010.6.JNS091660
Sonabend AM, Zacharia BE, Goldstein H, Bruce SS, Hershman D, Neugut AI, Bruce JN (2014) The role for adjuvant radiotherapy in the treatment of hemangiopericytoma: a surveillance, epidemiology, and end results analysis: clinical article. J Neurosurg 120:300–308. https://doi.org/10.3171/2013.10.JNS13113
Rutkowski MJ, Bloch O, Jian BJ, Chen C, Sughrue ME, Tihan T, Barani IJ, Berger MS, McDermott MW, Parsa AT (2011) Management of recurrent intracranial hemangiopericytoma. J Clin Neurosci 18:1500–1504. https://doi.org/10.1016/j.jocn.2011.04.009
Riley DS, Barber MS, Kienle GS, Aronson JK, von Schoen-Angerer T, Tugwell P, Kiene H, Helfand M, Altman DG, Sox H, Werthmann PG, Moher D, Rison RA, Shamseer L, Koch CA, Sun GH, Hanaway P, Sudak NL, Kaszkin-Bettag M, Carpenter JE, Gagnier JJ (2017) CARE guidelines for case reports: explanation and elaboration document. J Clin Epidemiol 89:218–235. https://doi.org/10.1016/j.jclinepi.2017.04.026
Preferred Reporting Items for Systematic Reviews andMeta-Analyses: The PRISMA Statement - Google Search. https://www.google.com/search?q=Preferred+Reporting+Items+for+Systematic+Reviews+andMeta-Analyses%3A+The+PRISMA+Statement&oq=Preferred+Reporting+Items+for+Systematic+Reviews+andMeta-Analyses%3A+The+PRISMA+Statement&aqs=chrome..69i57.723j0j7&sourceid=chrome&ie=UTF-8. Accessed 22 Feb 2021
Duval M, Hwang E, Kilty SJ (2013) Systematic review of treatment and prognosis of sinonasal hemangiopericytoma. Head Neck 35(8):1205–10. https://doi.org/10.1002/hed.23074. Epub 2012 Jun 25.
Dandekar M, McHugh JB (2010) Sinonasal glomangiopericytoma: case report with emphasis on the differential diagnosis. Arch Pathol Lab Med 134(10):1444–1449. https://doi.org/10.5858/2010-0233-CR
Higashi K, Nakaya K, Watanabe M et al (2011) Glomangiopericytoma of the nasal cavity. Auris Nasus Larynx 38(3):415–417. https://doi.org/10.1016/j.anl.2010.08.009 (Epub 2010 Nov 19)
Yokoi H, Arakawa A, Kuribayashi K, Inoshita A, Haruyama T, Ikeda K (2011) An immunohistochemical study of sinonasal hemangiopericytoma. Auris Nasus Larynx 38(6):743–746. https://doi.org/10.1016/j.anl.2011.04.009
Sazgar AA, Ghazizadeh M (2011) Endoscopic transnasal resection of sinonasal haemangiopericytoma involving anterior skull base: a case report and literature review. B-ENT 7(3):205–208
Pfammatter A, Brändle P, Hürlimann S, Schlegel-Wagner C (2012) Sinonasal hemangiopericytoma in the columellar base, an unusual location. Otolaryngol Neck Surg 146(4):682–683. https://doi.org/10.1177/0194599811421751
Arpaci RB, Kara T, Vayisoğlu Y, Ozgur A, Ozcan C (2012) Sinonasal glomangiopericytoma. J Craniofac Surg 23(4):1194–1196. https://doi.org/10.1097/SCS.0b013e31824e6d09
Terada T, Kato T (2012) Sinonasal-type hemangiopericytoma of the nasal cavity and paranasal sinus. Int J Clin Oncol 17(2):169–173. https://doi.org/10.1007/s10147-011-0263-x
Jung ES, Yang S-W, Kim J-H, Kim SW (2013) A case of glomangiopericytoma involving the orbital wall. Ear Nose Throat J 92(4):E13–E15. https://doi.org/10.1177/014556131309200422
Ledderose GJ, Gellrich D, Holtmannspötter M, Leunig A (2013) Endoscopic resection of sinonasal hemangiopericytoma following preoperative embolisation: a case report and literature review. Case Rep Otolaryngol 2013:1–7. https://doi.org/10.1155/2013/796713
Lee GG, Dhong H-J, Park Y-S, Ko YH (2014) Sinonasal glomangiopericytoma causing oncogenic osteomalacia. Clin Exp Otorhinolaryngol 7(2):145. https://doi.org/10.3342/ceo.2014.7.2.145
Roy N, Desai D, Jain S (2015) Glomangiopericytoma of nasal cavity. Indian J Pathol Microbiol 58(4):554. https://doi.org/10.4103/0377-4929.168864
Ray S, Chakraborty PP, Biswas K, Ghosh S, Mukhopadhyay S, Chowdhury S (2015) A case of oncogenic osteomalacia due to occult nasal sinus tumor. Clin Cases Miner Bone Metab Jan-Apr 12(1):65–68. https://doi.org/10.11138/ccmbm/2015.12.1.065
Shobha B, Shivakumar B, Reddy S, Dutta N (2015) Sinonasal hemangiopericytoma: a rare case report with review of literature. J Oral Maxillofac Pathol 19(1):107. https://doi.org/10.4103/0973-029X.157214
Handra-Luca A, Abd Elmageed ZY, Magkou C, Lae M (2015) Immunophenotype heterogeneity in nasal glomangiopericytoma. Case Rep Otolaryngol 2015:1–3. https://doi.org/10.1155/2015/308743
Asimakopoulos P, Syed MI, Andrews T, Syed S, Williams A (2016) Sinonasal glomangiopericytoma: is anything new? Ear Nose Throat J 95(2):E1–E6. https://doi.org/10.1177/014556131609500202
Psoma E, Karkos PD, Dova S et al (2016) Sinonasal glomangiopericytoma treated with preoperative embolisation and endoscopic sinus surgery. Cancer Med Sci 10:192. https://doi.org/10.3332/ecancer.2016.692
Simmonds JC, Rebeiz EE (2017) Surgical resection of sinonasal hemangiopericytoma involving anterior skull base: case reports and literature review. Am J Otolaryngol 38(1):87–91. https://doi.org/10.1016/j.amjoto.2016.09.003
Kassaby S, Patterson E (2018) Sinonasal glomangiopericytoma: a case report of an unusual neoplasm with emphasis on the differential diagnosis. Am J Clin Pathol 149(suppl_1):S110. https://doi.org/10.1093/ajcp/aqx123.258
Chang C-J, Sun C-H, Chen T-S, Wu H-P (2018) Navigation-assisted endoscopic endonasal surgery of a glomangiopericytoma with intraorbital extension: a case report and literature review. Tzu Chi Med J 30(2):119. https://doi.org/10.4103/tcmj.tcmj_161_17
Eid M, Elgabry W, Fawzy T, Wageh W (2018) Endoscopic management of true hemangiopericytoma arising from the nasal septum: case study and literature review. S-0038–1640833. https://doi.org/10.1055/s-0038-1640833
Muranjan S, Bommakanti VJ, Shah N (2018) Coblator assisted resection of sinonasal Hemangiopericytoma-a case report. Otolaryngol Case Rep 9:15–17. https://doi.org/10.1016/j.xocr.2018.10.001
Anzai T, Saito T, Tsuyama S, Toh M, Ikeda K, Ito S (2018) A case of glomangiopericytoma at the nasal septum. Head Neck Pathol 12(4):572–575. https://doi.org/10.1007/s12105-017-0870-6
Li J, Huang Y, Yang F, Zhang Q, Chen D, Wang Q (2018) Sinonasal hemangiopericytoma caused hypophosphatemic osteomalacia: a case report. Medicine (Baltimore) 97(52):e13849. https://doi.org/10.1097/MD.0000000000013849
Abdulsattar J, AlZubaidi Y, Lozano G, Al-Delfi F (2018) 140 Sinonasal glomangiopericytoma: a diagnostic challenge. Am J Clin Pathol 149(suppl_1):S60. https://doi.org/10.1093/ajcp/aqx119.139
Sheikh S, Sarwar F, Khan NU, Khan MS (2018) Endonasal endoscopic laser-assisted resection of septal glomangiopericytoma. BMJ Case Rep 2018:bcr-2017–223752. https://doi.org/10.1136/bcr-2017-223752
Sharma N, Mandlik D, Patel P et al (2019) A rare case of sinonasal glomangiopericytoma post operative accidental diagnosis and managment—A case report. Int J Surg Case Rep 62:54–57. https://doi.org/10.1016/j.ijscr.2019.06.066
Min HJ, Kim KS (2019) Sinonasal glomangiopericytoma: a case report and literature review. Bangladesh J Med Sci 18(3):651–655. https://doi.org/10.3329/bjms.v18i3.41644
Saito Y, Ohta N, Konosu-fukaya S et al (2019) Endoscopic treatment of sinonasal glomangiopericytoma: a case report in light of the literature. Yonago Acta Med 62(2):236–239. https://doi.org/10.33160/yam.2019.06.009
Ciceri EF, Plebani M, Augelli R et al (2019) Transnasal devascularisation of a sinonasal hypervascular tumour (glomangiopericytoma) with direct injection of liquid polymer agent (Squid®). Interv Neuroradiol 25(2):230–233. https://doi.org/10.1177/1591019918805776
Kono M, Bandoh N, Matsuoka R et al (2019) Glomangiopericytoma of the nasal cavity with CTNNB1 p.S37C mutation: a case report and literature review. Head Neck Pathol 13(3):298–303. https://doi.org/10.1007/s12105-018-0961-z
Ameya SK, Asarkar A (2019) (2019) Giant Hemangiopericytoma: evaluation and Treatment. Otolaryngol Neck Surg 161(2S):203. https://doi.org/10.2321/ons.2019.04.15
Obeidin F, Jennings LJ, Alexiev BA (2019) Sinonasal glomangiopericytoma: a clinicopathologic study. Pathol Res Pract 215(5):983–987. https://doi.org/10.1016/j.prp.2019.02.004
Suh CH, Lee JH, Lee MK et al (2020) CT and MRI findings of glomangiopericytoma in the head and neck: case series study and systematic review. Am J Neuroradiol 41(1):155–159. https://doi.org/10.3174/ajnr.A6336
Gomez-Rivera F, Fakhri S, Williams MD, Hanna EY, Kupferman ME (2012) Surgical management of sinonasal hemangiopericytomas: a case series. Head Neck 34:1492–1496. https://doi.org/10.1002/hed.21926
Ye L, Zhou X, Li J, Jin J (2011) Coblation-assisted endonasal endoscopic resection of juvenile nasopharyngeal angiofibroma. J Laryngol Otol 125:940–944. https://doi.org/10.1017/S0022215111001344
Cannon DE, Poetker DM, Loehrl TA, Chun RH (2013) Use of coblation in resection of juvenile nasopharyngeal angiofibroma. Ann Otol Rhinol Laryngol 122:353–357. https://doi.org/10.1177/000348941312200601
Bhattacharyya N, Shapiro NL, Metson R (1997) Endoscopic resection of a recurrent sinonasal hemangiopericytoma. Am J Otolaryngol 18:341–344. https://doi.org/10.1016/S0196-0709(97)90031-4
Fletcher CDM, McKEE PH (1985) Sarcomas-a clinicopathological guide with particular reference to cutaneous manifestation III. Angiosarcoma, malignant haemangiopericytoma, fibrosarcoma and synovial sarcoma. Clin Exp Dermatol 10:332–349. https://doi.org/10.1111/j.1365-2230.1985.tb00580.x
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Warman, M., Syn-Hershko, A., Cohen, O. et al. Sino-nasal hemangiopericytoma: a case series and systematic literature review. Eur Arch Otorhinolaryngol 279, 3989–3996 (2022). https://doi.org/10.1007/s00405-021-07239-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-021-07239-w