Abstract
Objective
Postoperative comfort of the patients undergoing rhinoplasty might be poor because of edema and ecchymosis caused by lateral osteotomy. In this animal experiment, we aimed at performing a quantitative assessment of effects of hyaluronic acid usage on healing process of lateral osteotomy.
Methods
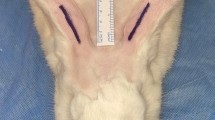
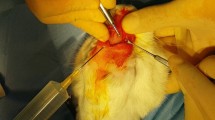
Fourteen New Zealand rabbits with a weight of 2000–2500 kg and an age of 8–12 weeks were included. Under anesthesia, nasal dorsums were exposed with midline incision and lateral osteotomies on both sides were performed using a 2 mm chisel. A hyaluronic acid-based mesh (Hyalonect®) (1 × 1 cm) was embedded on the left osteotomy areas of all rabbits. Right osteotomy areas were left blank as control group. Collagen density and capillary development were quantitatively compared.
Results
Convergence of fracture lines was observed in 6 (60%) of 10 samples from Hyalonect® group, while was observed in 4 (40%) of 10 samples from control group. Although a higher rate of convergence was seen in the Hyalonect® group (60% vs 40%), the difference was not statistically significant (p = 0.5). Median collagen score was 2 (1–3) in the Hyalonect® group and 1 (1–2) in the control group. Median capillary count value was 4 (1–23) in the Hyalonect® group and 3 (1–17) in the control group. Both collagen score and capillary count values were significantly greater in the in the Hyalonect® group compared with the control group (p = 0.023 and p = 0.019, respectively).
Conclusion
The effects of hyaluronic acid-based meshes on the bone healing process of the lateral osteotomy area might be investigated furthermore, on more comprehensive studies, as a material facilitating collagen organization and capillary development.





Similar content being viewed by others
References
Bektas G, Cinpolat A, Rizvanovic Z (2020) Nasal filling in plastic surgery practice: primary nasal filling, nasal filling for post-rhinoplasty defects, rhinoplasty after hyaluronidase injection in dissatisfied nasal filling patients. Aesthetic Plast Surg 44(6):2208–2218. https://doi.org/10.1007/s00266-020-01895-9
Bertossi D, Malchiodi L, Albanese M, Nocini R, Nocini P (2020) Nonsurgical rhinoplasty with the novel hyaluronic acid filler VYC-25L: results using a nasal grid approach. Aesthet Surg J. https://doi.org/10.1093/asj/sjaa196
Kassir R, Venkataram A, Malek A, Rao D (2020) Non-surgical rhinoplasty: the ascending technique and a 14-year retrospective study of 2130 cases. Aesthetic Plast Surg. https://doi.org/10.1007/s00266-020-02048-8
Rho NK, Youn CS, Youn SJ, Lee S, Kim HS (2021) A comparison of the safety, efficacy, and longevity of two different hyaluronic acid fillers in filler rhinoplasty: a multicenter study. Dermatol Ther 34(1):e14707. https://doi.org/10.1111/dth.14707
Bian X, Liu H, Sun J, Zhang X, Li N, Chen M (2020) Efficacy of dexamethasone for reducing edema and ecchymosis after rhinoplasty: a systematic review and meta-analysis. Aesthetic Plast Surg 44(5):1672–1684. https://doi.org/10.1007/s00266-020-01743-w
Hanci D, Üstün O, Yılmazer AB, Göker AE, Karaketir S, Uyar Y (2020) Evaluation of the efficacy of hilotherapy for postoperative edema, ecchymosis, and pain after rhinoplasty. J Oral Maxillofac Surg 78(9):1628.e1621-1628.e1625. https://doi.org/10.1016/j.joms.2020.03.032
Karimi S, Sadeghi M, Amali A, Saedi B (2020) Effect of photobiomodulation on ecchymosis after rhinoplasty: a randomized single-blind controlled trial. Aesthetic Plast Surg 44(5):1685–1691. https://doi.org/10.1007/s00266-020-01760-9
Rostami K, Shahaboddin MA, Niazi F, Karimi Rouzbahani A, Nadri S, Mahmoudvand H (2020) The effect of hirodoid cream on ecchymosis and edema around eyes after rhinoplasty. World J Plast Surg 9(2):128–134. https://doi.org/10.29252/wjps.9.2.128
Tandelilin RT, Sofro ASM, Soesatyo MH, Asmara W (2006) The density of collagen fiber in alveolus mandibular bone of rabbit after augmentation with powder demineralized bone matrix post incisivus extraction. Dent J 39(2):43–47. https://doi.org/10.20473/j.djmkg.v39.i2.p43-47
Locketz GD, Lozada KN, Becker DG (2020) Osteotomies—when, why, and how? Facial Plast Surg 36(1):57–65. https://doi.org/10.1055/s-0040-1701478
Chen WY, Abatangelo G (1999) Functions of hyaluronan in wound repair. Wound Repair Regen 7(2):79–89. https://doi.org/10.1046/j.1524-475x.1999.00079.x
Saliba I, Alzahrani M, Zhu T, Chemtob S (2014) Growth factors expression in hyaluronic acid fat graft myringoplasty. Laryngoscope 124(6):E224-230. https://doi.org/10.1002/lary.24468
Güneri EA, Tekin S, Yilmaz O, Ozkara E, Erdağ TK, Ikiz AO, Sarioğlu S, Güneri A (2003) The effects of hyaluronic acid, epidermal growth factor, and mitomycin in an experimental model of acute traumatic tympanic membrane perforation. Otol Neurotol 24(3):371–376. https://doi.org/10.1097/00129492-200305000-00004
Dessy LA, Mazzocchi M, Rizzo MI, Onesti MG, Scuderi G (2013) Scalp reconstruction using dermal induction template: state of the art and personal experience. In Vivo 27(1):153–158
Jang CH, Park H, Cho YB, Choi CH (2008) The effect of anti-adhesive packing agents in the middle ear of guinea pig. Int J Pediatr Otorhinolaryngol 72(11):1603–1608. https://doi.org/10.1016/j.ijporl.2008.07.012
Simman R, Mari W, Younes S, Wilson M (2018) Use of hyaluronic acid-based biological bilaminar matrix in wound bed preparation: a case series. Eplasty 18:e17
Chareancholvanich K, Pornrattanamaneewong C, Narkbunnam R (2014) Increased cartilage volume after injection of hyaluronic acid in osteoarthritis knee patients who underwent high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 22(6):1415–1423. https://doi.org/10.1007/s00167-013-2735-1
Otsuki S, Nakajima M, Lotz M, Kinoshita M (2008) Hyaluronic acid and chondroitin sulfate content of osteoarthritic human knee cartilage: site-specific correlation with weight-bearing force based on femorotibial angle measurement. J Orthop Res 26(9):1194–1198. https://doi.org/10.1002/jor.20571
Funding
This project was funded by the Scientific Research Project Unit of Giresun University.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest to declare.
Ethical approval
All procedures performed in this study were in accordance with the ethical standards of local ethical committee of Giresun University for animal experiments (Number: 2017/18).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yildirim, G., Ozcan, K.M., Erisgin, Z. et al. Effects of hyaluronic acid on the bone healing after lateral osteotomy: an experimental animal model. Eur Arch Otorhinolaryngol 279, 2959–2964 (2022). https://doi.org/10.1007/s00405-021-07096-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-021-07096-7