Abstract
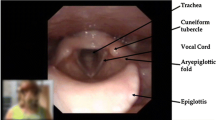
A method for combined ergo-spirometry and continuous laryngeal inspection during exercise, entitled continuous laryngoscopy exercise test (CLE-test) has been developed in order to study airway obstruction at the laryngeal level during exercise. The aim of the study was to apply the CLE-test on patients experiencing respiratory distress during exercise in order to reveal the usefulness of the CLE-test both as a diagnostic tool in the selection of patients for surgery and in evaluation of treatment effects postoperatively. Until now, 81 patients with a history of exercise-induced stridor have undergone the CLE-test. Ten of these patients were selected for surgical treatment based on the severity of symptoms and their motivation for treatment. All ten patients underwent endoscopic supraglottoplasty (ES), with laser incision in both aryepiglottic folds anterior to the cuneiform cartilages and removal of the mucosa around the top of the tubercles. Each patient was examined by the CLE-test before and 3 months after surgery. Eight patients felt subjectively that their breathing capacity during exercise was improved. When pre- and postoperative ergo-spirometry evaluations were compared, increased peak oxygen consumption was observed in four out of ten patients and better maximal minute ventilation in seven out of ten. Postoperative evaluation of the laryngeal images showed less prominent aryepiglottic folds. The typical adduction of the supraglottic structures concomitant with inspiratory stridor found preoperatively was not present in any of the patients during exercise postoperatively. The ES procedure is an efficient surgical treatment for exercise-induced laryngeal supraglottic obstruction and the CLE-test eases the selection of patients for surgery and facilitates the evaluation of treatment effects.



Similar content being viewed by others
References
Beaty MM, Wilson JS, Smith RJH (1999) Laryngeal motion during exercise. Laryngoscope 109:136–139
Bent JP 3rd, Miller DA, Kim JW, Bauman NM, Wilson JS, Smith RJH (1996) Pediatric exercise-induced laryngomalacia. Ann Otol Rhinol Laryngol 105:169–175
Bittleman DB, Smith RJH, Weiler JM (1994) Abnormal movement of the arytenoid region during exercise presenting as exercise-induced asthma in an adolescent athlete. Chest 106:615–616
Bjornsdottir US, Gudmundsson K, Hjartarson H, Brondbo K, Magnusson B, Juliusson S (2000) Exercise-induced laryngochalasia: an imitator of exercise-induced bronchospasm. Ann Allergy Asthma Immunol 85:387–391
Bucca C, Rolla G, Brussino L, De Rose V, Bugiani M (1995) Are asthma-like symptoms due to bronchial or extrathoracic airway dysfunction? Lancet 346:791–795
Cumming GR, Everatt D, Hastman L (1978) Bruce treadmill test in children: normal values in a clinic population. Am J Cardiol 41:69–75
Fahey JT, Bryant NJ, Karas D, Goldberg B, Destefano R, Gracco LC (2005) Exercise-induced stridor due to abnormal movement of the arytenoid area: videoendoscopic diagnosis and characterization of the “at risk” group. Pediatr Pulmonol 39:51–55
Gessler EM, Simko EJ, Greinwald JH Jr (2002) Adult laryngomalacia: an uncommon clinical entity. Am J Otolaryngol 23:386–389
Goldman J (1997) All that wheezes is not asthma. Practitioner 241:35–38
Heimdal JH, Roksund OD, Halvorsen T, Skadberg BT, Olofsson J (2006) Continuous laryngoscopy exercise test: a method for visualizing laryngeal dysfunction during exercise. Laryngoscope 116:52–57
Holinger LD, Konior RJ (1989) Surgical management of severe laryngomalacia. Laryngoscope 99:136–142
Kayani S, Shannon DC (1998) Vocal cord dysfunction associated with exercise in adolescent girls. Chest 113:540–542
Lakin RC, Metzger WJ, Haughey BH (1984) Upper airway obstruction presenting as exercise-induced asthma. Chest 86:499–501
Mandell DL, Arjmand EM (2003) Laryngomalacia induced by exercise in a pediatric patient. Int J Pediatr Otorhinolaryngol 67:999–1003
Maschka DA, Bauman NM, McCray PB Jr, Hoffman HT, Karnell MP, Smith RJH (1997) A classification scheme for paradoxical vocal cord motion. Laryngoscope 107:1429–1435
Olney DR, Greinwald JH Jr, Smith RJH, Bauman NM (1999) Laryngomalacia and its treatment. Laryngoscope 109:1770–1775
Powell DM, Karanfilov BI, Beechler KB, Treole K, Trudeau MD, Forrest LA (2000) Paradoxical vocal cord dysfunction in juveniles. Arch Otolaryngol Head Neck Surg 126:29–34
Ruddy BH, Davenport P, Baylor J, Lehman J, Baker S, Sapienza C (2004) Inspiratory muscle strength training with behavioural therapy in a case of a rower with presumed exercise-induced paradoxical vocal-fold dysfunction. Int J Pediatr Otorhinolaryngol 68:1327–1332
Rundell KW, Spiering BA (2003) Inspiratory stridor in elite athletes. Chest 123:468–474
Seear M, Wensley D, West N (2005) How accurate is the diagnosis of exercise induced asthma among Vancouver schoolchildren? Arch Dis Child 90:898–902
Smith RJH, Bauman NM, Bent JP, Kramer M, Smits WL, Ahrens RC (1995) Exercise-induced laryngomalacia. Ann Otol Rhinol Laryngol 104:537–541
Sullivan MD, Heywood BM, Beukelman DR (2001) A treatment for vocal cord dysfunction in female athletes: an outcome study. Laryngoscope 111:1751–1755
Treole K, Trudeau MD, Forrest LA (1999) Endoscopic and stroboscopic description of adults with paradoxical vocal fold dysfunction. J Voice 13:143–152
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Maat, R.C., Roksund, O.D., Olofsson, J. et al. Surgical treatment of exercise-induced laryngeal dysfunction. Eur Arch Otorhinolaryngol 264, 401–407 (2007). https://doi.org/10.1007/s00405-006-0216-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-006-0216-6