Abstract
Purpose
Groin sentinel lymph node (SLN) identification and removal has become a standard of care for women with clinical early stage vulval cancer. There is evidence to support safe detection of the SLN with minimal morbidity. The purpose of this study is to report our experience of managing patients focusing on patient selection, adverse events, quality assurance of the procedure and any benefits and/or disadvantages to patients.
Methods
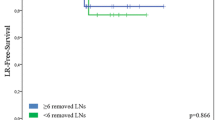
This was a retrospective study of patients with clinical early stage vulval cancer in a cancer centre over 5 years. Notes and hospital data were reviewed including admissions to emergency departments. Statistical software was used for the statistical analysis and the Kaplan Meier survival curve was generated to present survival rates.
Results
61 cases were analysed. A total of 156 nodes have been removed and positive nodes were identified in 14 cases. In total, 9 women (14.75%) had disease recurrence within 5 years from primary surgery. Overall, 4 patients (6.5%) developed groin recurrence. In 3 of these patients there was isolated groin recurrence (4.9%). The median length of admission was 3 days and 6 cases were managed as day cases.
Conclusions
Since the closure of the GROINNS-2 trial we have continued the procedure of SLN identification for women with clinical early stage vulval cancer. We have shown high level of adherence to our protocol and survival and complication rates comparable to other studies on the same field. There were a few patients managed as day-case which was of benefit to the patients.


Similar content being viewed by others
Data availability
We confirm that the dataset is available to be shared if requested to do so.
Abbreviations
- BMI:
-
Body mass index
- DSS:
-
Disease-specific survival
- FU:
-
Follow-up
- GROINNS V:
-
GROningen INternational Study on Sentinel nodes in Vulvar cancer
- IFL:
-
Inguinofemoral lymphadenectomy
- Mm:
-
Millimetres
- MDT:
-
Multidisciplinary team
- OS:
-
Overall survival
- patient no:
-
Patient number
- post-op:
-
Post-operative
- SLN:
-
Sentinel lymph node
- SPSS:
-
Statistical Package for the Social Sciences
- VIN:
-
Vaginal intra-epithelial neoplasia
References
Burger MPM, Hollema H, Emanuels AG, Krans M, Pras E, Bouma J (1995) The importance of the groin node status for the survival of T1 and T2 vulval carcinoma patients. Gynecol Oncol 57(3):327–334. https://doi.org/10.1006/gyno.1995.1151
Oonk MHM, Slomovitz B, Baldwin PJW, van Doorn HC, van der Velden J, de Hullu JA et al (2021) Radiotherapy versus inguinofemoral lymphadenectomy as treatment for vulvar cancer patients with micrometastases in the sentinel node: results of GROINSS-V II. J Clin Oncol 39(32):3623–3632. https://doi.org/10.1200/JCO.21.00006
Van der Zee AGJ, Oonk MH, De Hullu JA, Ansink AC, Vergote I, Verheijen RH et al (2008) Sentinel node dissection is safe in the treatment of early-stage vulvar cancer. J Clin Oncol 26(6):884–889. https://doi.org/10.1200/JCO.2007.14.0566
Zach D, Åvall-Lundqvist E, Falconer H, Hellman K, Johansson H, Flöter RA (2021) Patterns of recurrence and survival in vulvar cancer: a nationwide population-based study. Gynecol Oncol 161(3):748–754. https://doi.org/10.1016/j.ygyno.2021.03.013
Froeding LP, Høgdall C, Kristensen E, Zobbe V, Niemann I, Ørtoft G et al (2020) Recurrence and survival rates in node negative patients after sentinel node biopsy for early-stage vulva cancer—a nationwide study. Gynecol Oncol 156(1):124–130. https://doi.org/10.1016/j.ygyno.2019.10.024
Levenback CF, Ali S, Coleman RL, Gold MA, Fowler JM, Judson PL et al (2012) Lymphatic mapping and sentinel lymph node biopsy in women with squamous cell carcinoma of the vulva: a gynecologic oncology group study. J Clin Oncol 30(31):3786–3791. https://doi.org/10.1200/JCO.2011.41.2528
Mahner S, Jueckstock J, Hilpert F, Neuser P, Harter P, de Gregorio N et al (2015) Adjuvant therapy in lymph node-positive vulvar cancer: the AGO-CaRE-1 study. J Natl Cancer Inst 107(3):dju426. https://doi.org/10.1093/jnci/dju426
Morrison J, Baldwin P, Buckley L, Cogswell L, Edey K, Faruqi A et al (2020) British Gynaecological Cancer Society (BGCS) vulval cancer guidelines: Recommendations for practice. Eur J Obstet Gynecol Reprod Biol 252:502–525
Oonk MHM, Planchamp F, Baldwin P, Bidzinski M, Brännström M, Landoni F et al (2017) European Society of Gynaecological Oncology Guidelines for the management of patients with vulvar cancer. Int J Gynecol Cancer 27(4):832–837
Mokhtech M, Gao SJ, Kassick M, Menderes G, Damast S (2022) Declining use of inguinofemoral lymphadenectomy in the treatment of clinically negative, pathologic node positive vulvar cancer. Gynecol Oncol 166(1):61–68. https://doi.org/10.1016/j.ygyno.2022.05.001
Gitas G, Proppe L, Baum S, Kruggel M, Rody A, Tsolakidis D et al (2021) A risk factor analysis of complications after surgery for vulvar cancer. Arch Gynecol Obstet 304(2):511–519. https://doi.org/10.1007/s00404-020-05949-w
Goker A, Guvenal T, Yanikkerem E, Turhan A, Koyuncu FM (2011) Quality of life in women with gynecologic cancer in Turkey. Asian Pac J Cancer Prev APJCP 12(11):3121–3128
Rahm C, Adok C, Dahm-Kähler P, Bohlin KS (2022) Complications and risk factors in vulvar cancer surgery—a population-based study. Eur J Surg Oncol 48(6):1400–1406. https://doi.org/10.1016/j.ejso.2022.02.006
Wills A, Obermair A (2013) A review of complications associated with the surgical treatment of vulvar cancer. Gynecol Oncol 131(2):467–479. https://doi.org/10.1016/j.ygyno.2013.07.082
Mullen MM, Merfeld EC, Palisoul ML, Massad LS, Woolfolk C, Powell MA et al (2019) Wound complication rates after vulvar excisions for premalignant lesions. Obstet Gynecol 133(4):658–665. https://doi.org/10.1097/AOG.0000000000003185
Cham S, Chen L, Burke WM, Hou JY, Tergas AI, Hu JC et al (2016) Utilization and outcomes of sentinel lymph node biopsy for vulvar cancer. Obstet Gynecol 128(4):754–760. https://doi.org/10.1097/AOG.0000000000001648
Klapdor R, Hertel H, Soergel P, Hillemanns P (2017) Groin recurrences in node negative vulvar cancer patients after sole sentinel lymph node dissection. Int J Gynecol Cancer 27(1):166–170. https://doi.org/10.1097/IGC.0000000000000860
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
EK: project development, Data collection, Data analysis, Manuscript writing. AJ: project development, Data collection. ZZO: project development, Data collection. RO: project development. DN: project development, manuscript editing. KG: project development, manuscript editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethics approval
This was a retrospective anonymised data collection; therefore, no ethic approval is required.
Consent to publish
No individual photographs or data are published in this study; therefore, consent to publish was not needed.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Katsanevakis, E., Joshi, A., Ong, Z.Z. et al. A study of recurrence, complication and survival rates in patients with early stage vulval cancer undergoing sentinel lymph node sampling: a single-centre experience. Arch Gynecol Obstet 308, 561–567 (2023). https://doi.org/10.1007/s00404-023-06968-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-023-06968-z