Abstract
Purpose
The mode of delivery depends on multiple parameters. After assisted reproductive technology (ART), previous studies have shown elevated C-section rates but few studies differentiated between elective and emergency operations and different protocols of cryopreservation. Because these studies did not use multiparity as exclusion criteria which reduces confounding with previous pregnancies, aim of this study is to compare mode of delivery of different techniques of ART using data of primiparae only [1, 2].
Methods
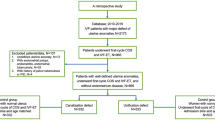
Retrospective analysis of patient data treated at the university hospital of Luebeck in a period of 12 years. Patients were divided in different groups according to their way of conception: spontaneous conception and conception after ART. The group of ART was further divided into: (a) a group of fresh transferred embryos (IVF/ICSI), (b) vitrification and (c) slow freezing. Exclusion criteria were defined as: multiparity, delivery <24. + 0 p.m., incomplete data and treatment outside university of Luebeck. Main parameter of this study was mode of delivery which was divided into spontaneous delivery or C-section. C-sections were further differentiated into elective or emergency C-sections.
Results
The group of fresh transferred embryos and slow freezing showed higher risks for elective and emergency C-sections (elective C-sections odds ratio 2.0, CI 95% 1.6–2.6, emergency C-sections odds ratio 1.4, CI 95% 1.1–1.9). Moreover, all groups of ART show enhanced risk of significant perinatal bleeding.
Conclusion
Patients after ART treatment suffer from higher C-section rates during their stage of delivery.

Similar content being viewed by others
References
Maheshwari A, Pandey S, Shetty A, Hamilton M, Bhattacharya S (2012) Obstetric and perinatal outcomes in singleton pregnancies resulting from the transfer of frozen thawed versus fresh embryos generated through in vitro fertilization treatment: a systematic review and meta-analysis. Fertil Steril 98(2):368–377
Pandey S, Shetty A, Hamilton M, Bhattacharya S, Maheshwari A (2012) Obstetric and perinatal outcomes in singleton pregnancies resulting from IVF/ICSI: a systematic review and meta-analysis. Hum Reprod Update 18(5):485–503
Bohlmann MK, Luedders DW, Beyer D, Kavallaris A, Baumann K, Diedrich K, Hornemann A (2010) Nulliparous patients with small stature delivering at term have an increased risk of secondary cesarean section. Arch Gynecol Obstet 282(3):241–244. doi:10.1007/s00404-009-1216-8 (Epub 2009 Aug 28)
Dhont M, De Sutter P, Ruyssinck G, Martens G, Bekaert A (1999) Perinatal outcome of pregnancies after assisted reproduction: a case–control study. Obstet Gynecol 181:688–695
Pelkonen S, Koivunen R, Gissler M, Nuojua-Huttunen S, Suikkari A, Hyden- Granskog C et al (2010) Perinatal outcome of children born after frozen and fresh embryo transfer: the finnish cohort study 1995–2006. Hum Reprod 25:914–923
McMahon CA, Ungerer JA, Beaurepaire J, Tennant C, Saunders D (1997) Anxiety during pregnancy and fetal attachment after in vitro fertilization conception. Hum Reprod 12:176–182
Sazonova A, Kllen K, Thurin-Kjellberg A, Wennerholm UB, Bergh C (2011) Factors affecting obstetric outcome of singletons born after IVF. Hum Reprod 26:2878–2886
Healy DL, Breheny S, Halliday J, Jaques A, Rushford D, Garrett C et al (2010) Prevalence and risk factors for obstetric haemorrhage in 6730 singleton births after assisted reproductive technology in Victoria, Australia. Hum Reprod 25:265–274
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Conflict of interest
There are no conflicts of interest for any of the authors.
Rights and permissions
About this article
Cite this article
Neumann, K., Cirkel, C., Rody, A. et al. Do ART patients face higher C-section rates during their stage of delivery? A German monocenter experience. Arch Gynecol Obstet 295, 481–485 (2017). https://doi.org/10.1007/s00404-016-4252-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-016-4252-1