Absract
Purpose
The primary aim of our study was to evaluate mesh movement on ultrasonography and to compare the relationship between suburethral mesh angle and incontinence recurrence.
Methods
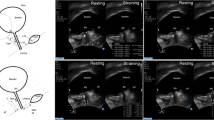
This study was carried out at the University of Selcuk, Konya, Turkey, Beyhekim State Hospital, Konya, Turkey and the Mus State Hospital between September 2012 and January 2015. In total, the results from 109 patients were evaluated in the statistical analysis. The suburethral mesh angle (SMA) is the angle between the two arms of the trans-obturator tape (TOT) mesh under the urethra. This angle was measured at 10 days, 6 months and 1 year after surgery. Potential risk factors for incontinence recurrence and SMA were compared in logistic regression models. The best cut-off value for SMA was calculated to predict incontinence recurrence.
Results
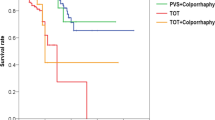
The mean resting SMA did not change with time during follow-up (p = 0.373). However, when comparing coughing SMA values, the first day measurement was significantly different from the other measurements. Another comparison was performed according to the cSMA value at each visit. The difference was significant from the first day. Lung disease and the change in the SMA (cSMA) on day 10 were significant predictors of treatment failure. The cSMA on day 10 to predict first-year treatment failure was 10°, with 61% sensitivity and 96% specificity.
Conclusions
Measurement of the SMA can be used as a prognostic factor in TOT surgery. Further research is required to determine the importance of SMA as a prognostic factor.


Similar content being viewed by others
References
Haylen BT, de Ridder D, Freeman RM, Swift SE, Berghmans B, Lee J et al (2010) An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. Neurourol Urodyn 29:4
Luber KM (2004) The definition, prevalence, and risk factors for stress urinary incontinence. Rev Urol 6(Suppl 3):S3
Hunskaar S, Lose G, Sykes D et al (2004) The prevalence of urinary incontinence in women in four European countries. BJU Int 93:324–330
Lawrence JM, Lukacz ES, Liu ILA, Nager CW, Luber KM (2007) Pelvic floor disorders, diabetes, and obesity in women findings from the kaiser permanente continence associated risk epidemiology study. Diabetes Care 30(10):2536–3541
Matthews CA, Whitehead WE, Townsend MK, Grodstein F (2013) Risk factors for urinary, fecal or dual incontinence in the nurses’ health study. Obstet Gynecol 122(3):539
Lukacz ES, Lawrence JM, Contreras R, Nager CW, Luber KM (2006) Parity, mode of delivery, and pelvic floor disorders. Obstet Gynecol 107(6):1253–1260
Delorme E (2001) Transobturator urethral suspension: mini-invasive procedure in the treatment of stress urinary incontinence in women. Progres en urologie journal de l’Association francaise d’urologie et de la Societe francaise d’urologie 11(6):1306–1313
Schierlitz L, Dwyer PL, Rosamilia A, Murray C, Thomas E, De Souza A et al (2008) Effectiveness of tension-free vaginal tape compared with transobturator tape in women with stress urinary incontinence and intrinsic sphincter deficiency: a randomized controlled trial. Obstet Gynecol 112(6):1253–1261
Costantini E, Kocjancic E, Lazzeri M, Giannantoni A, Zucchi A, Carbone A et al (2016) Long-term efficacy of the trans-obturator and retropubic mid-urethral slings for stress urinary incontinence: update from a randomized clinical trial. World J Urol 134(4):585–593
Tantanasis T, Daniilidis A, Pantelis A, Chatzis P, Vrachnis N (2013) Minimally invasive techniques for female stress urinary incontinence, how, why, when. Arch Gynecol Obstet 288(5):995–1001
Bazi T, Takahashi S, Ismail S, Bo K, Ruiz-Zapata AM, Duckett J et al (2016) Prevention of pelvic floor disorders: international urogynecological association research and development committee opinion. Int Urogynecol J 1–11. doi:10.1007/s00192-016-2993-9
Barber MD, Kleeman S, Karram MM, Paraiso MFR, Ellerkmann M, Vasavada S et al (2008) Risk factors associated with failure 1 year after retropubic or transobturator midurethral slings. Am J Obstet Gynecol 199(6):666–e1
Daneshgari F, Moore C, Frinjari H, Babineau D (2006) Patient related risk factors for recurrent stress urinary incontinence surgery in women treated at a tertiary care center. J Urol 176(4):1493–1499
Stav K, Dwyer PL, Rosamilia A, Schierlitz L, Lim YN, Lee J (2010) Risk factors of treatment failure of midurethral sling procedures for women with urinary stress incontinence. Int Urogynecol J 21(2):149–155
Cetinel B, Demirkesen O, Onal B, Akkus E, Alan C, Can G (2004) Are there any factors predicting the cure and complication rates of tension-free vaginal tape? Int Urogynecol J Pelvic Floor Dysfunct 15(3):188–193
Chen HY, Yeh LS, Chang WC, Ho M (2007) Analysis of risk factors associated with surgical failure of inside-out transobturator vaginal tape for treating urodynamic stress incontinence. Int Urogynecol J Pelvic Floor Dysfunct 18(4):443–447
Toozs-Hobson P, Devani P, Pick J, Moran PA, Assassa P, Burton C (2016) Does age affect the outcome of suburethral tape surgery? The importance of national registries in answering bigger questions. Int Urogynecol J 27:1541
Lee KS, Choo MS, Doo CK, Han DH, Lee YS, Kim JY et al (2008) The long term (5-years) objective TVT success rate does not depend on predictive factors at multivariate analysis: a multicentre retrospective study. Eur Urol 53(1):176–182
Frohme C, Ludt F, Varga Z, Olbert PJ, Hofmann R, Hegele A (2014) TOT approach in stress urinary incontinence (SUI)—outcome in obese female. BMC Urol. 14:20
Iancu G, Peltecu G (2014) Predicting the outcome of mid-urethral tape surgery for stress urinary incontinence using preoperative urodynamics—a systematic review. Chirurgia (Bucur) 109(3):359–368
Norton PA, Nager CW, Brubaker L, Lemack GE, Sirls LT, Holley R et al (2016) Urinary incontinence treatment network. The cost of preoperative urodynamics: a secondary analysis of the ValUE trial. Neurourol Urodyn 35(1):81–84
The American College of Obstetricians and Gynecologists (2014) Evaluation of uncomplicated stress urinary incontinence in women before surgical treatment. Committee Opinion No. 603. Obstet Gynecol 123:1403–1407
Abou-Gamrah A, Fawzy M, Sammour H, Tadros S (2014) Ultrasound assessment of bladder wall thickness as a screening test for detrusor instability. Arch Gynecol Obstet 289(5):1023–1028
Staack A, Vitale J, Ragavendra N, Rodríguez LV (2014) Translabial ultrasonography for evaluation of synthetic mesh in the vagina. Urology. 83(1):68–74
Rodrigo N, Wong V, Shek KL, Martin A, Dietz HP (2014) The use of 3-dimensional ultrasound of the pelvic floor to predict recurrence risk after pelvic reconstructive surgery. Aust N Z J Obstet Gynaecol 54(3):206–211
Chene G, Cotte B, Tardieu AS, Savary D, Mansoor A (2008) Clinical and ultrasonographic correlations following three surgical anti incontinence procedures (TOT, TVT and TVT-O). Int Urogynecol J Pelvic Floor Dysfunct 19(8):1125–1131
Yang JM, Yang SH, Huang WC, Tzeng CR (2013) Matched-pair analyses of resting and dynamic morphology between Monarc and TVT-O procedures by ultrasound. Eur J Obstet Gynecol Reprod Biol 169(2):402–407
Pereira-lucena CG, Artigiani Neto R, de Rezende DT, Lopes-Filho Gde J, Matos D, Linhares MM (2014) Early and late postoperative inflammatory and collagen deposition responses in three different meshes: an experimental study in rats. Hernia 18(4):563–570
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
None.
Conflict of interest
Author 1: TT Ilhan declares that he has no conflict of interest. Author 2: T Saymaz İlhan declares that she has no conflict of interest. Author 3: MG Ucar declares that he has no conflict of interest. Author 4: A Kebapcılar declares that she has no conflict of interest. Author 5: M Kıvrak declares that he has no conflict of interest. Author 6: Ç Çelik declares that he has no conflict of interest.
Rights and permissions
About this article
Cite this article
Ilhan, T.T., Ilhan, T.S., Ucar, M.G. et al. Can the suburethral mesh angle be used to predict trans-obturator tape results?. Arch Gynecol Obstet 295, 361–366 (2017). https://doi.org/10.1007/s00404-016-4230-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-016-4230-7