Abstract
The timing pattern in which dipeptidyl-peptidase IV inhibitors (DPP4i) confer the risk of bullous pemphigoid (BP) is unknown. To investigate the odds of BP following exposure to DPP4i and to perform a duration-response analysis evaluating the risk of BP in relation to the duration of exposure to the culprit drug. A population-based nested case–control study was performed comparing diabetic patients with BP (n = 1458) with age-, sex- and ethnicity-matched diabetic control subjects (n = 6051) with respect to the prevalence of exposure to DPP4i. Adjusted odds ratios (ORs) were estimated by logistic regression. Overall exposure to DPP4i was associated with an 80% increase in the odds of subsequent BP (OR, 1.81; 95% CI, 1.46–2.08; P < 0.001). In an intraclass analysis, the odds of BP were increased in association with vildagliptin (OR, 3.40; 95% CI, 2.69–4.29; P < 0.001) and sitagliptin (OR, 1.56; 95% CI, 1.33–1.84; P < 0.001). In a duration-response analysis, the highest likelihood of BP was found 1–2 years after commencing the drug (OR, 2.66; 95% CI, 1.97–3.59; P < 0.001). The odds of BP were increased across all time periods and retained its statistical significance even ≥ 6 years after the drug initiation (OR, 1.44; 95% CI, 1.09–1.91; P = 0.011). Relative to other diabetic patients with BP, patients with DPP4i-associated BP were more likely to be admitted to inpatient dermatologic wards (OR, 1.66; 95% CI, 1.30–2.13; P < 0.001) and had higher mean(SD) numbers of outpatient dermatologist visits (14.7[14.8] vs. 12.3[13.2], respectively; P = 0.006). DPP4i should be suspected as a predisposing factor for BP even numerous years after the drug initiation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The last two decades witnessed a substantial increase in the incidence of bullous pemphigoid (BP) [1]. This epidemiological observation has been ascribed to multiple factors, including the increasing exposure to culprit medications [1]. Multiple lines of evidence denoted that dipeptidyl-peptidase IV inhibitors (DPP4i), or gliptins, second- to third-line oral antidiabetic drugs, are associated with an increased risk of developing BP [2,3,4,5,6,7,8].
While DPP4i emerged as an indisputable risk factor of BP [9], a debate is still surrounding the question of whether DPP4i-associated BP is typified by a unique morphological, immunological, genetic, or histologic profile distinguishing it from typical BP [5, 8, 10,11,12,13,14,15,16,17,18]. Another crucial unanswered question relates to the existence of duration-response relation between exposure to DPP4i and the emergence of BP. To elaborate, inconsistency still exists with regard to the time in which DPP4i confers the highest risk of BP development.
The aim of the current study is to evaluate the odds of BP under different DPP4i agents. A specific spotlight will be shed on a duration-response analysis evaluating the risk of BP in relation to the duration of exposure to the culprit drugs. The secondary endpoint is to delineate the clinical and prognostic outcomes of patients with DPP4i-associated BP as compared to other diabetic patients with BP.
Methods
Study design and dataset
The current study was designed as a population-based nested case–control study. The computerized database of Clalit Health Service (CHS) was the origin of the current study. The study was approved by the Institutional Review Board of CHS (0212-17-COM).
CHS is the largest health maintenance organization in Israel, ensuring 4.6 million enrollees, which represent 51% of the general Israeli population. The computerized database of CHS continuously retrieves data from all tiers of healthcare facilities, including primary healthcare services, outpatient referral clinics, and inpatient wards. The database undergoes constant logarithmic checks to ascertain the validity of the diagnoses. The loss to follow-up is minor and access to CHS services is free, thus rendering the database compatible with generating robust epidemiological data. Further characteristics of CHS database are detailed in our previous publications [19,20,21].
Study population and definition of variables
The CHS database was systematically screened for incident cases with a diagnostic code BP and type 2 diabetes mellitus (T2DM) between the years 2007 and 2019. The diagnosis of BP was based on at least one of the following eligibility criteria: (i) a documented diagnosis of BP documented at least twice by a board-certified dermatologist, or (ii) a diagnosis of BP in discharge letters from dermatological wards. The diagnosis of T2DM relied on one of the following criteria: (i) two random tests of blood glucose greater than 200 mg/dL, (ii) one random test of blood glucose over 200 mg/dL with proven target organ damage, or (iii) two fasting glucose tests over 126 mg/dL.
A control group including 4–5 individuals per each case of BP was additionally enrolled. All control individuals lacked a diagnosis of BP but had a diagnosis of T2DM. Controls were matched based on sex, 5-year age group, and ethnicity and were recruited on the day in which the corresponding case was diagnosed.
Exposure to DPP4i agent was defined when sitagliptin, vildagliptin, linagliptin, or saxagliptin were prescribed for at least one month. Given uncertainties related to the timing of onset reported in the literature, the following durations of exposure to DPP4i have been arbitrarily chosen in the duration-response analysis (< 1, 1–2, 2–4, 4–6, ≥ 6 years). Outcome measures were adjusted for Charlson comorbidity index (CCI), an epidemiological scale that estimates the extent and severity of the comorbidities of each study participant. This index is widely utilized in epidemiological studies and was proved reliable in predicting mortality [22].
Since we did not have direct access to severity scores of patients, the burden of the disease was indirectly evaluated by the therapeutic regimen (e.g., the need for systemic corticosteroids and immunosuppressive/immunomodulatory adjuvant drugs) and healthcare utilization. Long-term systemic and topical corticosteroid variables were defined in cases managed by any drug pertaining to these classes for ≥ 6 months. Immunosuppressive/immunomodulatory adjuvant drugs included methotrexate, azathioprine, mycophenolate mofetil, rituximab, intravenous immunoglobulins, and plasmapheresis. Number of admission to dermatologic wards as well as number of visits to outpatient dermatologists following the diagnosis of BP was evaluated to provide an indirect estimate of disease severity.
Statistical analysis
Baseline characteristics were described by means and standard deviations (SD)s for continuous variables, whilst categorical values were signified by percentages. The comparison between different subgroups was performed using the Chi-square test and t-test, as indicated.
Logistic regression was used to calculate odds ratios (ORs) and 95% confidence intervals (CI)s to compare cases and controls regarding the presence of preceding DPP4i exposure. Owing to the temporal relationship between exposure and outcome in case–control studies, the association was calculated only based on individuals who developed BP after DPP4i. Two-tailed P-values less than 0.05 were considered statistically significant. Differences in the all-cause mortality of DPP4i-associated BP and diabetic patients with non- DPP4i-associated BP were evaluated using a stratified log-rank test. All statistical analyses were performed using SPSS software, version 25 (SPSS, Armonk, NY: IBM Corp).
Results
Characteristics of the study participants
The current study population comprised 7509 participants, of whom 1458 were diabetic patients with BP and 6051 were diabetic control subjects. The mean (SD) age at the diagnosis of diabetic patients with BP was 76.9 (11.0) years, 676 (46.4%) were males, and 1380 (94.7%) were of Jewish ancestry (Table 1). Patients with BP experienced an increased burden of comorbidities relative to controls, as demonstrated by a higher mean (SD) CCI score (3.4 [2.4] vs. 3.0 [2.3], respectively; P < 0.001). Demographic and clinical features of the study participants are detailed in Table 1.
The odds of bullous pemphigoid following the exposure to DPP4i
Out of eligible patients with BP, 322 (22.1%) have been managed by DPP4i prior to the development of their disease. Sitagliptin was the most frequent agent (n = 234), followed by vildagliptin (n = 134), linagliptin (n = 12), and saxagliptin (n = 7), with 65 patients being managed by more than an individual DPP4i agent.
Overall exposure to DPP4i was associated with an 80% increase in the odds of subsequent BP (OR, 1.81; 95% CI, 1.46–2.08; P < 0.001). In an intraclass analysis, the odds of BP were highest in association with vildagliptin (OR, 3.40; 95% CI, 2.69–4.29; P < 0.001) and were additionally increased among those treated by sitagliptin (OR, 1.56; 95% CI, 1.33–1.84; P < 0.001). Linagliptin (OR, 0.61; 95% CI, 0.33–1.13; P = 0.113) and saxagliptin (OR, 1.39; 95% CI, 0.59–3.27; P = 0.451) were not significantly associated with the development of BP (Table 2).
In a sex-stratified analysis, the odds of BP were more prominent among males undergoing overall DPP4i (OR, 1.97; 95% CI, 1.61–2.40; P < 0.001) and vildagliptin (OR, 3.69; 95% CI, 2.71–5.04; P < 0.001) treatment. When patients were divided on the basis of the median age, those younger than 78.6 years demonstrated a higher likelihood of BP following overall DPP4i (OR, 1.92; 95% CI, 1.57–2.34; P < 0.001), vildagliptin (OR, 3.74; 95% CI, 2.73–5.12; P < 0.001), and sitagliptin (OR, 1.67; 95% CI, 1.33–2.09; P < 0.001; Table 2). The outcome measures have not altered meaningfully in a multivariate analysis adjusting for age, sex, ethnicity, and comorbidities (Table 2).
A duration-response analysis estimating the odds of BP in relation to the duration of exposure
The median (range) latency separating the start of exposure to DPP4i agents and the development of BP was 3.3 (0.1–10.3) years (Fig. 1A). When the odds of DPP4i-associated BP were evaluated in relation to the duration of exposure, the highest likelihood of BP was found 1–2 years after commencing the drug (OR, 2.66; 95% CI, 1.97–3.59; P < 0.001). The risk was increased across all time periods and retained its statistical significance even ≥ 6 years following the drug initiation (OR, 1.44; 95% CI, 1.09–1.91; P = 0.011; Fig. 1B).
Clinical characteristics of patients with DPP4i-associated BP relative to other diabetic patients with BP
Table 3 delineates the clinical features of patients with DPP4i-associated BP (n = 322) as compared to diabetic patients with non-DPP4i-associated BP (n = 1136). Patients in the former group were typified by a male preponderance (OR, 1.66; 95% CI, 1.30–2.13; P < 0.001) and a higher frequency of smoking (OR, 1.36; 95% CI, 1.05–1.75; P = 0.018). With regard to the therapeutic approach, patients with DPP4i-associated BP were more likely to be admitted to inpatient dermatologic wards (OR, 1.66; 95% CI, 1.30–2.13; P < 0.001) and had higher mean (SD) numbers of outpatient dermatologists visits (14.7 [14.8] vs. 12.3 [13.2], respectively; P = 0.006) after their diagnosis.
We then compared the risk of all-cause mortality among the two aforementioned subgroups. After adjusting for age, sex, ethnicity, and comorbidities, the risk of all-cause mortality was comparable between patients with DPP4i-associated BP and diabetic patients with non- DPP4i-associated BP (HR, 0.85; 95% CI, 0.68–1.05; P = 0.125; Supplementary Fig. 1).
Discussion
The current population-based study depicted that exposure to DPP4i was associated with an 80% increase in the likelihood of subsequent BP. The odds of BP peaked 1–2 years following the initiation of DPP4i and remained statistically significant for more than 6 years after drug initiation. Compared with other diabetic patients with BP, those with DPP4i-associated BP displayed a greater frequency of admissions to inpatient dermatologic wards and visits to outpatient dermatologists.
The knowledge about the risk of BP with DPP4i therapy stemmed originally from anecdotal case reports and national pharmacovigilance database analyses [23, 24], and was subsequently authenticated by numerous observational controlled studies [2,3,4,5,6,7,8]. A recent meta-analysis has revealed that exposure to DPP4i was associated with more than a threefold increased risk of developing BP (pooled OR, 3.16; 95% CI 2.57–3.89) [9].
The current study revealed an 80% increased odds of BP under DPP4i. This estimate is lower than the pooled OR of the quantitative synthesis [9] and particularly than a large-scale case–control Finnish study reporting an OR of 3.45 (95% CI, 2.69–4.44) [3]. Since the latter study did not set a history of T2DM as an eligibility criterion for cases and controls, it was very likely to overestimate the association given that patients with BP are at an increased risk of T2DM at baseline. To elaborate further, the high OR probably mirrors the increased frequency of T2DM in BP rather than the predisposing effect of DPP4i [3]. Our estimate is closer to the hazard ratios (1.42 [95% CI, 1.17–1.72] [7] and 2.2 [95% CI, 1.45–3.38] [6]) provided by two large-scale retrospective cohort studies estimating the incidence of BP among patients with T2DM placed on DPP4i relative to second-line antidiabetic drugs. These two observational studies, typified by a robust design and large study population, were statistically and methodologically powered to investigate the association of BP with DPP4i and were not included in the aforementioned meta-analysis [9].
In congruence with the vast majority of other studies [2, 3, 5, 10], vildagliptin was implicated with the strongest potential of triggering BP. Vildagliptin is typified by a relatively lower selectivity for the DPP4 enzyme in comparison with other members of the DPP family, such as DPP-8 and DPP-9 [25]. Therefore, it has been assumed that off-target DPP-8/DPP-9 inhibition might account for the excessive risk associated with this individual drug [7]. In the current study, sitagliptin imposed a statistically significant risk of eliciting BP. While this finding aligns with the observation of Varpuluoma et al. [3], it negates other studies signifying that sitagliptin is not associated with BP [2, 5, 7, 10]. Although linagliptin was found to predispose diabetic patients to BP in several studies [2, 5,6,7], the current study failed to reproduce this observation, probably due to the few exposed events. Due to the low number of patients under saxagliptin, the current study, similar to three recent studies [6,7,8], was underpowered to gauge the odds of saxagliptin-associated BP.
The pattern of timing in which DPP4i leads to the development of BP is a question with enormous clinical implications. The median latency between the commencement of DPP4i and the onset of BP varied noticeably in different reports, ranging between 6.0 to 26.4 months [2, 3, 5, 8, 13, 23]. The median latency in our cohort (3.3 years) was higher than all previous reports. Temporal trends in the risk of BP throughout the duration of exposure to DPP4i were evaluated in a single study and were found to peak after 20 months of treatment [6]. This finding accords with our study depicting that the maximal odds of BP occur 1–2 years following the initiation of DPP4i. Intriguingly, the elevated odds of BP persisted even beyond 6 years after the initiation of the drug. This finding is commensurate with the study of Douros et al. [6], which attested that the risk of BP remains elevated almost 6 years after the start of the treatment. Consequently, DPP4i should be suspected as a putative trigger for BP, even if it had been started numerous years prior to the onset of BP. The delayed onset of BP following the administration of DPP4i might suggest that additional factors are required to break the tolerance to BP180. The latter is continuously maintained as might be inferred by the increased risk of BP after checkpoint inhibitors [26].
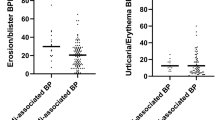
Several observational studies have attributed a more severe phenotype for DPP4i-associated BP. Ständer et al. [27] found that patients with DPP4i-associated BP had a more severe bullous component, as indicated by a higher erosion/blister BPDAI score. Correspondingly, Kridin [5] reported that patients with DPP4i-associated BP presented with significantly more extensive disease. Additionally, Patsatsi et al. [17] revealed that patients with DPP4i-associated BP had higher total BPDAI scores with a trend towards significance (41.0 vs. 34.1; P = 0.063). The current study was unable to measure severity scores of eligible patients but has provided indirect estimates of the disease burden and severity. Relative to other diabetic patients with BP, patients with DPP4i-associated BP had an increased frequency of dermatologic hospitalizations and a higher number of visits to outpatient dermatologists. These findings probably reflect a more severe and recalcitrant disease and provide a population-based evidence regarding an increased burden of this disease subtype.
Since CHS provides healthcare services for more than 50% of the general Israeli population, our findings feature high generalizability for the Israeli population. The retrieval of medical data from all tiers of healthcare facilities argues against selection bias and provides a comprehensive insight into the investigated question. The free access to healthcare services, negligible loss to follow-up, and inconsequential missing data all represent additional strengths of the study. The study has some limitations to acknowledge. Owing to its population-based nature, the study lacked direct immunopathological validation of the diagnosis of BP. The validity of the diagnosis, however, was substantiated by confining its documentation to certified dermatologists and dermatologic inpatient wards. In Israel, it is highly unlikely for dermatologists to base a diagnosis of BP without performing the globally acceptable immunodiagnostic essays like direct and indirect immunofluorescence [28]. Since the ethnic background of study participants was relatively homogenous, global generalizability might be lacking.
In conclusion, the current population-based study denoted that exposure to DPP4i is implicated with an 80% increase in the likelihood of subsequent BP. In an intraclass analysis, vildagliptin conferred the greatest odds of provoking BP. The risk of BP reached its peak 1–2 years following the initiation of DPP4i and remained elevated for more than 6 years following drug initiation. Patients with DPP4i-associated BP exhibited a greater disease burden. These observations imply an increased burden and corroborate previous reports about a more severe phenotype of this disease subtype. Clinicians should be aware that DPP4i might still be able to elicit BP even numerous years after drug initiation. Further studies investigating patients from different ethnic backgrounds are warranted to validate our findings.
References
Kridin K, Ludwig RJ (2018) The growing incidence of Bullous pemphigoid: overview and potential explanations. Front Med 5:220
Benzaquen M, Borradori L, Berbis P, Cazzaniga S, Valero R, Richard M-A et al (2017) Dipeptidyl peptidase IV inhibitors, a risk factor for bullous pemphigoid: retrospective multicenter case-control study from France and Switzerland. J Am Acad Dermatol 78:1090–1096
Varpuluoma O, Försti AK, Jokelainen J, Turpeinen M, Timonen M, Huilaja L et al (2018) Vildagliptin significantly increases the risk of bullous pemphigoid: a Finnish Nationwide Registry Study. J Invest Dermatol 138(7):1659–1661
Schaffer C, Buclin T, Jornayvaz FR, Cazzaniga S, Borradori L, Gilliet M et al (2018) Use of dipeptidyl-peptidase IV inhibitors and bullous pemphigoid. Dermatology 233(5):401–403. https://doi.org/10.1159/000480498
Kridin K, Bergman R (2018) Association of bullous pemphigoid with dipeptidyl-peptidase 4 inhibitors in patients with diabetes: estimating the risk of the new agents and characterizing the patients. JAMA Dermatol 154(10):1152–1158. https://doi.org/10.1001/jamadermatol.2018.2352
Douros A, Rouette J, Yin H, Yu OHY, Filion KB, Azoulay L (2019) Dipeptidyl peptidase 4 inhibitors and the risk of bullous pemphigoid among patients with type 2 diabetes. Diabetes Care 42(8):1496–1503
Lee SG, Lee HJ, Yoon MS, Kim DH (2019) Association of dipeptidyl peptidase 4 inhibitor use with risk of bullous pemphigoid in patients with diabetes. JAMA Dermatol 155(2):172–177
Plaquevent M, Tétart F, Fardet L, Ingen-Housz-Oro S, Valeyrie-Allanore L, Bernard P et al (2019) Higher frequency of dipeptidyl peptidase-4 inhibitor intake in bullous pemphigoid patients than in the French general population. J Invest Dermatol. 139:835–841
Kridin K, Cohen AD (2018) Dipeptidyl-peptidase IV inhibitor-associated bullous pemphigoid: a systematic review and meta-analysis. J Am Acad Dermatol 85:501–503
Nishie W, Tasanen K (2019) Gliptin-associated bullous pemphigoid: a valuable model of the mechanism of breakdown of immune tolerance against BP180. J Investig Dermatol 139:755–756
Nishie W (2019) Dipeptidyl peptidase IV inhibitor-associated bullous pemphigoid: a recently recognized autoimmune blistering disease with unique clinical, immunological and genetic characteristics. Immunol Med 42:22–28
Tasanen K, Varpuluoma O, Nishie W (2019) Dipeptidyl peptidase-4 inhibitor-associated bullous pemphigoid. Front Immunol 10:1238
Chijiwa C, Takeoka S, Kamata M, Tateishi M, Fukaya S, Hayashi K et al (2018) Decrease in eosinophils infiltrating into the skin of patients with dipeptidyl peptidase-4 inhibitor-related bullous pemphigoid. J Dermatol 45:596–599. https://doi.org/10.1111/1346-8138.14245
Izumi K, Nishie W, Mai Y, Wada M, Natsuga K, Ujiie H et al (2016) Autoantibody profile differentiates between inflammatory and noninflammatory bullous pemphigoid. J Invest Dermatol 136:2201–2210
Ujiie H, Muramatsu K, Mushiroda T, Ozeki T, Miyoshi H, Iwata H et al (2018) HLA-DQB1*03:01 as a biomarker for genetic susceptibility to bullous pemphigoid induced by DPP-4 inhibitors. J Invest Dermatol 138(5):1201–1204
Lindgren O, Varpuluoma O, Tuusa J, Ilonen J, Huilaja L, Kokkonen N et al (2019) Gliptin-associated bullous pemphigoid and the expression of dipeptidyl peptidase-4/CD26 in bullous pemphigoid. Acta Derm Venereol 99(6):602–609
Patsatsi A, Kyriakou A, Meltzanidou P, Trigoni A, Lamprou F, Kokolios M et al (2018) Bullous pemphigoid in patients with DPP-4 inhibitors at the onset of disease: does this differ from common bullous pemphigoid? Eur J Dermatology 28(5):711–713
Fania L, Salemme A, Provini A, Pagnanelli G, Collina MC, Abeni D et al (2018) Detection and characterization of IgG, IgE, and IgA autoantibodies in patients with bullous pemphigoid associated with dipeptidyl peptidase-4 inhibitors. J Am Acad Dermatol 78(3):592–595. https://doi.org/10.1016/j.jaad.2017.09.051
Kridin K, Ludwig RJ, Schonmann Y, Damiani G, Cohen AD (2020) The bidirectional association between bullous pemphigoid and psoriasis: a population-based cohort study. Front Med. 7:511
Kridin K, Zelber-Sagi S, Comaneshter D, Cohen AD (2018) Coexistent solid malignancies in pemphigus a population-based study. JAMA Dermatol 154(4):435–440
Cohen AD, Dreiher J, Regev-Rosenberg S, Yakovson O, Lieberman N, Goldfracht M et al (2010) The quality indigators program in Clalit Health Services: the first decade. Harefuah. 149(4):204–209
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40(5):373–383
Béné J, Moulis G, Bennani I, Auffret M, Coupe P, Babai S et al (2016) Bullous pemphigoid and dipeptidyl peptidase IV inhibitors: a case–noncase study in the French Pharmacovigilance Database. Br J Dermatol 175(2):296–301
García M, Aranburu MA, Palacios-Zabalza I, Lertxundi U, Aguirre C (2016) Dipeptidyl peptidase-IV inhibitors induced bullous pemphigoid: a case report and analysis of cases reported in the European pharmacovigilance database. J Clin Pharm Ther 41(3):368–370. https://doi.org/10.1111/jcpt.12397
Baetta R, Corsini A (2011) Pharmacology of dipeptidyl peptidase-4 inhibitors: similarities and differences. Drugs 71:1441–1467
Lopez AT, Khanna T, Antonov N, Audrey-Bayan C, Geskin L (2018) A review of bullous pemphigoid associated with PD-1 and PD-L1 inhibitors. Int J Dermatol 57(6):664–669
Ständer S, Schmidt E, Zillikens D, Ludwig RJ, Kridin K (2021) More severe erosive phenotype despite lower circulating autoantibody levels in dipeptidyl peptidase-4 inhibitor (DPP4i)-associated bullous pemphigoid: a retrospective cohort study. Am J Clin Dermatol 22(1):117–127
Kridin K, Zelber-Sagi S, Khamaisi M, Cohen AD, Bergman R (2016) Remarkable differences in the epidemiology of pemphigus among two ethnic populations in the same geographic region. J Am Acad Dermatol 75(5):925–930
Funding
Open Access funding enabled and organized by Projekt DEAL. None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
ADC served as an advisor, investigator, or speaker for Abbvie, BI, Dexcel Pharma, Janssen, Novartis, Perrigo, Pfizer, and Rafa. None of the other authors have any conflicts of interest to declare.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Kridin, K., Avni, O., Damiani, G. et al. Dipeptidyl-peptidase IV inhibitor (DPP4i) confers increased odds of bullous pemphigoid even years after drug initiation. Arch Dermatol Res 315, 33–39 (2023). https://doi.org/10.1007/s00403-021-02317-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00403-021-02317-9