Abstract
Introduction
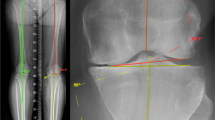
The assessment of the knee alignment on long leg radiographs (LLR) postoperative to corrective knee osteotomies (CKOs) is highly dependent on the reader’s expertise. Artificial Intelligence (AI) algorithms may help automate and standardise this process. The study aimed to analyse the reliability of an AI-algorithm for the evaluation of LLRs following CKOs.
Materials and methods
In this study, we analysed a validation cohort of 110 postoperative LLRs from 102 patients. All patients underwent CKO, including distal femoral (DFO), high tibial (HTO) and bilevel osteotomies. The agreement between manual measurements and the AI-algorithm was assessed for the mechanical axis deviation (MAD), hip knee ankle angle (HKA), anatomical-mechanical-axis-angle (AMA), joint line convergence angle (JLCA), mechanical lateral proximal femur angle (mLPFA), mechanical lateral distal femoral angle (mLDFA), mechanical medial proximal tibia angle (mMPTA) and mechanical lateral distal tibia angle (mLDTA), using the intra-class-correlation (ICC) coefficient between the readers, each reader and the AI and the mean of the manual reads and the AI-algorithm and Bland–Altman Plots between the manual reads and the AI software for the MAD, HKA, mLDFA and mMPTA.
Results
In the validation cohort, the AI software showed excellent agreement with the manual reads (ICC: 0.81–0.99). The agreement between the readers (Inter-rater) showed excellent correlations (ICC: 0.95–0. The mean difference in the DFO group for the MAD, HKA, mLDFA and mMPTA were 0.50 mm, − 0.12°, 0.55° and 0.15°. In the HTO group the mean difference for the MAD, HKA, mLDFA and mMPTA were 0.36 mm, − 0.17°, 0.57° and 0.08°, respectively. Reliable outputs were generated in 95.4% of the validation cohort.
Conclusion
he application of AI-algorithms for the assessment of lower limb alignment on LLRs following CKOs shows reliable and accurate results.
Level of evidence
Diagnostic Level III.



Similar content being viewed by others
Data availability
All data supporting the findings of this study are available within the paper. The raw data that of this study are not openly available due to reasons of sensitivity and are available from the corresponding author upon reasonable request. Data are located in controlled access data storage at the Orthopaedic Hospital Speising, Vienna, Austria.
References
Fakhrai N, Widhalm P, Chiari C, Weber M, Langs G, Donner R, Ringl H, Jantsch M, Peloschek P (2010) Automatic assessment of the knee alignment angle on full-limb radiographs. Eur J Radiol 74:236–240. https://doi.org/10.1016/j.ejrad.2009.02.004
Dawson MJ, Ollivier M, Menetrey J, Beaufils P (2022) Osteotomy around the painful degenerative varus knee: a 2022 ESSKA formal consensus. Knee Surg Sport Traumatol Arthrosc. https://doi.org/10.1007/s00167-022-07024-0
Smith JO, Wilson AJ, Thomas NP (2013) Osteotomy around the knee: evolution, principles and results. Knee Surg Sport Traumatol Arthrosc 21:3–22. https://doi.org/10.1007/s00167-012-2206-0
Eberbach H, Mehl J, Feucht MJ, Bode G, Südkamp NP, Niemeyer P (2017) Geometry of the valgus knee: contradicting the dogma of a femoral-based deformity. Am J Sports Med 45:909–914. https://doi.org/10.1177/0363546516676266
Briem K, Ramsey DK, Newcomb W, Rudolph KS, Snyder-Mackler L (2007) Effects of the amount of valgus correction for medial compartment knee osteoarthritis on clinical outcome, knee kinetics and muscle co-contraction after opening wedge high tibial osteotomy. J Orthop Res 25:311–318. https://doi.org/10.1002/jor.20326
Luís NM, Varatojo R (2021) Radiological assessment of lower limb alignment. EFORT Open Rev 6:487–494. https://doi.org/10.1302/2058-5241.6.210015
Dexel J, Kirschner S, Günther K-P, Lützner J (2014) Agreement between radiological and computer navigation measurement of lower limb alignment. Knee Surg Sport Traumatol Arthrosc 22:2721–2727. https://doi.org/10.1007/s00167-013-2599-4
Prijs J, Liao Z, Ashkani-Esfahani S, Olczak J, Gordon M, Jayakumar P, Jutte PC, Jaarsma RL, IJpma FFA, Doornberg JN (2022) Artificial intelligence and computer vision in orthopaedic trauma. Bone Jt J 104-B:911–914. https://doi.org/10.1302/0301-620X.104B8.BJJ-2022-0119.R1
Ramkumar PN, Kunze KN, Haeberle HS, Karnuta JM, Luu BC, Nwachukwu BU, Williams RJ (2021) Clinical and research medical applications of artificial intelligence. Arthrosc J Arthrosc Relat Surg 37:1694–1697. https://doi.org/10.1016/j.arthro.2020.08.009
Tiulpin A, Thevenot J, Rahtu E, Lehenkari P, Saarakkala S (2018) Automatic knee osteoarthritis diagnosis from plain radiographs: a deep learning-based approach. Sci Rep 8:1–10. https://doi.org/10.1038/s41598-018-20132-7
Schock J, Truhn D, Abrar DB, Merhof D, Conrad S, Post M, Mittelstrass F, Kuhl C, Nebelung S (2021) Automated analysis of alignment in long-leg radiographs by using a fully automated support system based on artificial intelligence. Radiol Artif Intell 3:e200198. https://doi.org/10.1148/ryai.2020200198
Simon S, Schwarz GM, Aichmair A, Frank BJH, Hummer A, DiFranco MD, Dominkus M, Hofstaetter JG (2022) Fully automated deep learning for knee alignment assessment in lower extremity radiographs: a cross-sectional diagnostic study. Skeletal Radiol 51:1249–1259. https://doi.org/10.1007/s00256-021-03948-9
Schwarz GM, Simon S, Mitterer JA, Frank BJH, Aichmair A, Dominkus M, Hofstaetter JG (2022) Artificial intelligence enables reliable and standardized measurements of implant alignment in long leg radiographs with total knee arthroplasties. Knee Surg Sport Traumatol Arthrosc 30:2538–2547. https://doi.org/10.1007/s00167-022-07037-9
Webb JI, Stoner RS, Afzal I, Evans CR, Scott G, Field RE (2021) The Medial Rotation Knee replacement: clinical and radiological results of a multi-centre surveillance study at five years. Knee 28:247–255. https://doi.org/10.1016/j.knee.2020.12.025
Paley D (2002) Principles of deformity correction. Springer Berlin Heidelberg, Berlin, Heidelberg
Koo TK, Li MY (2016) A guideline of selecting and reporting intraclass correlation coefficients for reliability research. J Chiropr Med 15:155–163. https://doi.org/10.1016/j.jcm.2016.02.012
Kowe M (2019) Die intra-cluster-correlation im kontext der fallzahlschätzung cluster-randomisierter studien in der pegewissenschaft. Philosophisch-Theologischen Hochschule Vallendar
Hirschmann MT, Moser LB, Amsler F, Behrend H, Leclerq V, Hess S (2019) Functional knee phenotypes: a novel classification for phenotyping the coronal lower limb alignment based on the native alignment in young non-osteoarthritic patients. Knee Surg Sport Traumatol Arthrosc 27:1394–1402. https://doi.org/10.1007/s00167-019-05509-z
Knutson GA (2005) Anatomic and functional leg-length inequality: a review and recommendation for clinical decision-making. Part I, anatomic leg-length inequality: prevalence, magnitude, effects and clinical significance. Chiropr Osteopat 13:1–10. https://doi.org/10.1186/1746-1340-13-11
Obuchowski NA, Subhas N, Schoenhagen P (2014) Testing for interchangeability of imaging tests. Acad Radiol 21:1483–1489. https://doi.org/10.1016/j.acra.2014.07.004
Matsuura M, Murata H, Fujino Y, Hirasawa K, Yanagisawa M, Asaoka R (2018) Evaluating the usefulness of MP-3 microperimetry in glaucoma patients. Am J Ophthalmol 187:1–9. https://doi.org/10.1016/j.ajo.2017.12.002
Bernstein P, Metzler J, Weinzierl M, Seifert C, Kisel W, Wacker M (2021) Radiographic scoliosis angle estimation: spline-based measurement reveals superior reliability compared to traditional COBB method. Eur Spine J 30:676–685. https://doi.org/10.1007/s00586-020-06577-3
Jamali AA, Meehan JP, Moroski NM, Anderson MJ, Lamba R, Parise C (2017) Do small changes in rotation affect measurements of lower extremity limb alignment? J Orthop Surg Res 12:1–8. https://doi.org/10.1186/s13018-017-0571-6
Ahmad SS, Weinrich L, Giebel GM, Beyer MR, Stöckle U, Konrads C (2021) Frontal knee alignment influences the vertical orientation of the femoral neck in standing position. Bone Jt Open 2:1057–1061. https://doi.org/10.1302/2633-1462.212.BJO-2021-0100.R1
Kunze KN, Polce EM, Patel A, Courtney PM, Levine BR (2021) Validation and performance of a machine-learning derived prediction guide for total knee arthroplasty component sizing. Arch Orthop Trauma Surg 141:2235–2244. https://doi.org/10.1007/s00402-021-04041-5
Tsai A (2022) A deep learning approach to automatically quantify lower extremity alignment in children. Skelet Radiol 51:381–390. https://doi.org/10.1007/s00256-021-03844-2
Hirschmann A, Cyriac J, Stieltjes B, Kober T, Richiardi J, Omoumi P (2019) Artificial intelligence in musculoskeletal imaging: review of current literature, challenges, and trends. Semin Musculoskelet Radiol 23:304–311. https://doi.org/10.1055/s-0039-1684024
Schwarz GM, Simon S, Mitterer JA, Huber S, Frank BJH, Aichmair A, Dominkus M, Hofstaetter JG (2023) Can an artificial intelligence powered software reliably assess pelvic radiographs. Int Orthop. https://doi.org/10.1007/s00264-023-05722-z
Langerhuizen DWG, Janssen SJ, Mallee WH, Van Den Bekerom MPJ, Ring D, Kerkhoffs GMMJ, Jaarsma RL, Doornberg JN (2019) What are the applications and limitations of artificial intelligence for fracture detection and classification in orthopaedic trauma imaging? A systematic review. Clin Orthop Relat Res 477:2482–2491. https://doi.org/10.1097/CORR.0000000000000848
Sailhan F, Jacob L, Hamadouche M (2017) Differences in limb alignment and femoral mechanical-anatomical angles using two dimension versus three dimension radiographic imaging. Int Orthop 41:2009–2016. https://doi.org/10.1007/s00264-017-3428-z
Lee NK, Kim TW, Lee S, Choi YS, Kang SB, Chang CB (2021) Effect of distance between the feet on knee joint line orientation after total knee arthroplasty in standing full-limb radiographs. Knee Surg Sport Traumatol Arthrosc 30:3032–3040. https://doi.org/10.1007/s00167-021-06662-0
Klemt C, Cohen-Levy WB, Robinson MG, Burns JC, Alpaugh K, Yeo I, Kwon Y-M (2022) Can machine learning models predict failure of revision total hip arthroplasty? Arch Orthop Trauma Surg 143:2805–2812. https://doi.org/10.1007/s00402-022-04453-x
Acknowledgements
We would like to acknowledge Matthew D. DiFranco, PhD and Allan Hummer, PhD for the technical support, Bernd Otzelberger for statistical support and Susana Gardete-Hartmann, PhD for conceptualization.
Funding
The “Michael Ogon Laboratory for Orthopaedic Research” received a research grant from “Image Biopsy Lab GmbH”. The collection, analysis, and interpretation of data, writing of the report, and the decision to submit the paper for publication were performed by the authors and not influenced by Image Biopsy Lab.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. JAM, SH, SS, MP, FK and BJHF performed material preparation, data collection and analysis. JAM wrote the first draft of the manuscript and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript. Conceptualization and Methodology: JAM, SH, GMS, SS and JGH. Formal analysis and investigation: JAM, SH, GMS and JGH. Writing—original draft preparation: JAM. Writing—review and editing: JAM, SH, GMS and JGH. Funding acquisition, Resources and Supervision: JGH.
Corresponding author
Ethics declarations
Conflict of Interest
There is no agreement with commercial interest related to this study, which would limit or delay the publication in any way or would limit all data generated for the study.
Ethical approval
EK 46/2020
Informed consent
Individual informed consent was waived.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mitterer, J.A., Huber, S., Schwarz, G.M. et al. Fully automated assessment of the knee alignment on long leg radiographs following corrective knee osteotomies in patients with valgus or varus deformities. Arch Orthop Trauma Surg 144, 1029–1038 (2024). https://doi.org/10.1007/s00402-023-05151-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-023-05151-y