Abstract
Introduction
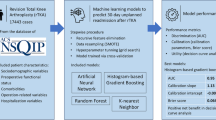
The total length of stay (LOS) is one of the biggest determinators of overall care costs associated with total knee arthroplasty (TKA). An accurate prediction of LOS could aid in optimizing discharge strategy for patients in need and diminishing healthcare expenditure. The aim of this study was to predict LOS following TKA using machine learning models developed on a national-scale patient cohort.
Methods
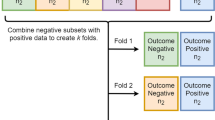
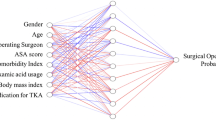
The ACS-NSQIP database was queried to acquire 267,966 TKA cases from 2013 to 2020. Four machine learning models—artificial neural network (ANN), random forest, histogram-based gradient boosting, and k-nearest neighbor were trained and tested on the dataset for the prediction of prolonged LOS (LOS exceeded the 75th of all values in the cohort). The model performance was assessed by discrimination (area under the receiver operating characteristic curve [AUC]), calibration, and clinical utility.
Results
ANN delivered the best performance among the four models. ANN distinguished prolonged LOS in the study cohort with an AUC of 0.71 and accurately predicted the probability of prolonged LOS for individual patients (calibration slope: 0.82; calibration intercept: 0.03; Brier score: 0.089). All models demonstrated clinical utility by generating positive net benefits in decision curve analyses. Operation time, pre-operative transfusion, pre-operative laboratory tests (hematocrit, platelet count, and white blood cell count), and BMI were the strongest predictors of prolonged LOS.
Conclusion
ANN demonstrated modest discrimination capacity and excellent performance in calibration and clinical utility for the prediction of prolonged LOS following TKA. Clinical application of the machine learning models has the potential to improve care coordination and discharge planning for patients at high risk of extended hospitalization after surgery. Incorporating more relevant patient factors may further increase the models’ prediction strength.



Similar content being viewed by others
References
Memtsoudis SG, Della Valle AG, Besculides MC et al (2009) Trends in demographics, comorbidity profiles, in-hospital complications and mortality associated with primary knee arthroplasty. J Arthroplasty 24:518–527. https://doi.org/10.1016/j.arth.2008.01.307
Sarpong NO, Boddapati V, Herndon CL et al (2019) Trends in length of stay and 30-day complications after total knee arthroplasty: an analysis from 2006 to 2016. J Arthroplasty 34:1575–1580. https://doi.org/10.1016/j.arth.2019.04.027
Song X, Xia C, Li Q et al (2020) Perioperative predictors of prolonged length of hospital stay following total knee arthroplasty: a retrospective study from a single center in China. BMC Musculoskelet Disord 21:62. https://doi.org/10.1186/s12891-020-3042-x
Yakkanti RR, Miller AJ, Smith LS et al (2019) Impact of early mobilization on length of stay after primary total knee arthroplasty. Ann Transl Med 7:69–69. https://doi.org/10.21037/atm.2019.02.02
van den Belt L, van Essen P, Heesterbeek PJC, Defoort KC (2015) Predictive factors of length of hospital stay after primary total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 23:1856–1862. https://doi.org/10.1007/s00167-014-3313-x
Burn E, Edwards CJ, Murray DW et al (2018) Trends and determinants of length of stay and hospital reimbursement following knee and hip replacement: evidence from linked primary care and NHS hospital records from 1997 to 2014. BMJ Open 8:e019146. https://doi.org/10.1136/bmjopen-2017-019146
Culler SD, Jevsevar DS, Shea KG et al (2015) The incremental hospital cost and length-of-stay associated with treating adverse events among medicare beneficiaries undergoing TKA. J Arthroplasty 30:19–25. https://doi.org/10.1016/j.arth.2014.08.023
Sloan M, Premkumar A, Sheth NP (2018) Projected volume of primary total joint arthroplasty in the U.S., 2014 to 2030. J Bone Joint Surg 100:1455–1460. https://doi.org/10.2106/JBJS.17.01617
Molloy IB, Martin BI, Moschetti WE, Jevsevar DS (2017) Effects of the length of stay on the cost of total knee and total hip arthroplasty from 2002 to 2013. J Bone Joint Surg Am 99:402–407. https://doi.org/10.2106/JBJS.16.00019
Specht K, Kjaersgaard-Andersen P, Pedersen BD (2016) Patient experience in fast-track hip and knee arthroplasty–a qualitative study. J Clin Nurs 25:836–845. https://doi.org/10.1111/jocn.13121
Haughom BD, Schairer WW, Hellman MD et al (2015) An analysis of risk factors for short-term complication rates and increased length of stay following unicompartmental knee arthroplasty. HSS J 11:112–116. https://doi.org/10.1007/s11420-014-9422-8
Klemt C, Tirumala V, Barghi A et al (2022) Artificial intelligence algorithms accurately predict prolonged length of stay following revision total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 30:2556–2564. https://doi.org/10.1007/s00167-022-06894-8
Mathijssen NMC, Verburg H, van Leeuwen CCG et al (2016) Factors influencing length of hospital stay after primary total knee arthroplasty in a fast-track setting. Knee Surg Sports Traumatol Arthrosc 24:2692–2696. https://doi.org/10.1007/s00167-015-3932-x
Sephton BM, Bakhshayesh P, Edwards TC et al (2020) Predictors of extended length of stay after unicompartmental knee arthroplasty. J Clin Orthop Trauma 11:S239–S245. https://doi.org/10.1016/j.jcot.2019.09.009
Zhong H, Poeran J, Gu A et al (2021) Machine learning approaches in predicting ambulatory same day discharge patients after total hip arthroplasty. Reg Anesth Pain Med 46:779–783. https://doi.org/10.1136/rapm-2021-102715
Cohen-Levy WB, Klemt C, Tirumala V et al (2022) Artificial neural networks for the prediction of transfusion rates in primary total hip arthroplasty. Arch Orthop Trauma Surg. https://doi.org/10.1007/s00402-022-04391-8
Klemt C, Harvey MJ, Robinson MG et al (2022) Machine learning algorithms predict extended postoperative opioid use in primary total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 30:2573–2581. https://doi.org/10.1007/s00167-021-06812-4
Klemt C, Laurencin S, Uzosike AC et al (2022) Machine learning models accurately predict recurrent infection following revision total knee arthroplasty for periprosthetic joint infection. Knee Surg Sports Traumatol Arthrosc 30:2582–2590. https://doi.org/10.1007/s00167-021-06794-3
Mohammed H, Huang Y, Memtsoudis S et al (2022) Utilization of machine learning methods for predicting surgical outcomes after total knee arthroplasty. PLoS One 17:e0263897. https://doi.org/10.1371/journal.pone.0263897
Yeo I, Klemt C, Melnic CM et al (2022) Predicting surgical operative time in primary total knee arthroplasty utilizing machine learning models. Arch Orthop Trauma Surg. https://doi.org/10.1007/s00402-022-04588-x
Sridhar S, Whitaker B, Mouat-Hunter A, McCrory B (2022) Predicting length of Stay using machine learning for total joint replacements performed at a rural community hospital. PLoS One 17:e0277479. https://doi.org/10.1371/journal.pone.0277479
Han C, Liu J, Wu Y et al (2021) To predict the length of hospital stay after total knee arthroplasty in an orthopedic center in China: the use of machine learning algorithms. Front Surg 8:606038. https://doi.org/10.3389/fsurg.2021.606038
Navarro SM, Wang EY, Haeberle HS et al (2018) Machine learning and primary total knee arthroplasty: patient forecasting for a patient-specific payment model. J Arthroplasty 33:3617–3623. https://doi.org/10.1016/j.arth.2018.08.028
Abbas A, Mosseri J, Lex JR et al (2022) Machine learning using preoperative patient factors can predict duration of surgery and length of stay for total knee arthroplasty. Int J Med Inform 158:104670. https://doi.org/10.1016/j.ijmedinf.2021.104670
Ramkumar PN, Karnuta JM, Navarro SM et al (2019) Deep learning preoperatively predicts value metrics for primary total knee arthroplasty: development and validation of an artificial neural network model. J Arthroplasty 34:2220-2227.e1. https://doi.org/10.1016/j.arth.2019.05.034
Klemt C, Laurencin S, Alpaugh K et al (2022) The utility of machine learning algorithms for the prediction of early revision surgery after primary total hip arthroplasty. J Am Acad Orthop Surg 30:513–522. https://doi.org/10.5435/JAAOS-D-21-01039
Klemt C, Yeo I, Cohen-Levy WB et al (2022) Artificial neural networks can predict early failure of cementless total hip arthroplasty in patients with osteoporosis. J Am Acad Orthop Surg 30:467–475. https://doi.org/10.5435/JAAOS-D-21-00775
Mandrekar JN (2010) Receiver operating characteristic curve in diagnostic test assessment. J Thorac Oncol 5:1315–1316. https://doi.org/10.1097/JTO.0b013e3181ec173d
Ferro CAT (2007) Comparing probabilistic forecasting systems with the brier score. Weather Forecast 22:1076–1088. https://doi.org/10.1175/WAF1034.1
Rufibach K (2010) Use of Brier score to assess binary predictions. J Clin Epidemiol 63:938–939. https://doi.org/10.1016/j.jclinepi.2009.11.009
Vickers AJ, van Calster B, Steyerberg EW (2019) A simple, step-by-step guide to interpreting decision curve analysis. Diagn Progn Res 3:18. https://doi.org/10.1186/s41512-019-0064-7
Stepaniak PS, Heij C, De Vries G (2010) Modeling and prediction of surgical procedure times. Stat Neerl 64:1–18. https://doi.org/10.1111/j.1467-9574.2009.00440.x
Zhang Z, Ji Y, Wang Z et al (2018) The association between platelet indices and deep surgical site infection after open induction internal fixation for traumatic limb fractures. Infect Drug Resist 11:2533–2538. https://doi.org/10.2147/IDR.S184877
Gu A, Maybee CM, Wei C et al (2019) Preoperative blood transfusion associated with increased length of stay and increased postoperative complications after revision total knee arthroplasty. J Orthop 16:265–268. https://doi.org/10.1016/j.jor.2019.02.014
Duarte GDC, Catanoce AP, Zabeu JL et al (2021) Association of preoperative anemia and increased risk of blood transfusion and length of hospital stay in adults undergoing hip and knee arthroplasty: an observational study in a single tertiary center. Health Science Reports 4:e448. https://doi.org/10.1002/hsr2.448
Noble JW, Moore CA, Liu N (2012) The value of patient-matched instrumentation in total knee arthroplasty. J Arthroplasty 27:153–155. https://doi.org/10.1016/j.arth.2011.07.006
Zajonz D, Höhn C, Neumann J et al (2020) Increasing efficiency by optimizing table position for elective primary THA and TKA: a prospective monocentric pilot study. Arthroplasty 2:29. https://doi.org/10.1186/s42836-020-00048-2
Schwartz AJ, Clarke HD, Sassoon A et al (2020) The clinical and financial consequences of the centers for medicare and medicaid services’ two-midnight rule in total joint arthroplasty. J Arthroplasty 35:1-6.e1. https://doi.org/10.1016/j.arth.2019.08.048
Zhang W, Lyman S, Boutin-Foster C et al (2016) Racial and ethnic disparities in utilization rate, hospital volume, and perioperative outcomes after total knee arthroplasty. J Bone Joint Surg Am 98:1243–1252. https://doi.org/10.2106/JBJS.15.01009
Obermeyer Z, Emanuel EJ (2016) Predicting the future—big data, machine learning, and clinical Medicine. N Engl J Med 375:1216–1219. https://doi.org/10.1056/NEJMp1606181
Funding
The study did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest relevant to this article.
Informed consent
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chen, T.LW., Buddhiraju, A., Seo, H.H. et al. Can machine learning models predict prolonged length of hospital stay following primary total knee arthroplasty based on a national patient cohort data?. Arch Orthop Trauma Surg 143, 7185–7193 (2023). https://doi.org/10.1007/s00402-023-05013-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-023-05013-7