Abstract
Purpose
There is growing interest around short stems as they provide a less invasive approach for total hip arthroplasty preserving bone stock for a possible revision surgery if required. The main purpose of this work was to assess the long-term performance of an uncemented metaphyseal short stem in terms of survival rate and in addition its clinical and radiological outcomes.
Materials and methods
From January to December 2010, we prospectively enrolled all consecutive patients undergoing primary total hip arthroplasty with an uncemented metaphyseal short stem in our institution with a minimum follow-up of 10 years. The radiographic features investigated were the varus–valgus stem orientation, areas of osteolysis and radiolucencies, stress shielding, and heterotopic calcifications. The clinical outcomes were measured using the HHS.
Results
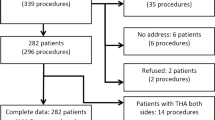
A total of 163 patients (172 hips) were finally included and the measured survival rate at 10 years was 99.6%. The average HHS increased from 55.0 preoperatively to 97.8 at the last follow-up (p < 0.0001). Among them, 137 patients (164 hips) were also available for radiographic assessment. Mild varus malalignment was observed in 40% of cases and remained stable in the serial X-rays and was not associated with step loosening. Mild stress shielding was observed around 13 stems (9%) and moderate only around 3 implants.
Conclusion
In conclusion, the uncemented metaphyseal short stems showed excellent survival and clinical results at 10 years and at a radiographical level very low stress shielding was observed; moreover, besides the high frequency of varus alignment the implanted stems was not associated with revision surgery or with worse clinical outcomes.



Similar content being viewed by others
Availability of data and materials
Available data are currently under transfer on a digital data repository that will be available soon.
Code availability
No code is available yet.
References
Mäkelä KT, Matilainen M, Pulkkinen P et al (2014) Failure rate of cemented and uncemented total hip replacements: register study of combined Nordic database of four nations. BMJ 348:f7592. https://doi.org/10.1136/bmj.f7592
Mäkelä KT, Eskelinen A, Pulkkinen P et al (2008) Total hip arthroplasty for primary osteoarthritis in patients fifty-five years of age or older. An analysis of the Finnish arthroplasty registry. J Bone Jt Surg Am 90:2160–2170. https://doi.org/10.2106/JBJS.G.00870
Mäkelä KT, Eskelinen A, Pulkkinen P et al (2011) Results of 3,668 primary total hip replacements for primary osteoarthritis in patients under the age of 55 years. Acta Orthop 82:521–529. https://doi.org/10.3109/17453674.2011.618908
Khanuja HS, Banerjee S, Jain D et al (2014) Short bone-conserving stems in cementless hip arthroplasty. J Bone Jt Surg Am 96:1742–1752. https://doi.org/10.2106/JBJS.M.00780
Rometsch E, Bos PK, Koes BW (2012) Survival of short hip stems with a “modern”, trochanter-sparing design—a systematic literature review. Hip Int 22:344–354. https://doi.org/10.5301/HIP.2012.9472
Banerjee S, Pivec R, Issa K et al (2013) Outcomes of short stems in total hip arthroplasty. Orthopedics 36:700–707. https://doi.org/10.3928/01477447-20130821-06
Goebel D, Schultz W (2009) The Mayo cementless femoral component in active patients with osteoarthritis. Hip Int 19:206–210. https://doi.org/10.1177/112070000901900303
Malahias M-A, Tejaswi P, Chytas D et al (2021) The clinical outcome of the Metha short hip stem: a systematic scoping review. Hip Int 31:24–33. https://doi.org/10.1177/1120700020903719
Schnurr C, Schellen B, Dargel J et al (2017) Low short-stem revision rates: 1–11 year results from 1888 total hip arthroplasties. J Arthroplasty 32:487–493. https://doi.org/10.1016/j.arth.2016.08.009
Wittenberg RH, Steffen R, Windhagen H et al (2013) Five-year results of a cementless short-hip-stem prosthesis. Orthop Rev (Pavia) 5:e4. https://doi.org/10.4081/or.2013.e4
Liang H-D, Yang W-Y, Pan J-K et al (2018) Are short-stem prostheses superior to conventional stem prostheses in primary total hip arthroplasty? A systematic review and meta-analysis of randomised controlled trials. BMJ Open 8:e021649. https://doi.org/10.1136/bmjopen-2018-021649
Ishaque BA (2022) Short stem for Total Hip Arthroplasty (THA)—overview, patient selection and perspectives by using the Metha® hip stem system. Orthop Res Rev 14:77–89. https://doi.org/10.2147/ORR.S233054
Jawad MU, Scully SP (2011) In brief: Crowe’s classification: arthroplasty in developmental dysplasia of the hip. Clin Orthop Relat Res 469:306–308. https://doi.org/10.1007/s11999-010-1316-6
Kacmaz IE, Turgut A, Basa CD et al (2022) Comparison of the reliability of three scoring systems used to decide whether to apply cement in hip arthroplasty among fracture patients and the effect of surgical experience: the spotorno, dorr, and canal flare indices. J Arthroplasty 37:1348–1353. https://doi.org/10.1016/j.arth.2022.03.062
Zini R, Longo UG, de Benedetto M et al (2013) Arthroscopic management of primary synovial chondromatosis of the hip. Arthroscopy 29:420–426. https://doi.org/10.1016/j.arthro.2012.10.014
Nishioka ST, Andrews SN, Mathews K, Nakasone CK (2022) Varus malalignment of short femoral stem not associated with post-hip arthroplasty fracture. Arch Orthop Trauma Surg 142:3533–3538. https://doi.org/10.1007/s00402-021-04244-w
Grappiolo G, Blaha JD, Gruen TA et al (2002) Primary total hip arthroplasty using a grit-blasted, press-fit femoral prosthesis. Long-term results with survivorship analysis. Hip Int 12:55–72. https://doi.org/10.5301/HIP.2008.3845
Engh CA, Bobyn JD (1988) The influence of stem size and extent of porous coating on femoral bone resorption after primary cementless hip arthroplasty. Clin Orthopaed Related Res 231:7
Brooker AF, Bowerman JW, Robinson RA, Riley LH (1973) Ectopic ossification following total hip replacement. Incidence and a method of classification. J Bone Jt Surg Am 55:1629–1632
Gruen TA, McNeice GM, Amstutz HC (1979) “Modes of failure” of cemented stem-type femoral components: a radiographic analysis of loosening. Clin Orthop Relat Res. https://doi.org/10.1097/00003086-197906000-00002
Loppini M, Longo UG, Caldarella E et al (2017) Femur first surgical technique: a smart non-computer-based procedure to achieve the combined anteversion in primary total hip arthroplasty. BMC Musculoskelet Disord 18:331. https://doi.org/10.1186/s12891-017-1688-9
Hug KT, Alton TB, Gee AO (2015) In brief: classifications in brief: Brooker classification of heterotopic ossification after total hip arthroplasty. Clin Orthop Relat Res 473:2154–2157. https://doi.org/10.1007/s11999-014-4076-x
Toci GR, Magnuson JA, DeSimone CA et al (2022) A systematic review and meta-analysis of non-database comparative studies on cemented versus uncemented femoral stems in primary elective total hip arthroplasty. J Arthroplasty S0883–5403(22):00388–00396. https://doi.org/10.1016/j.arth.2022.03.086
Nadorf J, Thomsen M, Gantz S et al (2014) Fixation of the shorter cementless GTS™ stem: biomechanical comparison between a conventional and an innovative implant design. Arch Orthop Trauma Surg 134:719–726. https://doi.org/10.1007/s00402-014-1946-3
Kutzner KP, Freitag T, Donner S et al (2017) Outcome of extensive varus and valgus stem alignment in short-stem THA: clinical and radiological analysis using EBRA-FCA. Arch Orthop Trauma Surg 137:431–439. https://doi.org/10.1007/s00402-017-2640-z
Lee B-S, Cho H-I, Bin S-I et al (2018) Femoral component varus malposition is associated with tibial aseptic loosening after TKA. Clin Orthop Relat Res 476:400–407. https://doi.org/10.1007/s11999.0000000000000012
Morales de Cano JJ, Gordo C, Illobre JM (2014) Early clinical results of a new conservative hip stem. Eur J Orthop Surg Traumatol 24:359–363. https://doi.org/10.1007/s00590-013-1198-x
Morales De Cano JJ, Molina RC, Puertolas ET (2022) Medium-term outcomes of short stems in total hip arthroplasty. J Orthopaed Trauma Rehabilit 29:22104917221092164. https://doi.org/10.1177/22104917221092165
Cherian JJ, Jauregui JJ, Banerjee S et al (2015) What host factors affect aseptic loosening after THA and TKA? Clin Orthop Relat Res 473:2700–2709. https://doi.org/10.1007/s11999-015-4220-2
Biz C, Pavan D, Frizziero A et al (2015) Heterotopic ossification following hip arthroplasty: a comparative radiographic study about its development with the use of three different kinds of implants. J Orthop Surg Res 10:176. https://doi.org/10.1186/s13018-015-0317-2
Kim Y-H, Jang Y-S, Kim E-J (2021) A prospective, randomized comparison of the long-term clinical and radiographic results of an ultra-short vs a conventional length cementless anatomic femoral stem. J Arthroplasty 36:1707–1713. https://doi.org/10.1016/j.arth.2020.12.030
Funding
FMG, MS, KC, and EM declare they have no financial interests. ML has received royalties and speaker and consultant honoraria from the company Zimmer Biomet. In addition, he received research funding through a national research grant (GR-2018-12367275) to IRCCS Humanitas Research Hospital, from Italian Ministry of Health. GG has received royalties and speaker and consultant honoraria from the companies Zimmer Biomet, Innomed, and Adler Ortho.
Author information
Authors and Affiliations
Contributions
All the authors contributed to the study conception and design. Material preparation, and data collection and analysis were performed by FMG and MS. The first draft of the manuscript was written by ML and all the authors commented on previous versions of the manuscript. All the authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
FMG, MS, KC, and EM have no competing interests to declare that are relevant to the content of this article. ML has received royalties and speaker and consultant honoraria from the company Zimmer Biomet. In addition, he received research funding through a national research grant (GR-2018-12367275) to IRCCS Humanitas Research Hospital, from Italian Ministry of Health. GG has received royalties and speaker and consultant honoraria from the companies Zimmer Biomet, Innomed, and Adler Ortho.
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Ethical Committee of Humanitas Research Hospital (protocol number: 1907, date January 2010).
Consent to participate
Informed consent was obtained from all individual participants included in this study.
Consent to publish
The authors affirm that human research participants provided informed consent for publication of the images in Figs. 1, 2 and 3.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Grappiolo, G., Gambaro, F.M., Spera, M. et al. Clinical and radiological outcomes of an uncemented metaphyseal short stem at minimum 10 years of follow-up: a prospective observational study. Arch Orthop Trauma Surg 144, 425–431 (2024). https://doi.org/10.1007/s00402-023-05012-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-023-05012-8