Abstract
Introduction
Fragility fractures (FF) are associated with increased morbidity and mortality and reflect a dramatic turning point in the life of older adults. The scientific discourse is dominated by proximal femoral fractures, but FF affect multiple parts of the body and often precede hip fractures. Orthogeriatric co-management has multiple shown to improve patient’s outcome. We hypothesize that all geriatric patients with FF benefit from orthogeriatric co-management.
Materials and methods
We retrospectively evaluated all patients over 70 years with FF (hip joint, periprosthetic, spine, pelvic ring, and humerus) of our geriatric trauma center for the years 2019–2021, who received orthogeriatric co-management. Demographic data, fracture type, complications, discharge modality and in-hospital mortality were recorded. For patients transferred to geriatrics, the Barthel Index (BI) and the discharge modality were recorded. Primary outcome parameters were discharge modality and BI difference. Secondary outcome parameters were complication rates and in-hospital mortality. Logistic regression analysis was performed.
Results
555 patients (83.8 ± 6.5 years, 182 males, 373 females) were evaluated. 245 (44.1%) patients were referred to geriatrics for further orthogeriatric treatment. Positive predictors were age, surgery, and a high Charlson Comorbidity Index. The overall in-hospital mortality was 8.6% (n = 48) (5.8% (n = 32) during acute trauma care and 6.5% (n = 16) during stay in geriatrics). The mortality rate of nursing home residents was significantly higher compared to patients living at home (10.4% vs. 5.6%). The rate of non-surgical complications was 44.5%. 26.9% of patients living at home were discharged to a nursing home, while 51.3% were able to return home. The risk of admission to a nursing home was reduced for thoracolumbar fractures (OR = 0.22) and increased markedly for periprosthetic fractures (OR = 3.95). During orthogeriatric treatment, all fractures showed a significant increase in BI. Patients living at home benefited more than nursing home residents (20.5 ± 19.5 vs. 8.7 ± 18.0 points). The chance of a BI increase (> 19 points) was increased for hip and pelvic ring fractures. Devastating results showed patients with dementia. In comparison, mentally healthy patients had a 4.5-fold increased chance of increasing their BI (> 19 points).
Conclusions
Presented data shows that all patients with FF are at high risk for complications and could benefit from standardized orthogeriatric management. Modern patient care requires a holistic orthogeriatric approach to improve patient’s outcome.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Fragility fractures, caused by low-energy trauma, are associated with increased morbidity and mortality and often represent a dramatic turning point in the life of older adults [1,2,3]. Beside their serious impact on individual’s fate, fragility fractures becoming a major burden for healthcare systems and demographic change is expected to further increase fracture-associated costs in the next decades [4].
Geriatric patients are a vulnerable patient group, as they often suffer from multiple comorbidities and functional impairments. Associated with pre-existing limited physical and mental resources the geriatric patient is highly at risk for post-operative complications and increased mortality [5, 6], making treatment of those patients challenging.
Considering above-described developments and the special issues of the geriatric patient the liaison of orthopaedic surgeons and geriatricians in terms of multidisciplinary orthogeriatric care is still an emerging topic [7]. Albeit, different orthogeriatric care models are coexisting [6] an interdisciplinary approach in treating geriatric hip fracture patients has shown to increase postoperative clinical as well as cost-associated outcome measures in terms of length of stay, in-hospital mortality, long-term mortality and postoperative complications [8,9,10].
Hip fractures clearly dominating the scientific discourse [11], but fragility fractures occur in multiple parts of the human body, such as humerus, pelvis, spine or wrist [12] and often precede devastating hip fractures [13]. Data on orthogeriatric care in the course of different fragility fractures is poor [14]. Here, we hypothesize that not only hip fracture patient benefit from orthogeriatric care. For this purpose, we retrospectively evaluated the patient’s outcome of different fracture types in our orthogeriatric care of a level 1 trauma centre.
Materials and methods
All patients ≥ 70 years with hip, proximal femur, periprosthetic, spinal, pelvic, and humerus fractures treated in our level 1 trauma center are routinely screened using the Identification of Seniors at risk (ISAR) score at first day of admission. All patient with ISAR score 2 or higher receive further standardized geriatric assessment and treatment by a geriatric consultant during hospitalization in our traumatology department until discharge. This complex early geriatric rehabilitative treatment includes regular interdisciplinary meetings, development of rehabilitation goals with focus on geriatric syndromes. Patient discharge is managed by social workers, attending surgeons and geriatric consultants. Patients, who discharge from acute trauma center to geriatrics, receive continuously weekly visits by an experienced trauma surgeon. The orthogeriatric care includes occupational therapy, physiotherapy, nutrition counseling, sport therapy and constant supervision by geriatrician and orthopedic trauma surgeons.
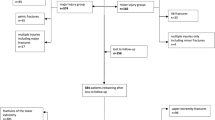
For this study, we retrospectively reviewed all patients of our trauma department in the treatment period from 2019 to 2021 who received geriatric assessment and treatment (Fig. 1). Presented data were obtained with institutional and local ethical committee approval for the use of the data. All patient charts were reviewed for demographical data, type of injury, surgical and non-surgical complications, discharge destination and hospital mortality. In Patients discharged to geriatrics after trauma center Barthel index (BI) and home accommodation before and after treatment was recorded. Primary outcome measures were discharging modality and change in BI during orthogeriatric care. Secondary outcome measures were rate of surgical and non-surgical complications, and hospital mortality. Surgical complications like hematoma, bleeding, surgical site infection, implant failure or fracture displacement were recorded if surgical revision was needed. We recorded major non-surgical complications, like serious cardiovascular (e.g., thrombosis, embolism, infarction, stroke), infectious (pneumonia, urinary tract infection) events as well as acute organ failure (kidney, heart, and liver failure) and anemia requiring red blood cell transfusion.
Data analysis was performed using SPSS (v25.0, Co., IBM, Armonk, NY, USA). Demographic characteristics are described as mean and standard deviation, and categorical data as absolute and relative frequencies. For the primary and secondary categorical outcome measures logistic/ordinal regression was performed considering related variables to prevent confounding. A p-value < 0.05 was considered as statistically significant.
Results
Patient population
For 555 patients, medical records were reviewed. Out of these 555 patients, 182 were male and 373 were female. The youngest patient was 70, while the oldest was 104 years old. The mean age was 83.8 ± 6.5 years with a mean age adjusted Charlson Comorbidity Index (CCI) of 6. There were 128 patients with hip fractures, 158 with proximal femur fractures, 30 with periprosthetic fractures of the proximal femur, 41 with proximal humerus fractures, 93 with pelvic ring fractures, 74 with thoracolumbar fractures and 31 with cervical fractures. Overall, 87.4% (n = 485) of the fractures were treated surgically. Further data and complication rate shows Table 1. Table 2. shows the composition of non-surgical complications.
Discharge from acute trauma care.
Overall, 24.9% (n = 138) of the patients were discharged home, 44.1% (n = 245) into further orthogeriatric care (geriatrics with orthopedic consultant service), 15.3% (n = 85) into a nursing home, 9.9% (n = 55) into another medical department and 5.8% (n = 32) died during acute trauma care. For further analysis logistic regression was performed excluding cases with discharge modalities to another medical department, unknown destination, or death. Patient with high age, surgical treatment, non-surgical complications or high CCI were statistically more often admitted into orthogeriatric care (p < 0.05). Cervical fractures had a significantly higher chance of been released directly home compared to all other (p < 0.05). Discharge modality out of acute trauma care shows Tab. 3.
Outcome of orthogeriatric care
From acute trauma care 245 patients were admitted to geriatrics with weekly orthopedic consultant service for orthogeriatric care. Mean hospital stay in geriatrics was 23.4 ± 13.5 days. During the treatment 12 patients (4.9%) had surgical complications and 109 (44.5%) had non-surgical complications. Out of the 245 patients 197 lived at home and 48 lived in a nursing facility before injury. From the patients living at home 51.3% (n = 101) could return to their homes, while 26.9% (n = 53) were released to a nursing facility. Out of the remaining patients 16.2% (n = 32) were discharged to another hospital and 5.6% (n = 11) of the patients died during hospital stay. Patients living in a nursing facility before the injury showed a significantly higher mortality (5.6% vs 10.4%; p < 0.05). Logistic regression showed that the risk for transfer to a nursing home was lowered by factor 0.22 (p < 0.05) for thoracolumbar fractures and increased by factor 3.95 (p < 0.05) for periprosthetic fractures. Age increased the risk by 1.067 per year of age (p < 0.05) for discharge to a nursing facility. Discharge modality after geriatrics with orthopedic consultant services shows Tab. 4.
BI could be evaluated for 191 out of 245 patients in geriatrics with orthogeriatric care. Mean BI at admission was 35.6 ± 16.0 and improved to a mean value of 51.2 ± 26.4 at discharge. Patients living at home before the injury had a significantly higher improvement compared to people living in a nursing home (20.5 ± 19.5 vs. 8.7 ± 18.0 points; p < 0.05). Logistic regression showed that the chance of BI improvement over 19 points was significantly higher by factor 4.4 for hip fractures and by factor 5.8 for pelvic ring fractures compared to the other injuries (p < 0.05). For patients living at home before injury the chance of BI improvement tended to be significant higher by factor 2.3 (p = 0.067). Improvement of the BI over time for the different injuries shows Fig. 2.
Outcome was heavily influenced by the mental state of the patients. Patients with diagnosed dementia improved significantly less during orthogeriatric care (BI improvement 6.8 ± 17.8 vs. 22.4 ± 18.3 points; p < 0.05). Compared to patients suffering from dementia mentally healthy patients had a 4.5 times higher chance of an improvement above 19 points (p < 0.05). Furthermore, patients with dementia were significantly more often released into a nursing facility (58.5% vs. 36.1%; p < 0.05) and were released earlier out of orthogeriatric care (21.9 d ± 10.0 vs. 28.8 d ± 15.4; p < 0.05).
Discussion
Multidisciplinary orthogeriatric treatment of older hip fracture patients has multiply shown to improve patient’s outcome [8,9,10, 15]. Exemplarily, Prestmo et al. showed a better functional outcome [16] as well as Rapp et al. showed a reduced mortality of hip fracture patients after orthogeriatric care [17]. The aim of this work was to illuminate the outcome of different fragility fractures after orthogeriatric care.
Different orthogeriatric care models are co-existing, like geriatric ward with orthopaedic consultant service, orthopaedic ward with geriatric consultant service or integrated care models. All have shown their benefits on patient’s outcome [5, 8]. In our department we are running a two centre orthogeriatric care model. All patients ≥ 70 years with hip, proximal femur, periprosthetic, spinal, pelvic, and humerus fractures are screened in our traumatology department by ISAR score at admission. Patients with the need of orthogeriatric care (ISAR ≥ 2) receive further assessment and treatment by a geriatric consultant. More than 40% of all patients needed further care and were discharged to orthogeriatric care in geriatrics with high age, surgical treatment, non-surgical complications and high CCI as positive predictors. Patients with cervical spine fractures significant more often returned directly home compared to all other fracture types, which may underline the importance of mobility to avoid further need of care. Contrary to this, patients with cervical spine fractures showed the highest in-hospital mortality. Over 40% of the patients in our study cohort were patients with other fractures separate from fractures of the hip joint and proximal femur, which emphasizes the need for orthogeriatric care during management of other injury types as well.
Mortality after hip fractures is still devastating with 30-day-mortality of around 10% and 1-year-mortality over 20% [17,18,19]. In our patient cohort overall in-patient mortality was 8.6%. During further orthogeriatric care in geriatrics in-patient mortality was 6.5%. Nursing home residents were at a significantly higher risk (10.4%) during inpatient stay compared to patients living at home (5.6%). Considering, that fragility fractures of different modalities are compared to hip fractures, observed mortality is still high and emphasizes the need of orthogeriatric care not only for hip fracture patients. Similarly, Wiedl et al. observed an increased mortality after “major fragility fractures”—like pelvic, hip or thoracolumbar fractures—compared to “minor fragility fractures”—like upper extremity, cervical spine or rib fractures—in 1-year but not in 2-year follow-up [14].
During orthogeriatric care overall rate of surgical complication was lower than 5%, with clear discrepancy between different fracture types, as surgical complication rate in proximal humerus fractures reached 12.1%. Rate of non-surgical complications—like for e.g., pneumonia, delirium, heart, and kidney failure—reached 44.5%. In a meta-analysis of surgery geriatric patients, excluding cardiac surgery patients, Luger et al. reported postoperative complication rates between 6.9 and 25% [20]. The German national hip fracture database reports a non-surgical complication rate of approximately 10% after hip fractures [21, 22]. Flikweert et al. stated a long-term complication rate of 75% during 6 months after surgery, whereas half where classified as major complications [23]. Observed differences may arise from different recording periods and recording modalities but our reported non-surgical complication rate is located at the upper end compared to rates from literature [23,24,25,26], which may show that our screening successfully identified high-risk patients. In addition, it must be noted that all patients with frailty fractures are at high risk for complications, with injuries of the proximal femur as major risk factor.
More than half of patients living at home before fracture event could return to their home, while one quarter of patients were released to a nursing home. The risk for transfer to a nursing facility was lower for patients with thoracolumbar fractures (OR = 0.22) and increased multiple for periprosthetic fractures (OR = 3.95), which identifies periprosthetic fractures as a high-risk factor for need of long-term care. Observed poor outcome may be due to required limited weight bearing after surgical care and might be causal for observed poor improvement of BI in periprosthetic fracture patients.
The BI was recorded as marker for patient’s independence and need of care. Patients in orthogeriatric care showed significant improvement of BI between admission and at discharge. Patients living at home before fracture showed a significant higher improvement compared to nursing home residents (20.5 ± 19.5 vs. 8.7 ± 18.0 points; p < 0.05). Poor outcome of nursing home residents after fragility fractures is commonly known. Gosh et al. observed a 1-year-mortality rate of 29.4% in a group of long-term care residents after fragility fractures and orthogeriatric co-management. But, the author also found an BI improvement from day 5 to 3-month follow-up in nursing home residents, which indicates an existing rehabilitation potential [27]. The chance of Barthel index improvement over 19 points was significantly increased in patients with hip fractures and pelvic ring fractures. This finding may be attributed to patient’s regained mobility during orthogeriatric care.
Devastating results showed patients with diagnosed dementia. Those patients benefitted significant less from orthogeriatric care compared to mentally healthy patients, who had a 4.5 higher chance to improve Barthel index over 19 points. Our results identify dementia patients as highly vulnerable and with little recovery potential. Poor recovery progress may have resulted in observed significantly earlier discharge from orthogeriatric care of dementia patients. Future challenges consist in developing specific dementia programs to improve outcomes of this special patient group. Our findings are supported by hip fracture data, as dementia patients are identified as high-risk patients with less functional recovery potential and increased mortality [28, 29].
Data on the outcome of orthogeriatric care in the course of different fragility fractures besides hip fractures is lacking. We and few others could show that all geriatric patients are at high-risk for non-surgical complications and benefit from a standardised orthogeriatric assessment regardless of fracture modality [14, 27, 30]. Therefore, for a modern holistic orthogeriatric approach it is crucial to identify high-risk patients that require special care to improve our patient’s outcome and to enable a better use of the limited resources of healthcare systems.
Due to the retrospective design, one limitation of our study is a missing follow-up that should be part of future studies. Additionally, factors affecting patient’s outcome are multifactorial. Exemplarily, Luger et al. showed in a meta-analysis that type of anaesthesia affects morbidity and mortality of geriatric surgery patients [20]. We did not record the anaesthesia modality for the surgical patients. Therefore, further work could examine the influence of other factors, such as duration of the surgery, type of anaesthesia or bleeding management, on patient outcome.
Conclusion
All patients with fragility fractures are at high risk for non-surgical complications and benefit from standardised orthogeriatric co-management. This work identifies several risk factors associated with a poor outcome, as dementia and periprosthetic fracture patients benefit significantly less from orthogeriatric care, while hip fracture patients benefit significantly, but showed the highest rate of transfer to a nursing home.
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request, [CP].
References
Hertz K, Santy-Tomlinson J (eds) (2018) Fragility fracture nursing. Holistic Care and Management of the Orthogeriatric Patient, Cham
Pioli G, Bendini C, Pignedoli P et al (2018) Orthogeriatric co-management-managing frailty as well as fragility. Injury 49:1398–1402. https://doi.org/10.1016/j.injury.2018.04.014
Dyer SM, Crotty M, Fairhall N et al (2016) A critical review of the long-term disability outcomes following hip fracture. BMC Geriatr 16:1–18. https://doi.org/10.1186/s12877-016-0332-0
Borgström F, Karlsson L, Ortsäter G et al (2020) Fragility fractures in Europe: burden, management and opportunities. Arch Osteoporos 15:1–21. https://doi.org/10.1007/s11657-020-0706-y
Kammerlander C, Roth T, Friedman SM et al (2010) Ortho-geriatric service—a literature review comparing different models. Osteoporos Int 21:637–646. https://doi.org/10.1007/s00198-010-1396-x
Moyet J, Deschasse G, Marquant B et al (2019) Which is the optimal orthogeriatric care model to prevent mortality of elderly subjects post hip fractures? A systematic review and meta-analysis based on current clinical practice. Int Orthop 43:1449–1454. https://doi.org/10.1007/s00264-018-3928-5
Ranhoff AH, Saltvedt I, Frihagen F et al (2019) Interdisciplinary care of hip fractures.: orthogeriatric models, alternative models, interdisciplinary teamwork. Best Pract Res Clin Rheumatol 33:205–226. https://doi.org/10.1016/j.berh.2019.03.015
van Heghe A, Mordant G, Dupont J et al (2021) Effects of orthogeriatric care models on outcomes of hip fracture patients: a systematic review and meta-analysis. Calcif Tissue Int 110:162–184. https://doi.org/10.1007/s00223-021-00913-5
Patel JN, Klein DS, Sreekumar S et al (2020) Outcomes in multidisciplinary team-based approach in geriatric hip fracture care: a systematic review. J Am Acad Orthop Surg 28:128–133. https://doi.org/10.5435/JAAOS-D-18-00425
Grigoryan KV, Javedan H, Rudolph JL (2014) Orthogeriatric care models and outcomes in hip fracture patients: a systematic review and meta-analysis. J Orthop Trauma 28:e49-55. https://doi.org/10.1097/BOT.0b013e3182a5a045
Bastian JD, Meier MK, Ernst RS et al (2022) A bibliometric analysis of orthogeriatric care: top 50 articles. Eur J Trauma Emerg Surg 48:1673–1682. https://doi.org/10.1007/s00068-021-01715-y
Migliorini F, Giorgino R, Hildebrand F et al (2021) Fragility fractures: risk factors and management in the elderly. Medicina (Kaunas). https://doi.org/10.3390/medicina57101119
Schnell AD, Curtis JR, Saag KG (2018) Importance of recent fracture as predictor of imminent fracture risk. Curr Osteoporos Rep 16:738–745. https://doi.org/10.1007/s11914-018-0487-z
Wiedl A, Förch S, Fenwick A et al (2022) Orthogeriatric co-management: differences in outcome between major and minor fractures. Eur J Trauma Emerg Surg 48:2953–2966. https://doi.org/10.1007/s00068-022-01974-3
Folbert EC, Hegeman JH, Vermeer M et al (2017) Improved 1-year mortality in elderly patients with a hip fracture following integrated orthogeriatric treatment. Osteoporos Int 28:269–277. https://doi.org/10.1007/s00198-016-3711-7
Prestmo A, Saltvedt I, Helbostad JL et al (2016) Who benefits from orthogeriatric treatment? Results from the Trondheim hip-fracture trial. BMC Geriatr 16:49. https://doi.org/10.1186/s12877-016-0218-1
Rapp K, Becker C, Todd C et al (2020) The association between orthogeriatric co-management and mortality following hip fracture: an observational study of 58000 patients from 828 hospitals. Dtsch Arztebl Int 117:53–59. https://doi.org/10.3238/arztebl.2020.0053
Åhman R, Siverhall PF, Snygg J et al (2018) Determinants of mortality after hip fracture surgery in Sweden: a registry-based retrospective cohort study. Sci Rep. https://doi.org/10.1038/s41598-018-33940-8
Asheim A, Marie Nilsen S, Toch-Marquardt M et al (2018) Time of admission and mortality after hip fracture: a detailed look at the weekend effect in a nationwide study of 55,211 hip fracture patients in Norway. Acta Orthop 89:610–614. https://doi.org/10.1080/17453674.2018.1533769
Luger TJ, Kammerlander C, Luger MF et al (2014) Mode of anesthesia, mortality and outcome in geriatric patients. Z Gerontol Geriatr. https://doi.org/10.1007/s00391-014-0611-3
IQTIG - Institut für Qualitätssicherung und Transparenz im Gesundheitswesen (2021) Bundesauswertung zum Erfassungsjahr 2020 - Hüftendoprothesenversorgung: Qualitätsindikatoren und Kennzahlen. IQTIG - Institut für Qualitätssicherung und Transparenz im Gesundheitswesen, Berlin
IQTIG - Institut für Qualitätssicherung und Transparenz im Gesundheitswesen (2021) Bundesauswertung zum Erfassungsjahr 2020 - Hüftgelenknahe Femurfraktur mit osteosynthetischer Versorgung: Qualitätsindikatoren und Kennzahlen. IQTIG - Institut für Qualitätssicherung und Transparenz im Gesundheitswesen, Berlin
Flikweert ER, Wendt KW, Diercks RL et al (2018) Complications after hip fracture surgery: are they preventable? Eur J Trauma Emerg Surg 44:573–580. https://doi.org/10.1007/s00068-017-0826-2
Dy CJ, Dossous P-M, Ton QV et al (2012) The medical orthopaedic trauma service: an innovative multidisciplinary team model that decreases in-hospital complications in patients with hip fractures. J Orthop Trauma 26:379–383. https://doi.org/10.1097/BOT.0b013e3182242678
Roche JJW, Wenn RT, Sahota O et al (2005) Effect of comorbidities and postoperative complications on mortality after hip fracture in elderly people: prospective observational cohort study. BMJ Med 331:1374. https://doi.org/10.1136/bmj.38643.663843.55
Leung AH-C, Lam T-P, Cheung W-H et al (2011) An orthogeriatric collaborative intervention program for fragility fractures: a retrospective cohort study. J Trauma 71:1390–1394. https://doi.org/10.1097/TA.0b013e31821f7e60
Gosch M, Hoffmann-Weltin Y, Roth T et al (2016) Orthogeriatric co-management improves the outcome of long-term care residents with fragility fractures. Arch Orthop Trauma Surg 136:1403–1409. https://doi.org/10.1007/s00402-016-2543-4
Hou M, Zhang Y, Chen AC et al (2021) The effects of dementia on the prognosis and mortality of hip fracture surgery: a systematic review and meta-analysis. Aging Clin Exp Res 33:3161–3172. https://doi.org/10.1007/s40520-021-01864-5
Schuetze K, Eickhoff A, Rutetzki K-S et al (2022) Geriatric patients with dementia show increased mortality and lack of functional recovery after hip fracture treated with hemiprosthesis. Eur J Trauma Emerg Surg 48:1827–1833. https://doi.org/10.1007/s00068-020-01472-4
Hafner T, Kollmeier A, Laubach M et al (2021) Care of geriatric patients with lumbar spine, pelvic, and acetabular fractures before and after certification as a geriatric trauma center DGU®: a retrospective cohort study. Medicina (Kaunas). https://doi.org/10.3390/medicina57080794
Funding
Open Access funding enabled and organized by Projekt DEAL. This research received no external funding. No author received or will receive any form of payment related to this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there is no conflict of interest. No company had influence in the collection of data, contributed to, or had influence on the conception, design, analysis and writing of the study. No further funding was received.
Ethical approval
This article does not contain any studies with human participants or animals. All presented data were obtained with permission of the local ethical committee and stored anonymously.
Informed consent
For this retrospective chart review informed consent was not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Pankratz, C., Risch, A., Oxen, J. et al. Orthogeriatric care—outcome of different fragility fractures. Arch Orthop Trauma Surg 143, 6641–6647 (2023). https://doi.org/10.1007/s00402-023-04993-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-023-04993-w