Abstract
Background
Total knee arthroplasty are among the most frequently conducted surgeries, due to an aging society. Since hospital costs are subsequently rising, adequate preparation of patients and reimbursement becomes more and more important. Recent literature revealed anemia as a risk factor for enhanced length of stay (LOS) and complications. This study analyzed whether preoperative hemoglobin (Hb) and postoperative Hb were associated with total hospital costs and general ward costs.
Methods
The study comprised 367 patients from a single high-volume hospital in Germany. Hospital costs were calculated with standardized cost accounting methods. Generalized linear models were applied to account for confounders, such as age, comorbidities, body mass index, insurance status, health-related quality of life, implant types, incision-suture-time and tranexamic acid.
Results
Preoperative anemic women had 426 Euros higher general ward costs (p < 0.01), due to increased LOS. For men, 1 g/dl less Hb loss between the preoperative value and the value before discharge reduced total costs by 292 Euros (p < 0.001) and 161 Euros fewer general ward costs (p < 0.001). Total hospital costs were reduced by 144 Euros with 1 g/dl higher Hb on day 2 postoperatively for women (p < 0.01).
Conclusion
Preoperative anemia was associated with increased general ward costs for women and Hb loss with decreasing total hospital costs for men and women. Cost containment, especially reduced utilization of the general ward, may be feasible with the correction of anemia for women. Postoperative Hb values may be a factor for adjustments of reimbursement systems.
Level of evidence
Retrospective cohort study, III.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
End-stage osteoarthritis (OA) is a global burden with a high prevalence, due to an aging society, with total knee arthroplasty (TKA) as a common surgery to improve pain and function [16]. The problem of rising costs for healthcare systems entails the challenge of preparing patients appropriately and designing adequate reimbursement systems. Recently, comorbidities were investigated as risk factors for high costs, especially for patients who exceeded the bundled-payment system for total joint replacements (TJR) in the US [15, 39]. One of the possible modifiable comorbidities was preoperative anemia, which increased the total episode of care costs [15, 39]. Patients with revision total hip arthroplasty and iron deficiency anemia had higher length of stay (LOS), exceeded costs in the bundled-payment system and more complications compared to patients without anemia [32]. For primary total hip arthroplasty (THA), anemic patients below 11 g/dl Hb had higher LOS and below 12 g/dl further risk assessments were recommended [30]. The total episode of care costs in the bundled payment system includes all costs, until 90 days after discharge from the hospital [21]. Hence, risk adjusted pricing was recommended, because without adequate adjustments special patient groups may lose access to TJR [21]. Hospitals in the US had higher charges on the day of surgery, readmissions and emergency visits for patients with THA and preoperative iron deficiency anemia [29]. Similarly, poorer outcomes were found for anemic TKA patients [19]. Utilizing a cost simulation model for THA and TKA, a Swedish study found increased costs for nursing days and reduced transfusion costs during the hospital stay for patients with preoperative correction of iron deficiency anemia [37]. Patients who attended a blood management program had lower risk for blood transfusions, postoperative complications, and LOS for primary arthroplasties [1]. However, just a part of the anemic patients, who attended the blood management program, were no longer anemic at the day of surgery [1]. This shows that preoperative anemia may be corrected partly, but not for all patients undergoing TKA. Guidelines about preoperative anemia are currently under consideration in Germany and no clear recommendations for preparing anemic patients exist [7]. The increased LOS and higher complication rates for those patients indicate higher resource utilization and thereof higher hospital costs. LOS is especially relevant for nursing and the general ward, because the longer the patients need care, the higher the costs. Last, but clearly not least, preoperative as well as postoperative anemia is associated with increased morbidity, mortality [24] and infection rate [26].
Due to the challenging correction of anemia preoperatively, the correction of iron deficiency anemia is also done postoperatively, but the improvements were not immediately significant during the hospital stay [18]. Additionally, postoperative moderate and severe anemia was associated with preoperative Hb values and intraoperative blood loss for TKA [4]. Preoperative Hb for men < 13.85 g/dl and < 13.15 g/dl for women resulted in moderate or severe anemia, postoperatively [4]. Additionally, to the treatment of iron deficiency anemia with iron supplements, tranexamic acid (TRX) is applied intraoperatively, because it is regarded to be effective for reducing blood loss and transfusion rates for THR and TKA [2, 12]. Due to the reduced transfusion rates with TRX the preoperative screening of patients with TJA was discussed controversially [34, 35].
Since Hb values are important screening parameters, preoperatively and postoperatively, this study investigated their association to hospital costs, in order to bridge the gap between medical care and financial management. The preoperative Hb values were examined, to reveal whether anemia is associated with not only negative effects, such as complications and increased LOS for the patient, but also whether its economic impact may provide a link to cost containment. Associations of preoperative anemia and costs might be an argument for standardized correction of anemia to reduce costs for the healthcare system with simultaneous positive effects for the patients. Although, there may be patient groups where a correction is not feasible, as mentioned implicitly in the discussion about preoperative anemia in the bundled-payment system, which revealed the research gap of postoperative Hb values and their use for risk adjustments into reimbursement systems. In this study the hospital costs were calculated for the reimbursement system of diagnoses related groups (DRG) in Germany. These hospital costs included inpatient costs and were sub-divided into general ward costs, which allowed a detailed analyses of cost components, especially with regard to LOS. An association of these hospital costs with postoperative Hb values may be the basis for risk adjustments in reimbursement systems. To the best of our knowledge this is the first paper to investigate preoperative anemia and its association with hospital costs for TKA as well as the course of postoperative Hb values and their association with hospital costs. In the last decade, transfusion rates were reduced sharply, and surgical techniques were improved, due to TRX. Hence, only patients without transfusions were analyzed to explore whether preoperative and postoperative Hb values were associated with hospital costs. The following research (RQ) questions were developed:
RQ1: Was preoperative anemia associated with increased total hospital costs and general ward costs for TKA?
RQ2: Which postoperative Hb values were associated with total hospital costs and general ward costs for TKA?
Materials and methods
The observational study comprised 367 patients from a single hospital in Germany, which was certified as an arthroplasty center of maximum medical care (endoCert®). The study is a part of the research project Munich Network Health Care Research—MobilE-Net. Patients with primary TKA, due to OA, were retrospectively included. All patients had one TKA, no simultaneous bilateral TKA. This study was approved by the ethics committee of Ludwig-Maximilians-Universität München (reference number: 18–274). All patients had a surgery between 5 August 2019 and 30 November 2020 and signed the consent to participate. The cross-sectional data was split into men and women, because Hb values differ between genders.
Surgical procedure and bleeding management
Anemia screening was performed prior to surgery to rule out preoperative anemia. In case of values below 12 g/dl, a preoperative clarification was performed by the resident physician or specialist and, if possible, treatment was given. Especially in case of iron deficiency anemia, intravenous iron substitution was performed before surgery. Intraoperatively, tranexamic acid was administered intravenously and/or locally, provided there were no contraindications (e.g., condition after thromboembolic events, coronary heart disease and condition after stenting, epilepsy, etc.). Tourniquets or drains were not used.
Thromboprophylaxis was performed in all cases with low-molecular-weight heparin from the evening of the day of surgery for 11–14 days postoperatively according to the applicable guideline. In cases with an increased thromboembolic risk, semi-therapeutic doses were administered from the 3rd postoperative day. In exceptional cases (for example, in the presence of allergies or injection phobias), new oral anticoagulants (NOACs) were also used.
About 10% of patients were on antiplatelet medication (usually aspirin). In patients taking warfarin or other oral anticoagulants prior to surgery, the medication was paused preoperatively and bridged with a low molecular weight heparin if necessary.
TRX was used according to an in-house standard in all cases in which there was no contraindication to its administration, regardless of the presence of preoperative anemia, except patients had a thrombosis, deep vein thrombosis or pulmonary embolism. Additionally, TRX was not given to patients with an apoplex, cardiac infarction or stent implantation within 12 months before surgery.
Hospital costs
Hospital costs were collected for each patient from the financial department of the hospital and were calculated according to the standard of the Institute for the Hospital Remuneration System in Germany [36]. Total hospital costs comprised all inpatient costs. This included direct attributable costs, such as implants and drugs, but also indirect, non-attributable costs, such as general ward costs and the cost for the surgery. Outpatient costs, such as preoperative physician costs, or costs for rehabilitation were not included. 0.5% inflation rate was considered for patients from 2019.
Preoperative anemia and Hb values
Preoperative anemia was included as a binary variable with one indicating anemia and zero otherwise. The definition of anemia follows the suggestions of the World Health Organization (WHO) [38], for men < 13 g/dl and for women < 12 g/dl. There were no patients with a severe preoperative anemia, according to the WHO definition (< 8 g/dl for men and women). Hb values were measured for each patient preoperatively, at the first and second day after the surgery and on the day before discharge. Additionally, the Hb loss as the difference between the preoperative Hb and the Hb on the day before discharge was calculated.
Confounders
Confounders were selected thoroughly, because the cross-sectional, observational data were not randomized. The statistical analyses were based on a regression model, because with univariate statistical tests confounding is not possible. Hence, the study evaluated several variables as confounders, with reasons.
General health before surgery was measured with the EQ VAS (EuroQoL Visual Analog Scale), part of the EQ-5D-5L questionnaire [3]. This confounder served as a proxy for the health status before surgery. This health status was considered relevant, because patients with preoperative anemia might have a lower health status than patients without anemia. Hence, this circumstance was considered with the confounder of the preoperative EQ VAS. Additionally, age and body mass index (BMI) were collected. The age was considered as a relevant confounder, because with the age of patients the costs may vary, due to possible higher care needs of elderly patients. Similarly, for patients with a high BMI, the care needs might be higher as for patients with a normal BMI. As a proxy for the socioeconomic status the insurance status was evaluated, distinguishing between statutory and non-statutory insurance, because Edwards et al. [9] found associations of socioeconomic status and utilization of THA. To control for comorbidities, the ASA Score (American Society of Anesthesiologists Physical Status Classification System) [27] was included as a measure of the anesthetic assessment. Furthermore, Charlson Scores [5] and Elixhauser Scores [11], adapted with weightings for orthopedics from Menendez [22], were calculated from orthopedics’ notes. Patients were categorized into 3 groups, with ascending comorbidities (< 0, = 0, > 0). Comorbidities were considered to be relevant confounders, because patients with a higher comorbidity score might be more costly than patients with a low comorbidity score. Hence, the ASA Score and the Menendez Score were included in the regression model to control for this circumstance. Intraarticular TRX was included as a binary confounder, because TRX reduces generally blood loss during the surgery. Patients with TRX were considered to have a more stable Hb value postoperatively than patients without TRX. The type of implant was previously investigated as a cost driver for joint replacements [31]. Hence, the implant types were included as categorical variables, distinguished between unicompartmental and bicondylar, with and without patella, and constrained versus unconstrained.
Since the study was conducted during the COVID-19 pandemic, the lockdown status was included [28]. The lockdownstatus separated the patients into three groups, namely into patients with a surgery before the first lockdown, during the first lockdown and after the first lockdown, in Germany. This confounder was considered relevant, because during the first lockdown elective surgeries were sharply reduced. Additionally, hospital costs were affected by the COVID-19 pandemic, resulting in higher costs during and after the first lockdown in Germany [28].
Sample corrections
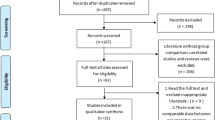
From the 367 patients, 1 patient with 0 Euros total costs, 1 patient with 0 Euros implant costs, 1 patient with 0 days of LOS and 1 patient with a BMI > 200 were excluded, because all these values seemed to be not meaningful. Outliers were detected using boxplots and excluded above and below 1.5 times the 75% quantiles (22 patients). 341 patients remained for the analyses.
Statistical analyses
Generalized linear models (GLM) with gamma distribution and log-link function were applied to account for confounders, due to the positive values of hospital costs. Coefficients below 1 indicate a negative association with the respective costs and coefficients above 1 indicate a positive association. The coefficients were interpreted in percentages of the mean. Anemia and each of the 4 Hb values were included in the models with the same confounders for men and women, referring to total- and ward costs respectively, resulting in 20 models. Model selection was done with the Akaike information criterion (AIC) [8] and the model with the lowest AIC was reported in the results. The pseudo R2 from McFadden was used to evaluate the fit of the models, with a R2 between 0.2 and 0.4 indicating an excellent fit [20]. The minimum threshold for p-values was 0.05. Multicollinearity was detected with the variation inflation factor and a threshold below 2.5 was considered unproblematic [14]. The data collection was done with Microsoft Excel® and the statistical analyses with R [13, 25, 33, 40,41,42].
Sensitivity analyses
Several sensitivity analyses were performed [23]. The main results did not change. Details were reported in the Supplementary material A.
Results
Study cohort
The descriptive results show that 147 men and 194 women received TKA with 21 preoperative anemic men and 21 preoperative anemic women. Total hospital costs were 8119 Euros for men with preoperative anemia and 7859 Euros for men without preoperative anemia. For women, the total hospital costs were 8204 Euros with preoperative anemia and 8015 Euros without preoperative anemia. Total hospital costs for these patients were about 260 Euros higher for men and 189 Euros higher for women with preoperative anemia and total hospital costs were generally higher for women compared to men. Normal ward costs were also increased for patients with preoperative anemia (331 Euros for men, 376 Euros for women). The mean Hb values comprised 11.9 g/dl for men with preoperative anemia and 11.4 g/dl for preoperative anemic women. For patients without preoperative anemia the mean Hb were 14.9 g/dl for men and 13.7 g/dl for women. The course of Hb was similar for both genders, with − 1.8 g/dl for men with preoperative anemia and − 1.6 g/dl for women (without preoperative anemia − 2.8 g/dl for men and − 2.6 g/dl for women). The LOS was increased by 1 day for anemic women, but only by a third of a day for men. TRX was applied by roughly 78% of all patients with very low costs, because the drug costs per patient amounted in approximately 75 Euros. The implant costs were a major cost component with approximately 2000 Euros per patient (Table 1).
Results preoperative anemia
When accounting for confounders, the results for preoperative anemia revealed different findings for men and women. Preoperative anemia increased general ward costs per patient for women by 14.1% compared to patients without anemia, in total approximately 426 Euros. General ward costs for men did not indicate any differences for anemic versus non-anemic patients. Similarly, total costs were not significantly different for preoperative anemic women and preoperative anemic men. Implant types and TRX were significantly associated with general ward costs and total costs for men and women. Whereas incision-suture time was associated with total costs for men and women, but not for general ward costs. The pseudo R2 indicated a relatively good fit for all models (Table 2).
Results postoperative Hb values
For men, the Hb loss between the preoperative Hb and the day before discharge was highly significantly associated with general ward costs and total costs. The general ward costs were reduced by 5.7% (approximately 161 Euros) with 1 g/dl less loss in Hb. The reductions for total costs were 3.7% (approximately 292 Euros) for 1 g/dl less loss in Hb. For women, the Hb on day 2 postoperatively was decisive, but only slightly significant for total costs (p < 0.05) and moderately significant for general ward costs (p < 0.01). General ward costs decreased by 2.6% (approximately 79 Euros) and total costs decreased by 1.8% (approximately 144 Euros) with 1 g/dl increased Hb. (Table 3) All models for postoperative Hb values with its pseudo R2 and AIC are shown in Table B (Supplementary material).
Discussion
The main findings were the association of preoperative anemia for women with higher general ward costs and the association of distinct Hb values with total hospital costs. These findings were generally in line with previous findings about anemic patients, extended LOS, and subsequently higher costs. However, differences exist in sequelae of preoperative anemia between men and women. There were no associations for men with total hospital costs and general ward costs, whereas for women the general ward costs were associated with preoperative anemia due to increased LOS. This indicated that the preoperative Hb is not as important as the reductions for men and TKA. For women, the associations of the Hb on day 2 postoperatively was in line with the findings of previous literature, because it implies that the postoperative Hb depended on the preoperative Hb, already investigated by Cao et al. [4]. The natural process of Hb values with TKA and THA was evaluated by Cho et al. [6] with the focus on blood transfusions. Patients had the lowest Hb on day 3 postoperatively [6]. This is not directly in line with the findings of this study, as the mean Hb value was lowest on the day before discharge. It is worth mentioning that Cho et al. [6] investigated an inpatient period of 2 weeks, which is approximately 5–8 days longer than in Germany. Compared to several years ago, LOS has been reduced dramatically worldwide with TJR being even regularly performed in an outpatient set-up nowadays [10]. Regarding TRX, a recent review on blood management revealed reduced blood transfusion with TRX and therefore less costs [17]. TRX was related to hospital costs for both genders confirming its importance in TKA.
This study revealed that preoperative anemia and the association with general ward costs for TKA patients without blood transfusions was especially a problem for women, but not for men. This was mainly due to increased LOS for women. Whether men would have similar increasing LOS, the general ward costs would be significant, too. Since general ward costs consists to a large extent on personnel costs for nurses, less utilization of caring for patients could be beneficial for nursing shortages. Interestingly, Total hospital costs did not show any association with preoperative anemia, neither for men nor for women. This was due to other major costs components, such as implant types, which were comparable for anemic and non-anemic patients. In sum, cost containment with a correction of anemia may be feasible only for women for general ward costs, because the change in Hb is medically not easy to increase during the hospital stay. Although, for healthcare policy the findings of this study may be a starting point for further research on whether Hb values or other laboratory values could be a screening parameter for high-cost patients, and thus a reason for additional reimbursements for hospitals. The reimbursement system would have to differentiate between genders, because for women the levels of Hb were important and for men the reductions.
This study has several limitations. Due to the cross-sectional- and observational data only associations and no influence was analyzed. Generalizability is small, because only one hospital with a specific patient cohort (TKA due to OA without blood transfusions) was analyzed. There were only 21 women and 21 men with preoperative anemia. This is a relatively small number, hence there might be a bias, due to other reasons than anemia. Patients with blood transfusion were excluded, because the transfusion rate was approximately 1%, which was regarded to be too low for an analysis without a bias. Although the lockdown status for the COVID-19 pandemic was included as a dummy variable, a bias due to the pandemic cannot be excluded. TRX was generally applied for all patients with a consent on the medical information, despite not being approved for this indication. There are few contraindications where TRX was not given, including thrombosis, deep vein thrombosis and pulmonary embolism. Additionally, it was not given whether a patient had an apoplex, cardiac infarction or stent implantation within the last 12 months before surgery. This might cause a bias because patients were not randomly selected with and without TRX. All patients were treated with similar standards and therefore regarded to be comparable with respect to surgical approach and peri- and postoperative care. Nevertheless, there may be biases, due to different surgeons (for example use of tourniquet, drains and local infiltration analgesia). Moreover, the model selection was explorative, hence further confirmation is required. Costs were calculated according to the InEK standard, not distinguishing between direct and indirect costs. General ward costs and total hospital costs included indirect and direct costs. Whether solely the direct or indirect costs would be evaluated, the results might change.
Conclusion
Preoperative anemia was a risk factor for high costs for women and general ward costs, but not for men. Total hospital costs decreased for specific Hb values, especially the difference between discharge and preoperative Hb for men, and day 2 postoperatively for women. Hence, preparation of patients and further development of reimbursement systems should consider both, preoperative anemia, especially for women, and postoperative Hb values. Monitoring Hb values appeared to be a goal congruence between medicine and financial management, because all significant results revealed cost reductions with improved Hb.
Data availability
Data is not publicly available, due to privacy issues.
References
Bailey A, Eisen I, Palmer A, Beaulé PE, Fergusson DA, Grammatopoulos G (2021) Preoperative anemia in primary arthroplasty patients-prevalence, influence on outcome, and the effect of treatment. J Arthroplast 36(7):2281–2289
Bemelmans Y, Van Haaren E, Boonen B, Hendrickx R, Schotanus M (2021) Low blood transfusion rate after implementation of tranexamic acid for fast- track hip- and knee arthroplasty. An observational study of 5205 patients. Acta Orthop Belg 87(1):9–16
Brooks R (1996) EuroQol: the current state of play. Health Policy 37(1):53–72
Cao G, Yang X, Xu H et al (2021) Association between preoperative hemoglobin and postoperative moderate and severe anemia among patients undergoing primary total knee arthroplasty: a single-center retrospective study. J Orthop Surg Res 16(1):572
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40(5):373–383
Cho MR, Jun CM, Song SK, Choi WK (2021) Natural course of hemoglobin level after total knee arthroplasty and the benefit of tranexamic acid injection in the joint. Medicine (Baltimore) 100(35):e27097
Deutsche Gesellschaft für Anästhesiologie und Intensivmedizin (2018) S3 Leitlinie Präoperative Anämie. AWMF Das Portal der wissenschaftlichen Medizin
Dunn PK, Smyth GK (2018) Generalized linear models with examples in R. Springer, New York
Edwards NM, Varnum C, Overgaard S, Pedersen AB (2021) The impact of socioeconomic status on the utilization of total hip arthroplasty during 1995–2017: 104,055 THA cases and 520,275 population controls from national databases in Denmark. Acta Orthop 92(1):29–35
Edwards PK, Milles JL, Stambough JB, Barnes CL, Mears SC (2019) Inpatient versus outpatient total knee arthroplasty. J Knee Surg 32(8):730–735
Elixhauser A, Steiner C, Harris DR, Coffey RM (1998) Comorbidity measures for use with administrative data. Med Care 36(1):8–27
Fillingham YA, Ramkumar DB, Jevsevar DS et al (2018) The efficacy of tranexamic acid in total knee arthroplasty: a network meta-analysis. J Arthroplast 33(10):3090-3098.e3091
Gasparini A (2018) Comorbidity: an R package for computing comorbidity scores. J Open Source Softw 3(23):648–650
Johnson DJ, Greenberg SE, Sathiyakumar V et al (2015) Relationship between the Charlson Comorbidity Index and cost of treating hip fractures: implications for bundled payment. J Orthop Traumatol 16(3):209–213
Karas V, Kildow BJ, Baumgartner BT et al (2018) Preoperative patient profile in total hip and knee arthroplasty: predictive of increased Medicare payments in a bundled payment model. J Arthroplast 33(9):2728-2733.e2723
Kloppenburg M, Berenbaum F (2020) Osteoarthritis year in review 2019: epidemiology and therapy. Osteoarthr Cartil 28(3):242–248
Lu Q, Peng H, Zhou GJ, Yin D (2018) Perioperative blood management strategies for total knee arthroplasty. Orthop Surg 10(1):8–16
Maniar AR, Mishra A, Sanghavi N, Maniar RN (2022) Does postoperative intravenous ferric carboxymaltose hasten the recovery of hemoglobin in patients post total knee arthroplasty? J Arthroplast 37(6s):S155-s158
Mathew KK, Vakharia RM, Salem HS et al (2020) Is iron deficiency anemia a risk factor for poorer outcomes in primary total knee arthroplasty? J Arthroplast 35(5):1252–1256
McFadden D (1977) Quantitative methods for analysing travel behaviour of individuals: some recent developments. Cowles Found 474:279–318
McLawhorn AS, Buller LT (2017) Bundled payments in total joint replacement: keeping our care affordable and high in quality. Curr Rev Musculoskelet Med 10(3):370–377
Menendez ME, Neuhaus V, Ring D (2015) Inpatient mortality after orthopaedic surgery. Int Orthop 39(7):1307–1314
Mihaylova B, Briggs A, O’Hagan A, Thompson SG (2011) Review of statistical methods for analysing healthcare resources and costs. Health Econ 20(8):897–916
Neuwirth AL, Boddapati V, Held MB et al (2022) Preoperative anemia is associated with 30-day morbidity in total knee arthroplasty. Orthopedics 45(2):e86–e90
R Core Team (2020) R: a language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria. https://www.eea.europa.eu/data-and-maps/indicators/oxygen-consuming-substances-in-rivers/r-development-core-team-2006. Accessed 5 Apr 2022
Ren X, Ling L, Qi L et al (2021) Patients’ risk factors for periprosthetic joint infection in primary total hip arthroplasty: a meta-analysis of 40 studies. BMC Musculoskelet Disord 22(1):776
Saklad M (1941) Grading of patients for surgical procedures. Anesthesiology 2(3):281–284
Schatz C, Leidl R, Plötz W, Bredow K, Buschner P (2022) Preoperative patients’ health decrease moderately, while hospital costs increase for hip and knee replacement due to the first COVID-19 lockdown in Germany. Knee Surg Sports Traumatol Arthrosc 30(10):3304–3310
Sequeira SB, Quinlan ND, Althoff AD, Werner BC (2021) Iron deficiency anemia is associated with increased early postoperative surgical and medical complications following total hip arthroplasty. J Arthroplast 36(3):1023–1028
Sicat CS, Muthusamy N, Singh V, Davidovitch RI, Slover JD, Schwarzkopf R (2022) Impact of preoperative anemia severity on primary total hip arthroplasty outcomes. J Arthroplast 37(4):721–726
Stargardt T (2008) Health service costs in Europe: cost and reimbursement of primary hip replacement in nine countries. Health Econ 17(1 Suppl):S9-20
Sylla MM, Gruffi L, Roth ES, Rosato FE, Wong CHJ, Razi AE (2021) How does iron deficiency anemia impact outcomes following revision total hip arthroplasty? Hip Pelvis 33(3):140–146
Tingeley D, Yamamoto T, Hirose K, Keele L, Imai K (2004) Mediation: R package for cuasal mediation analysis. J Stat Softw 59(5):1–38
Vestermark GL, Rowe TM, Martin JR, Odum SM, Springer BD, Fehring TK (2020) In the era of tranexamic acid, are type and screens for primary total joint arthroplasty obsolete? J Arthroplasty 35(9):2363–2366
Vestermark GL, Rowe TM, Martin JR, Odum SM, Springer BD, Fehring TK (2020) Response to Letter to the Editor on ‘In the era of tranexamic acid, are type and screens for primary total joint arthroplasty obsolete?’ J Arthroplast 35(10):3057–3058
Vogl M (2012) Assessing DRG cost accounting with respect to resource allocation and tariff calculation: the case of Germany. Health Econ Rev 2(1):15
Wan S, Sparring V, Cabrales DA, Jansson K, Wikman A (2020) Clinical and budget impact of treating preoperative anemia in major orthopedic surgery—a retrospective observational study. J Arthroplast 35(11):3084–3088
WHO, World Health Organization (2011) Haemoglobin concentrations for the diagnosis of anemia and assessment of severity. WHO guidelines
Wodowski AJ, Pelt CE, Erickson JA, Anderson MB, Gililland JM, Peters CL (2019) ‘Bundle busters’: who is at risk of exceeding the target payment and can they be optimized? Bone Jt J 101-b(7_Supple_C):64–69
Zeileis A (2004) Econometric computing with HC and HAC covariance matrix estimators. J Stat Softw 11(10):1–17
Zeileis A, Hothorn T (2002) Diagnostic checking in regression relationships. R News 2(3):7–10
Zeileis A, Köll S, Graham N (2020) Various versatile variances: an object-oriented implementation of clustered covariances in R. J Stat Softw 95(1):1–36
Acknowledgements
The authors would like to thank Ardit Gashi for feedback on an earlier draft of this article, Antonia Marx for the collection of medical data and the administrative staff of the participating hospital for providing cost- and laboratory data.
Funding
Open Access funding enabled and organized by Projekt DEAL. This work is part of the project “Munich Network Health Care Research—MobilE-Net” and was funded by the German Federal Ministry of Education and Research Grant number 01GY1603A.
Author information
Authors and Affiliations
Contributions
CS conceptualization, data analyzes and interpretation, writing—main manuscript. WP funding, supervision, writing—review and editing. JB supervision, writing—review and editing. KB writing—main manuscript, data collection. RL funding, supervision, writing—review and editing. PB organization of data, supervision, writing—review and editing.
Corresponding author
Ethics declarations
Conflict of interest
J.B. is a consultant for Conformis and Smith & Nephew and a board member of Deutsche Gesellschaft für Endoprothetik (AE), Deutsche Knie Gesellschaft (DKG) and the European Knee Society (EKS) with no conflicts with this study.
Ethics approval
This study was approved by the ethics committee of Ludwig-Maximilians-Universität München (reference number: 18-274).
Informed consent
All included patients signed the consent to participate.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Schatz, C., Plötz, W., Beckmann, J. et al. Associations of preoperative anemia and postoperative hemoglobin values with hospital costs in total knee arthroplasty (TKA). Arch Orthop Trauma Surg 143, 6741–6751 (2023). https://doi.org/10.1007/s00402-023-04929-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-023-04929-4