Abstract
Introduction
Hip fracture patients are fragile, and the majority fail to fully recover to their pre-fracture functional level, resulting in an increase in institutionalization. We aimed to investigate risk factors for being dependent at discharge and for failure to return to independent living 12 months after a hip fracture.
Materials and methods
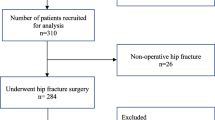
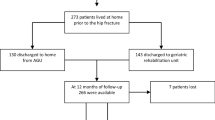
From 2011 to 2017, all surgically treated hip fracture patients admitted from their own homes were included in this prospective cohort study. Patient characteristics were registered, including age, sex, lifestyle, comorbidities, pre-fracture New Mobility Score (NMS), biochemical measures, fracture type, and surgical method. Dependency was measured at discharge using a cumulated ambulatory score (CAS < 6) and the timed-up-and-go test (TUG > 20 s). At 12 months, patients were interviewed regarding residence, NMS, and care needs. Multivariable logistic regression was used, reporting odds ratio (OR) with 95% confidence intervals (CI).
Results
A total of 2006 patients were included in the study with data regarding their hospital stay and discharge. In all, 1342 patients underwent follow-up at 12 months. The risk factors found to be associated with dependency at discharge were mostly static. Modifiable variables associated with dependency at discharge (CAS < 6) were hypoalbuminemia (OR: 1.94, 95% CI 1.38–2.71), not having been mobilized to standing within 24 h (OR: 1.88, 95% CI 1.12–3.15), and general anesthesia (OR: 1.35, 95% CI 1.07–1.71). Failure to return to independent living at 12 months was found in 10% of the patients, and was primarily associated with patient characteristics and proxy variables for comorbidities, but also with dependency at discharge (CAS < 6).
Conclusions
Mobilizing patients to standing within 24 h from hip fracture surgery was vital in maximizing short-term functional recovery. Failure to return to independent living was seen in the frailest patients. However, the majority remained in their own home with little increase in care needs.

Similar content being viewed by others
Availability of data and materials
The study protocol and data analysis files are available upon reasonable request to the corresponding author. For data sharing, relevant local authorities need to grant permission.
References
World Health Organization 2020 Decade of healthy ageing
Osnes EK, Lofthus CM, Meyer HE et al (2004) Consequences of hip fracture on activities of daily life and residential needs. Osteoporos Int 15:567–574. https://doi.org/10.1007/s00198-003-1583-0
Dyer SM, Crotty M, Fairhall N et al (2016) A critical review of the long-term disability outcomes following hip fracture. BMC Geriatr 16:158. https://doi.org/10.1186/s12877-016-0332-0
Gamboa-Arango A, Duaso E, Malafarina V et al (2020) Prognostic factors for discharge to home and residing at home 12 months after hip fracture: an anoia hip study. Aging Clin Exp Res 32:925–933. https://doi.org/10.1007/s40520-019-01273-9
Vochteloo AJH, Van Vliet-Koppert ST, Maier AB et al (2012) Risk factors for failure to return to the pre-fracture place of residence after hip fracture: a prospective longitudinal study of 444 patients. Arch Orthop Trauma Surg 132:823–830. https://doi.org/10.1007/s00402-012-1469-8
Martinez-Reig M, Ahmad L, Duque G (2012) The orthogeriatrics model of care: systematic review of predictors of institutionalization and mortality in post-hip fracture patients and evidence for interventions. J Am Med Dir Assoc 13:770–777. https://doi.org/10.1016/j.jamda.2012.07.011
Uriz-Otano F, Pla-Vidal J, Tiberio-López G, Malafarina V (2016) Factors associated to institutionalization and mortality over three years, in elderly people with a hip fracture—an observational study. Maturitas 89:9–15. https://doi.org/10.1016/j.maturitas.2016.04.005
Xu BY, Yan S, Low LL et al (2019) Predictors of poor functional outcomes and mortality in patients with hip fracture: a systematic review. BMC Musculoskelet Disord 20:568. https://doi.org/10.1186/s12891-019-2950-0
Sheehan KJ, Williamson L, Alexander J et al (2018) Prognostic factors of functional outcome after hip fracture surgery: a systematic review. Age Ageing 47:661–670. https://doi.org/10.1093/ageing/afy057
Ju J, Zhang P, Jiang B (2019) Risk factors for functional outcomes of the elderly with intertrochanteric fracture: a retrospective cohort study. Orhtopaedic Surg 11:643–652. https://doi.org/10.1111/os.12512
Meng D, Bai X, Wu H et al (2019) Patient and perioperative factors influencing the functional outcomes and mortality in elderly hip fractures. J Investig Surg. https://doi.org/10.1080/08941939.2019.1625985
Wong RMY, Qin J, Chau WW et al (2021) Prognostic factors related to ambulation deterioration after 1-year of geriatric hip fracture in a Chinese population. Sci Rep 11:1–8. https://doi.org/10.1038/s41598-021-94199-0
World Health Organization Body mass index—BMI 2021 https://www.euro.who.int/en/health-topics/disease-prevention/nutrition/a-healthy-lifestyle/body-mass-index-bmi
Jensen CM, Mainz H, Lamm M, et al. (2008) Reference programme for treatment of patients with proximal femur fractures. Dansk Sygeplejeråd, Danske Fysioterapeuter Dansk Ortopædisk Selskab 1–128.
Parker MJ, Palmer CR (1993) A new mobility after score for predicting mortality. J Bone Jt Surg Br 75:797–798
Kristensen MT, Bandholm T, Foss NB et al (2008) High inter-tester reliability of the new mobility score in patients with hip fracture. J Rehabil Med. https://doi.org/10.2340/16501977-0217
Kristensen MT, Foss NB, Kehlet H (2007) A new mobility score for predicting mortality after hip fracture. Physical 87:24–30
Danish Multidisciplinary Hip Fracture Registry (2019) Annual report 2019.
Frandsen CF, Glassou EN, Stilling M, Hansen TB (2021) Poor adherence to guidelines in treatment of fragile and cognitively impaired patients with hip fracture: a descriptive study of 2804 patients. Acta Orthop. https://doi.org/10.1080/17453674.2021.1925430
Kristensen MT, Kehlet H (2018) The basic mobility status upon acute hospital discharge is an independent risk factor for mortality up to 5 years after hip fracture surgery—survival rates of 444 pre-fracture ambulatory patients evaluated with the cumulated ambulation score. Acta Orthop 89:47–52. https://doi.org/10.1080/17453674.2017.1382038
Foss N, Kristensen M, Kehlet H (2006) Prediction of postoperative morbidity, mortality and rehabilitation in hip fracture patients: the cumulated ambulation score. Clin Rehabil 20:701–708
Kristensen MT, Öztürk B, Röck ND et al (2019) Regaining pre-fracture basic mobility status after hip fracture and association with post-discharge mortality and readmission—a nationwide register study in Denmark. Age Ageing 48:278–284. https://doi.org/10.1093/ageing/afy185
Podsiadlo D, Richardson S (1991) The timed “up & go”: a test of basic functional mobility for frail elderly persons. JAGS 39:142–148
Kristensen MT, Bandholm T, Holm B, Ekdahl C (2009) Timed up & go test score in patients with hip fracture is related to the type of walking aid. Arch Phys Med Rehabil 90:1760–1765. https://doi.org/10.1016/j.apmr.2009.05.013
Kristensen MT, Foss NB, Kehlet H (2007) Timed “up & go” test as a predictor of falls within 6 months after hip fracture surgery. Phys Ther 87:24–30. https://doi.org/10.1016/0308-5953(77)90120-9
Bischoff HA, Stähelin HB, Monsch AU et al (2003) Identifying a cut-off point for normal mobility: a comparison of the timed ‘ up and go ’ test in community-dwelling and institutionalised elderly women. Age Ageing 32:315–320
Tabori-jensen S, Hansen TB, Bøvling S et al (2018) Good function and high patient satisfaction at mean 2. 8 years after dual mobility THA following femoral neck fracture: a cross-sectional study of 124 patients. Clin Interv Aging 13:615–621
Van Der SMPL, Van EM, Tong WH et al (2020) Independent factors associated with long-term functional outcomes in patients with a proximal femoral fracture: a systematic review. Exp Gerontol. https://doi.org/10.1016/j.exger.2020.111035
Kamel HK, Iqbal MA, Mogallapu R et al (2003) Time to Ambulation After Hip Fracture Surgery: Relation to Hospitalization Outcomes. J Gerontol 58:1042–1045. https://doi.org/10.1093/gerona/58.11.M1042
Morri M, Forni C, Marchioni M et al (2018) Which factors are independent predictors of early recovery of mobility in the older adults’ population after hip fracture? a cohort prognostic study. Arch Orthop Trauma Surg 138:35–41. https://doi.org/10.1007/s00402-017-2803-y
Goubar A, Martin FC, Potter C et al (2021) The 30-day survival and recovery after hip fracture by timing of mobilization and dementia : a UK database study. Bone Joint J. https://doi.org/10.1302/0301-620X.103B7.BJJ-2020-2349.R1
Frandsen CF, Glassou EN, Stilling M, Hansen TB (2021) Malnutrition poor function and comorbidities predict mortality up to one year after hip fracture: a cohort study of patients. Eur Geriatr Med. https://doi.org/10.1007/s41999-021-00598-x
Scurrah A, Shiner CT, Stevens JA, Faux SG (2018) Regional nerve blockade for early analgesic management of elderly patients with hip fracture—a narrative review. Anaesthesia 73:769–783. https://doi.org/10.1111/anae.14178
Garlich JM, Pujari A, Debbi EM et al (2020) Time to block: early regional anesthesia improves pain control in geriatric hip fractures. J Bone Jt Surg 102:866–872
Guay J, Kopp S (2020) Peripheral nerve blocks for hip fractures in adults ( Review ). Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.CD001159.pub3.www.cochranelibrary.com
Fukuda T, Imai S, Nakadera M et al (2018) Postoperative daily living activities of geriatric patients administered general or spinal anesthesia for hip fracture surgery: a retrospective cohort study. J Orthop Surg 26:1–9. https://doi.org/10.1177/2309499017754106
Sieber F, Magaziner J, Marcantonio ER et al (2021) Spinal Anesthesia or general Anesthesia for hip surgery in older adults. N Engl J Med. https://doi.org/10.1056/NEJMoa2113514
Fields AC, Dieterich JD, Buterbaugh K, Moucha CS (2015) Short-term complications in hip fracture surgery using spinal versus general anaesthesia. Injury 46:719–723. https://doi.org/10.1016/j.injury.2015.02.002
Hershkovitz A, Borow Y, Beeri A, Nissan R (2020) Initial functional recovery as a measure for rehabilitation outcome in post- acute hip fractured patients. Arch Gerontol Geriatr. https://doi.org/10.1016/j.archger.2020.104070
Nygard H, Matre K, Fevang JM (2016) Evaluation of timed up and go test as a tool to measure postoperative function and prediction of one year walking ability for patients with hip fracture. Clin Rehabil 30:472–480. https://doi.org/10.1177/0269215515591039
Schulz C, Büchele G, Peter RS et al (2020) Regional variation of care dependency after hip fracture in Germany: a retrospective cohort study using health insurance claims data. PLoS ONE 15:1–17. https://doi.org/10.1371/journal.pone.0230648
Funding
This study was funded by the department only and has not received any external funding.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study’s conception and design. Data collection was performed by MS, Torben Bæk Hansen, and Christina Frølich Frandsen. Eva Natalia Glassou and Christina Frølich Frandsen performed the analyses. Christina Frølich Frandsen prepared the first draft of the manuscript, and all authors read, revised, and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no competing interests to declare relevant to this article's contents.
Ethics approval
The study was registered with the Danish Data Protection Agency (number 2007–58-0010). Under Danish law, no requirement for approval from the National Ethics committee applied.
Consent to participate and for publication
Under Danish law, no requirement for written consent applies.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Frandsen, C.F., Stilling, M., Glassou, E.N. et al. The majority of community-dwelling hip fracture patients return to independent living with minor increase in care needs: a prospective cohort study. Arch Orthop Trauma Surg 143, 2475–2484 (2023). https://doi.org/10.1007/s00402-022-04472-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-022-04472-8