Abstract
Purpose
The aims of this study were to investigate conventional radiographic parameters and introduce a novel parameter (arc center distance, ACD) for volar Barton fractures.
Methods
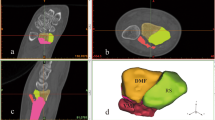
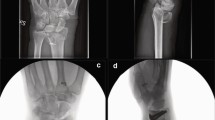
Twenty-four cases of volar Barton fracture were retrospectively analyzed. We measured volar tilt angle (VTA), anteroposterior distance (APD), teardrop angle (TDA), and capitate-to-axis-of-radius distance (CARD) on lateral plain radiographs. The ACD was measured on the sagittal images of computed tomography scans. VTAs, APDs, TDAs, and CARDs were compared between the fractured and normal contralateral wrist. The area under the receiver operating characteristic curve was calculated for each parameter.
Results
TDAs did not differ significantly between the fractured wrists and the controls. On the other hand, VTAs, APDs, and CARDs were all significantly greater in the fractured wrists (mean values were 17.25°, 20.70 mm, and − 3.40 mm, respectively). The area under the curve value was highest (0.943) for the ACD. When a cutoff value of 1.02 mm was used as a threshold, a sensitivity of 100% and specificity of 80.95% were achieved.
Conclusions
The mean values of conventional parameters (VTA, APD, TDA and CARD) in volar Barton fractures were presented. The ACD can be useful parameter for quantitatively evaluating volar Barton fractures.



Similar content being viewed by others
References
Ilyas A, Mudgal C, Jupiter J (2009) Volar rim and Barton’s fracture. Fractures and injuries to the distal radius and carpus, 1st edn. Elseveir, Philadelphia, pp 157–163
Lu Y, Li S, Wang M (2016) A classification and grading system for Barton fractures. Int Orthop 40(8):1725–1734. https://doi.org/10.1007/s00264-015-3034-x
Unglaub F, Langer MF, Hohendorff B et al (2017) Distale Radiusfraktur. Orthopäde 46(1):93–110. https://doi.org/10.1007/s00132-016-3347-5
Caldwell RA, Shorten PL, Morrell NT (2018) Common upper extremity fracture eponyms: a look into what they really mean. J Hand Surg Am 44(4):331–334. https://doi.org/10.1016/j.jhsa.2018.07.012
Meinberg EG, Agel J, Roberts CS, Karam MD, Kellam JF (2018) Fracture and dislocation classification compendium-2018. J Orthop Trauma 32:S1–S10. https://doi.org/10.1097/BOT.0000000000001063
Quadlbauer S, Pezzei C, Jurkowitsch J et al (2020) Functional and radiological outcome of distal radius fractures stabilized by volar-locking plate with a minimum follow-up of 1 year. Arch Orthop Trauma Surg 140(6):843–852. https://doi.org/10.1007/s00402-020-03411-9
Lee JK, Lee Y, Kim C, Kim M, Han SH (2021) Volar locking plate removal after distal radius fracture: a 10-year retrospective study. Arch Orthop Trauma Surg 141(10):1711–1719. https://doi.org/10.1007/s00402-020-03637-7
Paryavi E, Christian MW, Eglseder WA, Pensy RA (2015) Sustentaculum lunatum: appreciation of the palmar lunate facet in management of complex intra-articular fractures of the distal radius. Am J Orthop 44(9):E303–E307
Ng CY, McQueen MM (2011) What are the radiological predictors of functional outcome following fractures of the distal radius? J Bone Joint Surg Br 93(2):145–150. https://doi.org/10.1302/0301-620X.93B2.25631
Fujitani R, Omokawa S, Iida A, Santo S, Tanaka Y (2012) Reliability and clinical importance of teardrop angle measurement in intra-articular distal radius fracture. J Hand Surg Am 37(3):454–459. https://doi.org/10.1016/j.jhsa.2011.10.056
Kuhnel SP, Bigham AT, McMurtry RY, Faber KJ, King GJW, Grewal R (2019) The capitate-to-axis-of-radius distance (CARD): a new radiographic measurement for wrist and carpal alignment in the sagittal plane. J Hand Surg Am 44(9):797.e791-797.e798. https://doi.org/10.1016/j.jhsa.2018.10.024
Kitay A, Mudgal C (2014) Volar carpal subluxation following lunate facet fracture. J Hand Surg Am 39(11):2335–2341. https://doi.org/10.1016/j.jhsa.2014.04.027
Hawkins-Rivers S, Budoff JE, Ismaily SK, Noble PC, Haddad J (2008) MRI study of the capitate, lunate, and lunate fossa with relevance to proximal row carpectomy. J Hand Surg Am 33(6):841–849. https://doi.org/10.1016/j.jhsa.2008.02.021
Andermahr J, Lozano-Calderon S, Trafton T, Crisco JJ, Ring D (2006) The volar extension of the lunate facet of the distal radius: a quantitative anatomic study. J Hand Surg Am 31(6):892–895. https://doi.org/10.1016/j.jhsa.2006.03.010
Lee SH, Kim MB, Lee W, Kang H-J, Lee YH (2020) Quantitative evaluation of posterior talar subluxation in posterior malleolar fractures: a preliminary study. Injury 51(7):1669–1675. https://doi.org/10.1016/j.injury.2020.03.064
Lee SH, Kim MB, Lee YH, Kang HJ (2021) Reduction of olecranon fractures with no or minimal dorsal cortex comminution based on the contour of the posterior ulnar cortex: does it restore the greater sigmoid notch? Arch Orthop Trauma Surg. https://doi.org/10.1007/s00402-021-03934-9
Matullo KS, Dennison DG (2010) Lateral tilt wrist radiograph using the contralateral hand to position the wrist after volar plating of distal radius fractures. J Hand Surg Am 35(6):900–904. https://doi.org/10.1016/j.jhsa.2010.03.010
McCallister WV, Smith JM, Knight J, Trumble TE (2004) A cadaver model to evaluate the accuracy and reproducibility of plain radiograph step and gap measurements for intra-articular fracture of the distal radius. J Hand Surg Am 29(5):841–847. https://doi.org/10.1016/j.jhsa.2004.04.019
Porrino JA Jr, Maloney E, Scherer K, Mulcahy H, Ha AS, Allan C (2014) Fracture of the distal radius: epidemiology and premanagement radiographic characterization. AJR Am J Roentgenol 203(3):551–559. https://doi.org/10.2214/AJR.13.12140
Palola V, Ponkilainen V, Huttunen T, Launonen A, Mattila VM (2021) Incidence for volar locking plate removal following distal radius fracture surgery. Arch Orthop Trauma Surg 141:1297–1302. https://doi.org/10.1007/s00402-020-03565-6
Walenkamp MM, Aydin S, Mulders MA, Goslings JC, Schep NW (2016) Predictors of unstable distal radius fractures: a systematic review and meta-analysis. J Hand Surg Eur 41(5):501–515. https://doi.org/10.1177/1753193415604795
Beck JD, Harness NG, Spencer HT (2014) Volar plate fixation failure for volar shearing distal radius fractures with small lunate facet fragments. J Hand Surg Am 39(4):670–678. https://doi.org/10.1016/j.jhsa.2014.01.006
Medoff RJ (2009) Radiographic evaluation and classification of distal radius fractures. Fractures and injuries of the distal radius and carpus, 1st edn. Elseveir, Philadelphia, pp 17–31
Tanabe K, Nakajima T, Sogo E, Denno K, Horiki M, Nakagawa R (2011) Intra-articular fractures of the distal radius evaluated by computed tomography. J Hand Surg Am 36(11):1798–1803. https://doi.org/10.1016/j.jhsa.2011.08.021
Biswas D, Bible JE, Bohan M, Simpson AK, Whang PG, Grauer JN (2009) Radiation exposure from musculoskeletal computerized tomographic scans. J Bone Joint Surg Am 91(8):1882–1889. https://doi.org/10.2106/JBJS.H.01199
Acknowledgements
We thank Kwang Ryeol Lee, our first-year orthopedic resident, for his participation in the ACD measurements.
The English in this document has been checked by at least two professional editors, both native speakers of English. For a certificate, please see: http://www.textcheck.com/certificate/uW1p5R.
Funding
The authors received no financial support for the research, authorship, or publication of this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This retrospective study was approved by Seoul National University College of Medicine / Seoul National University Hospital Institutional Review Board. IRB No.: H-2104-017-1210.
Informed consent
Informed consent was waived by Seoul National University College of Medicine / Seoul National University Hospital Institutional Review Board.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kim, M.B., Lee, J.H. & Lee, Y.H. Arc center distance as a novel quantitative radiographic parameter for volar Barton fractures. Arch Orthop Trauma Surg 142, 3765–3770 (2022). https://doi.org/10.1007/s00402-021-04240-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-021-04240-0