Abstract
Introduction
The purpose of this study was to describe the indications and technical aspects as well as evaluate the clinical and functional outcome of lengthening osteotomy of the lateral trochlear ridge in patients with patellofemoral pain and/or patella instability and presence of trochlear dysplasia Dejour type A or lack of Dejour type dysplasia and short lateral articular trochlea.
Materials and methods
Six consecutive adult patients were treated with a lateral trochlear lengthening osteotomy. Five patients received a concomitant medial patellofemoral ligament reconstruction. Three patients had prior patella stabilization surgeries. Trochlea dysplasia (Dejour classification), Caton–Dechamps index, tibial tubercle trochlear groove (TT-TG) distance, patellar tilt and lateral condylar index were measured in preoperative MRIs. Clinical and functional evaluation included the Kujala Anterior Knee Pain Scale, the Lysholm Knee Score, the Tegner Activity Score, a subjective evaluation form and isokinetic muscle strength.
Results
Four patients had a Dejour type A dysplasia, two patients had no dysplasia. The mean (range) Caton-Dechamps index was 1.09 (0.95–1.16), TT-TG distance 10.9 mm (9.2–15.6 mm), patellar tilt 15° (4–32°) and lateral condylar index 82.0% (74–90%). One patient was lost to follow up, all others were followed for 2–5 years. All patients were satisfied with the clinical outcome. The Lysholm score increased from 55 (37–79) to 89 (76–100), the Tegner activity score from 3.6 (2–6) to 5.6 (5–7). The Kujala score postoperative was 90 (75–96). Some but not all patients had full strength recovery compared to the contralateral leg.
Conclusion
We recommend measuring the lateral condylar index and considering the indication of a lateral trochlear lengthening osteotomy as an additional or isolated procedure in selected patients with trochlear dysplasia Dejour type A or lack of dysplasia and short lateral articular trochlea depending on the extent of the patellar instability.
Level of evidence
Level IV, Case Series.
Trial registration number
NCT04378491, clinicaltrials.gov, May 7, 2020.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Trochlear dysplasia has been recognized as one of the main reasons leading to patellofemoral instability and is found in 85% of patients suffering from recurrent instability [1]. Trochlear dysplasia is typically classified into four types according to Dejour et al. [2]. This classification considers the depth and shape of the trochlear groove as a crucial factor for stabilizing the patella primarily in the first 30° of flexion. Different trochleoplasties have been described trying to address this problem [3]. Out of these, the Dejour deepening trochleoplasty [4] and the subchondral deepening trochleoplasty (Bereiter technique) [5] have been favoured and modified [6]. Although the results of such trochleoplasties are satisfying, they receive substantial criticism because of the high surgical complexity and the high rate of complications [3], and hence their indication is restricted. Most surgeons only use trochleoplasties in severe dysplasia or as a second line treatment after previous failed surgery [7].
Dejour et al. described the different types of trochlear dysplasia and listed major and minor instability factors [2]. According to this approach, the ‘menu à la carte’ was introduced by the Lyon group to address the individual needs of each patient [8]. However, the length of the lateral trochlea was not included as evaluation parameter of patellofemoral disorders. Therefore, another type of trochlear dysplasia not included in the classification of Dejour et al. [2] has been described: a dysplasia defined by a short lateral articular trochlea quantified by the trochlear index [9]. A short lateral articular trochlea leads to failure in stabilizing the patella close to full extension of the knee [9]. To address this type of pathology, a trochlear lengthening osteotomy has been described [10]. To the best of our knowledge, to date only one report involving two cases reported the clinical outcome of this new osteotomy [11].
The purpose of the present study was to describe the technical aspects as well as to evaluate the functional and clinical outcome of a lengthening osteotomy of the lateral trochlea ridge as an additional or isolated procedure in patients with patellofemoral pain and/or patella instability, presence of a trochlear dysplasia Dejour type A or lack of Dejour type dysplasia and short lateral articular trochlea quantified by the lateral condyle index.
Materials and methods
This study was approved by the regional ethics board.
Inclusion/indications of the lateral trochlear lengthening osteotomy
Over a period of 3 years, six consecutive patients with an indication for a lateral trochlear lengthening osteotomy were operated by two senior surgeons and included in this study. The indications for the lateral trochlea lengthening osteotomy included the presence of patellofemoral pain and/or patella instability with a short lateral condyle as quantified by the lateral condylar index (values below 93% are considered pathological) [9] and an absence of other clinical or radiological abnormalities to be corrected according to the Lyon ‘menu à la carte’. Namely, this procedure was indicated in patients with trochlear dysplasia Dejour type A or lack of Dejour type dysplasia, normal tibial tubercle to trochlear groove (TT-TG) distance (< 20 mm)[1], Caton–Deschamps index (0.6–1.2) [12], patellar tilt (< 20°) [1] and lack of femoral and tibial torsional deformities (Fig. 1).
Indication for a lateral lengthening osteotomy in a patient with short lateral trochlea (lateral condylar index i/ii = 84%, a) and lack of trochlear dysplasia Dejour type (sulcus angle 133°, b), normal patellar height quantified by a normal Caton–Deschamps index of 0.95 (i/ii, c), TT-TG distance of 9.2 mm (d), and normal patellar tilt of 13° (e)
Pre- and postoperative clinical and radiological measurements
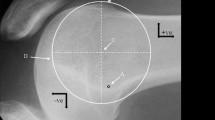
Preoperatively, patients were evaluated clinically and radiologically. Clinical evaluation included range of motion (ROM), lateral gliding test [13], patellar apprehension test (Fairbank’s test) [14] and moving patellar apprehension test (MPAT) [15] as well as control for torsional deformities of the tibia [16] and of the femur [17]. The radiological evaluation included anteroposterior and lateral plane radiographs of the knee, skyline patellar view images and magnetic resonance images (MRI). Torsional deformities were investigated with MRI and computer tomography (CT) scans only if the patient had pathologic values on the clinical examination of the femoral and tibial torsion. The trochlea dysplasia according to the Dejour classification was documented according to the axial views in the MRI [2, 18]. Furthermore, in sagittal MRIs the Caton-Deschamps index [19] was measured to evaluate a possible patella alta. In axial MRIs the TT-TG distance [20] was measured to evaluate a possible tubercle lateralization and the patellar tilt [1] as a sign of muscular and ligamentous balance. The presence of a Biedert type trochlear dysplasia was evaluated according to the lateral condylar index. The measurement of this index has been previously described [9]. Briefly, sagittal MRIs are used to draw the axis of the femur at the level where the anterior cruciate ligament is present at its entire length. The length of the most anterior and posterior aspects of the cartilaginous part of the lateral condyle is measured. The index of the anterior/posterior cartilaginous length is the lateral condylar index, expressed as a percentage (Fig. 2). Values below 93% are considered pathologic, and values below 86% are diagnostic for the presence of a short lateral condyles.
The lateral condylar index: two circles are drawn in a sagittal MRI image at the level where the anterior cruciate ligament is present at its entire length. The line connecting the centers of the two circles defines the femoral axis. A line vertical to the femoral axis tangential to the distal femoral cartilage serves as baseline to measure the length of the anterior (a) and posterior (p) cartilage length. The value (a/p × 100%) is the lateral condylar index. In this patient a pathologic lateral condylar index of 80% was calculated
Patients were followed up 6 weeks, 12 weeks, 6, 12, and 24 months postoperatively. An additional last follow up was performed at the time of conduction of this study. The initial clinical tests were performed at each follow up. Anteroposterior and lateral views of the knee as well as axial patellar views were performed 6 weeks postoperatively. Additionally, an MRI was performed in patients having discomfort at the 12 weeks follow up. The subjective evaluation was conducted through the Kujala Anterior Knee Pain Scale [21], the Lysholm Knee Score and the Tegner Activity Score [22]. Furthermore, patients were asked to subjectively evaluate the outcome of the operation according to the following options (subjective evaluation score): 5—excellent; 4—somewhat improved; 3—unchanged; 2—somewhat worse; 1—significantly worse [23], and asked if they would have the operation again. Lastly, isokinetic knee flexor and extensor strength tests were performed at 60°/s using an isokinetic dynamometer (Biodex System 4 Pro: Biodex Medical Systems, Shirley, NY, USA). The limb symmetry index (LSI) [24] (maximum torque operated side/maximum torque unaffected side × 100) of the flexors (hamstrings) and extensors (quadriceps) as well as the hamstring to quadriceps ratio (H/Q ratio) [25] were calculated.
Procedure
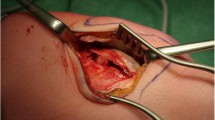
The patients were operated according to the technique described by Biedert et al. [10]. Through a short lateral parapatellar approach the length of the lateral trochlea was first observed, and the pathology confirmed. An osteotomy was performed with a chisel 5 mm posterior to the lateral cartilage of the trochlea along the anteroposterior axis and at the level of trochlear cartilage to periosteum transition in craniocaudal direction. The cartilage and periosteum were elevated proximally. Cancellous bone was harvested from the lateral femoral condyles and inserted in the osteotomy gap in a press fit technique. Allograft was used in case that the harvested cancellous bone was not sufficient. The periosteum was reattached with an absorbable Vicryl size 2 suture (Figs. 3, 4, 5). In case of the presence of a symptomatic lateral bump this was corrected as part of the lengthening procedure (Fig. 6). Figure 7 demonstrates an illustration of the technical procedure.
Preoperative (a) and postoperative (b) MRI images of a patient with a lateral trochlear lengthening osteotomy. Note the difference between the anterior condyle length before the operation (blue arrow, a) and after the operation (red arrow, b). The lateral condylar index was 84% preoperatively and 120% postoperatively. The yellow arrow represents the posterior condyle length and the green line the femoral axis (a, b)
a An osteotomy was performed with a chisel 5 mm posterior to the lateral cartilage of the trochlea along the anteroposterior axis (red dashed line), beginning at the level of trochlear cartilage to periosteum transition (green arrow) in craniocaudal direction. b The cartilage and periosteum were elevated proximally providing a lengthening of the lateral trochlea (blue arrow). Cancellous bone was harvested from the lateral femoral condyles and inserted in the osteotomy gap in a press fit technique (red arrow)
Postoperative care
Since the lateral lengthening osteotomy is rarely performed as a single operation, a part of the rehabilitation may be dictated by the concomitant procedures. Postoperatively, the patients were mobilized with partial weight bearing of 15 kg for 6 weeks. A hinged knee brace with a restriction of the knee joint ROM of 0/0/60° was applied for 3 weeks and 0/0/90° for another 3 weeks. Physiotherapy was initiated at the first postoperative day and continued for 6 months postoperatively. For the first 6 weeks only limited exercises with the goal of effusion elimination, gait control and leg control restoration were performed. After week 6, continuous passive motion and active ROM exercises, closed chain quadriceps exercises, and balance and proprioception exercises were included. After week 12, sport specific exercises were added. Return to sports was allowed when full ROM and lack of discomfort were achieved.
Results
Four of the six patients had a patellar instability and two had a lateral patellar compression syndrome. Three had chondral lesions grade III or IV according to International Cartilage Repair Society (ICRS) Cartilage Lesion Classification System [26]. Five patients had been previously operated at another institution before being referred to our institution. Concomitant procedures at our institution included interventions at the medial patellofemoral ligament (MPFL) in five cases and cartilage procedures in three cases. The diagnosis, procedures prior to the presentation at our institution, as well as the concomitant procedures are presented in Table 1. The radiological parameters of each patient are presented in Table 2. One patient was lost to follow up. One patient was followed up until 1 year postoperatively but did not present herself at the 2-year follow up because of her remote place of residence. However, she reported excellent results during the telephone interview 2 years postoperatively. All other patients attended the final follow up a minimum of 2 years postoperatively. One patient had to be revised at an external institution because of an overtight MPFL reconstruction. There were no other intra- or postoperative complications. No patient had a postoperative dislocation or signs of instability. The lateral gliding test [13], the patellar apprehension test (Fairbank’s test) [14] and the MPAT [15] were negative for all patients at each follow up, and the knee flexion was above 120° with no extension deficit at the last follow up. The clinical scores of each patient at the last follow up can be found in Table 3. Two patients had full strength recovery compared to the contralateral side as well as a satisfactory H/Q ratio while two had significant strength deficits and pathologic H/Q values (Table 3).
Discussion
This study presents the surgical procedure and functional outcomes of the lateral trochlea lengthening osteotomy. The outcomes of this case series allow us to recommend this procedure for selected patients. This is highly relevant for orthopaedic surgeons because it presents an additional treatment option in patients lacking the indication criteria for other surgical options.
The presence of a short lateral trochlea and the procedure of a lateral trochlear lengthening osteotomy are not included in the diagnostic and treatment concepts of most orthopaedic surgeons. A recent systematic review on trochleoplasties did not include this procedure as possible treatment [3]. Furthermore, Ntagiopoulos et al. [7] concluded that the ideal indication for a trochleoplasty is a presence of a high grade trochlear dysplasia (B or D), and Camathias et al. [6]—although including the lateral condylar index in their diagnostic procedures—considered a trochlea dysplasia type A as a contraindication for a trochleoplasty.
The ‘menu à la carte’ as introduced by the Lyon group [8] provides individual strategies tailored to the needs of each patient based on the original works of Dejour et al. [1, 2, 7]. This algorithm distinguishes between four major pillars causing patellar instability that can be addressed individually. Namely, a lateral tibial tubercle can be addressed with a medialization osteotomy; a patella alta with a distalisation of the tibial tubercle; a pathological patellar tilt with ligament balancing procedures and a trochlea dysplasia with a trochleoplasty. Nevertheless, as in this case series, there are rarely patients with patellofemoral pain and/or instability that do not match any of these pathologies. If the lateral condylar index is not controlled and the option of a lengthening osteotomy not discussed, these patients could remain untreated or be treated with unnecessary surgeries. In this case series, five of six patients were already unsuccessfully operated with different techniques before presenting at our clinic (Table 2). This could at least partially explain the large residual strength deficits presented in the patients of the present study because they were inactive for a long time prior to the operation. Postoperatively, the patients had good functional outcomes, lack of postoperative dislocations and were satisfied with the result of the operation. There were significant strength deficits and pathologic H/Q values in two patients. Although it is difficult to identify the reason of these deficits, it seems logical that it is the result of the long period of symptoms of the patients prior to being referred to our institution rather than with the operation itself.
In our experience, the lateral trochlea lengthening osteotomy is rarely indicated as solitary procedure. An isolated trochlea lengthening osteotomy would be indicated in patients with patellofemoral pain syndrome and short lateral trochlea without patella instability, further pathologies according to the ‘menu à la carte’ or chondral lesions. This was not the case in any of our patients. In the present study all patients received a concomitant procedure; five of the six patients received a concomitant MPFL reconstruction. Furthermore, the patient group being treated with this operation was very heterogeneous. This makes drawing conclusions regarding the single effect of this procedure difficult. Nonetheless, this procedure involves a limited surgical approach and—in contrast with other trochleoplasties—does not violate the articular surface, hence having minimal or no impact on the cartilage. Therefore, it is not expected to be associated with an increased risk of osteoarthritis. The theoretical risk of a cartilage fracture during the performance of the osteotomy did not appear in our case series. Moreover, according to Biedert et al. [10], even if this complication occurs it should be of no importance as long as the sharp edges are smoothed. Furthermore, this procedure only requires the removal of a limited amount of cancellous bone from the lateral condyle without further incisions and does not require any hardware. Altogether, we believe that this procedure provides an excellent choice as a safe, less invasive, complimentary procedure in selected patients. In case of a concomitant MPFL reconstruction, the lengthening osteotomy can provide the necessary static stability to protect the MPFL reconstruction (cases 1–3, 5–6). In case of a presence of a bony bump, the trochlear lengthening with a cartilage repair as concomitant operation and hence bump levelling may improve patellofemoral biomechanics and provide the necessary bony congruence to allow cartilage healing (cases 2–4, Fig. 6).
Strengths and limitations
The small sample size, the heterogeneity of the patients and the lack of control group are major limitations of this study. However, because this procedure is performed rarely and most patients had prior surgery, it would be unrealistic to expect a controlled study with a large sample size on this topic in the near future. Furthermore, the operation was not performed as a single intervention and hence it is not possible to evaluate its solitary effect.
Conclusion
We recommend measuring the lateral condylar index and considering the indication of a lateral trochlear lengthening osteotomy as an additional or isolated procedure in selected patients with trochlear dysplasia Dejour type A or lack of dysplasia and short lateral articular trochlea depending on the extent of the patellar instability.
Abbreviations
- LSI:
-
Limb symmetry index
- H/Q ratio:
-
Hamstrings/quadriceps ratio
- TT–TG distance:
-
Tibial tubercle–trochlear groove distance
References
Dejour H, Walch G, Nove-Josserand L, Guier C (1994) Factors of patellar instability: an anatomic radiographic study. Knee Surg Sports TraumatolArthrosc 2(1):19–26
Dejour D, Le Coultre B (2007) Osteotomies in patello-femoral instabilities. Sports Med Arthrosc Rev 15(1):39–46. https://doi.org/10.1097/JSA.0b013e31803035ae
van Sambeeck JDP, van de Groes SAW, Verdonschot N, Hannink G (2018) Trochleoplasty procedures show complication rates similar to other patellar-stabilizing procedures. Knee Surg Sports TraumatolArthrosc 26(9):2841–2857. https://doi.org/10.1007/s00167-017-4766-5
Dejour H, Walch G, Neyret P, Adeleine P (1990) Dysplasia of the femoral trochlea. Rev ChirOrthopReparatriceAppar Mot 76(1):45–54
Bereiter H, Gautier E (1994) Thetrochleaplasty as a surgical therapy of recurrent dislocation of the patella in dysplastic trochlea of the femur. Arthroskopie 7:281–286
Camathias C, Studer K, Kiapour A, Rutz E, Vavken P (2016) Trochleoplasty as a solitary treatment for recurrent patellar dislocation results in good clinical outcome in adolescents. Am J Sports Med 44(11):2855–2863. https://doi.org/10.1177/0363546516652894
Ntagiopoulos PG, Dejour D (2014) Current concepts on trochleoplasty procedures for the surgical treatment of trochlear dysplasia. Knee Surg Sports TraumatolArthrosc 22(10):2531–2539. https://doi.org/10.1007/s00167-014-3013-6
Fithian DC, Neyret P, Servien E (2008) Patellar instability: the Lyon experience. CurrOrthopPract 19(3):328–338. https://doi.org/10.1097/BCO.0b013e32830320fc
Biedert RM, Netzer P, Gal I, Sigg A, Tscholl PM (2011) The lateral condyle index: a new index for assessing the length of the lateral articular trochlea as predisposing factor for patellar instability. IntOrthop 35(9):1327–1331. https://doi.org/10.1007/s00264-010-1142-1
Biedert RM (2010) Trochlear lengthening osteotomy with or without elevation of the lateral trochlear facet. In: Patellofemoral pain, instability, and arthritis. Springer, pp 209–215
Biedert RM (2012) Patellar instability with increased knee flexion due to lateral femoral condyle distal dysplasia: a report of two cases. Knee 19(2):140–143. https://doi.org/10.1016/j.knee.2010.12.003
Ntagiopoulos PG, Bonin N, Sonnery-Cottet B, Badet R, Dejour D (2014) The incidence of trochlear dysplasia in anterior cruciate ligament tears. IntOrthop 38(6):1269–1275
Manske RC, Davies GJ (2016) Examination of the patellofemoral joint. Int J Sports PhysTher 11(6):831
Malanga GA, Andrus S, Nadler SF, McLean J (2003) Physical examination of the knee: a review of the original test description and scientific validity of common orthopedic tests. Arch Phys Med Rehabil 84(4):592–603
Ahmad CS, McCarthy M, Gomez JA, Shubin Stein BE (2009) The moving patellar apprehension test for lateral patellar instability. Am J Sports Med 37(4):791–796
Staheli LT, Engel GM (1972) Tibial torsion: a method of assessment and a survey of normal children. ClinOrthop 86:183–186
Ryder CT, Crane L (1953) Measuring femoral anteversion: the problem and a method. J Bone JtSurg Am 35(2):321–328
Chhabra A, Subhawong TK, Carrino JA (2011) A systematised MRI approach to evaluating the patellofemoral joint. SkeletRadiol 40(4):375–387. https://doi.org/10.1007/s00256-010-0909-1
Caton J, Deschamps G, Chambat P, Lerat J, Dejour H (1982) Patella infera. Apropos of 128 cases. Rev ChirOrthopReparatriceAppar Mot 68(5):317–325
Wittstein JR, Bartlett EC, Easterbrook J, Byrd JC (2006) Magnetic resonance imaging evaluation of patellofemoralmalalignment. Arthroscopy 22(6):643–649
Kujala UM, Jaakkola LH, Koskinen SK, Taimela S, Hurme M, Nelimarkka O (1993) Scoring of patellofemoral disorders. Arthroscopy 9(2):159–163
Tegner Y, Lysholm J (1985) Rating systems in the evaluation of knee ligament injuries. ClinOrthop 198:43–49
Maroon JC, Bost JW, LePere DB, Bost SM, Williams L, Amos AS (2013) Clinical evaluation of TruFUSE® lumbar facet fusion system. SurgSci 4(02):166
Wellsandt E, Failla MJ, Snyder-Mackler L (2017) Limb symmetry indexes can overestimate knee function after anterior cruciate ligament injury. J Orthop Sports PhysTher 47(5):334–338
Struzik A, Pietraszewski B (2019) Relationships between hamstrings-to-quadriceps ratio and variables describing countermovement and drop jumps. Appl Bionics Biomech 2019:4505481–4505481. https://doi.org/10.1155/2019/4505481
Brittberg M, Winalski CS (2003) Evaluation of cartilage injuries and repair. J Bone JtSurg Am 85-A(Suppl 2):58–69. https://doi.org/10.2106/00004623-200300002-00008
Acknowledgements
The senior author acknowledges Mrs. pract. med. Farah Selman, resident of orthopaedic surgery, Balgrist University Hospital, Forchstrasse 340, 8008 Zürich for her extensive literature review regarding the lateral trochlea lengthening procedure that motivated the current study.
Funding
Open Access funding provided by Universität Basel (Universitätsbibliothek Basel). Funding was received from the Department of Orthopaedics and Traumatology, University Hospital of Basel and the Department of Surgery, University of Basel. The funding sources had no involvement in the preparation of the article.
Author information
Authors and Affiliations
Contributions
PI was involved in the follow up, participated in the data analysis and wrote the manuscript. CE conceived the study, participated in the interpretation of the data and revised the manuscript. CN was involved in conducting the experiments, processed and analyzed the data and revised the manuscript. AM analyzed and interpreted the data and was a major contributor to writing the manuscript. GP was the lead surgeon in all cases, the patients were referred to him, he developed the treatment algorithm and revised the manuscript. All authors read and approved the final manuscript. All authors had full access to all data and take responsibility for the integrity of the data and the accuracy of the data analysis.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ismailidis, P., Egloff, C., Nüesch, C. et al. Lateral trochlear lengthening osteotomy. Arch Orthop Trauma Surg 141, 1721–1730 (2021). https://doi.org/10.1007/s00402-020-03736-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-020-03736-5