Abstract
Objectives
The purpose of this study was to identify the optimal position for a precontoured-locking plating (PHILOS®) of the proximal humerus in Asians in terms of conformity and to determine the prevalence of screw exits in the position of the highest conformity.
Methods
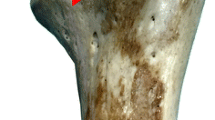
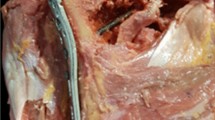
Twenty adult humeri and 14 cadaveric shoulders were included in this study. After placing the precontoured plate in the well-fitted position on the humerus, we measured the distance between the upper margin of the plate and the tip of greater tuberosity (GT) (distance A) and the distance between the anterior margin of the plate and lateral border of the bicipital groove (BG) (distance B). The prevalence of K-wire exits was assessed. In the 14 cadaver shoulders, the mutual relation between the most inferior locking sleeve of the optimally positioned plate and the axillary nerve was evaluated to assess the potential for axillary nerve injury.
Results
The precontoured plate was well-fitted and remained in a relatively constant position in all specimens. Distance A was an average of 3.6 mm (range 1.4–5.5 mm), and distance B was an average of 2.5 mm (range 0–4.6 mm). The K wire closest to the BG pierced it in four cases (20 %), and most inferior K wires exited at an average distance of 3.8 mm (range 1.6–9.0 mm) from the inferior articular margin of the humeral head. Regarding involvement of the BG, articular width was the only significant variable in the logistic regression model, with an odds’ ratio of 0.610. The axillary nerve was located at an average vertical distance of 59.7 mm (range 51.8–66.9 mm) from the tip of the GT in a vertically neutral position. The results did not differ between the left and right sides (t = 0.326, p = 0.755). Although the axillary nerve was slightly inferior to the most inferior locking holes of the proximal humerus, it was located in the path of their locking sleeves on the deltoid muscle.
Conclusion
The optimal position for the highest conformity led to ideal fixation of the proximal humerus and inferomedial support screw in Asians. However, the precontoured plate sometimes had screw exits that involved the BG, and articular width had a large impact on involvement of the BG. If locking sleeves for the most inferior holes were introduced on the deltoid muscle in a neutral position, there was high potential for injury to the axillary nerve in Koreans.






Similar content being viewed by others
References
Agudelo J, Schurmann M, Stahel P et al (2007) Analysis of efficacy and failure in proximal humerus fractures treated with locking plates. J Orthop Trauma 21(10):676–681
Anglen JO, Archdeacon MT, Cannada LK, Herscovici D Jr (2008) Avoiding complications in the treatment of humeral fractures. J Bone Jt Surg Am 90(7):1580–1589
Apaydin N, Tubbs RS, Loukas M, Duparc F (2010) Review of the surgical anatomy of the axillary nerve and the anatomic basis of its iatrogenic and traumatic injury. Surg Radiol Anat 32(3):193–201
Bai L, Fu Z, An S, Zhang P, Zhang D, Jiang B (2014) Effect of calcar screw use in surgical neck fractures of the proximal humerus with unstable medial support: a biomechanical study. J Orthop Trauma 28(8):452–457
Brunner F, Sommer C, Bahrs C et al (2009) Open reduction and internal fixation of proximal humerus fractures using a proximal humeral locked plate: a prospective multicenter analysis. J Orthop Trauma 23(3):163–172
Charalambous CP, Siddique I, Valluripalli K et al (2007) Proximal humeral internal locking system (PHILOS) for the treatment of proximal humeral fractures. Arch Orthop Trauma Surg 127(3):205–210
Cheung S, Fitzpatrick M, Lee TQ (2009) Effects of shoulder position on axillary nerve positions during the split lateral deltoid approach. J Shoulder Elbow Surg 18(5):748–755
Clavert P, Adam P, Bevort A, Bonnomet F, Kempf JF (2010) Pitfalls and complications with locking plate for proximal humerus fracture. J Shoulder Elbow Surg 19(4):489–494
Egol KA, Ong CC, Walsh M, Jazrawi LM, Tejwani NC, Zuckerman JD (2008) Early complications in proximal humerus fractures (OTA Types 11) treated with locked plates. J Orthop Trauma 22(3):159–164
Gardner MJ, Boraiah S, Helfet DL, Lorich DG (2008) Indirect medial reduction and strut support of proximal humerus fractures using an endosteal implant. J Orthop Trauma 22(3):195–200
Gardner MJ, Griffith MH, Dines JS, Briggs SM, Weiland AJ, Lorich DG (2005) The extended anterolateral acromial approach allows minimally invasive access to the proximal humerus. Clin Orthop Relat Res 434(434):123–129. doi:10.1097/01.blo.0000152872.95806.09
Gardner MJ, Weil Y, Barker JU, Kelly BT, Helfet DL, Lorich DG (2007) The importance of medial support in locked plating of proximal humerus fractures. J Orthop Trauma 21(3):185–191
Gerber C, Werner CM, Vienne P (2004) Internal fixation of complex fractures of the proximal humerus. J Bone Jt Surg Br 86(6):848–855
Hertel R (2005) Fractures of the proximal humerus in osteoporotic bone. Osteoporos Int 16(Suppl 2):S65–S72
Hinds RM, Garner MR, Tran WH, Lazaro LE, Dines JS, Lorich DG (2015) Geriatric proximal humeral fracture patients show similar clinical outcomes to non-geriatric patients after osteosynthesis with endosteal fibular strut allograft augmentation. J Shoulder Elbow Surg 24(6):889–896
Hirschmann MT, Fallegger B, Amsler F, Regazzoni P, Gross T (2011) Clinical longer-term results after internal fixation of proximal humerus fractures with a locking compression plate (PHILOS). J Orthop Trauma 25(5):286–293
Huttunen TT, Launonen AP, Pihlajamaki H, Kannus P, Mattila VM (2012) Trends in the surgical treatment of proximal humeral fractures—a nationwide 23-year study in Finland. BMC Musculoskelet Disord 13:261
Iacobellis C, Fountzoulas K, Aldegheri R (2011) Plating of proximal fracture of the humerus: a study of 30 cases. Musculoskel Surg 95(Suppl 1):S43–S48
Jones CB, Sietsema DL, Williams DK (2011) Locked plating of proximal humeral fractures: is function affected by age, time, and fracture patterns? Clin Orthop Relat Res 469(12):3307–3316
Konrad G, Bayer J, Hepp P et al (2010) Open reduction and internal fixation of proximal humeral fractures with use of the locking proximal humerus plate. Surgical technique. J Bone Jt Surg Am 92 Suppl 1 Pt 1:85–95
Labronici PJ, e Albuquerque RP, Schott V, Pires RE, Belangero WD, Franco JS (2014) Proximal humeral fractures: an understanding of the ideal plate positioning. Int Orthop 38(10):2191–2195
Launonen AP, Lepola V, Flinkkila T, Laitinen M, Paavola M, Malmivaara A (2015) Treatment of proximal humerus fractures in the elderly: a systemic review of 409 patients. Acta Orthop 86(3):280–285
Lee KW, Choi YJ, Ahn HS et al (2012) Internal fixation of proximal humerus fracture with polyaxial angular stable locking compression plate in patients older than 65 years. Clin Shoulder Elbow 15(1):25–31
Lin T, Xiao B, Ma X, Fu D, Yang S (2014) Minimally invasive plate osteosynthesis with a locking compression plate is superior to open reduction and internal fixation in the management of the proximal humerus fractures. BMC Musculoskelet Disord 15:206
Nho SJ, Brophy RH, Barker JU, Cornell CN, MacGillivray JD (2007) Innovations in the management of displaced proximal humerus fractures. J Am Acad Orthop Surg 15(1):12–26
Oh HK, Cho DY, Choo SK, Park JW, Park KC, Lee JI (2015) Lessons learned from treating patients with unstable multifragmentary fractures of the proximal humerus by minimal invasive plate osteosynthesis. Arch Orthop Trauma Surg 135(2):235–242
Osterhoff G, Ossendorf C, Wanner GA, Simmen HP, Werner CM (2011) The calcar screw in angular stable plate fixation of proximal humeral fractures—a case study. J Orthop Surg Res 6:50
Owsley KC, Gorczyca JT (2008) Fracture displacement and screw cutout after open reduction and locked plate fixation of proximal humeral fractures [corrected]. J Bone Jt Surg Am 90(2):233–240
Robinson CM, Longino D, Murray IR, Duckworth AD (2010) Proximal humerus fractures with valgus deformity of the humeral head: the spectrum of injury, clinical assessment and treatment. J Shoulder Elbow Surg 19(7):1105–1114
Robinson CM, Wylie JR, Ray AG et al (2010) Proximal humeral fractures with a severe varus deformity treated by fixation with a locking plate. J Bone Jt Surg Br 92(5):672–678
Saran N, Bergeron SG, Benoit B, Reindl R, Harvey EJ, Berry GK (2010) Risk of axillary nerve injury during percutaneous proximal humerus locking plate insertion using an external aiming guide. Injury 41(10):1037–1040
Smith J, Berry G, Laflamme Y, Blain-Pare E, Reindl R, Harvey E (2007) Percutaneous insertion of a proximal humeral locking plate: an anatomic study. Injury 38(2):206–211
Sohn HS, Shin SJ (2014) Minimally invasive plate osteosynthesis for proximal humeral fractures: clinical and radiologic outcomes according to fracture type. J Shoulder Elbow Surg 23(9):1334–1340
Solberg BD, Moon CN, Franco DP, Paiement GD (2009) Locked plating of 3- and 4-part proximal humerus fractures in older patients: the effect of initial fracture pattern on outcome. J Orthop Trauma 23(2):113–119
Sung CM, Roh GS, Sohn HJ, Park HB (2013) Prediction of the location of the anterior branch of the axillary nerve, using correlations with physical factors: a cadaveric study. J Shoulder Elbow Surg 22(11):e9–e16
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kwak, JY., Park, HB. & Jung, GH. Accurate application of a precontoured-locking plate for proximal humeral fractures in Asians: a cadaveric study. Arch Orthop Trauma Surg 136, 1387–1393 (2016). https://doi.org/10.1007/s00402-016-2538-1
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-016-2538-1