Abstract
Aims
The 6-min walk test is an inexpensive, safe, and easy tool to assess functional capacity in patients with cardiopulmonary diseases including heart failure (HF). There is a lack of reference values, which are a prerequisite for the interpretation of test results in patients. Furthermore, determinants independent of the respective disease need to be considered when interpreting the 6-min walk distance (6MWD).
Methods
The prospective Characteristics and Course of Heart Failure Stages A-B and Determinants of Progression (STAAB) cohort study investigates a representative sample of residents of the City of Würzburg, Germany, aged 30 to 79 years, without a history of HF. Participants underwent detailed clinical and echocardiographic phenotyping as well as a standardized assessment of the 6MWD using a 15-m hallway.
Results
In a sample of 2762 participants (51% women, mean age 58 ± 11 years), we identified age and height, but not sex, as determinants of the 6MWD. While a worse metabolic profile showed a negative association with the 6MWD, a better systolic and diastolic function showed a positive association with 6MWD. From a subgroup of 681 individuals without any cardiovascular risk factors (60% women, mean age 52 ± 10 years), we computed age- and height-specific reference percentiles.
Conclusion
In a representative sample of the general population free from HF, we identified determinants of the 6MWD implying objective physical fitness associated with metabolic health as well as with cardiac structure and function. Furthermore, we derived reference percentiles applicable when using a 15-m hallway.
Graphical abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The six-minute walk test (6MWT) reports the distance a subject is able to cover within a time span of 6 min (6MWD). As such, the 6MWT is a simple, safe, and inexpensive tool to estimate the functional capacity of an individual. Developed in the 1960s for the assessment of soldiers [1], the test was later refined for the application in patients with chronic bronchitis [2]. Nowadays, the 6MWT is frequently used to assess the functional capacity of patients with chronic respiratory diseases, [3, 4] heart failure, [5,6,7] infectious diseases, [8, 9] neurological disorders, [10,11,12,13] and cancer [14]. Further, the 6MWD has become an accepted end-point in clinical trials including heart failure [5, 15].
The latest recommendations of the American Thoracic Society ascribe to the 6MWT a good construct validity and test–retest reliability, a strong relationship with exercise performance and physical activity, and favorable responsiveness to treatment effects in patients with chronic respiratory diseases [16]. In patients with heart failure and preserved ejection fraction, the 6MWD correlated with invasively derived work load corrected pulmonary capillary wedge pressure[17] and the 6MWD carries prognostic information in patients with heart failure [5, 18,19,20]. The 6MWT is sensitive to variations in methodology including track length, oxygen supplementation, and encouragement; hence, stable conditions are key to ensure comparability of test results [5, 16] and walking courses of 25–30-m length are recommended [5, 16, 17].
Nevertheless, the recommendation to use a walking course of 25–30-m length is challenging to provide in clinical practice. Thus, mainly due to space constraints, several alternative protocols have been applied and used with comparable diagnostic quality [21,22,23,24,25].
Given the heterogeneity in methodology in addition to further factors potentially influencing the 6MWD like age, sex, and anthropometric characteristics, there is a lack of normal values serving as reference point for the assessment of impaired functional capacity. Reference equations were derived from several, mostly smaller study samples, but showed high heterogeneity and low predictive utility regarding the effective 6MWD [5, 16].
In the present study, we aimed to assess determinants of the 6MWD in a population-based cohort and to derive reference values from healthy individuals of a representative sample of the general population. Based on these results, we developed a calculator that also allows classifying the measured 6MWD in relation to the predicted 6MWD.
Methods
Study sample
The population-based Characteristics and Course of Heart Failure Stages A-B and Determinants of Progression (STAAB) Cohort Study recruited a representative sample of individuals without self-reported heart failure from the general population of Würzburg, Germany, between 12/2013 and 10/2017. A random sample of residents of the City of Würzburg (source population 124,297 inhabitants as of 2011 census) was drawn in November 2013 from the local registration office with predefined age and sex strata with ratios 1:1 for sex, and 10:27:27:27:10 for age groups of 30–39, 40–49, 50–59, 60–69, and 70–79 years, respectively. The detailed study design and methodology have been published [26].
All study-related procedures were subjected to a rigid and regular quality control process. The STAAB cohort study protocol and procedures comply with the Declaration of Helsinki and received positive votes from the Ethics Committee of the Medical Faculty as well as from the data protection officer of the University of Würzburg (vote #98/13). All participants provided written informed consent prior to any study examination [26].
The current analysis is based on the first follow-up examination, performed between 12/2017 and 08/2021. All participants attending the baseline examination were invited for a follow-up visit of about 3-h duration in the Joint Survey Unit of the Comprehensive Heart Failure Center, Würzburg, Germany, and gave their respective informed consent.
Clinical assessment
The follow-up visit included blood collection (> 8 h of fasting) for routine laboratory parameters, physical examination, anthropometry, assessment of blood pressure, and an electrocardiogram according to pre-specified standards [26, 27]. Further, all participants underwent an extensive, pre-specified transthoracic echocardiography protocol (Vivid S6 or Vivid E95, GE Healthcare, Horten, Norway) performed by dedicated certified personnel that was quality-controlled on a regular basis [26,27,28].
Six-minute walk test
The 6MWT was performed according to a standardized protocol using a 15-m test distance located in an undisturbed, straight, and flat indoor hallway. Each participant without contraindications (e.g., instable angina pectoris or myocardial infarction within the previous 4 weeks, blood pressure > 180/100 mmHg, or resting heart rate > 120 bpm), performed the 6MWT once, under the supervision of a trained staff member (graphical abstract). Participants were instructed to cover as much ground as possible within 6 min, without running or jogging (“walk as far as possible”). They could slow down or stop if necessary, but should resume walking as soon as possible. During the 6MWT, participants were encouraged verbally every 30 s, and the remaining time was announced every 2 min. Blood pressure, heart rate, and the Borg rating scale of perceived dyspnea [16] were assessed before and after the 6MWT. Additionally, the Borg rating scale of perceived exertion [29] was assessed after the 6MWT. The 6MWD was calculated from the number of 15-m laps completed within the 6 min plus the remaining meters of the last, incomplete lap and documented. Participants who terminated the test prematurely or were impaired due to specific reasons (e.g., inadequate footwear, musculoskeletal disorder, severe cardiac or pulmonary disease, neurological disorder) were graded as having an invalid 6MWD and were excluded from further analyses.
Subgroup “apparently healthy”
A subgroup of individuals, who were free from known cardiovascular disease and cardiovascular risk factors including hypertension (blood pressure ≥ 140/90 mmHg or anti-hypertensive drug), smoking (current or ex-smoker), obesity (body mass index > 30 kg/m2), dyslipidemia (low density lipoprotein ≥ 190 mg/dL or lipid-lowering therapy), or diabetes mellitus (HbA1c > 6.5% or fasting plasma glucose > 7 mmol/L or 2 h plasma glucose > 11.1 mmol/L), were defined as “apparently healthy.” This subgroup was selected to derive reference values.
Quality assurance
The effect of test–retest variability was evaluated based on information of healthy volunteers, who performed the 6MWT twice with at least 24 h between both tests. These volunteers additionally performed a third 6MWT (again with at least 24 h between tests) using the conventional 30-m hallway protocol allowing to compare the impact of test distance on the 6MWT result.
Data analysis
Statistical analysis was performed using the IBM SPSS Statistics (version 28.0) software. A p-value < 0.05 was considered as statistically significant. Determinants of the 6MWD were identified from the total sample of individuals with valid 6MWT result applying generalized linear models. The variable age was adjusted for sex. The variable sex was first adjusted only for age, then adjusted additionally for body height. All other variables were adjusted for sex and age. Multiplicative interaction terms with the variable sex were sought. In the case of a significant interaction with sex, the effect estimates were reported separately for women and men. We present the effect estimate with its 95% confidence interval (95%-CI), p-value of the effect estimate, and p-value of the sex interaction.
From the subgroup of apparently healthy individuals, selected as described above, reference percentiles of the 6MWD were computed using a non-linear regression with a piecewise linear function. The distribution of the residuals of the 6MWD was analyzed using the Shapiro–Wilk test. We display the 2.5 to the 97.5 percentiles. Percentiles for intermediate values of age and body height can be determined by linear interpolation as exemplified in the Appendix.
Results
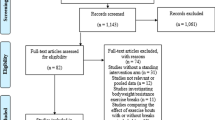
Of 4965 STAAB participants (52% women, 55 ± 12 years), 3901 (79%; 52% women, 58 ± 11 years) attended the first follow-up examination. Of those, 2762 (71%; 51% women, 58 ± 11 years) with valid 6MWD entered the analyses (Fig. 1). When compared to participants without valid 6MWD, those with valid 6MWD were significantly younger, less often female, and had a more favorable comorbidity and risk factor profile (Table 1).
The mean 6MWD of the total sample was 542 ± 86 m. Blood pressure before and after the 6MWT were 130 ± 17/77 ± 10 mmHg and 156 ± 22/83 ± 10 mmHg, respectively. Perceived dyspnea were 0.0 before and 1.0 immediately after the 6MWT; the perceived exertion immediately after the 6MWT was 10.0.
Determinants of the 6MWD
The 6MWD in the 2762 participants with a valid 6MWT was significantly associated with sex, age, and body height (all p < 0.001), the latter two without significant interaction with sex (Table 2). After adjustment for body height and age, the association of sex with the 6MWD lost statistical significance (Table 2). Further, the 6MWD was positively associated with higher cholesterol levels, left ventricular end-diastolic volume, left ventricular ejection fraction, and left ventricular stroke volume (men only), as well as with higher left ventricular relaxation velocity, while we observed a negative association of 6MWD with higher resting heart rate, estimated glomerular filtration rate (eGFR), body mass index, trigylcerides, glycosylated hemoglobin (HbA1c), fasting glucose, and NT-proBNP, as well as with higher E/e´, a measure of left ventricular filling pressure (Table 3).
Reference values of the 6MWD
Six hundred eighty-one participants with valid 6MWD (25%; 60% women, 52 ± 10 years) were considered apparently healthy (Table 1). Their mean 6MWD was 578 ± 71 m. Blood pressure before and after the 6MWT were 122 ± 12/74 ± 8 mmHg and 150 ± 20/82 ± 9 mmHg, respectively. Perceived dyspnea were 0.0 before and 0.7 immediately after the 6MWT; the perceived exertion immediately after the 6MWT was 9.0.
Based on the fact, that the 6MWD was associated with age (with a significant change in slope at the age of 56.2 years) and body height but not with sex, we derived age- and height-specific reference percentiles from these apparently healthy participants (Table 4).
We used the following regression equation:
An example for linear interpolation is given in the supplement. We further provide a Web-based tool for online calculation (https://6mwt.org/).
Quality assurance
N = 11 volunteers (32 ± 8 years, 8 women) performed serial 6MWT. The mean 6MWD of the first 6MWT using the 15-m test distance was 727 ± 57 m, of the second 6MWT using the 15-m test distance was 755 ± 71 m, and of the 6MWT using the 30-m test distance was 800 ± 78 m, respectively. Hence, the mean difference between the first and the second 15-m 6MWT was 28 ± 30 (95%CI 8; 48) m; the mean difference between the second 15-m 6MWT and the 30-m 6MWT was 44 ± 29 (95%CI 25; 64) m.
Discussion
In a well-characterized population-based sample, the 6MWD was significantly associated with age and body height, but not with sex. Accordingly, we derived age- and height-specific reference percentiles and provided a table to be used by linear interpolation. To enhance practical usage, we also provided an online calculator to determine an individual’s predicted 6MWD, which allows to put the effective 6MWD in relation to an expected result. In addition, we display the effect estimates of further determinants of the 6MWD in the general population like body mass index, metabolic parameters, and cardiac structure and function, to facilitate the refinement of an individual’s predicted 6MWD. These data might serve to grade an individual’s physical capacity and form a good basis for further research in patient collectives.
There is a large body of evidence that the 6MWT is a valid and reliable test with good construct validity and low test–retest variability [16]. Further, the 6MWD shows a strong relationship with measures of exercise performance as assessed for example by cardio-pulmonary exercise testing (CPET) [5, 16]. Although there is a good correlation with maximal oxygen uptake in CPET, the 6MWT is considered a submaximal exercise test, which better reflects an individual’s physical performance in daily life [5]. As detailed in a consensus document from the European Respiratory Society and the American Thoracic Society, the 6MWD is strongly associated with the risk of rehospitalization and mortality in patients with respiratory diseases. Further, the 6MWD is responsive to treatment effects and a minimal important difference of 30 m has been suggested as a meaningful change in patients with chronic respiratory diseases [16]. In patients with heart failure, the 6MWD also has been shown to carry prognostic information in the event of an acute decompensation as well as in the chronic state [5]. A recent meta-analysis reported that an increase in 6MWD of 80 m was associated with an improvement in quality of life in patients with heart failure [5, 30].
Nevertheless, the 6MWT is sensitive to changes in methodology. When compared to a straight indoor hallway, participants using a treadmill achieved a shorter 6MWD. By contrast, individuals achieved longer 6MWD when using a continuous (oval or circular) track or an outside track [16, 31]. The impact of the length of the respective test track on the 6MWD has been discussed controversially. In patients with chronic obstructive pulmonary disease [32], there was a difference in 6MWD depending on the length of the test track, there was no such effect observed in patients with severe pulmonary emphysema [31].
Further, there is a learning effect with longer 6MWD achieved during repeat performances of the 6MWT. This effect has been described in different populations, but with markedly varying orders of magnitude [16]. In patients with chronic respiratory diseases, the increase in the 6MWD ranged between 24 and 29 m, with 50–87% of patients walking a larger distance at the second occasion of the 6MWT [16].
Integrating current knowledge, the authors of the abovementioned consensus paper [16] recommend using a test distance of at least 30-m length and to perform the 6MWT twice as a baseline if serial assessment is planned. Nevertheless, both recommendations impose major challenges in clinical practice and several methodologies including varying test distances have been applied [5, 16]. Our quality assurance measures confirmed a longer 6MWD when performing the 6MWT a second time as well as a longer 6MWD when using a 30-m corridor compared to a 15-m test distance. Both findings have to be taken into consideration, when evaluating an individual’s 6MWD and highlight the need for standardization of methodology.
The 6MWD can be used to assess an individual’s physical performance. A prerequisite for valid grading of the 6MWD are reference values the effective 6MWD can be compared with. Several reference equations have been reported that were derived from collectives of different size, age, and sex distribution, using heterogeneous methodology [4, 5, 16, 33]. The application of these equations to a large set of patients with COPD resulted in largely varying and significantly differing values for the predicted 6MWD [4]. Hence, there is consensus that one should apply reference values from a matching population and with identical operating procedures and methodological standards.
Further, previous work reported a significant impact of age on 6MWD as well as of sex, height, weight, and other factors. To our knowledge, the studies identifying sex as significant determinant of the 6MWD did not test for sex interaction and did not adjust sex for height [4, 33]. When doing so, we found height but not sex a significant determinant of the 6MWD. Hence, we provide reference values adjusted for age and height as non-modifiable characteristics. We further provide estimates of the impact of other influencing factors for further refinement of an individual’s predicted 6MWD. An example of linear interpolation is shown in the appendix.
Higher body mass index and adverse metabolic profile as well as higher resting heart rate were associated with shorter 6MWD while more favorable cardiac structure and function went along with longer 6MWD. The negative association of eGFR with 6MWD in this collective of individuals with normal kidney function might be explained by higher muscle mass resulting in lower eGFR based on the underlying equation [34]. Nevertheless, in this population-based sample without symptomatic heart failure, we also found higher NT-proBNP associated with shorter 6MWD indicating myocardial stress associated with lower physical performance. The respective association has to be explored further in symptomatic patient collectives.
We here provide reference percentiles which can be applied to individuals aged 30 to 85 years who performed the 6MWT in a straight and flat 15-m indoor test walk. It allows to compare an individual’s test performance to the 6MWD of a healthy person of similar age and height. The 15-m setup is likely to facilitate testing as it is more readily available in doctors' offices as well as in patients’ homes. Screening and even repetitive assessment of physical performance in patients with chronic diseases including symptomatic heart failure might prove helpful in clinical decision making, but might also contribute to self-empowerment and self-motivation in these patients. Finally, the utilization of the online calculator facilitates this process and visualizes the test result. Translating the tool into a smartphone application might increase its acceptance not only in the population at large, but also in diseased groups of patients.
Conclusion
In a well-characterized representative sample of the general population, we identified age and body height, but not sex, independent determinants of the 6-min walk distance. Hence, we calculated age- and height-specific reference percentiles, which can be applied to individuals aged 30 to 85 years who performed the 6-min walk test in a straight and flat 15-m indoor test walk. We provide an online calculator to determine an individual’s predicted 6MWD. In addition, we display the effect estimates of further determinants of the 6MWD in the general population. Taken together, our results allow putting an individual person’s effective 6MWD in relation to an expected result.
Data availability
Data can be made available upon request.
References
Balke B (1963) A simple field test for the assessment of physical fitness. Rep 63–6. Rep Civ Aeromed Res Inst US. 1–8
Cooper KH (1968) A means of assessing maximal oxygen intake. Correlation between field and treadmill testing. JAMA. 203(3):201–4
Annegarn J, Spruit MA, Savelberg HH, Willems PJ, van de Bool C, Schols AM et al (2012) Differences in walking pattern during 6-min walk test between patients with COPD and healthy subjects. PLoS One 7(5):e37329. https://doi.org/10.1371/journal.pone.0037329
Andrianopoulos V, Holland AE, Singh SJ, Franssen FM, Pennings HJ, Michels AJ et al (2015) Six-minute walk distance in patients with chronic obstructive pulmonary disease: which reference equations should we use? Chron Respir Dis 12(2):111–119. https://doi.org/10.1177/1479972315575201
Giannitsi S, Bougiakli M, Bechlioulis A, Kotsia A, Michalis LK, Naka KK (2019) 6-Minute walking test: a useful tool in the management of heart failure patients. Ther Adv Cardiovasc Dis 13:1753944719870084. https://doi.org/10.1177/1753944719870084
Piepoli MF, Spoletini I, Rosano G (2019) Monitoring functional capacity in heart failure. Eur Heart J Suppl 21(Suppl M):M9–M12. https://doi.org/10.1093/eurheartj/suz216
Ross RM, Murthy JN, Wollak ID, Jackson AS (2010) The six minute walk test accurately estimates mean peak oxygen uptake. BMC Pulm Med 10:31. https://doi.org/10.1186/1471-2466-10-31
Robertson TE, Nouraie M, Qin S, Crothers KA, Kessinger CJ, McMahon D et al (2019) HIV infection is an independent risk factor for decreased 6-minute walk test distance. PLoS One 14(4):e0212975. https://doi.org/10.1371/journal.pone.0212975
Wong AW, Lopez-Romero S, Figueroa-Hurtado E, Vazquez-Lopez S, Milne KM, Ryerson CJ et al (2021) Predictors of reduced 6-minute walk distance after COVID-19: a cohort study in Mexico. Pulmonology 27(6):563–565. https://doi.org/10.1016/j.pulmoe.2021.03.004
Gomes E, Bastos T, Probst M, Ribeiro JC, Silva G, Corredeira R (2016) Reliability and validity of 6MWT for outpatients with schizophrenia: a preliminary study. Psychiatry Res 237:37–42. https://doi.org/10.1016/j.psychres.2016.01.066
Vancampfort D, Wyckaert S, Sienaert P, De Hert M, Soundy A, Rosenbaum S et al (2016) Test-retest study of the six-minute walk test in people with bipolar disorder. Psychiatr Danub 28(1):39–44
Ries JD, Echternach JL, Nof L, Gagnon BM (2009) Test-retest reliability and minimal detectable change scores for the timed “up & go” test, the six-minute walk test, and gait speed in people with Alzheimer disease. Phys Ther 89(6):569–579. https://doi.org/10.2522/ptj.20080258
Savci S, Inal-Ince D, Arikan H, Guclu-Gunduz A, Cetisli-Korkmaz N, Armutlu K et al (2005) Six-minute walk distance as a measure of functional exercise capacity in multiple sclerosis. Disabil Rehabil 27(22):1365–1371. https://doi.org/10.1080/09638280500164479
Schmidt K, Vogt L, Thiel C, Jager E, Banzer W (2013) Validity of the six-minute walk test in cancer patients. Int J Sports Med 34(7):631–636. https://doi.org/10.1055/s-0032-1323746
Butler J, Hamo CE, Udelson JE, Pitt B, Yancy C, Shah SJ et al (2016) Exploring new endpoints for patients with heart failure with preserved ejection fraction. Circ Heart Fail 9(11). https://doi.org/10.1161/CIRCHEARTFAILURE.116.003358
Holland AE, Spruit MA, Troosters T, Puhan MA, Pepin V, Saey D et al (2014) An official European Respiratory Society/American Thoracic Society technical standard: field walking tests in chronic respiratory disease. Eur Respir J 44(6):1428–1446. https://doi.org/10.1183/09031936.00150314
Wolsk E, Kaye D, Borlaug BA, Burkhoff D, Kitzman DW, Komtebedde J et al (2018) Resting and exercise haemodynamics in relation to six-minute walk test in patients with heart failure and preserved ejection fraction. Eur J Heart Fail 20(4):715–722. https://doi.org/10.1002/ejhf.976
Rostagno C, Olivo G, Comeglio M, Boddi V, Banchelli M, Galanti G et al (2003) Prognostic value of 6-minute walk corridor test in patients with mild to moderate heart failure: comparison with other methods of functional evaluation. Eur J Heart Fail 5(3):247–252. https://doi.org/10.1016/s1388-9842(02)00244-1
Mangla A, Kane J, Beaty E, Richardson D, Powell LH, Calvin JE Jr (2013) Comparison of predictors of heart failure-related hospitalization or death in patients with versus without preserved left ventricular ejection fraction. Am J Cardiol 112(12):1907–1912. https://doi.org/10.1016/j.amjcard.2013.08.014
Forman DE, Fleg JL, Kitzman DW, Brawner CA, Swank AM, McKelvie RS et al (2012) 6-min walk test provides prognostic utility comparable to cardiopulmonary exercise testing in ambulatory outpatients with systolic heart failure. J Am Coll Cardiol 60(25):2653–2661. https://doi.org/10.1016/j.jacc.2012.08.1010
Fell BL, Hanekom S, Heine M (2021) Six-minute walk test protocol variations in low-resource settings - a scoping review. S Afr J Physiother 77(1):1549. https://doi.org/10.4102/sajp.v77i1.1549
Nolen-Doerr E, Crick K, Saha C, de Groot M, Pillay Y, Shubrook JH et al (2018) Six-minute walk test as a predictive measure of exercise capacity in adults with type 2 diabetes. Cardiopulm Phys Ther J 29(3):124–129. https://doi.org/10.1097/CPT.0000000000000080
Matos Casano HA, Anjum F (2022) Six minute walk test. StatPearls. Treasure Island (FL)
Stewart T, Caffrey DG, Gilman RH, Mathai SC, Lerner A, Hernandez A et al (2016) Can a simple test of functional capacity add to the clinical assessment of diabetes? Diabet Med 33(8):1133–1139. https://doi.org/10.1111/dme.13032
Beriault K, Carpentier AC, Gagnon C, Menard J, Baillargeon JP, Ardilouze JL et al (2009) Reproducibility of the 6-minute walk test in obese adults. Int J Sports Med 30(10):725–727. https://doi.org/10.1055/s-0029-1231043
Wagner M, Tiffe T, Morbach C, Gelbrich G, Stork S, Heuschmann PU et al (2017) Characteristics and course of heart failure stages A-B and determinants of progression - design and rationale of the STAAB cohort study. Eur J Prev Cardiol 24(5):468–479. https://doi.org/10.1177/2047487316680693
Morbach C, Gelbrich G, Tiffe T, Eichner FA, Christa M, Mattern R et al (2021) Prevalence and determinants of the precursor stages of heart failure: results from the population-based STAAB cohort study. Eur J Prev Cardiol 28(9):924–934. https://doi.org/10.1177/2047487320922636
Morbach C, Gelbrich G, Breunig M, Tiffe T, Wagner M, Heuschmann PU et al (2018) Impact of acquisition and interpretation on total inter-observer variability in echocardiography: results from the quality assurance program of the STAAB cohort study. Int J Cardiovasc Imaging 34(7):1057–1065. https://doi.org/10.1007/s10554-018-1315-3
Borg GA (1982) Psychophysical bases of perceived exertion. Med Sci Sports Exerc 14(5):377–381
Ciani O, Piepoli M, Smart N, Uddin J, Walker S, Warren FC et al (2018) Validation of exercise capacity as a surrogate endpoint in exercise-based rehabilitation for heart failure: a meta-analysis of randomized controlled trials. JACC Heart Fail 6(7):596–604. https://doi.org/10.1016/j.jchf.2018.03.017
Sciurba F, Criner GJ, Lee SM, Mohsenifar Z, Shade D, Slivka W et al (2003) Six-minute walk distance in chronic obstructive pulmonary disease: reproducibility and effect of walking course layout and length. Am J Respir Crit Care Med 167(11):1522–1527. https://doi.org/10.1164/rccm.200203-166OC
Beekman E, Mesters I, Hendriks EJ, Klaassen MP, Gosselink R, van Schayck OC et al (2013) Course length of 30 metres versus 10 metres has a significant influence on six-minute walk distance in patients with COPD: an experimental crossover study. J Physiother 59(3):169–176. https://doi.org/10.1016/S1836-9553(13)70181-4
Cazzoletti L, Zanolin ME, Dorelli G, Ferrari P, DalleCarbonare LG, Crisafulli E et al (2022) Six-minute walk distance in healthy subjects: reference standards from a general population sample. Respir Res 23(1):83. https://doi.org/10.1186/s12931-022-02003-y
Levey AS, Stevens LA, Schmid CH, Zhang YL, Castro AF 3rd, Feldman HI et al (2009) A new equation to estimate glomerular filtration rate. Ann Intern Med 150(9):604–612. https://doi.org/10.7326/0003-4819-150-9-200905050-00006
Acknowledgements
We greatly appreciate the time of all STAAB participants and their willingness to provide data to the study. We also thank the Mayor of the City of Würzburg and the local registration office for their sustained support of our study. Finally, we thank the entire study team, study nurses, technicians, data managers, and students for their efforts on the STAAB study. We also thank T. Ludwig, ICE-B, for diligent data management.
Collection of biomaterials was supported by the Interdisciplinary Bank of Biomaterials and Data of the University Hospital of Würzburg and the Julius Maximilian University of Würzburg (ibdw). The implementation of the ibdw has been supported by a grant of the Federal Ministry for Education and Research (Grant number FKZ: 01EY1102).
The STAAB Consortium consists of the following: S Frantz (Dept. of Medicine I, Div. of Cardiology, University Hospital Würzburg); C. Maack (Comprehensive Heart Failure Center, University Hospital and University of Würzburg); G. Ertl (University Hospital Würzburg); M. Fassnacht (Dept. of Medicine I, Div. of Endocrinology, University Hospital Würzburg); C. Wanner (Dept. of Medicine I, Div. of Nephrology, University Hospital Würzburg); R. Leyh (Dept. of Cardiovascular Surgery, University Hospital Würzburg); J. Volkmann (Dept. of Neurology, University Hospital Würzburg); J. Deckert (Dept. of Psychiatry, Psychosomatics and Psychotherapy, Center of Mental Health, University Hospital Würzburg); H. Faller (Dept. of Medical Psychology, University of Würzburg); R. Jahns (Interdisciplinary Bank of Biomaterials and Data Würzburg, University Hospital Würzburg).
Funding
Open Access funding enabled and organized by Projekt DEAL. This work was supported by the German Ministry of Research and Education within the Comprehensive Heart Failure Centre Würzburg (BMBF 01EO1004 and 01EO1504).
C.M. receives financial support from the interdisciplinary center for clinical research—IZKF Würzburg (advanced clinician-scientist program, ADVCSP-3) as well as from the German Research Foundation (DFG) within the Comprehensive Research Center 1525 'Cardio-immune interfaces' (453989101, project C5).
F.K. is supported by the German Research Council (Deutsche Forschungsgemeinschaft, DFG), Project No. 413657723 as well as through the Clinician Scientist-Program UNION-CVD (Understanding InterOrgan Networks in Cardiac and Vascular Diseases).
Author information
Authors and Affiliations
Consortia
Contributions
Caroline Morbach Literature search, data collection, data analysis, data interpretation, writing.
Nicola Moser Literature search, figure, data analysis, data interpretation, writing.
Vladimir Cejka Data collection, data interpretation.
Michael Stach Data interpretation, development of online tool.
Floran Sahiti Data collection, data interpretation.
Fabian Kerwagen Data analysis, data interpretation.
Stefan Frantz Obtained funding, study design, data interpretation.
Rüdiger Pryss Data interpretation, supervision of the development of online tool.
Götz Gelbrich Study design, figure, data analysis, data interpretation.
Peter U. Heuschmann Obtained funding, study design, data interpretation.
Stefan Störk Obtained funding, study design, data interpretation, writing.
Corresponding author
Ethics declarations
Conflict of interest
C.M. reports research cooperation with the University of Würzburg and Tomtec Imaging Systems funded by a research grant from the Bavarian Ministry of Economic Affairs, Regional Development and Energy, Germany; she is supported by the German Research Foundation (DFG) within the Comprehensive Research Center 1525 “Cardio-immune interfaces” (453989101, project C5) and receives financial support from the Interdisciplinary Center for Clinical Research—IZKF Würzburg (advanced clinician-scientist program; AdvCSP 3). She further received advisory and speakers honoraria as well as travel grants from Tomtec, Alnylam, AKCEA, Pfizer, Boehringer Ingelheim, SOBI, AstraZeneca, NovoNordisk, Alexion, Janssen, and EBR Systems; principal investigator in trials sponsored by Alnylam, Bayer, NovoNordisk, and AstraZeneca.
N.M. has no conflicts of interest regarding the present work.
V.C. has no conflicts of interest regarding the present work.
M.S. has no conflicts of interest regarding the present work.
F.S. has no conflicts of interest regarding the present work.
F.K. has no conflicts of interest regarding the present work.
S.F. has no conflicts of interest regarding the present work.
R.P. has no conflicts of interest regarding the present work.
G.G. reports research cooperation with the University Hospital Würzburg and Tomtec Imaging Systems funded by a research grant from the Bavarian Ministry of Economic Affairs, Regional Development and Energy, Germany.
PU. H. has no conflicts of interest regarding the present work.
S.S. is supported by the CHFC Würzburg, and by the German Federal Ministry of Education and Research (BMBF). He has received consultancy and lecture fees from AstraZeneca, Bayer, Boehringer Ingelheim, Novartis, Pfizer, and Servier.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Morbach, C., Moser, N., Cejka, V. et al. Determinants and reference values of the 6-min walk distance in the general population—results of the population-based STAAB cohort study. Clin Res Cardiol (2024). https://doi.org/10.1007/s00392-023-02373-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00392-023-02373-3