Abstract
Aims
Management of comorbidities represents a critical step in optimal treatment of heart failure (HF) patients. However, minimal attention has been paid whether comorbidity burden and their prognostic value changes over time. Therefore, we examined the association between comorbidities and clinical outcomes in HF patients between 2002 and 2017.
Methods and results
The 2002-HF cohort consisted of patients from The Coordinating Study Evaluating Outcomes of Advising and Counseling in Heart Failure (COACH) trial (n = 1,032). The 2017-HF cohort were outpatient HF patients enrolled after hospitalization for HF in a tertiary referral academic hospital (n = 382). Kaplan meier and cox regression analyses were used to assess the association of comorbidities with HF hospitalization and all-cause mortality.
Patients from the 2017-cohort were more likely to be classified as HF with preserved ejection fraction (24 vs 15%, p < 0.001), compared to patients from the 2002-cohort. Comorbidity burden was comparable between both cohorts (mean of 3.9 comorbidities per patient) and substantially increased with age. Higher comorbidity burden was significantly associated with a comparable increased risk for HF hospitalization and all-cause mortality (HR 1.12 [1.02–1.22] and HR 1.18 [1.05–1.32]), in the 2002- and 2017-cohort respectively. When assessing individual comorbidities, obesity yielded a statistically higher prognostic effect on outcome in the 2017-cohort compared to the 2002-HF cohort (p for interaction 0.026).
Conclusion
Despite major advances in HF treatment over the past decades, comorbidity burden remains high in HF and influences outcome to a large extent. Obesity emerges as a prominent comorbidity, and efforts should be made for prevention and treatment.
Graphical abstract
Created with BioRender.com.

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Multimorbidity, generally defined as the co-occurrence of more than one chronic condition, frequently accompanies heart failure (HF) [1, 2]. It has been put forward that comorbid conditions are important determinants of HF outcomes and have major impact on quality of life [3, 4]. In today’s ageing society, comorbidities are the rule rather than the exception [5, 6], making healthcare professionals face the challenge of simultaneous management of HF and underlying conditions. For years, the European Society of Cardiology (ESC) Heart Failure guidelines emphasize routine testing for coexisting comorbidities in all patients suspected for HF [7]. Also in the 2021 guidelines, assessment and treatment of comorbid conditions has a prominent position [8].
Despite advances in care and treatment modalities, HF patients – especially those with worsening and acute HF – remain at high risk for adverse events, with 1-year HF hospitalization and mortality rates up to 26 and 27%, respectively [9]. Because of the significant impact of comorbidities on outcome, we assessed whether prevalence and prognostic importance of comorbidities have changed over time in HF patients after an episode of acute decompensation requiring hospitalization.
Methods
2002-HF cohort
The Coordinating Study Evaluating Outcomes of Advising and Counselling in Heart Failure (COACH) was a multicenter, randomized controlled trial in which 1023 patients were enrolled after hospitalization with acute HF as the primary diagnosis [10, 11]. Patients were included between October 2002 and February 2005 and randomly assigned to a control group (follow-up by a cardiologist) or one of two intervention groups (additional basic or intensive support by a nurse specialized in the management of HF patients). The mean follow-up period was 1.2 (± 0.5) years and patients were hospitalized for 13 days (± 10) after admission with acute HF. All patients were ≥ 18 years of age.
2017-HF cohort
This cohort consisted of all HF patients (n = 842) who visited the outpatient clinic of the University Medical Center Groningen (UMCG), in Groningen, the Netherlands, between March 2014 till December 2017. Their data were published previously [12].
In an attempt to make the 2002- and 2017-HF cohort as comparable as possible, patients from the 2017-HF cohort were only included if they visited the outpatient clinic on short term (i.e. < 2 weeks) after hospitalization for HF. In total, 382 HF patients were included in present analyses. Mean follow-up was 2.0 (± 1.0) years. All patients were ≥ 18 years of age and were treated according to the European Society of Cardiology (ESC) guidelines [7, 8].
Establishing the diagnosis of heart failure
Regarding the 2002- and 2017-HF cohort, HF diagnosis was based on typical signs and symptoms of HF, for which hospitalization was required. HF hospitalization was defined as an unplanned overnight stay with acute HF as the primary diagnosis. In both cohorts, patients with reduced as well as preserved ejection fraction were included, according to the ESC HF guidelines in force at that time [7, 13]. In present analyses, classification of patients into EF strata was based on current HF guidelines: HF with reduced EF (HFrEF, LVEF < 40%), HF with mildly reduced EF (HFmrEF, LVEF 40–49) and HF with preserved EF (HFpEF, LVEF ≥ 50).
Ethics approval
Both studies conform to the 1975 Declaration of Helsinki; with regard to the 2017-HF cohort, the Medical Ethical Committee of the UMCG waived the need for informed consent due to the retrospective nature of the study. For the 2002-HF cohort (COACH), the Medical Ethical Committee of the UMCG gave approval and all study participants provided written informed consent.
Definitions of comorbidities
The twelve cardiovascular (CV) and non-CV comorbidities included in the current study were coronary artery disease (CAD), atrial fibrillation/atrial flutter, hypertension, peripheral artery disease (PAD), cerebrovascular disease, anemia, obesity, hypercholesterolemia, diabetes mellitus, rheumatoid arthritis, chronic obstructive pulmonary disease (COPD) and chronic kidney disease (CKD). Comorbidity selection was based on available data from medical records from both HF cohorts. All medical data included in present analyses were adjudicated by one investigator and reviewed by a second investigator. Definitions of included comorbidities are shown in Supplemental Table 1. Besides the definitions, comorbidities were also included if they were noted in the inpatient or outpatient medical records or on the basis of appropriate medical treatment for this typical comorbidity. No additional diagnostic tests were performed to determine the presence of comorbidities.
Study endpoints
The primary endpoint was defined as the composite of hospitalization for HF and all-cause mortality (first to occur), during a total follow-up of 1.5 years. Hospitalization was defined as an unplanned overnight stay in the hospital due to worsening HF. Secondary endpoints were the separate components of the primary endpoint, namely HF hospitalization and all-cause mortality.
Statistical analyses
Normally distributed data are presented as means ± SD. Non-normally distributed variables are presented as medians (interquartile range [IQR]). Categorical variables are presented as a number (%). Biomarker levels of NT-proBNP were log transformed prior to analysis to obtain approximately normal distributions. Differences between two groups were analyzed with the use of the Student’s T-test for normally distributed data, the Mann-Whitney U test for non-normally distributed data and the Spearman's chi square test for categorical variables. Differences in outcome in Kaplan-Meier analysis were compared using the log-rank test. In some of these analyses HF patients were categorized as having either 0–2, 3–4 or ≥ 5 comorbid conditions. To study the association between comorbidities and several endpoints, cox proportional hazard regression analysis was performed with comorbidities as a continuous variable. All analyses were adjusted for age and sex and a multivariate model (referred to as “clinical risk model”). This clinical risk model was based on the COACH risk engine - a valuable tool to predict survival and HF hospitalization in acute HF patients [14]. Since we used comorbidities as an independent variable, all comorbidities and factors what comorbidities are based on (i.e. blood pressure) were omitted from the COACH risk engine. Eventually, the clinical risk model used in present analyses consisted of the following parameters: age, sex, left ventricular EF (LVEF), serum sodium, plasma NT-proBNP and estimated glomerular filtration rate (eGFR). All reported p values are two-tailed. For the interaction term, a p value of < 0.10 was considered to indicate statistical significance. For all other analyses, a p value < 0.05 was considered statistically significant. Analyses were performed with STATA software version 16.0 (Stata Corp LP, College Station, TX, USA) and GraphPad Prism version 8.4.2 (GraphPad Software Inc., La Jolla, USA).
Results
Patient characteristics
Baseline characteristics of the 1,023 and 382 HF patients of the 2002- and 2017-cohort are presented in Table 1. 384 (38%) and 150 (39%) of the patients of the 2002- and 2017-cohort were female, patients from the 2017-cohort showed a slightly higher LVEF (36 vs 34%, p < 0.001), had lower rates of severe HF (NYHA III-IV) and lower levels of NT-proBNP (1944 vs 2528 ng/L, p < 0.001) compared to patients from the 2002-cohort. In the 2017-cohort, a higher percentage of patients could be classified as HF with preserved EF (HFpEF), compared to the 2002-HF cohort (24% vs 15%, p < 0.001) and a lower percentage as HF with reduced EF (HFrEF; 57% vs 70%, p < 0.001). At inclusion, patients from the 2017-HF cohort were more likely to have cardiac device therapy (28 vs 8%, p < 0.001) and to receive guideline-recommended therapies with β-blockers (93 vs 66%, p < 0.001) compared to patients from the 2002-cohort. No difference in medication use between both cohorts was seen in angiotensin converting enzyme inhibitors (ACEi)/angiotensin II receptor blockers (ARB), angiotensin receptor neprilysin inhibitors (ARNI), aldosterone antagonists and diuretics.
Demographics of comorbidities
In the 2002- and 2017-HF cohort, almost all patients (e.g. 98% and 99%, respectively) suffered from comorbidities (Data not shown). The number of comorbidities ranged from 0 to 10 per individual, without difference in comorbidity burden between both HF cohorts (mean comorbidity burden of 3.9 in patients from both cohorts p = 0.92). Patients classified as HFpEF showed higher comorbidity burden compared to HFrEF patients (4.3 vs 3.7 comorbidities, p < 0.001).
To provide insight in the extensiveness of comorbidities present in HF patients, we plotted this according to age group (Fig. 1). In both HF populations, comorbidity burden substantially increased with age. While none of the patients younger than 40 years of age suffered from more than 4 comorbidities, this involved 40% and 39% of the patients aged 80 years and over, in the 2002- and 2017-cohort, respectively. HF patients from the 2002-cohort suffered more often from CAD (59 vs 48%, p < 0.001), hypercholesterolemia (39 vs 7%, p < 0.001) and rheumatoid arthritis (7 vs 3%, p = 0.004), while in patients from the 2017-cohort, anemia (45 vs 26%, p < 0.001), obesity (29 vs 23%, p < 0.001) and diabetes mellitus (45 vs 28%, p < 0.001) were more common (Table 1).
Outcomes in 2002- and 2017-HF cohort
During 1.5 years of follow-up, 260 patients of the 2002-cohort (25%) were readmitted for HF and 272 patients (27%) died, compared to 92 (24%) and 101 (26%) in the 2017-HF cohort. The primary composite endpoint was reached 411 (40%) and 138 (36%) times, respectively. No difference in event-free survival was observed between both HF cohorts (Log-rank p = 0.12) (Fig. 2).
To study if an increasing number of comorbidities was associated with a higher risk for the primary endpoint, HF patients were categorized as having either 0–2, 3–4 or ≥ 5 comorbid conditions. In both the 2002- and 2017-HF cohort, higher comorbidity burden was associated with higher risk for the primary combined endpoint (Log-rank for trend p < 0.0001 and p = 0.0037, respectively) (Supplemental Fig. 1A, B).
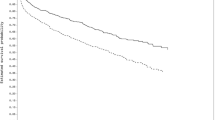
Using cox proportional hazard regression analyses, we observed that comorbidities remained a significant predictor for the combined endpoint in both HF cohorts, even after adjustment for our clinical risk model (HR 1.12 [1.02–1.22], p = 0.017 and HR 1.18 [1.05–1.32], p = 0.006 for the 2002- and 2017-HF cohort respectively), without significant difference between both cohorts (p for interaction 0.840) (Table 2). This also applies to HF hospitalization and all-cause mortality separately (Table 2). Additionally, adjusted cox regression splines for the primary combined endpoint demonstrated the association between number of comorbidities and the primary combined endpoint for both HF cohorts (Fig. 3).
Relationship between number of comorbidities and the estimated hazard ratio of the combined endpoint (e.g. HF hospitalization and all-cause mortality) in patients from the 2002-HF cohort (orange) and the 2017-HF cohort (dark green). Data is adjusted for the clinical risk model: age, sex, LVEF, sodium, log(NT-proBNP) and eGFR. The histogram represents the percentage of patients with that specific number of comorbidities
Given the awareness that individual comorbidities may have different impact on adverse outcomes, we used adjusted cox proportional hazard analyses to assess the association of individual comorbidities with the primary combined endpoint for both HF cohorts, as depicted in the Forest plot in Fig. 4. In the 2002-HF cohort, cerebrovascular disease, diabetes mellitus and CKD showed to be an independent predictor for adverse outcome, with respect to HF hospitalization and all-cause mortality (p = 0.002, p = 0.006, p = 0.021, respectively), and atrial fibrillation/flutter showed a trend towards poor outcome, although not significant. In the 2017-HF cohort, anemia, obesity and COPD were independently associated with an increased risk of the combined endpoint (p = 0.017, p = 0.002 and p = 0.009, respectively). Additionally, CKD showed a trend towards poor outcome, although not significant. CAD, hypertension, PAD, hypercholesterolemia and rheumatoid arthritis were not independently associated with primary outcome when correcting for the clinical risk model in both HF cohorts.
Forest plot showing the hazard ratio [95% CI] associated with individual comorbidities to the primary combined endpoint. Data is adjusted for the clinical risk model: age, sex, LVEF, sodium, log(NT-proBNP) and eGFR. p-values for interaction refer to interaction term between 2002- and 2017-HF cohort and respective comorbidity. Bold values denote statistical significance at the p < 0.10 level for interaction terms and p < 0.05 level for all other analyses
Test of interaction between individual comorbidities and HF-cohort (2002 or 2017) regarding clinical outcome is shown in the right column of Fig. 4. There was statistical evidence that the effect of cerebrovascular disease on outcome was greater in the 2002-cohort compared to the 2017-cohort (p for interaction 0.059). Interestingly, obesity yielded a stronger prognostic effect in the 2017-HF cohort compared to the 2002-HF cohort (p for interaction 0.026).
Discussion
Overall, there are four major findings of this study: 1) our data confirm the persistent high burden of comorbidities in HF patients and the increase of comorbidity burden with age, 2) greater comorbidity burden was associated with higher rates of HF hospitalization and all-cause mortality after 1.5 years of follow-up, 3) individual comorbidities – and in particular obesity – have high prognostic value regarding outcome and 4) no differences in event-free survival were observed between the 2002- and 2017-HF cohort.
Firstly, we demonstrated that comorbidities were and are highly prevalent in HF patients and that comorbidity burden was higher as people aged. In recent years, multimorbidity is becoming increasingly common [15, 16], as has also been shown in a population-based study of 4 million UK residents [17]. In the present study, we observe similar comorbidity burden in HF patients over a time span of 15 years.
This highlights that comorbidities continue to play an important role in HF therapy and might implicate that medical treatment for HF patients is getting more and more complicated. Also, the substantial contribution of non-CV comorbidities emphasizes that treatment of HF patients should not only be approached from a cardiological perspective, but rather multidisciplinary, involving medical specialists as well as paramedics and nutritionists.
Although it is known that optimal medical therapy contributes to a substantial reduction in both HF morbidity and mortality [18], still many HF trials do not report comorbidities at baseline or during follow-up [19]. A systematic review of 118 HF trials concluded that assessment of comorbidities remains low and incomplete, which may be due to specific exclusion-criteria in efforts to avoid competing risks of mortality and to improve study drug tolerability [19]. This underscores the need for clinical trials specifically including HF patients with multimorbidity.
Whereas chronic comorbidity burden complicates optimal treatment of all patients [20], this appears to be especially profound in HF patients. In our study, the presence of comorbidities increased the relative risk for adverse outcomes with 12 and 18% in the 2002- and 2017-cohort, respectively. Additionally, increasing comorbidity burden was associated with higher risk for HF hospitalization and all-cause mortality. These results are in line with previously published data, including a cross-sectional study of over 122,000 individuals. Braunstein and colleagues showed that patients with multimorbidity (e.g. ≥ 5 comorbidities) accounted for more than 80% of total inpatient hospital days, while they make up only approximately 40% of the total HF patient population [3]. Also, an observational cohort study showed that female HF patients without major comorbidity – not males – have comparable survival estimates compared to age- and sex-matched control subjects [21]. Strikingly, in this study, the risk of comorbidities on outcome did not decrease in the past 15 years.
Individual comorbidities also contribute largely to adverse outcomes, and not only comorbidity burden per se. When comparing the 2002- with the 2017-HF cohort, a shift in comorbidity profile was observed. An interesting example is the prevalence of obesity: While in the 2002-cohort 23% of the patients could be classified as obese (BMI ≥ 30 kg/m2), this concerned 29% of the population of the 2017-cohort. This observation may be reflective of change in HF subtype: In the 2017-cohort, a higher percentage of patients were HFpEF patients compared to the 2002-cohort (24 vs 15%, respectively). Nevertheless, the prevalence of obesity is rising drastically, nowadays exceeding 20% in many European countries. It is even expected that half of the United States population will have obesity by 2030 [22].
Interestingly, in our study, the association between obesity and HF hospitalization and all-cause mortality was stronger in the 2017-cohort compared with the 2002-cohort, resulting in an 89% increased risk for adverse outcomes. These data might suggest a shift in prognostic importance of obesity in the last 15 years. Studies have repeatedly shown that obesity is associated with HF. Results from the Framingham Heart Study revealed that subjects with obesity had a two-fold increased risk for new-onset HF, compared to their lean counterparts [23]. A post-hoc analysis in 3,310 HFpEF patients from the TOPCAT trial assessed the impact of abdominal obesity on all-cause mortality, which showed a 52% increased risk for poor outcome [24]. On the other hand, it has been proven that reduction of obesity decreases the risk of HF. A prospective cohort study of Jamaly and colleagues showed that bariatric surgery decreased the risk of HF with 35% in Swedish obese subjects [25]. Several other studies emphasize the efficacy of exercise training and lifestyle adaptation to increase quality of life and prognosis in HF patients [26, 27]. Tackling obesity effectively – by physical activity programs and nutrition – will presumably also lead to a reduction in other comorbidities and eventually better outcome.
Lastly, we did not observe differences in event-free survival between the 2002- and 2017-HF cohort, although patients from the 2017-cohort showed lower levels of NT-proBNP and were more likely to receive guideline-recommended therapies with β-blockers and cardiac devices.
Lack of improvement in HF outcomes over the past years has been shown previously by an Australian study in over 12,000 patients hospitalized for HF. Over a period of ten years, no significant change was seen in 1-year all-cause mortality and all-cause rehospitalization rates. However, 1-year rehospitalization for HF decreased slightly during their study period (30% in 2005 vs 24% in 2014) [28]. Although HF guidelines emphasize assessment and treatment of comorbidities for years [7, 8], it is debatable what we exactly have achieved in recent years, regarding comorbidity therapy. With the high number of new-onset HF cases there is the urgent need for a different – most likely multidisciplinary – approach.
Collectively, our findings underscore the importance of comorbidities as a factor promoting exacerbation of HF and worsening survival. To the best of our knowledge, this is the first study to determine the association and prognostic value of overall and individual comorbidity burden in HF patients over a time span of 15 years.
Strengths and limitations
In this retrospective study, two different HF cohorts were compared. A strength of this study is that patients from both study cohorts have been well-characterized upon cohort entry in a hospital specialized in HF care. From all patients demographic data, medical history, physical examination, laboratory measurements, electrocardiogram and echocardiogram were available.
However, there are several limitations to the present study that should be acknowledged. First, all analyses performed in this study were post-hoc analyses and should also be interpreted as such. Second, we have highlighted several major comorbidities in HF patients. Nevertheless, some comorbidities were not documented in one or both study cohorts, such as for example cancer, liver disease, mental disorders and cognitive impairment, which have been shown to be independent predictors of adverse outcomes in HF [3, 29,30,31]. For this reason, it was not possible to use a validated comorbidity score, for instance the Charlson or Elixhauser Comorbidity Index. However, we acknowledge that each comorbidity category may have an associated weight on outcome, as can also be seen in our own results. Third, comorbidities were only included at the time of cohort entry, but were not examined during the follow-up period. Severity of comorbidities at baseline and disease progression over time (e.g. glycemic control in diabetes mellitus patients) may also have a great impact on outcome, rather than the exact number of comorbidities alone. Furthermore, novel treatment strategies for HF and associated comorbidities have been emerging. This is evident from the higher proportion of patients receiving cardiac device therapy and β-blockers in the 2017-HF cohort in comparison to the 2002-HF cohort. Nevertheless, only 1 patient (0.3%) from the 2017-HF cohort was treated with ARNI at inclusion, which may not be fully reflective of the contemporary HF population in 2022. Medication use was only described at the time of cohort entry, which might explain the low percentage of patients using ARNI in the 2017-HF cohort. Additionally, large registries describe that adaption of ARNI in medical practise was a slow process with only 2% of patients using ARNI one year after FDA approval [32]. Lastly, a large proportion of HF patients in the 2017-HF cohort were not eligible for ARNI therapy based on their LVEF classification.
Last, we did not observe differences in overall survival between the 2002- and 2017-HF cohort. This might be explained by differences in both HF populations. The 2002-HF cohort was a multicenter design with specific enrollment criteria, in which intervention was mainly aimed at education and support, rather than medical treatment. By contrast, the 2017-HF cohort was a single-center study in which all patients were included in an academic center specialized in HF care. Consequently, it is possible that the 2017-cohort represented more complex HF patients in comparison with the 2002-HF cohort, which has consequences on outcome. Furthermore, both cohorts consist of post-discharge patients, who are known to be at higher risk of adverse outcomes.
Conclusion
Comorbidities are daily practice in HF and determine HF outcome to a large extent. In this study, we validate the strong impact of comorbidities – and in particular obesity – on prognosis and conclude that comorbidity burden in HF patients has not improved in recent years, despite major advances in HF treatment. These data suggest that a multidisciplinary approach – rather than the “cardiological” approach – is strongly needed to optimally treat HF patients. Since obesity directly contributes to CV risk factors and onset of HF, further studies to determine the effect of lifestyle adaptation programs, physical activity and nutritional status are urgently needed.
References
van Deursen VM, Urso R, Laroche C, Damman K, Dahlström U, Tavazzi L et al (2014) Co-morbidities in patients with heart failure: an analysis of the European heart failure pilot survey. Eur J Heart Fail 16:103–111. https://doi.org/10.1002/ejhf.30
Chamberlain AM, St Sauver JL, Gerber Y, Manemann SM, Boyd CM, Dunlay SM et al (2015) Multimorbidity in heart failure: a community perspective. Am J Med 128:38–45. https://doi.org/10.1016/j.amjmed.2014.08.024
Braunstein JB, Anderson GF, Gerstenblith G, Weller W, Niefeld M, Herbert R et al (2003) Noncardiac comorbidity increases preventable hospitalizations and mortality among medicare beneficiaries with chronic heart failure. J Am Coll Cardiol 42:1226–1233. https://doi.org/10.1016/s0735-1097(03)00947-1
Tromp J, Tay WT, Ouwerkerk W, Teng T-HK, Yap J, MacDonald MR et al (2018) Multimorbidity in patients with heart failure from 11 Asian regions: a prospective cohort study using the ASIAN-HF registry. PLOS Med 15:e1002541. https://doi.org/10.1371/journal.pmed.1002541
Steinberg BA, Zhao X, Heidenreich PA, Peterson ED, Bhatt DL, Cannon CP et al (2012) Trends in patients hospitalized with heart failure and preserved left ventricular ejection fraction: Prevalence, therapies, and outcomes. Circulation 126:65–75. https://doi.org/10.1161/CIRCULATIONAHA.111.080770
Screever EM, Meijers WC, van Veldhuisen DJ, de Boer RA (2017) New developments in the pharmacotherapeutic management of heart failure in elderly patients: concerns and considerations. Expert Opin Pharmacother 18:645–655. https://doi.org/10.1080/14656566.2017.1316377
Ponikowski P, Voors AA, Anker SD, Bueno H, Cleland JGF, Coats AJS et al (2016) 2016 ESC guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur Heart J 37:2129–2200. https://doi.org/10.1016/j.rec.2016.11.005
McDonagh TA, Metra M, Adamo M, Gardner RS, Baumbach A, Böhm M et al (2021) 2021 ESC guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur Heart J 42:3599–3726. https://doi.org/10.1093/eurheartj/ehab368
Chioncel O, Collins SP, Ambrosy AP, Pang PS, Antohi EL, Iliescu VA et al (2018) Improving postdischarge outcomes in acute heart failure. Am J Ther 25:e475–e486. https://doi.org/10.1097/MJT.0000000000000791
Jaarsma T, van der Wal MHL, Hogenhuis J, Lesman I, Luttik M-LA, Veeger NJGM et al (2004) Design and methodology of the COACH study: a multicenter randomised Coordinating study evaluating outcomes of advising and counselling in heart failure. Eur J Heart Fail 6:227–233. https://doi.org/10.1016/j.ejheart.2003.09.010
Jaarsma T, van der Wal MHL, Lesman-Leegte I, Luttik ML, Hogenhuis J, Veeger NJ et al (2008) Effect of moderate or intensive disease management program on outcome in patients with heart failure: Coordinating study evaluating outcomes of advising and counseling in heart failure (COACH). Arch Intern Med 168:316–324. https://doi.org/10.1001/archinternmed.2007.83
Gehlken C, Screever EM, Suthahar N, van der Meer P, Westenbrink B, Coster J et al (2021) Left atrial volume and left ventricular mass indices in heart failure with preserved and reduced ejection fraction. ESC Hear Fail 8:2458–2466. https://doi.org/10.1002/ehf2.13366
Remme W, Swedberg K (2001) Guidelines for the diagnosis and treatment of chronic heart failure. Eur Heart J 22:1527–1560. https://doi.org/10.1053/euhj.2001.2783
Postmus D, van Veldhuisen DJ, Jaarsma T, Luttik ML, Lassus J, Mebazaa A et al (2012) The COACH risk engine: a multistate model for predicting survival and hospitalization in patients with heart failure. Eur J Heart Fail 14:168–175. https://doi.org/10.1093/eurjhf/hfr163
Sharma A, Zhao X, Hammill BG, Hernandez AF, Fonarow GC, Felker GM et al (2018) Trends in noncardiovascular comorbidities among patients hospitalized for heart failure. Circ Hear Fail 11:e004646. https://doi.org/10.1161/CIRCHEARTFAILURE.117.004646
Buddeke J, Bots M, van Dis I, Liem A, Visseren F, Vaartjes I (2017) Trends in comorbidity in patients hospitalised for cardiovascular disease. Int J Cardiol 248:382–388. https://doi.org/10.1016/j.ijcard.2017.06.106
Conrad N, Judge A, Tran J, Mohseni H, Hedgecott D, Perez Crespillo A et al (2018) Temporal trends and patterns in heart failure incidence: a population-based study of 4 million individuals. Lancet 391:572–580. https://doi.org/10.1016/S0140-6736(17)32520-5
Vaduganathan M, Claggett BL, Jhund PS, Cunningham JW, Pedro Ferreira J, Zannad F et al (2020) Estimating lifetime benefits of comprehensive disease-modifying pharmacological therapies in patients with heart failure with reduced ejection fraction: a comparative analysis of three randomised controlled trials. Lancet 396:121–128. https://doi.org/10.1016/S0140-6736(20)30748-0
Khan M, Tahhan A, Vaduganathan M, Greene S, Alrohaibani A, Anker S et al (2020) Trends in prevalence of comorbidities in heartfailure clinical trials. Eur J Heart Fail 22:1032–1042. https://doi.org/10.1002/ejhf.1818
Wolff JL, Starfield B, Anderson G (2002) Prevalence, expenditures, and complications of multiple chronic conditions in the elderly. Arch Intern Med 162:2269–2276. https://doi.org/10.1001/archinte.162.20.2269
Drozd M, Relton S, Walker A, Slater T, Gierula J, Paton M et al (2021) Association of heart failure and its comorbidities with loss of life expectancy. Heart 107:1417–1421. https://doi.org/10.1136/heartjnl-2020-317833
Ward ZJ, Bleich SN, Cradock AL, Barrett JL, Giles CM, Flax C et al (2019) Projected U.S. state-level prevalence of adult obesity and severe obesity. N Engl J Med 381:2440–2450. https://doi.org/10.1056/NEJMsa1909301
Kenchaiah S, Evans J, Levy D, Wilson P, Benjamin E, Larson M et al (2002) Obesity and the risk of heart failure. N Engl J Med 347:305–313. https://doi.org/10.1056/NEJMoa020245
Tsujimoto T, Kajio H (2017) Abdominal obesity is associated with an increased risk of all-cause mortality in patients with HFpEF. J Am Coll Cardiol 70:2739–2749. https://doi.org/10.1016/j.jacc.2017.09.1111
Jamaly S, Carlsson L, Peltonen M, Jacobson P, Karason K (2019) Surgical obesity treatment and the risk of heart failure. Eur Heart J 40:2131–2138. https://doi.org/10.1093/eurheartj/ehz295
Pandey A, Parashar A, Kumbhani D, Agarwal S, Garg J, Kitzman D et al (2015) Exercise training in patients with heart failure and preserved ejection fraction: a meta-analysis of randomized control trials. Circ Hear Fail 8:33–40. https://doi.org/10.1161/CIRCHEARTFAILURE.114.001615
Khera A, Emdin C, Drake I, Natarajan P, Bick A, Cook N et al (2016) Genetic Risk, Adherence to a healthy lifestyle, and coronary disease. N Engl J Med 375:2349–2358. https://doi.org/10.1056/NEJMoa1605086
Al-Omary M, Khan A, Davies A, Fletcher P, Mcivor D, Bastian B et al (2018) Outcomes following heart failure hospitalization in a regional Australian setting between 2005 and 2014. ESC Hear Fail 5:271–278. https://doi.org/10.1002/ehf2.12239
Bhatt A, Ambrosy A, Dunning A, DeVore A, Butler J, Reed S et al (2020) The burden of non-cardiac comorbidities and association with clinical outcomes in an acute heart failure trial - insights from ASCEND-HF. Eur J Heart Fail 22:1022–1031. https://doi.org/10.1002/ejhf.1795
Lawson C, Solis-Trapala I, Dahlstrom U, Mamas M, Jaarsma T, Kadam U et al (2018) Comorbidity health pathways in heart failure patients: a sequences-of-regressions analysis using cross-sectional data from 10,575 patients in the Swedish Heart Failure Registry. PLoS Med 15:e1002540. https://doi.org/10.1371/journal.pmed.1002540
Ergatoudes C, Schaufelberger M, Andersson B, Pivodic A, Dahlström U, Fu M (2019) Non-cardiac comorbidities and mortality in patients with heart failure with reduced vs. preserved ejection fraction: a study using the Swedish heart failure registry. Clin Res Cardiol 108:1025–1033. https://doi.org/10.1007/s00392-019-01430-0
Luo N, Fonarow GC, Lippmann SJ, Mi X, Heidenreich PA, Yancy CW et al (2017) Early adoption of sacubitril/valsartan for patients with heart failure with reduced ejection fraction: insights from get with the guidelines-heart failure (GWTG-HF). JACC Heart Fail 5:305–309. https://doi.org/10.1016/j.jchf.2016.12.018
Funding
This work was supported by grants from the Dutch Heart Foundation (CVON SHE-PREDICTS-HF, Grant 2017-21; CVON RED-CVD, Grant 2017-11; CVON PREDICT2, grant 2018-30; CVON DOUBLE DOSE, grant 2020B005; and grant 2000Z003), by a grant from the leDucq Foundation (Cure PhosphoLambaN induced Cardiomyopathy (Cure-PLaN)), and by a grant from the European Research Council (ERC CoG 818715, SECRETE-HF). Dr. Meijers is supported by the Mandema-Stipendium of the Junior Scientific Masterclass 2020-10 of the University Medical Center Groningen and by the Dutch Heart Foundation (Dekker grant 03-005-2021-T005). The funders had no role in the design and conduct of the study; collection, analysis, and interpretation of data; writing of the manuscript; and decision to submit the manuscript for publication.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The UMCG, which employs several of the authors has received research grants and/or fees from AstraZeneca, Abbott, Boehringer Ingelheim, Cardior Pharmaceuticals Gmbh, Ionis Pharmaceuticals, Inc., Novo Nordisk, and Roche. Dr. de Boer received speaker fees from Abbott, AstraZeneca, Bayer, Novartis, and Roche. All other authors report no disclosures.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Screever, E.M., van der Wal, M.H.L., van Veldhuisen, D.J. et al. Comorbidities complicating heart failure: changes over the last 15 years. Clin Res Cardiol 112, 123–133 (2023). https://doi.org/10.1007/s00392-022-02076-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00392-022-02076-1