Abstract
Purpose
The primary aim of this study was to characterize the frequency, severity, and distress of symptoms from the colostomy and colostomy acceptance in rectal cancer patients. The secondary aims were to study the symptomatic parastomal herniation, its relationship to stoma-related symptoms, and potential risk factors for the development of symptomatic parastomal herniation.
Methods
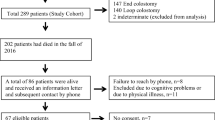
Data was collected from the Swedish Colorectal Cancer Registry and from surgical charts. Patients operated for rectal cancer with an abdominoperineal excision in Sweden between 2007 and 2009 and alive 3 years postoperatively were contacted (n = 852). Patients who consented to participate, had a colostomy constructed during the abdominoperineal excision, and who answered a questionnaire 3 years postoperative were included (n = 495). Answers were analyzed with emphasis on stoma-related symptoms and their intensity as well as the level of distress associated with the symptoms.
Results
Almost 90 % of patients did not feel limited in their daily life by their colostomy. Patients with symptomatic parastomal hernia had a 53 % higher risk of flatulence. Fifty-six patients developed symptomatic parastomal hernia (11 %). The only risk factor associated with the development of symptomatic parastomal hernia was high body mass index (BMI).
Conclusions
This study shows that most patients do not feel limited by their stoma 3 years after surgery for rectal cancer. Symptomatic parastomal hernia was associated with high BMI but not with the surgical technique.

Similar content being viewed by others
References
Miles WE (1971) A method of performing abdomino-perineal excision for carcinoma of the rectum and of the terminal portion of the pelvic colon (1908). CA Cancer J Clin 21(6):361–364
Holm T, Ljung A, Haggmark T, Jurell G, Lagergren J (2007) Extended abdominoperineal resection with gluteus maximus flap reconstruction of the pelvic floor for rectal cancer. Br J Surg 94(2):232–238
Hoerske C, Weber K, Goehl J, Hohenberger W, Merkel S (2010) Long-term outcomes and quality of life after rectal carcinoma surgery. Br J Surg 97(8):1295–1303
Cornish JA, Tilney HS, Heriot AG, Lavery IC, Fazio VW, Tekkis PP (2007) A meta-analysis of quality of life for abdominoperineal excision of rectum versus anterior resection for rectal cancer. Ann Surg Oncol 14(7):2056–2068
Pachler J, Wille-Jorgensen P (2005) Quality of life after rectal resection for cancer, with or without permanent colostomy. Cochrane Database Syst Rev (2):Cd004323
Fucini C, Gattai R, Urena C, Bandettini L, Elbetti C (2008) Quality of life among five-year survivors after treatment for very low rectal cancer with or without a permanent abdominal stoma. Ann Surg Oncol 15(4):1099–1106
Yau T, Watkins D, Cunningham D, Barbachano Y, Chau I, Chong G (2009) Longitudinal assessment of quality of life in rectal cancer patients with or without stomas following primary resection. Dis Colon Rectum 52(4):669–677
Vonk-Klaassen SM, de Vocht HM, den Ouden ME, Eddes EH, Schuurmans MJ (2015) Ostomy-related problems and their impact on quality of life of colorectal cancer ostomates: a systematic review. Qual Life Res
Londono-Schimmer EE, Leong AP, Phillips RK (1994) Life table analysis of stomal complications following colostomy. Dis Colon Rectum 37(9):916–920
Shellito PC (1998) Complications of abdominal stoma surgery. Dis Colon Rectum 41(12):1562–1572
Carne PWG, Frye JNR, Robertson GM, Frizelle FA (2003) Parastomal hernia following minimally invasive stoma formation. ANZ J Surg 73(10):843–845
Nastro P, Knowles CH, McGrath A, Heyman B, Porrett TR, Lunniss PJ (2010) Complications of intestinal stomas. Br J Surg 97(12):1885–1889
Arumugam PJ, Bevan L, Macdonald L, Watkins AJ, Morgan AR, Beynon J et al (2003) A prospective audit of stomas—analysis of risk factors and complications and their management. Colorectal Dis Off J Assoc Coloproctology Great Britain Ireland 5(1):49–52
Israelsson LA (2005) Preventing and treating parastomal hernia. World J Surg 29(8):1086–1089
Janes A, Cengiz Y, Israelsson LA (2004) Randomized clinical trial of the use of a prosthetic mesh to prevent parastomal hernia. Br J Surg 91(3):280–282
López-Cano M, Lozoya-Trujillo R, Quiroga S, Sánchez JL, Vallribera F, Martí M et al (2012) Use of a prosthetic mesh to prevent parastomal hernia during laparoscopic abdominoperineal resection: a randomized controlled trial. Hernia 16(6):661–667
Serra-Aracil X, Bombardo-Junca J, Moreno-Matias J (2009) Randomized, controlled, prospective trial of the use of mesh to prevent parastomal hernia. Dis Colon Rectum 52(9):1676
Tam KW, Wei PL, Kuo LJ, Wu CH (2010) Systematic review of the use of a mesh to prevent parastomal hernia. World J Surg 34(11):2723–2729
van Dijk SM, Timmermans L, Deerenberg EB, Lamme B, Kleinrensink GJ, Jeekel J et al (2015) Parastomal hernia: impact on quality of life? World J Surg 39(10):2595–2601
North J (2014) Early intervention, parastomal hernia and quality of life: a research study. Br J Nurs 23(5):S14–S18
Feddern ML, Emmertsen KJ, Laurberg S (2015) Life with a stoma after curative resection for rectal cancer. A population-based, cross-sectional study. Colorectal Dis Off J Assoc Coloproctology Great Britain Ireland
Lian L, Wu XR, He XS, Zou YF, Wu XJ, Lan P et al (2012) Extraperitoneal vs. intraperitoneal route for permanent colostomy: a meta-analysis of 1,071 patients. Int J Color Dis 27(1):59–64
Sjodahl R, Anderberg B, Bolin T (1988) Parastomal hernia in relation to site of the abdominal stoma. Br J Surg 75(4):339–341
Ortiz H, Sara MJ, Armendariz P, de Miguel M, Marti J, Chocarro C (1994) Does the frequency of paracolostomy hernias depend on the position of the colostomy in the abdominal wall? Int J Color Dis 9(2):65–67
Nguyen MH, Pittas F (1999) How large should a skin trephine be for an end stoma? Aust N Z J Surg 69(9):675–676
Resnick S (1986) New method of bowel stoma formation. Am J Surg 152(5):545–548
Prytz M, Angenete E, Bock D, Haglind E (2015) Extralevator abdominoperineal excision for low rectal cancer-extensive surgery to be used with discretion based on 3-year local recurrence results: a registry-based, Observational National Cohort Study. Ann Surg
Prytz M, Angenete E, Ekelund J, Haglind E (2014) Extralevator abdominoperineal excision (ELAPE) for rectal cancer—short-term results from the Swedish Colorectal Cancer Registry. Selective use of ELAPE warranted. Int J Color Dis 29(8):981–987
Asplund D, Prytz M, Bock D, Haglind E, Angenete E (2015) Persistent perineal morbidity is common following abdominoperineal excision for rectal cancer. Int J Colorectal Dis
Asplund D, Heath J, Gonzalez E, Ekelund J, Rosenberg J, Haglind E et al (2014) Self-reported quality of life and functional outcome in patients with rectal cancer—QoLiRECT. Dan Med J 61(5):A4841
Angenete E, Correa-Marinez A, Heath J, Gonzalez E, Wedin A, Prytz M et al (2012) Ostomy function after abdominoperineal resection—a clinical and patient evaluation. Int J Color Dis 27(10):1267–1274
Steineck G, Helgesen F, Adolfsson J, Dickman PW, Johansson JE, Norlen BJ et al (2002) Quality of life after radical prostatectomy or watchful waiting. N Engl J Med 347(11):790–796
Bergmark K, Avall-Lundqvist E, Dickman PW, Henningsohn L, Steineck G (1999) Vaginal changes and sexuality in women with a history of cervical cancer. N Engl J Med 340(18):1383–1389
Zou G (2004) A modified Poisson regression approach to prospective studies with binary data. Am J Epidemiol 159(7):702–706
Burch J (2007) Constipation and flatulence management for stoma patients. Br J Community Nurs 12(10):449–452
Evans MD, Williams GL, Stephenson BM (2009) Preventing parastomal herniation: is prophylactic prosthetic mesh absolutely necessary? World J Surg 33(7):1538–1539, author reply 40-1
Duchesne JC, Wang YZ, Weintraub SL, Boyle M, Hunt JP (2002) Stoma complications: a multivariate analysis. Am Surg 68(11):961–966, discussion 6
Janes A, Cengiz Y, Israelsson LA (2010) Experiences with a prophylactic mesh in 93 consecutive ostomies. World J Surg 34(7):1637–1640
Janes A, Cengiz Y, Israelsson LA (2009) Preventing parastomal hernia with a prosthetic mesh: a 5-year follow-up of a randomized study. World J Surg 33(1):118–121, discussion 22-3
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
ALF—The agreement concerning research and education of doctors at Sahlgrenska University Hospital, the Swedish Research Council, the Swedish Society of Medicine, and The Health and Medical Care Committee of the Regional Executive Board, Region Västra Götaland.
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Marinez, A.C., González, E., Holm, K. et al. Stoma-related symptoms in patients operated for rectal cancer with abdominoperineal excision. Int J Colorectal Dis 31, 635–641 (2016). https://doi.org/10.1007/s00384-015-2491-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-015-2491-4